Discovery Shows How Difficult
Study reports pre-clinical development of novel treatment andpotential for combination use with immunotherapy drugs
MD Anderson News ReleaseJuly 18, 2019
Researchers at The University of Texas MD Anderson Cancer Center have discovered how an aggressive form of prostate cancer called double-negative prostate cancer metastasizes by evading the immune system. The investigators also reported on the pre-clinical development of a new therapy, which, when given in combination with existing immunotherapies, appears to stop and even reverse metastasis in mouse models.
DNPC is difficult to treat and frequently arises in patients previously treated with therapies that inhibit androgen receptors , known to spur prostate cancer cells growth. Study findings were published in the July 18 online issue of Cancer Cell.
Filippo Giancotti, M.D., Ph.D., professor of Cancer Biology, reported that an epigenetic regulator known as the polycomb repressor complex 1 coordinates the initiation of metastasis by increasing the regenerative capacity of metastatic cells and by suppressing the immune system and spurring tumor blood vessel growth or angiogenesis.
Through in vivo genetic screening, the team identified a cytokine called CCL2 as the major pro-metastatic gene induced by PRC1. CCL2 binds to a tumor cell receptor called CCR4 to boost regenerative capacity and to CCR2 in immune cells, creating an immunosuppressive microenvironment and boosting tumor blood vessel growth.
Common Prostate Cancer Treatments Suppress Immune Response May Promote Relapse
- Date:
- UT Southwestern Medical Center
- Summary:
- Prostate cancer patients and their doctors may want to think twice about the best timing for chemotherapy or radiation therapy in conjunction with a common nonsurgical treatment, based on international research findings.
Prostate cancer patients and their doctors may want to think twice about the best timing for chemotherapy or radiation therapy in conjunction with a common nonsurgical treatment, based on international research findings led by UT Southwestern Medical Center investigators.
Researchers using mouse models found that many medical androgen deprivation therapies — the most commonly used nonsurgical treatments for prostate cancer — may suppress patients’ adaptive immune responses, preventing immunotherapies from working if both treatments are used but not sequenced properly. ADTs are anti-hormone therapies that decrease the body’s levels of androgens, the type of hormone that is required for prostate cancer to survive and grow.
The study findings were published this week in Science Translational Medicine.
“Medical ADTs have been used for a half century to treat prostate cancer, and promising clinical results for cancer immunotherapy have led to attempts to combine it and other standard-of-care therapies with immunotherapy to treat the disease,” said senior author and principal investigator Dr. Yang-Xin Fu, Professor of Pathology and Immunology.
Relapse of prostate tumors, however, has been a major problem.
Will My Regular Psa Tests Still Happen
Where possible, GP surgeries and hospitals are continuing to provide routine tests as normal. If you usually have blood tests at your GP surgery, you may be asked to wait outside . This is so that you dont have to wait with other patients or spend very long inside the building. If you have coronavirus symptoms, youll need to delay your blood test while you follow the latest government guidance on self-isolating at home.
In some areas, a nurse may be able to visit you at home to do blood tests if you are concerned, ask your GP surgery if this is an option. If you usually have regular blood tests at the hospital, you may be able to have these at your GP surgery or at home instead.
One small study of 91 men with Benign Prostatic Hyperplasia has suggested that PSA levels can increase at the point of testing positive for coronavirus infection. PSA may also continue to be raised during the early period after infection. However more research is needed to understand the importance of these changes. If you have concerns about how this might affect your treatment decisions, please talk to your medical team.
Don’t Miss: Is Prostate Cancer Curable In Homeopathy
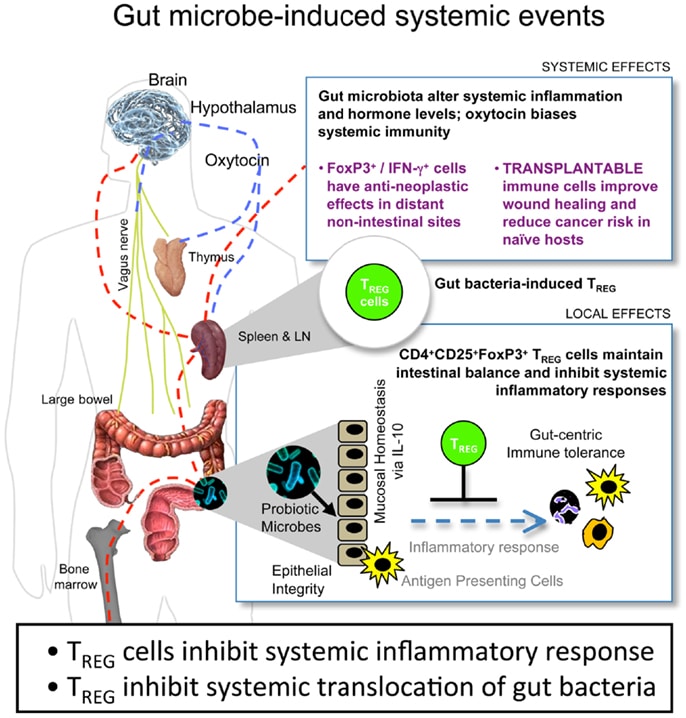
An Immunosuppressive Tumor Microenvironment
Prostate cancer is an immunologically cold tumor . Histopathological evaluation shows an immune-desert, defined as the absence of lymphocytes, or immune-excluded phenotype, where T cells remain trapped in the stroma without penetrating the intraepithelial tumor islets .
For those few patients with TILs infiltrating the TME, the T lymphocytes express mostly an exhausted and terminally differentiated phenotype . In this exhausted phenotype, there is upregulation of negative checkpoints including PD1/PD-L1 , CTLA4, lymphocyte activation gene 3 , T cell immunoglobulin and mucin domain 3 and V-domain Ig suppressor of T cell activation . They display low variability of the T cell receptor , due to reduced clonal differentiation of the TCR beta variable chain, which results in a restricted repertoire of peptide recognition and binding .
The TILs in PCa are unable to be reinvigorated with ICI, likely due to their exhausted and terminally-differentiated state, and due to the high immunological pressure dictated by an immunosuppressive TME which includes regulatory T cells , tumor-associated macrophages , myeloid-derived suppressor cells , and cancer-associated fibroblasts , and they deserve to be described here .
Radiation Volume Impacts Immune Cells
The ratio of CD8+ T cells to Tregs within CD4+ cells at the four timepoints for patients receiving standard vs extended RT. Mean and SEM are shown. Significant differences were detectable in the group treated with extended RT volumes at timepoint C compared to initial CD8+/Treg ratio, as well as between the treatment groups at timepoints C and D. * p < 0.05.
You May Like: Can You Remove Your Prostate
Ive Already Had A Flu Jab Do I Still Need The Covid
The flu jab doesnt protect against coronavirus. To protect yourself against the flu and coronavirus, you need to have both the flu vaccine and the COVID-19 vaccine.
You wont be able to have the flu and COVID-19 vaccines at the same appointment youll need to leave at least a week in-between, to ensure they both work properly.
Cancer Treatments And Blood Counts
While destroying or damaging cancer cells, treatments may also damage healthy blood cells and the bone marrow the body uses to produce new immune cells. And when treatments like chemotherapy and radiation therapy are used together, the combination may lead to conditions that lower blood counts and increase the risk of infection, including:
- Thrombocytopenia
Read Also: Can Prostate Cancer Be A Secondary Cancer
What B Cells Do
B cells react against invading bacteria or viruses by making proteins called antibodies. Your body makes a different antibody for each different type of germ . The antibody locks onto the surface of the invading bacteria or virus. This marks the invader so that the body knows it is dangerous and needs to be killed. Antibodies can also find and kill damaged cells.
The B cells are part of the memory of the immune system. The next time the same germ tries to invade the B cells that make the right antibody are ready for it. They are able to make their antibody very quickly.
Prostate Cancer And Covid
Since this virus is new, there is not much information regarding how it affects those with prostate cancer. What is known is that cancer patients in general are among those at a higher risk of developing a more serious illness due to a weakened immune system from the cancer itself and its treatments.
The link between COVID019 and prostate cancer lies in ones susceptibility to getting the virus and the possible severity.
You May Like: How To Know If You Have Prostatitis
Questions Patients Might Be Reluctant To Ask About Radiation Therapy
Getting a recommendation for radiation therapyas part of cancer treatment comes with a learning curve and a lot ofquestions. Morethan half of all patients with cancer receive radiation therapy at somepoint in their care, and patients and their families want to know how radiationworks and how it might affect their lives during and after treatment.
Still, we know some patients feel nervousasking questions about their cancer therapy. In a word: Dont. Asking questionshelps your doctors provide the best care.
Radiationoncologists at the UT Southwestern Harold C. Simmons Cancer Center areleaders in the field, conducting research studies and pioneering advancedradiation techniques such as stereotactic ablative radiotherapy ,brachytherapy, and novel combinations of radiotherapy with chemotherapy.
Were always happy to share the most currentradiation knowledge with our patients. So, here are answers to five of the mostcommon questions patients have said they were nervous to ask but were gladthey did.
What Is The Third Covid
The Joint Committee on Vaccination and Immunisation has recommended that everyone in the UK over the age of 12 with a severely weakened immune system have a third vaccine dose to help protect them from developing severe COVID-19 symptoms.
Some research has suggested that these severely immunosuppressed individuals may not build up a strong immune response to the COVID-19 vaccination. This means they may be less protected than the rest of the population.
Will I be offered the third dose?
The third dose is advised to anyone over the age of 12 who, at the time of their first or second vaccine dose, were severely immunosuppressed. This includes people with prostate cancer who had a vaccine dose within six months of their immunosuppressive chemotherapy or radiotherapy treatment. Chemotherapy and radiotherapy can weaken your immune system, this means you may not have built up a strong immune response to the first and second vaccinations.
External beam radiotherapy to the prostate shouldnt affect your immune system. If youve had radiotherapy to treat cancer inside your prostate, speak to your GP or consultant about whether you are eligible for a third dose.
Some men with advanced prostate cancer have radiotherapy to relieve bone pain in parts of the body where the cancer has spread. Depending on the bone treated and the dose of radiotherapy, this may have weakened your immune system. If youve had radiotherapy to treat advanced prostate cancer you may be offered a third dose.
Read Also: How Often To Get Prostate Exam
Changes In Peripheral Immune Cell Subsets During Rt
Peripheral blood mononuclear cells from 18 patients were collected at four timepoints during the study . Blood cell differential counts of four patients treated with localized RT were available at all successive time points. Leukocyte counts, but even more lymphocyte counts, decreased during the course of therapy . However, changes were overall not significant and cell counts appeared to recover three months after end of radiation .
Flow chart of the study and white blood cells counts. HLA-A*02+ patients undergoing primary RT for prostate cancer were included . RT regimens are shown . Blood samples were obtained before start of treatment , twice during therapy at 1 month intervals and three months after the end of treatment at a follow-up visit . As controls, three consecutive blood samples were obtained at one month intervals from HLA-A*02+ healthy donors . Absolute numbers of leucocytes and lymphocytes are shown before , during and post-therapy for four patients .
Impact of RT on T lymphocyte subsets. Percentage of total T cells among viable lymphocytes defined as CD3+ positive cells, CD8+ and CD4+ T cells and CD4+CD25+Foxp3+ cells within CD4+ cells are shown for the 4 timepoints A-D n = 18 RT patients are included. Healthy donors are shown in comparison . Bars indicate means. Significant differences: * p < 0.05 ** p < 0.01.
What To Expect With Provenge
Exploratory analysis of IMPACT
In a subanalysis of patients with PSA-matched cohorts, African American men lived longer than Caucasian menc,d
cThe PROCEED registry evaluated the expected safety and survival profile of PROVENGE received by patients in a real-world setting in which there was no control group. The study was conducted to quantify the risk of cerebrovascular events and survival. Patients may have received subsequent anti-cancer interventions per the local investigator’s standard of care.
dThis subgroup analysis of the PROCEED registry was exploratory and results need careful interpretation.
Recommended Reading: Can Constipation Affect The Prostate
What Are The Treatments For Prostate Cancer
Your treatment options usually depend on your age, your general health, and how serious the cancer is. Your treatment may include one or more of options:
- Observation,which is mostly used if you are older, your prostate cancer isn’t likely to grow quickly, and you don’t have symptoms or you have other medical conditions. Your doctor will keep checking on your cancer over time so to see whether you will need to start treatment for the cancer. There are two types of observation:
- Watchful waiting means having little or no testing. If symptoms begin or change, you will get treatment to relieve them, but not to treat the cancer.
- Active surveillance means having regular tests to see if your prostate cancer has changed. If the tests show the cancer is starting to grow or if you develop symptoms, then you will have treatment to try to cure the cancer.
Different Treatments Different Impacts
Because cancer treatments attack the disease in different ways, they may also affect the immune system in different ways. For instance:
Chemotherapy drugs are designed to kill fast growing cells, which most cancer cells are. But chemotherapy may also attack fast-growing healthy cells, such as those found bone marrow, which produces immune cells, hampering their ability to protect you from illnesses, bacteria and other threats.
Surgery, especially major surgery, may put a burden on the immune system, exhausting its reserves to help prevent infection and heal wounds caused by the procedure. Surgery requires cutting through the skin and layers of tissue, which may expose the body to germs. Also, surgeons may need to remove lymph nodes, which help fight infection.
Radiation therapy works by exposing cancer cells to ionizing waves of energy that kill the cells or stunt their growth. While destroying or damaging cancer cells, the treatment may also damage healthy cells and contribute to conditions that may lead to an increased risk of infection.
Immunotherapy drugs called checkpoint inhibitors are designed to boost the immune system by helping them to better recognize and attack cancer cells. But, in some cases, an overactive immune system may attack healthy cells and cause flu-like symptoms or potentially serious autoimmune conditions, such as colitis.
You May Like: How Do They Take A Biopsy Of The Prostate
What Is Coronavirus What Is Covid
Coronaviruses are a large family of viruses that cause illness ranging from the common cold to more severe diseases such as Middle East Respiratory Syndrome and Severe Acute Respiratory Syndrome .
COVID-19 is a new strain of coronavirus that has not been previously identified in humans. At present, the term coronavirus is usually intended to refer to COVID-19.
People can catch COVID-19 from others who have the virus. The disease can spread from person to person through small droplets from the nose or mouth which are spread when a person with COVID-19 coughs or exhales. These droplets can land in the mouths or noses of people who are nearby or possibly be inhaled into the lungs.
Side Effects Of Hormone Therapy
Whether through surgery or medication, hormone therapy can cause side effects that include hot flashes, low sexual desire, erectile dysfunction, fatigue, mood changes, muscle loss, weight gain and anemia.
Patients on long-term hormone therapy also have a risk of osteoporosis . To maintain bone health, ask your doctor about taking a calcium or vitamin D3 supplement. Your blood levels should be evaluated, as low vitamin D levels are common, and some individuals require a higher dose of this supplement. You should also participate in weight-bearing exercise regularly, as it helps to maintain bone health and muscle tone as well as reduce fatigue.
In addition, ADT’s effects on metabolism may increase your risk of diabetes and heart disease. We strongly recommend both aerobic and resistance exercise to maintain metabolic health, cardiovascular health, bone strength and quality of life. While treatment for advanced prostate cancer can disrupt your daily routine, it’s important not to abandon the healthy diet and exercise practices that are key to wellness and survival.
ADT’s impact on sex life is as important as the other side effects, and we hope to provide an open, supportive environment for you to discuss your condition and concerns. UCSF offers a program for treating erectile dysfunction.
You May Like: Can You Climax After Prostate Removal
A Note For Caregivers
Many places around the country are not allowing caregivers to attend appointments and treatments. Ask your loved ones provider to use the speakerphone during treatments so you can hear what is being said. Use technology and video conferencing to hear and see what is happening.
Above all, dont panic. You surely dont want care to be compromised, so follow all directions from the provider.
Contact Cleveland Urology Associates with additional questions or concerns about any links between COVID and prostate cancer.
As always, if you have any further questions or would like to schedule an appointment, please call or request an appointment online today!
What Is Oncolytic Virus Therapy
Oncolytic virus therapy, sometimes just called virus therapy, uses viruses that have been changed in a laboratory to destroy cancer cells. A genetically modified version of the virus is injected into the tumor. When the virus enters the cancer cells, it makes a copy of itself. As a result, the cancer cells burst and die. As the cells die, they release proteins that trigger your immune system to target any cancer cells in your body that have the same proteins as the dead cancer cells. The virus does not enter healthy cells.
Currently, one type of oncolytic virus therapy is approved in the United States to treat cancer:
Talimogene laherparepvec or T-VEC. This oncolytic virus therapy is approved to treat advanced melanoma that cannot be treated with surgery. It is used most often for people who cannot or choose not to receive any other recommended treatments. T-VEC is a modified version of the herpes simplex virus, which causes cold sores. It is injected directly into 1 or more melanoma tumors. Side effects of oncolytic virus therapy include flu-like symptoms and pain at the injection site.
Clinical trials are testing other oncolytic viruses for different cancers. They are also testing how the viruses work with other cancer treatments, such as chemotherapy.
Also Check: Hormone Therapy For Prostate Cancer Before Radiotherapy
