Surgically Removing The Prostate Gland
A radical prostatectomy is the surgical removal of your prostate gland. This treatment is an option for curing prostate cancer that has not spread beyond the prostate or has not spread very far.
Like any operation, this surgery carries some risks.
Before having any treatment, 67% of men said they could get erections firm enough for intercourse.
When the men who had a radical prostatectomy were asked again after 6 months, this had decreased to 12%. When asked again after 6 years, it had slightly improved to 17%.
For urinary incontinence, 1% of men said they used absorbent pads before having any treatment.
When the men who had a radical prostatectomy were asked again after 6 months, this had increased to 46%. After 6 years, this had improved to 17%.
Out of the men who were actively monitored instead, 4% were using absorbent pads at 6 months and 8% after 6 years.
In extremely rare cases, problems arising after surgery can be fatal.
Its possible that prostate cancer can come back again after treatment. Your doctor should be able to explain the risk of your cancer coming back after treatment, based on things like your PSA level and the stage of your cancer.
After a radical prostatectomy, youll no longer ejaculate during sex. This means you will not be able to have a child through sexual intercourse.
Read Also: What Is The Definition Of Prostate Gland
Urgent Signs And Symptoms
For emergencies that can’t wait, call 911.
- You have a persistent or recurring temperature greater than 101 F or repeated chills.
- Your catheter stops draining urine despite adequate hydration and no kinks in the tubing.
- Your urine in your Foley catheter is cloudy, foul smelling or persistently bloody .
- You have no bowel movement by day five after surgery.
- You have an unexplained severe pain that you didn’t experience while in the hospital.
- You are nauseated or vomiting.
- You have asymmetrical leg swelling .
- You have worsening redness, swelling or drainage from your incisions.
Other Robotic Prostatectomy Surgery Considerations
There are some other factors that I will look into in deciding if a patient is a good fit for surgery.
One of those factors is your weight. If you are really obese, then this can make the surgery difficult for a couple reasons. First of all, it can be technically challenging if there is a lot of fatty tissue in the body for a variety of reasons.
Additionally, for patients who are morbidly obese, it can make it technically risky from an anesthesia perspective, meaning that it may be hard to manage your breathing mechanics while you are off to sleep.
When we do this surgery, we position you with your legs in the air and your head towards the ground. All the weight from your belly can make it hard to breathe in that position, which is why for some people due to their weight I will not offer surgery as an option.
Another technical factor that I will consider is your prior medical/surgical history.
If you have had surgeries and/or radiation in your belly in the past for any reason, this can lead to added scar tissue formation, which can make the technical aspects of getting exposure to the prostate difficult.
Recommended Reading: What Causes Prostate Cancer In Young Males
How Soon Can We Detect This
One of the main advantages of surgery over radiotherapy for prostate cancer is that following prostate removal, the PSA should be very low , which we can of course detect with blood tests. If metastasis occurs, because the metastatic cells originated in the prostate and therefore make PSA, the PSA level in the blood starts to rise. Once it has reached a given threshold additional or salvage treatment will be discussed.
A PSA level of more than 0.2 ng/ml defines biochemical recurrence. At this stage the cancer is still much too small to be seen on scanning. If it can be seen on a scan it is termed clinical recurrence, which generally does not occur until the PSA level is more than 0.5 ng/ml. Symptoms, such as bone pain, dont usually occur until the PSA is more than 20 ng/ml.
Other Medications And Devices
Although medications like sildenafil and tadalafil are effective for many men with post-surgery erectile dysfunction, they arent the best choice for everyone.
If your prostatectomy causes damage to the nerves near your penis, or if you take medication for hypertension, angina or other health conditions, using an oral ED medication may not be a suitable option for you.
-
Penile injection therapy. This involves using injectable medications to stimulate blood flow and improve your erections. These medications are typically administered using a very small needle to minimize discomfort.Although this treatment method may sound unpleasant, its relatively simple to use and has a success rate of 70 percent to 80 percent.
-
Vacuum constriction devices . Also known as a penis pump, a VCD works by creating a vacuum around your penis. This draws blood into your penis and allows it to become erect.
Recommended Reading: Does An Enlarged Prostate Make It Hard To Poop
Can I Have Radiation Therapy First And Then Surgery
With modern radiation therapy techniques, local tissue damage is often kept at a minimum, and surgeons at some of the larger cancer centers have been seeing improved results with salvage prostatectomy performed after radiation. But even under the best of circumstances, post-radiation surgery is a very difficult operation to perform, and few surgeons across the country perform it regularly.
Who Should Not Take Cialis Or Generic Cialis
Do not take CIALIS® or generic CIALIS® if you:
- Have severe liver disease. Tell your doctor if you have mild to moderate liver disease as you may need dosage reductions.
- Have severe kidney disease. Tell your doctor if you have mild to moderate kidney disease as you may need dosage reductions
- Take any medicines called nitrates
- Use recreational drugs called poppers like amyl nitrite and butyl nitrite
- Take any medicines called guanylate cyclase stimulators, such as riociguat
- Are allergic to CIALIS®, tadalafil or ADCIRCA®, or any of its ingredients
Recommended Reading: Are Peanuts Bad For The Prostate
How You Might Feel
Being diagnosed with prostate cancer can be stressful. It is natural to have a wide variety of emotions after the diagnosis and during treatment, including anger, fear anxiety, sadness and resentment. These feelings may become stronger over time as you adjust to the physical side effects of treatment.
Everyone has their own ways of coping with their emotions. There is no right or wrong way. It is important to give yourself and those around you time to deal with the emotions that cancer can cause. For support, call Cancer Council 13 11 20.
If you have continued feelings of sadness, have trouble getting up in the morning or have lost motivation to do things that previously gave you pleasure, you may be experiencing depression. This is quite common among people who have had cancer.
If you think you may be depressed or feel that your emotions are affecting your day-to-day life, talk to your GP. Counselling or medication even for a short time may help. Some people can get a Medicare rebate for sessions with a psychologist. Cancer Council may also run a counselling program in your area.
For information about coping with depression and anxiety, call Beyond Blue on 1300 22 4636. For 24-hour crisis support, call Lifeline 13 11 14.
Hormone Therapy Helps Some Prostate Cancer Survivors Live Longer
A study published in the New England Journal of Medicine in January 2017 indicates that men whose prostates are removed to treat prostate cancer are likely to survive longer if they take drugs to block the male hormone testosterone in addition to undergoing radiation therapy.
Unfortunately, its not that simple.
Also Check: Is Dark Chocolate Good For Prostate
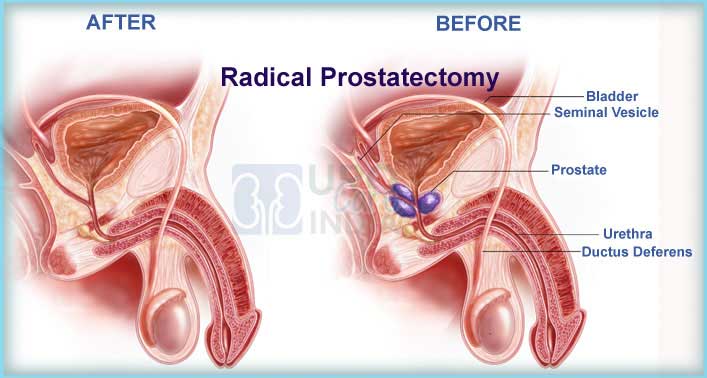
What Is A Radical Prostatectomy
Surgery to remove the prostate to treat prostate cancer is called a radical prostatectomy. The aim of surgery is to remove all of the cancer cells.
It is usually done when the cancer is contained in the prostate and has not spread to the surrounding area.
A prostatectomy may sometimes be done to treat locally advanced prostate cancer. But usually, this operation is not possible. This is because the surgeon would not be able to remove all the cancer cells that have spread outside the prostate. Other types of surgery, such as transurethral resection of the prostate , can help with the symptoms of locally advanced prostate cancer.
A prostatectomy is a big operation and may not be suitable for everyone. Your doctor can tell you whether it is suitable or if a different treatment may be best for you.
See also
How Is Prostate Cancer Staged
Prostate cancer is one of the most common types of cancer that develops in men and is the second leading cause of cancer deaths in American men, behind lung cancer and just ahead of colorectal cancer. The prognosis for prostate cancer, as with any cancer, depends on how advanced the cancer has become, according to established stage designations.
The prostate gland is a walnut-sized gland present only in men, found in the pelvis below the bladder. The prostate gland wraps around the urethra and lies in front of the rectum. The prostate gland secretes part of the liquid portion of the semen, or seminal fluid, which carries sperm made by the testes. The fluid is essential to reproduction.
The term to stage a cancer means to describe the evident extent of the cancer in the body at the time that the cancer is first diagnosed.
- Clinical staging of prostate cancer is based on the pathology results, physical examination, PSA, and if appropriate, radiologic studies.
- The stage of a cancer helps doctors understand the extent of the cancer and plan cancer treatment.
- Knowing the overall results of the different treatments of similarly staged prostate cancers can help the doctor and patient make important decisions about choices of treatment to recommend or to accept.
Recommended Reading: Does An Enlarged Prostate Affect A Man Sexually
Read Also: What Age To Have Prostate Exam
How Are Hormone Therapies For Prostate Cancer Administered
LHRH agonists, the most commonly used drug class for hormone therapy, are given in the form of regular shots: once a month, once every three months, once every four or six months, or once per year. These long-acting drugs are injected under the skin and release the drug slowly over time. LHRH antagonists include degarelix and relugolix, an oral form.
Confirming What Weve Practiced For Years
- What was the grade of the cancer?
- Was it at the edge of the removed prostate gland?
- Was it in the attached seminal vesicles or extending beyond the capsule?
- Was there cancer in any removed lymph nodes?
- What is the trend of serum PSA since surgery?
- How old is the patient, what are his other medical issues, and what are his goals?
You May Like: Metastatic Castration Resistant Prostate Cancer Mcrpc
Surgery To Remove Your Prostate Gland
You might have surgery to remove your prostate gland if:
- your cancer hasnt spread outside the prostate gland
- you are younger and have a fast growing tumour
- as part of treatment for locally advanced or high risk localised prostate cancer
The aim of a radical prostatectomy operation is to cure prostate cancer. It is major surgery with some possible side effects. If youre an older man with a slow growing prostate cancer, this type of surgery may not be necessary for you. This is because your cancer might grow so slowly that youre more likely to die of old age or other causes than from prostate cancer.
Radical Prostatectomy Retropubic Or Suprapubic Approach
You’ll be positioned on the operating table, lying on your back.
An incision will be made from below the navel to the pubic region.
The doctor will usually perform a lymph node dissection first. The nerve bundles will be released carefully from the prostate gland and the urethra will be identified. The seminal vesicles may also be removed if necessary.
The prostate gland will be removed.
A drain will be inserted, usually in the right lower area of the incision.
You May Like: Odds Of Surviving Prostate Cancer
What Are The Risks Of Radiation Treatment
Radiation treatment for prostate cancer may increase a manâs risk for having another cancer later in life, such as bladder or rectal cancer.
Some radiation side effects, like urinary problems, are usually short-term problems that go away with time. But a radiation side effect can become a long-term problem. Common side effects from radiation treatment include:
- Bowel problems, such as rectal pain, diarrhea, blood in your stool, and rectal leakage.
- In one study, 67 out of 100 men had erections firm enough for intercourse before they had radiation. Six years later, 27 out of 100 men who had radiation had erections firm enough for intercourse.footnote 4
For men with intermediate-risk or high-risk prostate cancer, radiation treatment may be given along with hormone therapy. Hormone therapy has side effects, such as the loss of bone density and muscle mass. It can also increase the risk for bone fractures, diabetes, and heart disease.
Your doctor might advise you to have surgery if:
- You are healthy enough to have major surgery.
- Radiation therapy isnât a good option for you because you have had previous radiation therapy to your pelvic area or you have a serious bowel disease such as ulcerative colitis.
Your doctor might advise you to have radiation if:
- You have other health problems that make surgery too risky.
What Happens To A Man When He Has His Prostate Removed
Prostate is a male reproductory gland located anterior to the rectum and inferior to the bladder surrounding the urethra. It is involved in the secretion of prostate fluid that forms an important constituent of semen. It also works in the propulsion of seminal fluid into the urethra and also blocks the connection between the urethra and the bladder by contracting at the time of ejaculation. The prostatic fluid constitutes about one third of the total seminal fluid containing various enzymes of which PSA is of specific importance, not only in thinning of the seminal fluid and helping proper motility of the sperm, but also in the testing procedure for prostate related diseases, such as BPH .
The location of prostate is such that, if the patient experiences BPH then it might lead to urethral compression causing difficulty in urination and leading to LUTS . Unfortunately, BPH is a common problem in adult men and the chances of BPH drastically increases after the age of 60 years. A growth in size of prostate is also a sign of prostatic cancer.
You May Like: Super Beta Prostate Supplement Side Effects
Also Check: What To Do For Enlarged Prostate
Doctor Visits And Tests
Your doctor visits will usually include PSA blood tests, possibly with digital rectal exams if your prostate hasnt been removed. These will probably begin within a few months of finishing treatment. How often you need follow-up visits and tests might depend to some extent on the stage of your cancer and the chance of it coming back. Most doctors recommend PSA tests about every 6 months or so for the first 5 years after treatment, and at least yearly after that. Bone scans or other imaging tests might also be done, depending on your medical situation and symptoms.
Prostate cancer can recur even many years after treatment, which is why its important to keep regular doctor visits and report any new symptoms .
Keeping Up With Appointments And Screenings
Attending your doctors appointments after youve entered remission is very important. If you need to skip an appointment, you should make another appointment as soon as possible.
Use these appointments as a time to discuss any concerns you may have with your doctor. Your doctor can also conduct tests to check for the cancers return during these appointments.
Two tests to detect recurrent prostate cancer include a digital rectal exam and a PSA blood test. During a DRE, your doctor will insert a finger into your rectum. If your doctor detects something unusual, theyll likely ask for additional follow-up tests. These tests may include bone scans and imaging studies, such as an ultrasound or MRI.
Men often experience side effects from their prostate cancer treatments. Some of these side effects may be immediate and temporary. Others may take several weeks or months to show up and never fully disappear.
Common side effects from prostate cancer treatment include:
Also Check: How Long Does It Take To Recover From Prostate Surgery
What If My Psa Rises While Im On Hormone Therapy
When the PSA is rising or cancer is spreading despite a low level of testosterone, prostate cancer is called castration-resistant, or hormone-refractory. Despite this name, some hormonal therapies may still work. But prostate cancer in this setting may progress and become more aggressive and resistant, and you should be prepared to discuss additional treatment strategies with your doctor. This is the time when a medical oncologist, if not already involved in your care, gets involved. These doctors specialize in medical, systemic treatments for prostate cancer, which is useful at this time given that your disease is typically metastatic, meaning that it is not confined to only one location. Cancer cells in this situation have typically spread through the blood stream or lymphatics to other places in the body, and localized treatments are rarely helpful except in circumstances where where you are having symptoms, such as problems with urination.
Fortunately, more and more treatments for metastatic castration-resistant prostate cancer have become available in recent years, including certain newer androgen directed therapies, taxane chemotherapy, immunotherapy, PARP inhibitors, and, in 2022, lutetium-PSMA radionuclide therapy. Additional tests are required for some of these treatments to see if your particular type of prostate cancer is likely to respond. See Chapter 5 in PCFs Prostate Cancer Patient Guide for more details.
