What To Expect After Radical Prostatectomy
Most men stay in the hospital for 1 to 3 days after radical prostatectomy. Your care team inserts a urinary catheter during the surgery, and some men may need to wear the catheter home for a few days to a few weeks. Another catheter inserted through the skin also may need to stay in place for a few days after returning home.
Pain after radical prostatectomy can generally be controlled with prescription pain medicines. It can take weeks or months for urinary and sexual function to return to their maximum levels.
After radical prostatectomy, itâs important to see your doctor for all your regular follow-up appointments to make sure your prostate cancer doesnât return.
Show Sources
What About Other Treatments I Hear About
When you have cancer you might hear about other ways to treat the cancer or treat your symptoms. These may not always be standard medical treatments. These treatments may be vitamins, herbs, special diets, and other things. You may wonder about these treatments.
Some of these are known to help, but many have not been tested. Some have been shown not to help. A few have even been found to be harmful. Talk to your doctor about anything youre thinking about using, whether its a vitamin, a diet, or anything else.
Recommended Reading: Alternative Cures For Prostate Cancer
Open Radical Prostatectomy Vs Minimally Invasive Radical Prostatectomy
In 2003, only 9.2% of radical prostatectomies were done using a minimally invasive procedure. By 2007, that number had jumped to 43.2%. In 2009, researchers in Boston reported on a study that compared outcomes, benefits, and complications of open surgery vs. minimally invasive surgery:
- No difference was found in deaths or in the need for additional cancer therapy between the two approaches.
- The median hospital stay was two days for minimally invasive surgery and three days for open surgery.
- 2.7% of men having laparoscopic surgery required a blood transfusion compared with 20.8% of men having open surgery.
- There was more anastomotic stricture narrowing of the suture where internal body parts are rejoined for open surgery than for minimally invasive surgery .
- There were fewer respiratory complications with minimally invasive surgery than with open surgery .
- There were lower rates of incontinence and erectile dysfunction with open surgery. The overall rate was 4.7% for laparoscopic surgery and 2.1% for open surgery.
You May Like: Hormone Therapy For Advanced Prostate Cancer
Read Also: Is Stage 4 Prostate Cancer Bad
What Are The Different Types Of Prostate Cancer Surgery
The most common one is called a radical prostatectomy. In this procedure, the entire prostate gland is removed, along with some of the surrounding tissue. In some cases, nearby lymph nodes are removed as well. There are several surgical approaches for this, including traditional open surgery. We can also use minimally invasive procedures, such as laparoscopic surgery and robot-assisted laparoscopic surgery.
A critical aspect of a radical prostatectomy is tailoring it to the individual features of each mans cancer. One size does not fit all. This means the exact same procedure is not appropriate for every person. The location, size, and other features of the cancer are considered to design an operation that is appropriate for the person.
In a laparoscopic radical prostatectomy, a surgeon inserts a tiny camera called a laparoscope through a small cut in the abdomen. The camera gives doctors a magnified, high-definition picture of the prostate gland. With that image as a guide, the surgeon can remove the prostate, seminal vesicles, and lymph nodes using special tools.
To do a robot-assisted procedure, a surgeon sits at a console that has a screen as well as hand, finger, and foot controls. The surgeons hand, wrist, finger, and foot movements control the robotic instruments inside the patient in real time.
What Typically Increases The Risk Of Complications From Prostate Cancer Surgery
Complication risks can be increased if prior surgery for unrelated reasons was done in the area or if we have to do extensive surgery to remove the cancer. But complication rates also go up dramatically when we do surgery on patients who have failed other prostate cancer treatments, such as radiation therapy.
Radiation is a very effective treatment for prostate cancer, but it doesnt work for everyone. In these patients, we often believe the cancer has recurred or persisted in the prostate without spreading, so removing the prostate following failed radiation treatment a procedure called salvage prostatectomy is potentially curative.
Salvage prostatectomy is more technically challenging than radical prostatectomy. Patients who have already had radiation therapy often have scarring in and around the prostate, which can make tissue in the area very difficult to separate while performing the operation. As a result, patients undergoing salvage prostatectomy have a much higher risk of urinary incontinence, and a higher rate of developing more scar tissue, strictures which is a narrowing of the urethra that blocks urine flow or injury to adjacent structures like the rectum.
Read Also: Is Coffee Bad For Prostate
Life After Prostate Removal
For many men with prostate cancer, prostate removal is never needed because the cancer is often slow-growing and managed with non-surgical treatments. But, if the cancer has grown beyond the prostate, the oncologist may recommend prostate removal surgery, also called a prostatectomy. If you are going to have prostate removal surgery, this information can help you in your discussion with the doctors.
Prostatectomy Age Limit May Not Apply
To determine if this upper age limit was justified, researchers compared the risk of complications and/or death within 30 days after radical prostatectomy in more than 11,000 men who underwent the procedure in Canada from 1990 to 1999.
The results, published in the Journal of the National Cancer Institute, showed that 0.5% of men died following the procedure and 20% experienced one or more complications.
Increasing age was associated with an increasing risk of complications, but the absolute risk of death was still relatively low for older men up to age 79. For example, the absolute risk of death was 0.66% among men aged 70 to 79 — only slightly higher than the overall risk.
Instead, researchers found the risk of complications or death was more closely related to the presence of other medical problems, such as heart disease or stroke, than age alone.
Researchers say these results suggest that radical prostatectomy is a relatively safe treatment option for otherwise healthy older men up to age 79. But more research should look at the use of detailed risk assessments and interventions to reduce the risks to men considering prostatectomy with other health conditions.
Show Sources
Journal of the National Cancer Institute
Recommended Reading: How Effective Is Hormone Treatment For Prostate Cancer
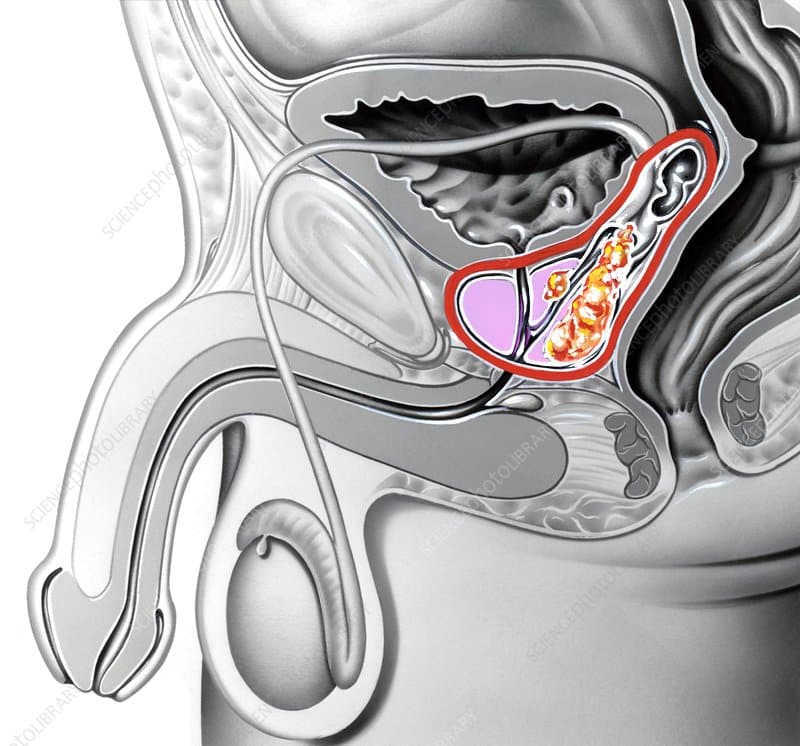
What Does The Prostate Do
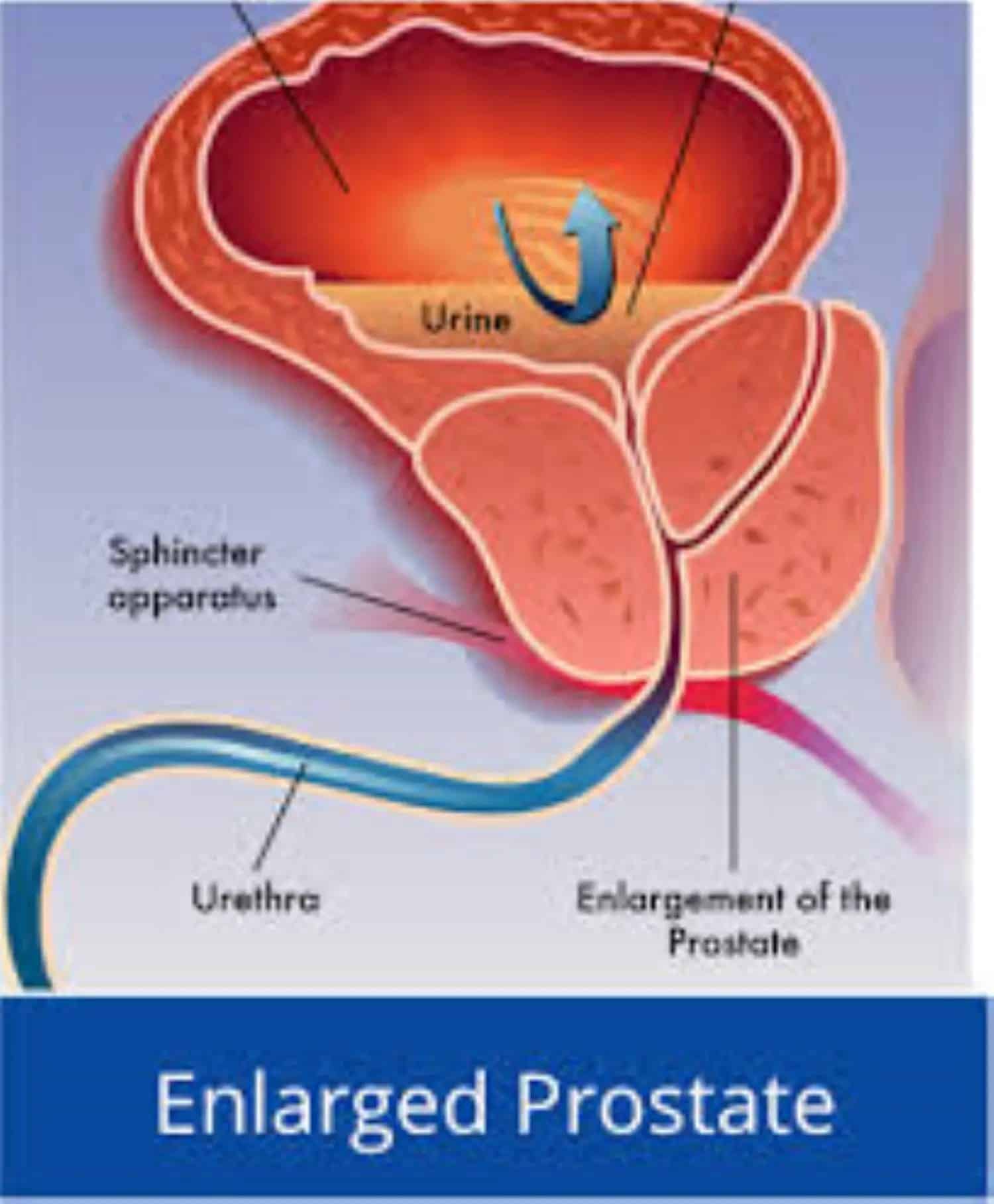
As men get older their prostate often enlarges.
Benign prostate enlargement causes men to urinate more frequently and is a common medical condition in men over 50.
BPE does not make a patient more likely to develop prostate cancer, however.
The causes of prostate cancer are largely unknown, although research suggests that its linked to obesity and family history.
Dont Miss: How To Check For Enlarged Prostate At Home
When To Call Your Doctor Or Nurse
Its important to tell your doctor or nurse if:
- your bladder feels full or your catheter isnt draining urine
- your catheter leaks or falls out
- your urine contains blood clots, turns cloudy, dark or red, or has a strong smell
- you have a fever
- you feel sick or vomit
- you get cramps in your stomach area that will not go away
- you get pain or swelling in the muscles in your lower legs.
Your doctor or nurse will let you know if you should go to the hospital.
Recommended Reading: Can Prostate Cancer Spread To The Esophagus
What Are The Side Effects Of Prostate Radiation
Even though both external beam radiation and brachytherapy use the same radiation as the cure from the cancer cells, they have some common side effects.
- Bowel problems: Radiation proctitis is a very common inflammation of the rectum that occurs as a result of the radiation treatment of prostate cancer where damage to the rectum was acquired. Proctitis can lead to diarrhea, with the blood in the stool, and rectal leakage. Most of these problems go away over time, but in rare cases, normal bowel function does not return. In order to minimize bowel problems, doctors will advise what kind of diet to follow during radiation therapy to help limit bowel movement during treatment.
- Urinary problems: Radiation cystitis is the side effect of inflammation and subsequent destruction of the normal work of the urinary bladder at the cellular level after the usage of radiation in the treatment. Patients will feel the need to urinate more often, have a burning sensation while the urinate process, and/or find blood in the urine itself. Urinary problems usually improve over time, but in some men, they never go away.
- Erection problems : Patience after the treatment, with radiation or through surgery, has the same rate of impotence level. These problems do not occur right after radiation therapy but are slowly developing over time. The effect of radiation treatment is more visible if the patient is elderly, where impotence is already on the low level.
Cancer Treatments And Erectile Dysfunction
Following surgery, many men experience erectile dysfunction , but for many, the disruption is temporary. Nerves damaged during surgery may result in erectile dysfunction. A nerve-sparing prostatectomy may reduce the chances of nerve damage. Another factor is the surgeons skill level for performing the nerve-sparing technique, which if done correctly, may improve patients likelihood of retaining erectile function, says Dr. Shelfo.
Prostate cancer may also be treated with various types of radiation therapybrachytherapy, external beam radiation or stereotactic body radiation therapy. Each type of therapy causes somewhat different side effects. About half of all prostate cancer patients who undergo any of these types of radiation therapy are likely to develop erectile dysfunction, according to a 2016 article published in Advances in Radiation Oncology.
- You will stay in hospital for two to five days.
- Nurses will monitor your vital signs.
- Your pain will be managed with medication.
- You may be given antibiotics to reduce the risk of infection.
- You may have a drip inserted into your arm or hand for a few days.
- You will most likely have a drain tube out of your abdomen that will be removed in the first day or two after the surgery.
- In most cases, you will have to go home still wearing the catheter. You will be taught how to care for it.
Recommended Reading: How To Reduce Prostate Size
What Is A Prostatectomy
A prostatectomy is a surgical procedure for the partial or complete removalof the prostate. It may be performed to treatprostate cancerorbenign prostatic hyperplasia.
A common surgical approach to prostatectomy includes making a surgicalincision and removing the prostate gland . This may beaccomplished with either of two methods, the retropubic or suprapubicincision , or a perineum incision .
Prior to having a prostatectomy, it’s often necessary to have aprostate biopsy. Please see this procedure for additional information.
How Effective Is Modern Radiation Treatment Of Prostate Cancer
Radiation therapy can give more radiation dose directly to the prostate than to surrounding healthy tissues, given the improvements in technology and imaging techniques. Physicians use various imaging techniques to see the prostate and surrounding tissues in three dimensions, so that the radiation beams can be tailored more precisely to the individual patients unique needs. Physicians can estimate and minimize the dose of radiation that will be received near the rectum, small bowel, bladder and hips during the course of radiation treatment to reduce the risk of side effects and complications. The goal is to safely provide a higher dose of radiation than even five years ago, which helps to improve the chances of cure. For similar stage and prostate cancer types, radiation therapy is as effective as surgery but with a different treatment process and different side effects.
Read Also: Recurrent Prostate Cancer Symptoms
Read Also: Does Prostate Cancer Affect Libido
How Effective Is Turp And What Consequences Can It Have
Studies have shown that TURP can permanently reduce prostate-related problems. Nine months after having TURP, about 75 out of 100 men only have mild symptoms. For example, at night they only need to get up to go to the bathroom once, or not at all. The other men usually still benefit from TURP, but the effect is smaller. Side effects are common, though.
Some men are afraid that they will have erection problems after surgery. Although there is no guarantee that this wont happen, research has shown that permanent erection problems are rare. Some men even feel more comfortable with their sexuality after surgery because they no longer have bothersome symptoms such as having to go to the bathroom a lot.
Advantages And Disadvantages Of Surgery
What may be important for one person might be less important for someone else. The advantages and disadvantages of surgery may depend on your age, general health and the stage of your cancer.
Advantages
- If the cancer is completely contained inside the prostate, surgery will remove all of the cancer.
- The prostate is looked at under a microscope to give a clearer picture of how aggressive your cancer is, whether it has spread outside your prostate and if you need further treatment.
- Your health professionals can get a good idea of whether your cancer was completely removed during surgery. Your PSA level should drop so low that its not possible to detect it at six to eight weeks after surgery.
- If there are signs that your cancer has come back or wasnt all removed, you may be able to have further treatment.
- Some men find it reassuring to know that their prostate has been physically removed, although you will still need to have follow-up tests to make sure no cancer cells have spread outside the prostate.
Disadvantages
Read Also: Natural Supplements For Prostate Inflammation
Don’t Miss: How Fast Does Prostate Cancer Grow
How Does The Procedure Work
After anesthesia, a surgeon will insert a tool called a resectoscope into the urethra. In some cases, a separate device will be used to flush sterile fluid through the surgical site.
Once the surgeon has positioned the resectoscope, they will use it to cut away abnormal prostate tissues and seal broken blood vessels.
Finally, the surgeon will insert a long plastic tube called a catheter into the urethra and flush destroyed prostate tissues into the bladder where they are excreted through urine.
Staging Of Prostate Cancer
Doctors will use the results of your prostate examination, biopsy and scans to identify the âstageâ of your prostate cancer .
The stage of the cancer will determine which types of treatments will be necessary.
If prostate cancer is diagnosed at an early stage, the chances of survival are generally good.
You May Like: Does Viagra Cause Prostate Cancer
What Current Options Exist To Treat Erectile Dysfunction After Radical Prostatectomy
Options include pharmacologic and nonpharmacologic interventions. Pharmacotherapies include the oral PDE-5 inhibitors , intraurethral suppositories , and intracavernous injections . Non-pharmacologic therapies, which do not rely on the biochemical reactivity of the erectile tissue, include vacuum constriction devices and penile implants .
Men who have undergone nerve-sparing technique should be offered therapies that are not expected to interfere with the potential recovery of spontaneous, natural erectile function. In this light, penile prosthesis surgery would not be considered an option in this select group, at least in the initial 2 year post-operative period, until it becomes evident in some individuals that such recovery is unlikely.
You May Like: What Supplements Are Good For Prostate Health
What Happens After Urethral Sling Surgery
Patients usually recover from this surgery quickly. Its best to limit demanding activities for approximately six weeks after surgery to avoid having the sling loosen before healing is complete.
After surgery, there may be swelling that makes it difficult to urinate. Youll have a catheter coming out of the urethra for two to three days. After this, the catheter is removed and just about everyone is able to void on their own. In rare cases, the catheter may have to be reinserted for a few days or up to a week if you cannot urinate.
After the swelling goes down, youll gradually be able to urinate on your own and empty your bladder. However, your normal urination pattern may not return for a few weeks.
The majority of men whove had this procedure have been cured of their urinary incontinence and no longer use pads. The others usually improve to the point where they dont use as many pads as they were before.
Also Check: Robotic Prostate Surgery Side Effects
Read Also: When Should You Get A Prostate Exam
Coping With Infertility After Prostate Surgery
The prostate is one of the only organs in a males body that never stops growing. This growth is slow and continual throughout your life and many doctors dont fully understand why it happens. In some instances, the prostate grows larger than your body can accommodate, and the result is benign prostatic hyperplasia or enlarged prostate. While this isnt life threatening, it can lead to an array of uncomfortable symptoms. There are treatment options for benign prostatic hyperplasia, with the most invasive being surgery. Some men will also develop prostate cancer during their lives. While prostate cancer has one of the highest curability rates, it needs to be diagnosed early so that surgery can eradicate the cancer completely. Regardless of why you need prostate surgery, certain instances can lead to problems such as infertility. In this article, well explore everything you need to know about the prostate and how to cope with infertility after prostate surgery.
Fast Facts On Bph Surgery:
- Surgery is rarely the first line of treatment for BPH.
- A doctor who specializes in the urinary tract does most TURP surgeries.
- TURP is considered a fairly safe, effective procedure for treating BPH.
According to the American Urological Association, transurethral resection of the prostate or TURP is the most common type of surgery used to treat BPH. Every year, doctors perform it on around 150,000 American men.
Surgeons perform most TURP procedures when the patient is under general anesthesia and unconscious or asleep.
Alternatively, they use spinal anesthesia, where a needle is placed in the spine to stop any sensation below the waist.
Also Check: Is Prostate Cancer More Common Than Breast Cancer
