When You Arrive At The Scan Department
The radiographer might ask you to change into a hospital gown. You might;not have to undress if your clothing doesnt have any metal, such as zips or clips.;
You have to:
- remove any jewellery, including body piercings and your watch
- remove your hair clips
- empty your pockets of coins and keys
Its safe to take a relative or friend into the scanning room with you. But check with the department staff first. Your friend or relative will also need to;remove any metal they have on them.
What Are Some Common Uses Of The Procedure
Your doctor uses MRI to evaluate prostate cancer and see if it is limited to the prostate. Mp-MRI provides information on how water molecules and blood flow through the prostate. This helps determine whether cancer is present and, if so, whether it is aggressive and if it has spread.
Occasionally, MRI of the prostate is used to evaluate other prostate problems, including:
- infection or prostate abscess.
- some older cardiac defibrillators;and pacemakers
Tell the technologist if you have medical or electronic devices in your body. These devices may interfere with the exam or pose a risk. Many implanted devices will have a pamphlet explaining the MRI risks for that particular device. If you have the pamphlet, bring it to the attention of the scheduler before the exam. MRI cannot be performed without confirmation and documentation of the type of implant and MRI compatibility. You should also bring any pamphlet to your exam in case the radiologist or technologist has any questions.
If there is any question, an x-ray can detect and identify any metal objects. Metal objects used in orthopedic surgery generally pose no risk during MRI. However, a recently placed artificial joint may require the use of a different imaging exam.
How Are Mri Scans Used In Prostate Cancer Assessments
MRI technology has developed very significantly in recent years. This affords a new role for MRI in the understanding of prostate cancer. Traditionally, MRI was used to stage prostate cancer after a biopsy had confirmed the presence of cancer. The purpose of the MRI scan was confined to the assessment of how far the cancer had spread.
At Birmingham Prostate Clinic, our practice is to carry out an MRI scan before a biopsy, in order to assess whether a biopsy is necessary.
Also Check: How To Massage A Man’s Prostate
What Are The Risks Of An Mri Keyboard_arrow_down
A very small number of people have an allergic reaction to the gadolinium contrast medium. Most reactions are mild, such as a rash or hives .;
You may be asked to have a blood test to check your kidney function before the scan. If you have very poor kidney function, you will not be given contrast medium.;
Nephrogenic systemic fibrosis is currently a recognised, but rare complication of MRI believed to be caused by the injection of certain MRI contrast material in patients with poor kidney function. We do not use this contrast material in I-MED practices.;
If an endorectal coil is used for the scan, there is also a very small risk of damage to the rectum from the balloon. If you have any concerns, please speak to one of our staff.
What Is The Procedure For A Pelvic Mri Scan
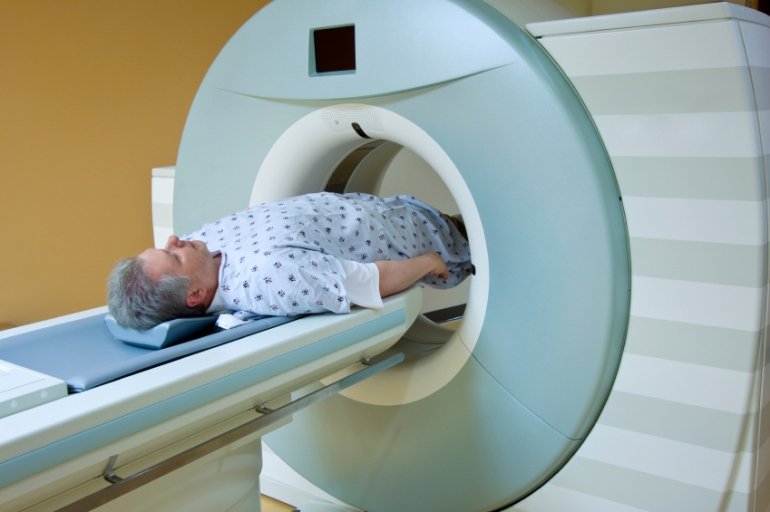
According to the Mayo Clinic, the magnetic field generated by the MRI temporarily aligns the water molecules in your body. Radio waves take these aligned particles and produce faint signals, which the machine then records as images.
If your test requires contrast dye, a nurse or doctor will inject it into your bloodstream through an IV line. You may need to wait for the dye to circulate through your body before beginning the test.
An MRI machine looks like a large metal and plastic doughnut with a bench that slowly glides you into the center of the opening. Youll be completely safe in and around the machine if you followed your doctors instructions and removed all metal. Youll lie on your back on the table that slides into the machine. And you may receive a pillow or blanket to make you more comfortable as you lay on the bench.
The technician may place small coils around your pelvic region to improve the quality of the scan images. One of the coils may need to go inside your rectum if your prostate or rectum is the focus of the scan.
The technician will be in another room and control the movement of the bench using a remote control. But theyll be able communicate with you over a microphone.
The machine may make some loud whirring and thumping noises as it takes the images. Many hospitals offer earplugs, while others have televisions or headphones to help you pass the time.
Also Check: What Happens To The Prostate Later In Life
How The Test Will Feel
An MRI exam causes no pain. If you have difficulty lying still or are very nervous, you may be given a medicine to relax you. Too much movement can blur MRI images and cause errors.
The table may be hard or cold, but you can request a blanket or pillow. The machine produces loud thumping and humming noises when turned on. You can wear ear plugs to help reduce the noise.
An intercom in the room allows you to speak to someone at any time. Some MRIs have televisions and special headphones that you can use to help the time pass.
There is no recovery time, unless you were given a medicine to relax. After an MRI scan, you can resume your normal diet, activity, and medicines.
About The Enhanced Mri Technology We Use At Bpc
There are two aspects of the new technology used at BPC in addition to more standard MRI technology:
Dynamic MRI
MRI scans have traditionally had a role in the staging of prostate cancer telling us to what extent the cancer has spread within or outside the gland. At BPC, we use what is known as dynamic contrast-enhanced MRI. It is sometimes referred to as the MRI movie because it does much more than a basic cross-section of the prostate; it goes through the prostate every 20 seconds for three minutes after contrast have been given into a small vein. This helps us to have a much clearer idea of whether the tumour is breaching the gland and whether the surrounding nodes are involved. This is particularly important if the surgeon is considering whether it is safe to undertake nerve-sparing surgery or whether it is necessary to use wider margins and remove some nerves in order to eradicate all cancer cells.
Diffusion Weighted-Imaging
I believe that the advances in MRI technology and the application of those advances to prostate cancer assessment is probably the most significant development in the whole field of prostate cancer in recent years. It has transformed the way we assess prostate cancer.
Alan Doherty, Consultant Urologist, Birmingham Prostate Clinic
Also Check: Can An Enlarged Prostate Cause Constipation
Positron Emission Tomography Scan
A PET scan is similar to a bone scan, in that a slightly radioactive substance is injected into the blood, which can then be detected with a special camera. But PET scans use different tracers that collect mainly in cancer cells. The most common tracer for standard PET scans is FDG, which is a type of sugar. Unfortunately, this type of PET scan isnt very useful in finding prostate cancer cells in the body.
However, newer tracers, such as fluciclovine F18, sodium fluoride F18, and choline C11, have been found to be better at detecting prostate cancer cells.
Other newer tracers, such as Ga 68 PSMA-11 and 18F-DCFPyl , attach to prostate-specific membrane antigen , a protein that is often found in large amounts on prostate cancer cells. Tests using these types of tracers are sometimes referred to as PSMA PET scans.
These newer types of PET scans are most often used if its not clear if prostate cancer has spread. For example, one of these tests might be done if the results of a bone scan arent clear, or if a man has a rising PSA level after initial treatment but its not clear where the cancer is in the body.
The pictures from a PET scan arent as detailed as MRI or CT scan images, but they can often show areas of cancer anywhere in the body. Some machines can do a PET scan and either an MRI or a CT scan at the same time, which can give more detail about areas that show up on the PET scan.;
D Evaluation For Local Recurence
mpMRI can be of value in men with biochemical failure after radical prostatectomy and radiation therapy, to help evaluate for local recurrence versus systemic recurrence, to help guide biopsies, and to help inform therapy choice. Suspicion of recurrence in the setting of biochemical failure is a valid reason for clinicians to request a mpMRI.
mpMRI can also be used to help targeted biopsies to more accurately diagnose radiation failure and to possibly determine who may benefit more from local and even focal salvage therapy.121 Diagnostic accuracy in the identification of tumors is better with a multi-parametric approach over strictly T2WI or DCE. Brachytherapy, external beam radiotherapy, and focal therapies tend to diffusely decrease the signal intensity of the peripheral zone on T2-weighted images due to the loss of water content, consequently mimicking tumor and hemorrhage. The combination of T2WI and functional studies such as DWI and DCE imaging improves the identification of local relapse. Tumor recurrence tends to restrict on diffusion images and avidly enhances after contrast administration.118
Key Point
Also Check: Does Enlarged Prostate Cause Constipation
How Do I Prepare For A Prostate Mri Keyboard_arrow_down
There is no special preparation for the scan. You should continue to take any regular medications, and generally eat and drink as normal.;
Before the examination begins, you will be asked a series of questions about whether you have any metal implants, such as artificial joints, or electronic devices, such as pacemakers, inside you. This is because some of these can cause you harm or be damaged if they are put into the strong magnetic field of the MRI machine.;
If you have a pacemaker, please let us know at the time of booking your appointment. You should also bring any report or previous scans with you to your appointment.;
Some metal bands and loops of wire can become quite hot if put into the scanner, so you will be asked to remove any such metal before entering the scan room.
Considering Prostate Cancer Screening Options A Prostate Mri May Save You From An Unnecessary Biopsy
1 in 9 men will be diagnosed with prostate cancer during their lifetime. A prostate biopsy is commonly used to diagnose prostate cancer. But a non-invasive, non-surgical alternative exists: prostate MRI. Learn about the advantages of prostate MRI, which may save you from an unnecessary biopsy. And talk to your care provider about having your prostate MRI performed at UVA Medical Center.
Don’t Miss: Enlarged Prostate Sexuality
Who Interprets The Results And How Do I Get Them
A radiologist, a doctor trained to supervise and interpret radiology exams, will analyze the images. The radiologist will send a signed report to your primary care or referring physician, who will share the results with you.
Follow-up exams may be needed. If so, your doctor will explain why. Sometimes a follow-up exam is done because a potential abnormality needs further evaluation with additional views or a special imaging technique. A follow-up exam may also be done to see if there has been any change in an abnormality over time. Follow-up exams are sometimes the best way to see if treatment is working or if an abnormality is stable or has changed.
What Are The Benefits Of A Prostate Mri
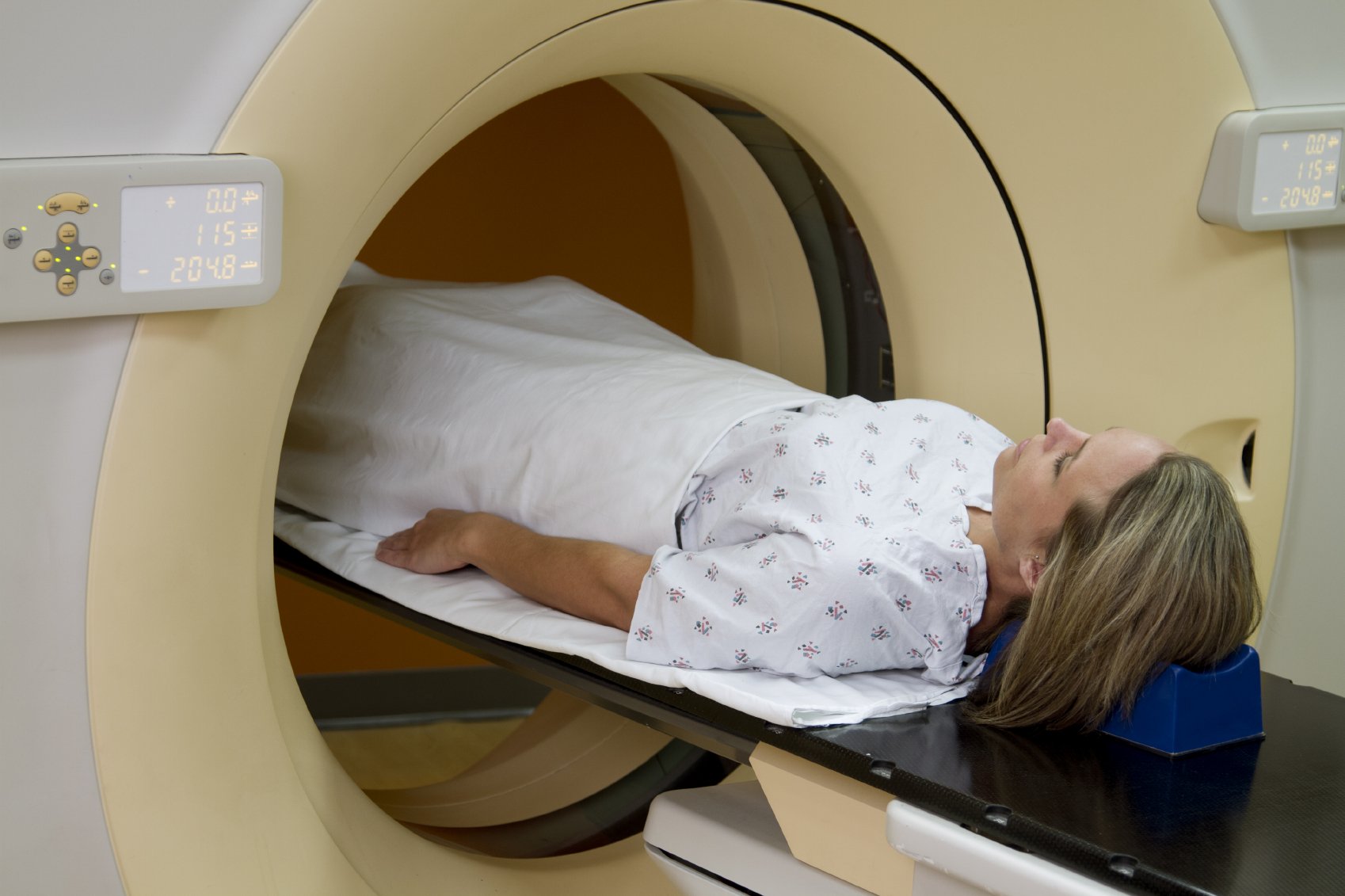
The MRI scan can help find a cancer of the prostate gland, especially if you have elevated or rising PSA.
If a cancer has already been found, the MRI images can show whether it has spread outside the prostate gland or not. This can have a very important impact on whether or not you have treatment, and if so, which type of treatment you receive.
Also Check: Does Cialis Shrink The Prostate
What Will I Experience During And After The Procedure
Most MRI exams are painless. However, some patients find it uncomfortable to remain still. Others may feel closed-in while in the MRI scanner. The scanner can be noisy. Sedation may be arranged for anxious patients, but fewer than one in 20 require it.
You may feel pressure while the doctor inserts the endorectal coil into your rectum. This is similar to that experienced during a digital rectal exam.
It is normal for the area of your body being imaged to feel slightly warm, but if it bothers you, notify the radiologist or technologist. It is important that you remain perfectly still while the images are being recorded, which is typically only a few seconds to a few minutes at a time. For some types of exams, you may be asked to hold your breath. You will know when images are being recorded because you will hear tapping or thumping sounds when the coils that generate the radiofrequency pulses are activated. You will be able to relax between imaging sequences, but will be asked to maintain your position as much as possible.
You will usually be alone in the exam room during the MRI procedure. However, the technologist will be able to see, hear and speak with you at all times using a two-way intercom. Many MRI centers allow a friend or parent to stay in the room as long as they are also screened for safety in the magnetic environment.
Preparation For The Biopsy
You cannot take aspirin or other blood thinners, such as Plavix, Eliquis, Brilinta, Pradaxa, Coumadin, Warfarin, Ibuprofen, Naproxen, Aleeve, Advil, Celebrex, Ecotrin, and many others for several days prior to your scheduled biopsy. If you take any of these or other anticoagulants please discuss this with your Urologist beforehand. It might be necessary that you also consult with your Cardiologist prior to stopping.
Recommended Reading: What Happens To The Prostate Later In Life
What Is Magnetic Resonance Imaging
Magnetic resonance imaging; is a medical imaging;technique used for both screening and diagnostic imaging.
This imaging;modality generates detailed images;of soft tissues;at different angles;and has an appropriate sensitivity when detecting tumors.
Its principle lies in how the water molecules in your body interact with a magnetic field;and radio waves.
The water molecules in the body are made of protons that align in the same direction as an MRI scanners magnetic field. Once the protons in your body are aligned with the high-intensity MRI scanners main magnet, a magnetic interference is introduced . When the interference is turned off, the protons will slowly return to their original spin. Interestingly, the protons produce a signal as they relax back to normal. Receivers measure the signal and transform it into MRI images.
Technologists;set up different types of sequences;to image various types of tissues. For instance, a sequence called T1 is great for analyzing bone structures on the MRI scan,;while a T2 is better for looking at tissues such as the liver or prostate.
A dark spot on a T1-weighed MRI scan;is interpreted as a zone with excess water like edema, inflammation, or hemorrhages. A dark spot on a T2-weighed scan would be seen as fibrosis, calcification, or low proton density tissue. A T2-weighed sequence is generally used to visualize tumors.
What Are The Limitations Of Mri Of The Prostate
High-quality images depend on your ability to remain perfectly still and follow breath-holding instructions while the images are being recorded. If you are anxious, confused or in severe pain, you may find it difficult to lie still during imaging.
A person who is very large may not fit into certain types of MRI machines. There are weight limits on the scanners.
Implants and other metallic objects can make it difficult to obtain clear images. Patient movement can have the same effect.
A very irregular heartbeat may affect the quality of images. This is because some techniques time the imaging based on the electrical activity of the heart.
MRI cannot always distinguish between cancer and inflammation or the presence of blood products within the prostate. Blood may sometimes appear due to a prostate biopsy. To avoid confusing any bleeding with cancer, your doctor may wait six to eight weeks after prostate biopsy to perform prostate MRI. This will allow any remnants of bleeding to resolve.
MRI typically costs more and may take more time to perform than other imaging methods. Talk to your insurance provider if you have concerns about the cost of MRI.
Don’t Miss: Prostatitis Symptoms Mayo
C Role Of Mpmri In Evaluating Regional Lymphatics
Currently available imaging modalities for the evaluation of lymph nodes in patients with intermediate to high risk prostate cancer have high specificity and accuracy but only low to moderate sensitivity. mpMRI appears to be equivalent to computerized tomography and positron emission tomography in this regard.
Although we are not aware of any contemporary direct comparisons of CT and mpMRI for pelvic lymph node metastases, a meta-analysis published in 2008 suggested no meaningful difference in operating characteristics, although both were notably suboptimal with pooled sensitivity of 0.39 0.42 and pooled specificity of 0.82.111
Von Below et al. showed that mpMRI DWI had a 90% specificity, 55% sensitivity, and 72.5% accuracy for lymph node metastasis in 40 patients with intermediate- and high-risk prostate cancer, 20 of whom had histologically-proven lymph node positive disease. The true-positive patients had significantly more involved lymph nodes , with larger diameter compared with the false-negative group.115 Vallini et al. showed that using 3.0T DWI mpMRI with a multiple b-value spin echo-echo planar imaging sequence may help distinguish benign from malignant pelvic lymph nodes in patients with prostate cancer.116
Key Points
