Locally Advanced Prostate Cancer
Doctors may describe prostate cancer as localised, locally advanced and metastatic. Locally advanced prostate cancer means that the cancer has broken through the capsule of the prostate gland. It may have spread into the:
- tissue around the prostate
- body organs nearby such as the back passage or bladder
- lymph nodes close to the prostate gland
In the TNM staging system, locally advanced prostate cancer is the same as T3 or T4. Below is a simplified description of the T3 and T4 stage:
T3 means the cancer has broken through the capsule of the prostate gland.
T4 means the cancer has spread into other body organs nearby, such as the back passage, bladder, or the pelvic wall.
Combining Nadt And Chemotherapy
Pan et al conducted a retrospective review of 3 different therapies in patients with very-high-risk localized prostate cancer: neoadjuvant chemohormonal therapy , in 60 men neoadjuvant hormonal therapy , in 73 men and immediate RP without neoadjuvant therapy , in 44 men. The NCHT group had better biochemical progression-free survival time after surgery compared with the NHT and No-NT groups . After RP, 81% of patients in NCHT group, 73% of patients in NHT group, and 48% of patients in No-NT group achieved an undetectable PSA , despite patients in the NCHT having significantly poorer prognostic factors. Randomized controlled investigations are needed to validate these results, and further follow-up is required.
Multiple phase I/II trials have also been performed to investigate the use of neoadjuvant chemotherapy alone prior to RP, however no patients in these trials achieved a complete pathologic response . As there is currently no evidence demonstrating improved clinical outcomes with the use of neoadjuvant chemotherapy alone or neoadjuvant androgen deprivation therapy alone, future research will likely focus on combined neoadjuvant chemohormonal therapy.
Although no data have yet emerged that definitively support the routine use of neoadjuvant chemohormonal therapy, its safety has been evidenced by several phase I/II clinical trials. Most of the trials on neoadjuvant chemohormonal therapy have investigated docetaxel. These are summarized in Table 4 below.
Metastasis And Contiguous Spread
Seminal vesicle involvement by prostatic adenocarcinoma is common, observed in about 12% of contemporary radical prostatectomy specimens from patients with cancer clinically confined to the prostate . There are three patterns of seminal vesicle invasion: direct spread along the ejaculatory duct complex into the seminal vesicles prostatic capsular perforation followed by extension into the periprostatic soft tissues and spread into the seminal vesicles and isolated deposits of cancer in the seminal vesicles .171-175 Intraepithelial spread most likely results from direct invasion of carcinoma from the muscular wall of seminal vesicles rather than extension from the ejaculatory duct system in the invaginated extraprostatic space.176 Endorectal coil MRI is accurate in detecting seminal vesicle invasion according to radical prostatectomy correlation studies, with loss of architectural contour as a dominant feature.177 Bilateral invasion portends a worse prognosis than does unilateral invasion.178
Rectal adenocarcinoma occasionally invades the seminal vesicles and prostate, and may cause diagnostic difficulty.184 Metastases to the seminal vesicles and retrovesicular space from other organs are rare, including renal cell carcinoma, seminoma, malignant thymoma, and melanoma.185-189
David G. Bostwick, in, 2008
You May Like: What Is A Nodule On The Prostate
Treatment Of Locally Advanced Prostate Cancer: A Case Report And Narrative Review
Frank PeinemannAcademic Editor: Received
Abstract
Introduction. Treatment of locally advanced prostate cancer is under discussion. Differences between clinical and pathological staging and risk factors such as positive surgical margins and seminal vesicle involvement challenge the individual treatment decisions. Case Presentation. Clinical tumor stage before treatment was assessed to be T2. After radical prostatectomy, pathological examination revealed the stage pT3b N0 M0 including positive surgical margin and seminal vesicle involvement. Early adjuvant androgen deprivation therapy and late adjuvant radiation therapy were added in response to the pathological risk factors. No evidence of disease was observed for 15 years after the treatment. The unexpected pathological findings were not explained by the physicians in charge. Discussion. A narrative review of the recent literature showed that multiple treatment modalities including adjuvant radiotherapy following radical prostatectomy are consistent with current recommendations. The multimodal approach has possibly cured a high-risk patient and may also work successfully in other patients. An alternative treatment option with better preservation of health-related quality of life might have also achieved a similar good overall survival.
1. Introduction
2. Case Presentation
3. Discussion
Conflict of Interests
Perineural Invasion On Prostate Biopsy: Does It Mean That I Have Advanced Prostate Cancer
The simple answer is NO, however it should change your treatment game plan.
A member of one of my support groups who has been doing active surveillance for about 5 years recently reported that their current biopsy indicated that they now have perineural invasion . They did not understand what was the significance of this finding and they wanted to know if they now had advanced prostate cancer.
In reality, PNI is found in almost 30% of positive biopsies.
However, before I discuss the significance of this finding it is important to understand what this means. When a pathologist finds that there is PNI they are saying that they have found prostate cancer cells surrounding or tracking along a nerve fiber within the prostate. This does not mean that the cancer has left the gland.
Not withstanding this the importance of this finding , it takes on a new light when you realize that nerves within the prostate travel outside of the gland through microscopic holes in the prostate capsule. The capsule is the outer covering of the prostate gland, which for some period of time can manage to contain cancer cells within the gland. In essence it is a barrier protecting the rest of your body from prostate cancer cells.
However, the nerves do pierce the capsule and can offer an easy exit point for cancer cells from the gland to the rest of your body.
Simply put, the presence of PNI doubles the chance of a man having T3 disease .
Stone NN, Stock RG, Parikh D, et al.J Urol. 1998 160:17221726.
Read Also: Do Prostate Massages Help Prevent Cancer
Perineural Invasion And Seminal Vesicle Involvement Predict Pelvic Lymph Node Metastasis In Men With Localized Carcinoma Of The Prostate
Stone NN, Stock RG, Parikh D, et al.
J Urol. 1998 160:17221726 .
In an effort to evaluate the ability of the presence of biopsy PNI to predict a subsequent finding of lymphatic or seminal vesicle involvement by prostate cancer, Stone and associates evaluated 212 men who presented with clinically localized prostate cancer and underwent staging pelvic lymph node dissection. Using univariate and multivariate analyses, the presence of biopsy PNI was correlated with the likelihood of metastatic prostate cancer found on pelvic lymphadenectomy. Stone and colleagues found that biopsy PNI was a better predictor of lymph node metastasis than serum prostate-specific antigen , biopsy Gleason score, or clinical stage. The authors concluded that men with biopsy PNI seeking definitive therapy for clinically localized prostate cancer should be counseled for staging pelvic lymph node dissection before definitive therapy. The potential role of biopsy PNI in predicting an increased likelihood of seminal vesicle invasion or lymphatic metastasis warrants further research. Additional support of the predictive power of PNI for lymphatic metastasis could strengthen the argument for staging lymph node dissection in the large number men with this biopsy finding who choose to undergo brachytherapy or external beam radiotherapy for clinically localized prostate cancer.
You May Like: Prostate Cancer In Young Men
Stages Of Prostate Cancer
In order to determine the stage of a patients prostate cancer, most doctors start by using the TNM staging system, which helps describe different aspects of the cancers growth.
- T the T category measures the size and extent of the Tumor
- N the N category measures whether and how far the cancer has spread to the Lymph Nodes
- M the M category whether the cancer has spread to other organs in the body (a process called Metastasis
The score for each of these categories is determined based on a pre-determined set of criteria. Your doctor cannot feel or see the tumor with a score of T1. A score of T3 means that the tumor has begun to grow outside of the prostate.
After calculating the TNM categories, doctors will combine the TNM score with the patients Gleason score and PSA levels assigning of a specific stage to the patients cancer.
Prostate cancer prognosis and survival rates can help give patients an idea of their chances of surviving the disease based on the stage and time of diagnosis. While some patients may find this information helpful, others may not want to know.
Recommended Reading: Extreme Fatigue After Prostate Removal
General Information About Prostate Cancer
In This Section
The median age at diagnosis of carcinoma of the prostate is 67 years. Prostate cancer may be cured when localized, and it frequently responds to treatment when widespread. The rate of tumor growth varies from very slow to moderately rapid, and some patients may have prolonged survival even after the cancer has metastasized to distant sites, such as bone. The 5-year relative survival rate for men diagnosed in the United States from 2011 to 2017 with local or regional disease was greater than 99%, and the rate for distant disease was 31% a 98% survival rate was observed for all stages combined. The approach to treatment is influenced by age and coexisting medical problems. Side effects of various forms of treatment should be considered in selecting appropriate management.
Many patientsespecially those with localized tumorsmay die of other illnesses without ever having suffered disability from the cancer, even if managed conservatively without an attempt at curative therapy. In part, these favorable outcomes are likely the result of widespread screening with the prostate-specific antigen test, which can identify patients with asymptomatic tumors that have little or no lethal potential. There is a large number of these clinically indolent tumors, estimated from autopsy series of men dying of causes unrelated to prostate cancer to range from 30% to 70% of men older than 60 years.
Robotic Assisted Laparoscopic Radical Prostatectomy
Minimally invasive surgical technique to remove the prostate and seminal vesicles. The surgeon performs the procedure through five 1-cm incisions spread in the shape of a fan across the lower abdomen. The surgeon performs the procedure using a robotic surgical assist device called the daVinci® Surgical System. Takes 2.5-3.5 hours to perform with a hospital stay of 24-48 hours.
Also Check: Different Types Of Radiation Therapy For Prostate Cancer
Which Treatments Are Best In Keeping Men In Remission
Here is your opportunity to compare prostate cancer treatments. Over 129,000 patients underwent PSA monitoring after treatment to see which treatments were most effective at keeping the cancer in remission. The charts show which treatments are more likely to leave patients Prostate Cancer Free, for how many years. Share this data, talk with your Doctor, or multiple Doctors and make an informed decision. Select the treatment option, that is best for you.
Compare Prostate Cancer Treatments by gathering information about your own Prostate Cancer Diagnosis. Your Doctor will provide three elements that describe your prostate cancer. Your PSA, Stage and Gleason Score. These three elements help you determine your risk group. Find and select your Risk Group in the table below. This will take you to the comparing prostate cancer treatments page, where you can select different prostate cancer treatments on an interactive chart and graphically see their effectiveness over time.
The treatments included in this study are Prostate Surgery or Prostatectomy, , Brachytherapy or Seeds, High Dose Rate Radiation, HDR, External Beam Radiation Therapy or EBRT, Androgen Deprivation Therapy, ADT, or Hormone Treatment, Proton Therapy, High-Intensity Focused Ultrasound, HIFU, Cryotherapy, Cryo and Hypo-Fractionated External Beam Radiation Therapy. For more advanced prostate cancer, treatments are combined to increase effectiveness.
Treatment Options Under Clinical Evaluation
Treatment options under clinical evaluation for patients with prostate cancer include the following:
Cryosurgery
Cryosurgery, or cryotherapy, is under evaluation for the treatment of localized prostate cancer. It is a surgical technique that involves destruction of prostate cancer cells by intermittent freezing of the prostate with cryoprobes, followed by thawing. There is limited evidence regarding its efficacy and safety compared with standard prostatectomy and radiation therapy, and the technique is evolving in an attempt to reduce local toxicity and normal tissue damage. The quality of evidence on efficacy is low, currently limited to case series of relatively small size, short follow-up, and surrogate outcomes of efficacy.
Serious toxic effects associated with cryosurgery include bladder outlet injury, urinary incontinence, sexual impotence, and rectal injury. Impotence is common, ranging from about 47% to 100%.
The frequency of other side effects and the probability of cancer control at 5 years’ follow-up have varied among reporting centers, and series are small compared with surgery and radiation therapy. Other major complications include urethral sloughing, urinary fistula or stricture, and bladder neck obstruction.
Proton-beam therapy
Vascular-targeted photodynamic therapy using a photosensitizing agent has been tested in men with low-risk prostate cancer.
Neoadjuvant hormonal therapy
The role of neoadjuvant hormonal therapy is not established.
Bicalutamide
Don’t Miss: What Are The Grades Of Prostate Cancer
What Are Grade Groups
Grade Groups are a new way to grade prostate cancer to address some of the issues with the Gleason grading system.
As noted above, currently in practice the lowest Gleason score that is given is a 6, despite the Gleason grades ranging in theory from 2 to 10. This understandably leads some patients to think that their cancer on biopsy is in the middle of the grade scale. This can compound their worry about their diagnosis and make them more likely to feel that they need to be treated right away.
Another problem with the Gleason grading system is that the Gleason scores are often divided into only 3 groups . This is not accurate, since Gleason score 7 is made up of two grades , with the latter having a much worse prognosis. Similarly, Gleason scores of 9 or 10 have a worse prognosis than Gleason score 8.
To account for these differences, the Grade Groups range from 1 to 5 :
- Grade Group 1 = Gleason 6
- Grade Group 2 = Gleason 3+4=7
- Grade Group 3 = Gleason 4+3=7
- Grade Group 4 = Gleason 8
- Grade Group 5 = Gleason 9-10
Although eventually the Grade Group system may replace the Gleason system, the two systems are currently reported side-by-side.
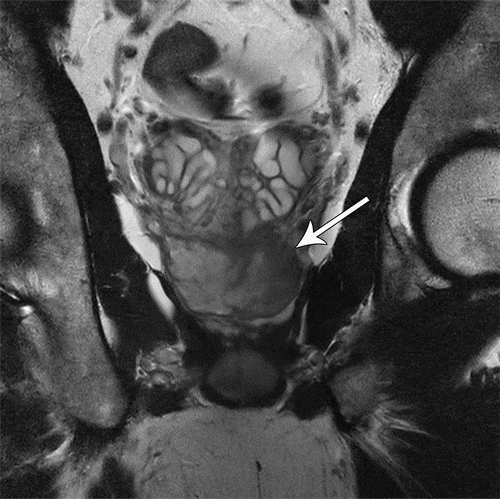
Detection Of Extraprostatic Disease And Seminal Vesicle Invasion In Patients Undergoing Magnetic Resonance Imaging

Erin M. Baumgartner1, Kristin K. Porter2, Jeffrey W. Nix3, Soroush Rais-Bahrami2,3, Jennifer B. Gordetsky1,2
1 University of Alabama at Birmingham , , USA
Contributions: Conception and design: S Rais-Bahrami, JB Gordetsky Administrative support: JW Nix Provision of study materials or patients: JB Gordetsky Collection and assembly of data: JB Gordetsky, EM Baumgartner Data analysis and interpretation: JB Gordetsky, EM Baumgartner Manuscript writing: All authors Final approval of manuscript: All authors.
Correspondence to:
Background: Finding incidental extraprostatic extension or seminal vesicle invasion by prostate cancer is rare on standard prostate biopsy. We evaluated the clinical-pathologic features associated with EPE and SVI on multiparametric magnetic resonance imaging /ultrasound fusion-guided targeted biopsy .
Methods: A retrospective review was performed from 20142017, selecting patients who had undergone TB. Clinical, pathologic, and radiologic features were evaluated.
Based on our small series, we hypothesize that MRI/US fusion TB outperforms SB in the identification of EPE and SVI. However, given the small sample size and the overall rarity of these pathologic findings on prostate biopsy, further validation is needed.
Keywords: Prostate cancer cancer staging cancer grading multiparametric magnetic resonance imaging
Submitted Jan 10, 2018. Accepted for publication Mar 09, 2018.
doi: 10.21037/tau.2018.03.15
Read Also: What Age Do You Start Screening For Prostate Cancer
What Is Prostate Cancer
Prostate cancer develops in the prostate, a small gland that makes seminal fluid. It is one of the most common types of cancer in men. Prostate cancer usually grows over time and in the beginning, typically stays within the prostate gland, where it may not cause serious harm. While some types of prostate cancer grow slowly and may need only a minimal amount of treatment or no treatment at all, other types are aggressive and can spread quickly.
When prostate cancer is caught early, a person has a better chance of treating it successfully.
Radiation Therapy And Radiopharmaceutical Therapy
External-beam radiation therapy
Candidates for definitive radiation therapy must have a confirmed pathologic diagnosis of cancer that is clinically confined to the prostate and/or surrounding tissues . Staging laparotomy and lymph node dissection are not required.
Radiation therapy may be a good option for patients who are considered poor medical candidates for radical prostatectomy. These patients can be treated with an acceptably low complication rate if care is given to the delivery technique.
Long-term results with radiation therapy are dependent on stage and are associated with dosimetry of the radiation.
Evidence :
Evidence :
Brachytherapy
Also Check: What Is Blood Test For Prostate Cancer
Seminal Vesicle Invasion: What Is The Best Adjuvant Treatment After Radical Prostatectomy
Cyrille Bastide
Level of Evidence2b
Whats known on the subject? and What does the study add?
Seminal vesicle invasion in prostate cancer has a poor prognosis. Nowadays, there is no consensus about the best adjuvant treatment after radical prostatectomy when seminal vesicle invasion is observed in the specimen.
To our knowledge, this is the first comparative study between different adjuvant treatments after radical prostatectomy when seminal vesicle invasion is observed in the specimen.
