How Does Brachytherapy Work
Brachytherapy involves implanting small, permanent radioactive seeds or temporary needles into the cancerous prostate.
After you are identified as a good candidate for brachytherapy, an ultrasound is used to guide the placement of needles into the prostate. Depending on whether you and your doctor have chosen permanent/low-dose brachytherapy or temporary/high-dose brachytherapy, these needles are then used to either put in permanent seeds or temporary radiation sources.
Placement of seeds is a minimally invasive procedure and does not require incisions. Men undergoing the procedure can return to full activity in less than a week. This is done as an outpatient procedure before you begin treatment.
Side Effects During Treatment
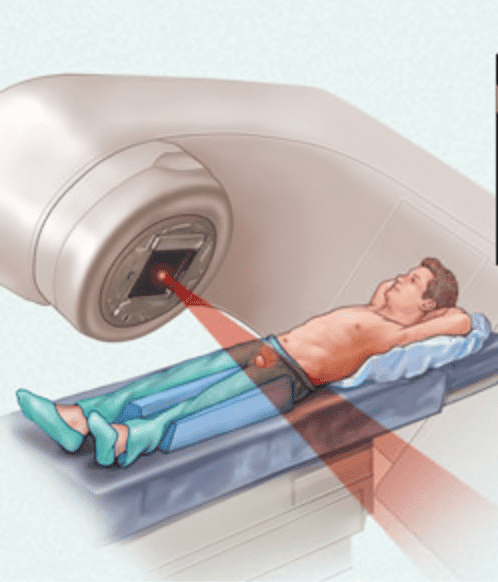
Undergoing EBRT is similar to having routine X-rays and no more uncomfortable. Radiation cannot be seen, smelled, or felt. Patients are usually able to continue with their normal daily activities during treatment. But many do experience side effects. If you’re having conventional radiation treatments, side effects generally don’t appear until the second or third week. They may show up earlier if you’re having prostate SBRT, LDR, or HDR brachytherapy.
Because radiation therapy is a local treatment, any side effects will primarily involve the area where the radiation is directed. With prostate cancer, patients may experience some or all of the following:
- Increased urination frequency
- Urinary urgency with rare leakage
- Weak urinary stream
- Mild burning or tingling during urination
- Loose stools or diarrhea
- Softer and smaller bowel movements
- Increased frequency of bowel movements
- Worsening of existing hemorrhoids or rectal irritation with occasional scant blood
- Generalized fatigue of varying severity
Despite the fatigue, patients receiving radiation therapy usually find they can function and work as usual. Many studies show that regular exercise during the course of radiation therapy can ease side effects, including fatigue.
Toxicity Of Conventional Two
Over 1000 patients treated on RTOG trials 7506 and 7706 were followed for a minimum of 7 years and had a reported incidence of at least grade 3 bowel complications of 3.3% and a reported incidence of grade 3 or greater urinary complications in 7.7% of patients. These trials established 70 Gy as the maximal tolerable dose prior to the advent of conformal planning techniques
Also Check: How To Milk A Man’s Prostate
Single Dose Of Targeted Radiotherapy Is Safe And Effective For Prostate Cancer
- Date:
- European Society for Radiotherapy and Oncology
- Summary:
- A single high dose of radiation that can be delivered directly to the tumor within a few minutes is a safe and effective technique for treating men with low-risk prostate cancer.
A single high dose of radiation that can be delivered directly to the tumour within a few minutes is a safe and effective technique for treating men with low risk prostate cancer, according to a study presented at the ESTRO 38 conference.
Radiotherapy traditionally involves a series of lower dose treatments that take place over several days or week. The new treatment is called high dose-rate brachytherapy and it delivers radiation via a set of tiny tubes.
Researchers say this technique could offer an effective treatment that is convenient for patients and brings potential time and cost savings for hospitals.
The research was presented by Dr Hannah Tharmalingam, a Clinical Research Fellow at Mount Vernon Cancer Centre, Northwood, and The Christie NHS Foundation Trust, Manchester, UK.
The research included 441 men with prostate cancer who were treated at one of seven UK hospitals between 2013 and 2018. Their cancers were classified, depending on how likely they were to spread, as either low risk , medium risk or high risk . All were treated with a single high dose of radiation 166 men also received hormone therapy but none had any surgery or chemotherapy.
Story Source:
Eight Types Of Standard Treatment Are Used:
Watchful waiting or active surveillance
Watchful waiting and active surveillance are treatments used for older men who do not have signs or symptoms or have other medical conditions and for men whose prostate cancer is found during a screening test.
Watchful waiting is closely monitoring a patients condition without giving any treatment until signs or symptoms appear or change. Treatment is given to relieve symptoms and improve quality of life.
Active surveillance is closely following a patient’s condition without giving any treatment unless there are changes in test results. It is used to find early signs that the condition is getting worse. In active surveillance, patients are given certain exams and tests, including digital rectal exam, PSA test, transrectal ultrasound, and transrectal needle biopsy, to check if the cancer is growing. When the cancer begins to grow, treatment is given to cure the cancer.
Other terms that are used to describe not giving treatment to cure prostate cancer right after diagnosis are observation, watch and wait, and expectant management.
Surgery
Patients in good health whose tumor is in the prostategland only may be treated with surgery to remove the tumor. The following types of surgery are used:
You May Like: Effects Of Lupron For Prostate Cancer
Pretreatment Evaluation Of Patients With Intermediate
In addition to routine history and physical examination, including a digital rectal examination, serum PSA, and serum testosterone, radiographical imaging of the abdomen and pelvis using computed tomography or magnetic resonance imaging should be obtained to assist in the evaluation of the extent of primary disease. Although the likelihood of bone metastases is low in men with intermediate-risk prostate cancer, bone scan may be appropriate for patients in whom there is high suspicion for metastatic disease based on laboratory, imaging, or clinical findings .
While CT imaging of the pelvis is the current standard, T2 MRI is superior to CT as it provides adequate soft tissue resolution to delineate the anatomy of the prostate, seminal vesicles, neurovascular bundles, and pelvic floor. MRI offers the ability to detect disease within and adjacent to the prostate gland that is not as easily visualized on CT . MRI, if obtained, can be fused to treatment planning CTs, allowing improved accuracy in contour definition of target and normal tissue volumes . This may result in improved clinical outcomes by decreasing normal tissue toxicity . MRI and magnetic resonance spectroscopy may have a role in the evaluation of tumor response to external beam radiation therapy and prostate brachytherapy .
What To Expect After Treatment
Most side effects lessen significantly in the first 3-4 weeks but you may experience urinary and bowel side effects for several weeks after you complete your EBRT treatment. Full recovery however takes three to six months and some patients may never recover to their baseline urinary and bowel function and may need to continue taking medications prescribed during treatment. Rare patients report continued but lessening fatigue for several weeks or months after treatment ends. The better the urinary and bowel functions are prior to radiation, the more likely full recovery occurs.
After both LDR and HDR brachytherapy, you may experience the following:
- burning with urination
- increased urination frequency
- slow or weak urinary stream
- incomplete emptying of the bladder
- a brief period of blood in urine
- perineal pain or soreness
You May Like: What Is A High Psa Level For Prostate
Possible Risks And Side Effects Of Brachytherapy
Radiation precautions: If you get permanent brachytherapy, the seeds will give off small amounts of radiation for several weeks or months. Even though the radiation doesnt travel far, your doctor may advise you to stay away from pregnant women and small children during this time. If you plan on traveling, you might want to get a doctors note regarding your treatment, as low levels of radiation can sometimes be picked up by detection systems at airports.
There’s also a small risk that some of the seeds might move . You may be asked to strain your urine for the first week or so to catch any seeds that might come out. You may be asked to take other precautions as well, such as wearing a condom during sex. Be sure to follow any instructions your doctor gives you. There have also been reports of the seeds moving through the bloodstream to other parts of the body, such as the lungs. As far as doctors can tell, this is uncommon and doesnt seem to cause any ill effects.
These precautions arent needed after HDR brachytherapy, because the radiation doesnt stay in the body after treatment.
Bowel problems: Brachytherapy can sometimes irritate the rectum and cause a condition called radiation proctitis. Bowel problems such as rectal pain, burning, and/or diarrhea can occur, but serious long-term problems are uncommon.
Focal Ablative Salvage Therapy
More recently, there is a growing body of research on focal salvage therapy to target just the identified tumor. This approach is called Focal Ablative Salvage Therapy, or FAST. Thanks to mpMRI and MRI targeted biopsy, the tumors location, extent, aggressiveness and genomics can be identified. Ablating just the tumor offers the dual advantage of cancer control plus low side effect risks. As with whole-gland primary treatment, the same three ablation methods can be used.
As of this writing, the most recent data was presented at the 2022 annual meeting of the American Urological Association by Dr. Deepika Reddy . The statistics were drawn from 288 consecutive cases of radiation recurrence that were treated with either focal HIFU or focal cryo . According to Dr. Reddys presentation, 265 patients had pertinent follow-up records for analysis. Patients had either stage T2 or T3 disease, and Grade Group 2, 3 or > 3.
Treatment was deemed successful based on failure-free survival and retreatment-free survival . The numbers are very encouraging, with 77% success rates for both FFS and RFS at 6 years post-FAST. About 7% of patients had adverse events following ablation, most of which were urinary infections. These patients avoided the surgical trauma of salvage prostatectomy, the increased cancer risk of salvage radiation, and the likely side effects of both.
Also Check: Red Meat And Prostate Cancer
The Grade Group And Psa Level Are Used To Stage Prostate Cancer
The stage of the cancer is based on the results of the staging and diagnostic tests, including the prostate-specific antigen test and the Grade Group. The tissue samples removed during the biopsy are used to find out the Gleason score. The Gleason score ranges from 2 to 10 and describes how different the cancer cells look from normal cells under a microscope and how likely it is that the tumor will spread. The lower the number, the more cancer cells look like normal cells and are likely to grow and spread slowly.
The Grade Group depends on the Gleason score. See the General Information section for more information about the Gleason score.
- Grade Group 1 is a Gleason score of 6 or less.
- Grade Group 2 or 3 is a Gleason score of 7.
- Grade Group 4 is a Gleason score 8.
- Grade Group 5 is a Gleason score of 9 or 10.
The PSA test measures the level of PSA in the blood. PSA is a substance made by the prostate that may be found in an increased amount in the blood of men who have prostate cancer.
Radiation Therapy Oncology Group 94
This multi-institutional study was conducted to evaluate the effect of the addition of AST to RT on overall survival, freedom from biochemical failure, freedom from clinical progression, and disease-free survival in patients with localized prostate cancer in response to the positive effect on these parameters seen in RTOG 86-10. To this end, 1979 patients with T1bT2b prostate cancer and PSA less than 20 ng/ml were randomized to receive EBRT alone or in conjunction with 2 months of neoadjuvant and 2 months of concurrent goserelin and flutamide.
Also Check: How Long To Cure Prostatitis
What Should Patients Know About Msks Approach To Treating Prostate Cancer
At MSK, we manage prostate cancer in a very comprehensive way, tailored to each patients disease. There is no one specific therapy that is best for everyone.
Our initial assessment includes a carefully evaluated biopsy and a very detailed MRI to show the location of the disease, the integrity or soundness of the capsule surrounding the prostate, and the amount of disease. We will often obtain next-generation imaging and do genomic testing. Then, based on that information and with input from the urologist, the radiation oncologist, and the medical oncologist we can provide a comprehensive recommendation.
The radiotherapy we do here at MSK is state-of-the-art and unparalleled. We are one of the few centers in the world to do MRI-based treatment planning and one of the few centers in the US to offer MRI-guided treatment. When we give brachytherapy, we use computer software that provides us with real-time information about the quality and accuracy of the seed implant during the procedure. It requires a great deal of collaboration with our medical physics team to try to get the most accurate positioning of the prostate during the actual three or four minutes of the treatment.
We make adjustments while the patient is still under anesthesia, so that when the procedure is completed, we have been able to achieve ideal placement of the radiation seeds. This translates into improved outcomes.
There Are Different Types Of Treatment For Patients With Prostate Cancer
Different types of treatment are available for patients withprostate cancer. Some treatments are standard , and some are being tested in clinical trials. A treatment clinical trial is a research study meant to help improve current treatments or obtain information on new treatments for patients with cancer. When clinical trials show that a new treatment is better than the standard treatment, the new treatment may become the standard treatment. Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
You May Like: Roto Rooter Surgery For Prostate
Treatment By Stage Of Prostate Cancer
Different treatments may be recommended for each stage of prostate cancer. Your doctor will work with you to develop a specific treatment plan based on the cancers stage and other factors. Detailed descriptions of each type of treatment are provided earlier on this same page. Clinical trials may also be a treatment option for each stage.
Early-stage prostate cancer
Early-stage prostate cancer usually grows very slowly and may take years to cause any symptoms or other health problems, if it ever does at all. As a result, active surveillance or watchful waiting may be recommended. Radiation therapy or surgery may also be suggested, as well as treatment in clinical trials. For those with a higher Gleason score, the cancer may be faster growing, so radical prostatectomy and radiation therapy are often recommended. Your doctor will consider your age and general health before recommending a treatment plan.
ASCO, the American Urological Association, American Society of Radiation Oncology, and the Society of Urologic Oncology recommend that patients with high-risk early-stage prostate cancer that has not spread to other areas of the body should receive radical prostatectomy or radiation therapy with hormonal therapy as standard treatment options.
Locally advanced prostate cancer
Watchful waiting may be considered for older adults who are not expected to live for a long time and whose cancer is not causing symptoms or for those who have another, more serious illness.
Active Surveillance And Watchful Waiting
If prostate cancer is in an early stage, is growing slowly, and treating the cancer would cause more problems than the disease itself, a doctor may recommend active surveillance or watchful waiting.
Active surveillance. Prostate cancer treatments may seriously affect a person’s quality of life. These treatments can cause side effects, such as erectile dysfunction, which is when someone is unable to get and maintain an erection, and incontinence, which is when a person cannot control their urine flow or bowel function. In addition, many prostate cancers grow slowly and cause no symptoms or problems. For this reason, many people may consider delaying cancer treatment rather than starting treatment right away. This is called active surveillance. During active surveillance, the cancer is closely monitored for signs that it is worsening. If the cancer is found to be worsening, treatment will begin.
ASCO encourages the following testing schedule for active surveillance:
-
A PSA test every 3 to 6 months
-
A DRE at least once every year
-
Another prostate biopsy within 6 to 12 months, then a biopsy at least every 2 to 5 years
Treatment should begin if the results of the tests done during active surveillance show signs of the cancer becoming more aggressive or spreading, if the cancer causes pain, or if the cancer blocks the urinary tract.
Read Also: Does A Cystoscopy Look At The Prostate
Side Effects Of Ebrt For Prostate Cancer
Many of the possible side effects of radiation therapy for prostate cancer involve the bladder and bowelthe prostate is very close to both. Although the goal is to target only the prostate with radiation, sometimes small amounts may cause problems to nearby areas of the body.
Some of the potential side effects from EBRT include:
- Bowel problems, including diarrhea, leakage or rectal bleeding
- Urinary symptoms, such as a need to urinate more frequently, incontinence or a burning sensation during urination
When Is Brachytherapy Alone The Right Choice
For some patients with disease that is confined to the prostate and not too aggressive , brachytherapy alone is a good option. It is also convenient for the patient as it is done in an outpatient setting and most people can get back to work within a few days.
But brachytherapy is not right for everyone. For some patients with less-aggressive disease, a watch-and-wait approach would be preferred. At MSK, our philosophy is that when the disease is caught very early, it is very appropriate to do active surveillance and hold off on treatment.
This philosophy applies to patients with a low PSA level, or nonaggressive disease as reflected by a Gleason score of 6 with evidence of cancer in only a few of the biopsy samples and no evidence from the MRI of a significant amount of disease. There are also very select patients with Gleason 7 disease who may be candidates for active surveillance.
Read Also: How To Do A Prostate Exam
