Does Msk Offer Proton Therapy For Prostate Cancer
Some men with prostate cancer may choose to receive another form of external-beam radiation therapy called proton therapy. Proton therapy can deliver a high radiation dose to the prostate while lowering the radiation dose to normal surrounding tissue. It is unclear if there is any advantage to proton therapy compared with IMRT. We are now studying how these approaches compare in terms of side effects and outcomes at the New York Proton Center. These efforts are being led by radiation oncologist Daniel Gorovets.
Potential Advantages And Disadvantages Of Pt
The potential advantages and disadvantages of PT result from its dosimetric features. Protons travel only a finite distance, proportional to their speed, which can be controlled during the acceleration process they deposit most of their energy at the end of their range in an area called the âBragg peakâ and, unlike photon-based radiation, there is no exit dose beyond the target. Additionally, the entrance dose is relatively low when compared to external-beam photon radiation. For many target locations, these features reduce the excess radiation dose delivered to surrounding organs and the number of beams needed to treat a target when compared to photon radiation . Multiple dosimetric comparisons have been performed evaluating the extent of the dosimetric improvements that PT offers for prostate cancer and, in general, they have shown that PT reduces the dose of excess radiation provided to OARs in the low-to-moderate range .
Figure 1
Nichols et al. retrospectively reviewed the medical records of 171 men treated with PT for localized prostate cancer and found that PT does not affect serum testosterone levels. PT provides less excess radiation dose to the testes when compared to photon-based radiation. Consequently, while photon-based radiation lowers testosterone by 9% to 27% on average, patients treated with PT can expect no changes in testosterone, which may reduce the risk for fatigue or sexual dysfunction after treatment .
How Proton Beam Therapy Works
Proton therapy is an advanced form of radiation treatment that uses protons instead of X-rays.
In regular radiation therapy, the beam of energy goes into the body, through the tumor, and out the other side. This exit dose of radiation might affect healthy tissue beyond the tumor. Protons, in contrast, are larger particles than those used in regular radiation. They release more of their energy within the tumor itself. This burst of energy can appear on a graph as what is called the Bragg peak.
After delivering the energy to the tumor, the protons stop: They do not exit the tumor and go into healthy tissue on the other side.
In this way, proton therapy reduces radiation exposure and potential damage to healthy tissue, especially in sensitive areas such as the brain, eyes, spinal cord, heart, major blood vessels and nerves.
Read Also: Effects Of Having Prostate Removed
You May Like: Does Enlarged Prostate Cause Pain When Sitting
Uf Health Proton Therapy Cancer Experts
As a major non-profit academic medical center, the University of Florida Health Proton Therapy Institute has treated more than 10,000 patients and led the way for innovative cancer care in the Southeast U.S. since 2006. As an academic health center, our published research is setting the standards for proton therapy cancer care worldwide, with dozens of clinical trials and more than 300 published research articles in peer-reviewed journals.
When you become a patient at UF Health Proton Therapy Institute, you are assured of receiving the highest quality cancer care as measured by state and national standards. We are committed to delivering the best possible patient outcomes. Our 125+ employees are dedicated to delivering proton cancer treatment in a way that takes the entire patient into account, so you can keep living life to the fullest.
1 Bryant C, Smith TL, Henderson RH, Hoppe BS, Mendenhall WM, Nichols RC, Morris CG, Williams CR, Su Z, Li Z, Lee D, Mendenhall NP. Five-Year Biochemical Results, Toxicity, and Patient-Reported Quality of Life Following Delivery of Dose- Escalated Image-Guided Proton Therapy for Prostate Cancer. International Journal of Radiation, Oncology, Biology, Physics. 2016 95:435-43.
Are you a candidate for Proton Therapy?
Do We Know Which Treatment Is Best For Prostate Cancer Brachytherapy Or External Beam Radiation
Its not a question of which type of radiation therapy is best in general, but rather which therapy is best for the patients specific disease and quality-of-life concerns. We want to use the most tailored, pinpointed radiation to treat the prostate tumor effectively while minimizing side effects. This can depend on the tumors size and stage as well as other patient characteristics and even a patients individual preferences.
Read Also: What Is Prostate Cancer In Hindi
How Proton Therapy Effectively Treats Prostate Cancer
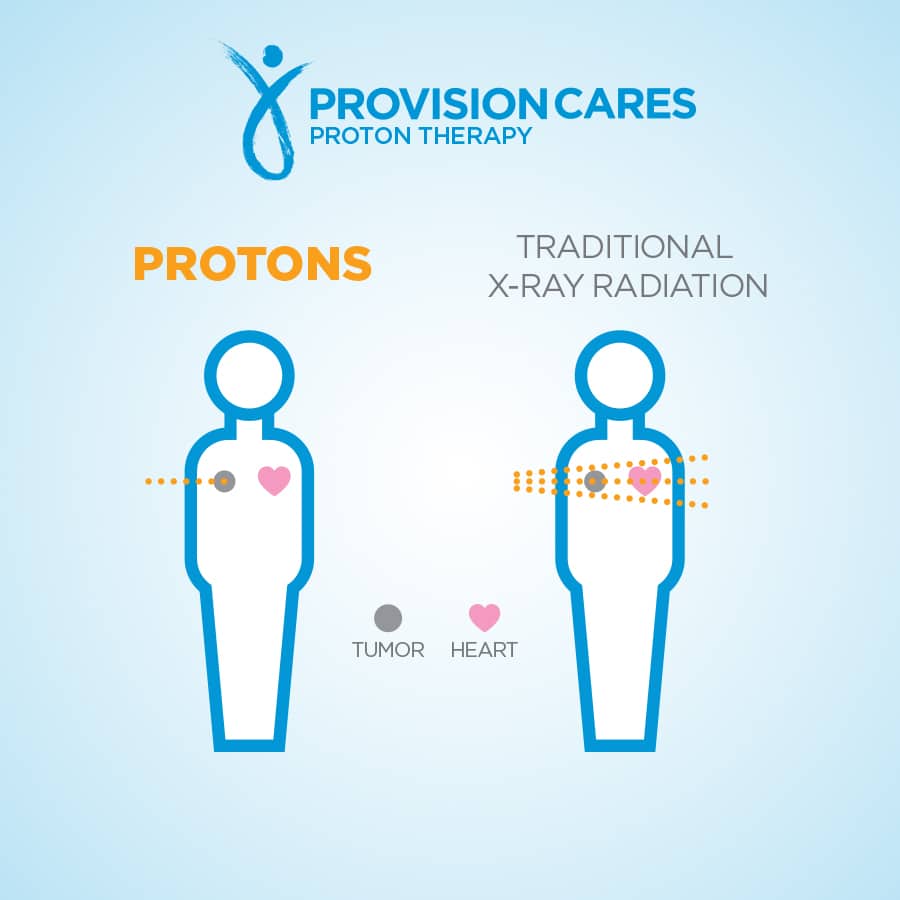
Proton therapy treats prostate cancer with high doses of radiation that are more accurate, and potentially more effective, than traditional radiation. Our targeted proton beams focus most of their destructive energy at the tumor site, therefore causing less damage to healthy surrounding tissue as they enter the body. Because of this, proton therapy patients dont have to worry about many of the side effects and additional healthy tissue damage that is commonly associated with X-ray therapy.
an effective cancer treatment alternative
Possible Side Effects Of Ebrt
Some of the side effects from EBRT are the same as those from surgery, while others are different.
Bowel problems: Radiation can irritate the rectum and cause a condition called radiation proctitis. This can lead to diarrhea, sometimes with blood in the stool, and rectal leakage. Most of these problems go away over time, but in rare cases normal bowel function does not return. To help lessen bowel problems, you may be told to follow a special diet during radiation therapy to help limit bowel movement during treatment. Sometimes a balloon-like device or gel is put between the rectum and the prostate before treatment to act like a spacer to lessen the amount of radiation that reaches the rectum.
Urinary problems: Radiation can irritate the bladder and lead to a condition called radiation cystitis. You might need to urinate more often, have a burning sensation while you urinate, and/or find blood in your urine. Urinary problems usually improve over time, but in some men they never go away.
Some men develop urinary incontinence after treatment, which means they cant control their urine or have leakage or dribbling. As described in the surgery section, there are different levels and types of incontinence. Overall, this side effect occurs less often with radiation therapy than after surgery. The risk is low at first, but it goes up each year for several years after treatment.
Also Check: Where Is The Prostate Located In A Man
Don’t Miss: Herbal Treatment For Prostate Cancer
Understanding Individual Cure Rate
An Individual Cure Rate is the percentage that represents the likelihood of curing your prostate cancer based on our definition of cure. We define cure as having a PSA level of 0.2 ng/ml 10 years after treatment and remaining at that level consistently. Your ICR is based solely on your prostate cancer situation and is completely unique to you.
Example of an Individual Cure Rate probability produced for a man based on his cancer characteristics. Treated with ProstRcision, this mans 15-year chance of zero PSA is 85%.
Whos A Good Candidate For This Procedure
Anyone who can have radiation therapy can have proton therapy. Proton therapy can be used as primary treatment for early stage prostate cancer or as part of a total treatment plan for prostate cancer. Its also an effective treatment for people who require pelvic radiation therapy after undergoing previous therapies.
Recommended Reading: Are There Any Symptoms Of Prostate Cancer
Better Quality Of Life
Proton therapy for prostate cancer improves quality of life during and after treatment.
Men who chose proton therapy for prostate cancer reported significantly better quality of life than those who chose other treatment options. A national survey profiled 755 men at least 12 months after prostate cancer treatment.
Patients who received proton therapy reported the best outcomes for overall quality of life, urinary function, sexual function, ability to remain active during treatment, and living life the way they wanted to after treatment.
My treatment did not interfere with my quality of life.
Why Choose Us For Prostate Cancer Care
- Prostate cancer specialists: Because our team is subspecialized in prostate cancer, you get the most comprehensive, most personalized care plan available.
- Unparalleled in proton therapy: We’ve treated over 10,000 prostate cancer patients using proton therapy more than any other center in the world.
- Leaders in robotic surgery: Our surgeons perform more minimally-invasive robotic surgeries each year than those at any other teaching hospital in the West.
- State-of-the-art tech: As the largest urology group in the region, we offer you access to the most advanced technology available.
- Clinical trials: You have access to many clinical trials for prostate cancer, which may offer potential new treatments.
You May Like: Different Types Of Radiation For Prostate Cancer
Lower Risk Of Side Effects
Clinical research shows that proton therapy for prostate cancer lowers the risk of side effects and improves overall survival rates.
- 5% increase in Overall Survival Rate for intermediate risk prostate cancer20
- 21% decrease in risk of urinary toxicity24
- 25% decrease in risk of erectile dysfunction24
- 35% decrease in radiation to the bladder22
- 42% decrease in relative risk of developing a secondary malignancy20
- 50% decrease in treatment-related bowel frequency and urgency23
- 59% decrease in radiation to the rectum22
Protons: A Different Mechanism
Protons can also be administered by two methods. The older method includes large beams of passively scattered protons that are shaped with the use of high-density blocks or apertures to shape the large beam as it exits the nozzle. Compensators are employed within the beam to alter the beam profile to better conform the SOBP to the actual tumor. A second, newer method employs a very narrow, pencil thin beam to paint the dose on the target, and no blocks or compensators are needed. The pencil beam is swept in a raster pattern back and forth across a target guided out of the nozzle by magnets . This allows the delivery of intensity-modulated proton beam therapy , with a greater ability to conform the dose to an irregularly shaped target. Although not widely available, many new facilities are being planned with pencil beam-only systems.
Pencil beam scanning. The pencil beam is swept in a raster pattern back and forth across a target. Reproduced with permission from Mayo Clinic News Network.
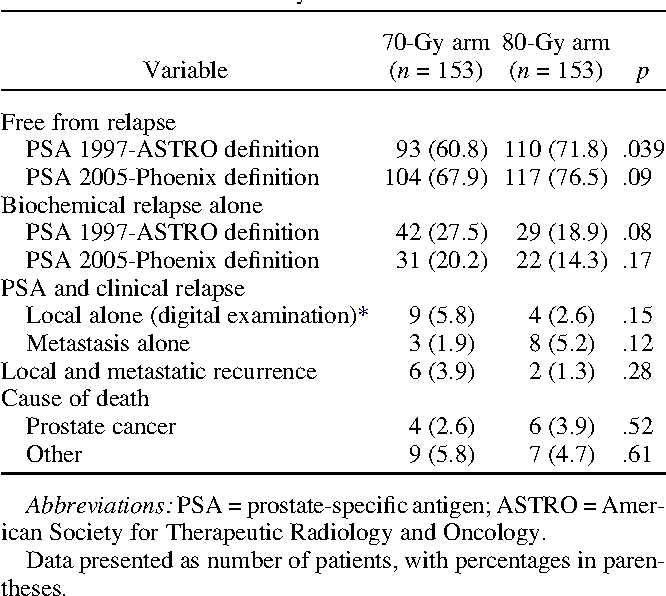
aAs determined by Phoenix criteria. bAs determined by American Society for Therapeutic Radiology Oncology criteria. c Determined by a rise in prostate-specific antigen to > 50% than the nadir and > 2 ng/mL.
2D, two-dimensional 3D, three-dimensional GI, gastrointestinal GU, genitourinary HD, high dose IMRT, intensity-modulated radiation therapy LD, low dose.
Also Check: How Do They Check Prostate
How Proton Therapy Works
Proton therapy can treat prostate cancer precisely while lowering the risk for side effects during and after treatment.
Proton therapy uses charged particles rather than x-rays to destroy cancer cells. Protons can be focused directly on the tumor and stop at that target in the body. With extreme accuracy, proton therapy results in excellent rates of cancer control with a lower risk for side effects than other forms of radiation therapy.
The controlled delivery and dosage of proton energy allows direct, customized targeting of the tumor, for the maximum prescribed dosage of radiation. These characteristics of proton therapy can benefit the patient:
- Improved quality of life, during and after treatment, from greater precision in treating the tumor.
- Lower risk of side effects and impact to bodily functions, as unnecessary radiation to nearby healthy tissue and vital organs is prevented.
- Cancer in critical areas or close to organs and structures that could be damaged by radiation can be safely targeted and treated.
- Patients with cancer recurrence, who have previously been treated with radiation can often safely and effectively be retreated with proton therapy to achieve local control.
The physical properties of protons, described by the Bragg-Peak , and the increased conformality of pencil beam scanning to conform to the exact shape of the cancer, make it possible to spare healthy surrounding organs from exposure to unnecessary radiation.
Limitations Of The Studys Design
The study leaders and other experts noted several limitations to the studys design.
For instance, this observational study cant establish a cause-and-effect relationship between proton therapy and fewer side effects. In addition, all of the study participants were treated at a single institution, which can make it difficult to generalize the findings to a larger population.
Those are very significant limitations that shouldnt be understated, Dr. Buchsbaum emphasized.
Although single-institution studies have inherent limitations, Dr. Baumann noted, all patients in this study received high-quality treatment at a large academic medical center, regardless of whether it was proton or traditional radiation therapy, which suggests that the benefit of proton therapy that we saw is meaningful.
Also, because patients were not randomly assigned to treatment groups, there were differences between patients who got proton and traditional radiation, and that may have skewed the results.
For instance, patients who received proton therapy were, on average, older and had more health issues.
The proton therapy group may also have included more patients from privileged backgrounds, Drs. Park and Yu noted. Socioeconomic status and social support can affect treatment outcomes, they wrote.
In addition, fewer people with head and neck cancerwho are more likely to suffer from radiation-associated side effectswere included in the proton therapy group, the editorialists added.
Don’t Miss: What Age Do You Get Prostate Cancer
Surgery For Prostate Cancer
A radical prostatectomy is the surgical removal of the prostate. This procedure may be performed through traditional open surgery, which involves one large incision in the abdomen. Laparoscopic surgery using the robotic daVinci® Surgical System is a minimally invasive alternative. Robotic surgery only requires a few small incisions in the abdomen, which may result in reduced pain, lower risk of infection and a shorter hospital stay after surgery.
The technology associated with the robotic surgical system is designed to give the surgeon greater precision and control, which may help spare healthy tissue and one or two of the nerve bundles on the sides of the prostate. This often allows the patient to have better erectile functionin both the short term and long term.
Recommended Reading: Psa Levels And Prostate Cancer
Communicate With Your Doctor
The most critical recommendation to reduce your risk is to keep in communication with your doctor. Your case is different from any other, and you deserve personalized treatment. These recommendations should adapt to your case, too. Thus, talk to your doctor and follow recommendations. If your doctor considers it appropriate to screen with PSA testing, talk about the pros and cons with him. And if you need treatment, discuss the benefits and drawbacks of your treatment options. Ask questions and inform yourself about prostate cancer and what to do about it.
You May Like: How To Get Rid Of Prostate Cancer
How Is Yale Medicines Approach Unique
âAt Yale Medicine, we take a number of approaches that set our care apart,â says Dr. Yu. âFirst, we have a large physics staff that is essential to designing and verifying our radiation treatment plans. Second, we make it a point to evaluate new radiation technologies critically. We dont hold onto old approaches, but neither do we jump on the latest trends without seriously assessing what they will contribute.â
Third, adds Dr. Yu, we are running a growing prostate cancer research program and Yale Medicine is home to leading voices in urology, medical oncology and radiation oncology. âWere also on the forefront of MRI-guided prostate biopsy,â he says, âand, our bedrock is Yales multidisciplinary prostate cancer program, which brings together multiple insights collaboratively.â
Entrance And Exit Dose Defined
Entrance dose: The dose of radiation that inadvertently makes contact with normal cells before it reaches the cancerous tissue.
Exit dose: Imagine the radiation hitting the tumor, but then continuing on beyond it, taking out normal cells in its path.
The primary difference between proton therapy and Cyberknife is that protons do not have an exit dose, says Dr. Cavanaugh. Both modalities deliver entrance and target dose.
Many insurers have been unimpressed with the differences in outcomes with proton therapy and have declined to pay.
For many patients I prefer HDR brachytherapy to both proton and Cyberknife therapy. HDR stands for high dose rate.
Dont Miss: How Long Does It Take For Prostate Cancer To Spread
Recommended Reading: Does A Prostate Biopsy Damage The Prostate
Current & Evolving Evidence
Improvements in targeting and dose delivery have led to improved disease control rates for patients receiving photon- or proton-based treatment. However, differences among patient characteristics, treatment techniques, and outcome measures have made it difficult to directly compare safety and efficacy endpoints across published studies. Both modern photon- and proton-based treatments have been shown to be effective with a well-defined toxicity profile, but it is not clear if one modality is superior to the other. Existing systematic reviews and the available data summarized above suggest similar tumor control with no clear benefit in terms of late effects and a suggestion that protons may be associated with higher incidence of late bowel toxicity.
External Beam Radiation For Prostate Cancer
When most patients think of radiation therapy, they think of external beam radiation therapy , in which a beam of radiation is directed at cancerous tissue from outside the body. Technological advances, such as intensity-modulated radiation therapy and image-guided radiation therapy , allow radiation oncologists to use computer-controlled devices and image-guidance technology to see and target a three-dimensional image of the tumor, making the treatment more precise than ever before.
EBRT used to require 40-45 daily treatments. Now, 25-28 treatments are the norm. This type of protracted, fractionated radiation therapy, however, is now generally considered to be less appropriate for low-risk and favorable intermediate-risk patients. Instead, hypofractionated techniques and brachytherapy techniques are generally more advisable for many patients.
Donât Miss: Can You Be Asleep During A Prostate Biopsy
Read Also: What Is The Prostate Used For
