Different Approaches To Starting Hormone Therapy
Experts debate how early treatment with hormone therapy should be started. Some argue that the benefits of hormone therapy for prostate cancer should be offered to men earlier in the course of the disease. Others assert that there’s little evidence that getting treatment early is better than getting it later.
“Unfortunately, there are still some doctors who are offering hormonal therapy earlier in the course of the disease than is commonly recommended,” Brooks says. Given that the side effects can be serious, Brooks argues that starting treatment with hormone therapy so early may not be a good idea.
However, Holden argues that early treatment may be helpful. “I think one of the reasons that the death rate from prostate cancer is going down is that we’re using hormone therapy early,” he tells WebMD. “We haven’t proved that early treatment improves overall survival yet, but I think we will.”
Researchers are also looking at “intermittent therapy,” starting and stopping hormone treatment for months at a time. The big advantage is that men could go off therapy temporarily and thus be free of the side effects. Early study results have been promising.
Androgens And The Prostate
Testicular hormone secretion has long been known to influence prostate growth. In the 18th century, surgical castration was noted to cause prostate atrophy in adult animals and halt prostate growth in younger animals. In the late 19th century, castration was utilized to treat urinary retention caused by prostatic hyperplasia. In one early case series published in 1895, over half of the patients experienced improvement of urinary symptoms after surgical castration.
Androgen deprivation therapy was first proposed as a treatment for prostate cancer in 1940 when castration was utilized to provide pain relief, stabilize tumor burden, and reduce serum acid phosphatase in prostate cancer patients with osseous metastatic tumors.,
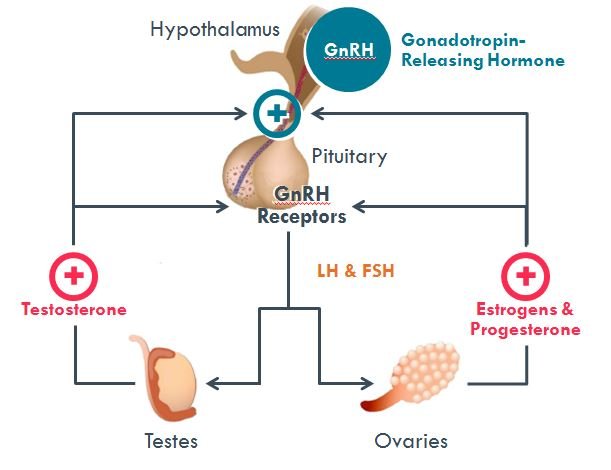
Given the morbidity of surgical orchiectomy and associated clinical side effects, alternative anti-androgenic measures have been sought. One early approach attempted chemical castration through injection of the female hormones stilbestrol and hexestrol to neutralize the effect of testicular androgens. The mechanism of this effect was discovered many years later: estrogen inhibits hypothalamic GnRH release through a negative feedback mechanism.
Tips For A Better Lupron Treatment Experience
Making the choice to treat your advanced prostate cancer can have its rewards and its challenges. To help yourself have the best possible treatment experience, take an active role in your therapy. These suggestions may help.
-
If you start experiencing side effects, don’t be silent. Talk to your doctor. He or she may have some ideas for helping to manage side effects. Its also important to let your healthcare team know if you experience new or worsening symptoms.
-
Stay committed to your LUPRON DEPOT therapy by going to all of your appointments. Get all the doses you are prescribed so you can get the most from your LUPRON DEPOT therapy.
-
If you miss an appointment, schedule another one as soon as you can. If scheduling is a problem, talk to your doctor about any options he or she may have.
-
Get monitored regularly to check your progress. During your scheduled visit, your Prostate Specific Antigen should be tested , and some doctors may also test your blood for testosterone levels to help your doctor determine how LUPRON DEPOT is working.1
Keep focused on the positive aspects of your life and the time you can spend with family and friends
Taking an active role in your treatment plan may help you feel more in control of what you’re going through.
What To Expect During Treatment
Doctors often use hormone therapies, such as Lupron, in combination with radiation therapy or other treatments. They may also use it following surgery.
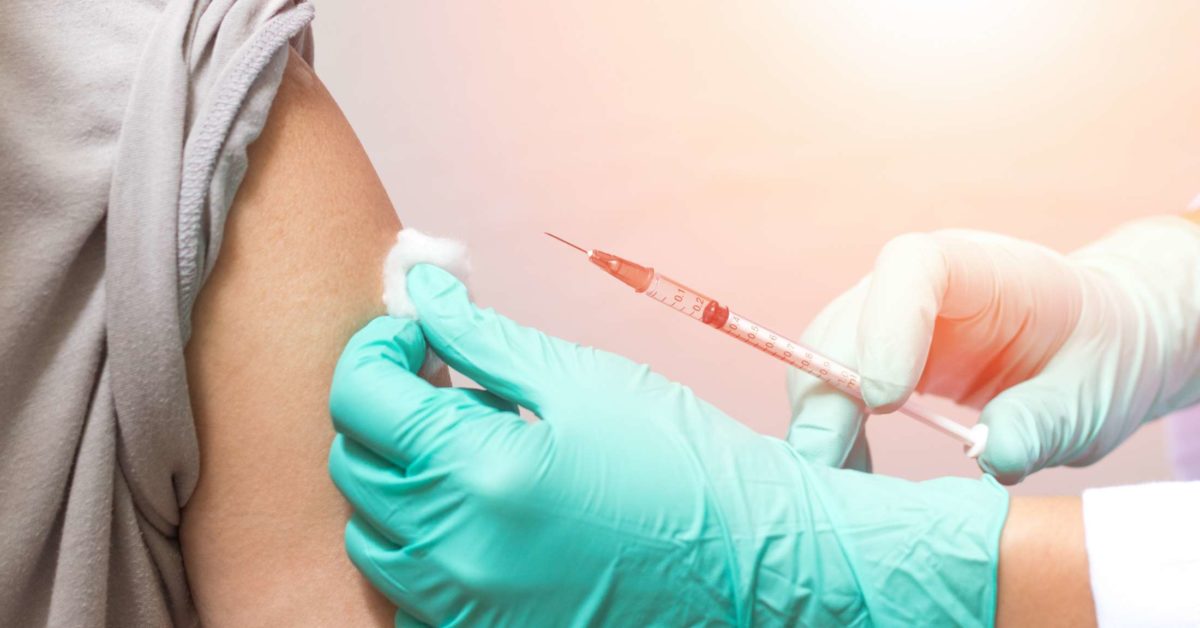
Healthcare professionals administer Lupron as a depot, which is a small implant that they inject under the persons skin. The individual can often choose an injection site that is suitable for them. Common injection sites include:
- upper arms
- outer thighs
- buttocks
The treatment regimen for Lupron will depend on the individuals circumstances, and a person can work with their doctor to determine the best dosage. Some typical dosages include:
- 7.5 mg one injection every 4 weeks
- 22.5 mg one injection every 12 weeks
- 30 mg one injection every 16 weeks
- 45 mg one injection every 24 weeks
When a person first starts treatment with Lupron, they may have a testosterone flare. Later on, they may experience side effects due to having very low testosterone levels in their body. After treatment stops, testosterone levels begin to return to normal.
When a person first takes Lupron, their testosterone levels may rise, or flare, before dropping to very low levels. For some people, particularly those with advanced prostate cancer, a testosterone flare can temporarily cause their symptoms to worsen.
The symptoms of a testosterone flare can include:
- blockage of the ureters, the tubes that carry urine from the kidneys to the bladder
- bone pain
- spinal cord compression
- issues with urination
- loss of muscle mass
- histrelin
- radiation therapy
Lupron Depot For Endometriosis
Lupron Depot is FDA-approved to treat endometriosis in women. It can help relieve pain associated with endometriosis. It can also reduce the size of lesions .
With endometriosis, the lining normally found inside the uterus begins to grow outside the uterus. This may occur in the ovaries, fallopian tubes, or other areas. These lesions can bleed and break down, resulting in pain and scar tissue. The lesions grow with the help of a hormone called estrogen thats naturally produced in the body.
Lupron Depot contains the drug leuprolide acetate, which belongs to a class of drugs called gonadotropin releasing hormone agonists. It works by blocking your body from creating certain hormones, like estrogen. This can help stop lesions from growing.
One of the possible side effects of Lupron Depot is a loss of bone density. Norethindrone acetate is a drug often given with Lupron Depot to prevent bone density loss.
Effectiveness for endometriosis
Lupron Depot has been found to be effective in treating endometriosis. For information on how the drug performed in clinical studies, see Lupron Depots prescribing information. The manufacturers site also provides details on the drugs effectiveness.
The American Association of Family Physicians recommends using a GnRH agonist, such as Lupron Depot, for treating endometriosis if hormonal contraceptives and NSAIDs arent effective.
Before Taking This Medicine
You should not use Lupron Depot if you are allergic to leuprolide or similar medicines such as buserelin, goserelin, histrelin, nafarelin, or if you have abnormal vaginal bleeding that has not been checked by a doctor.
Lupron Depot can cause birth defects. Do not use if you are pregnant. Tell your doctor right away if you become pregnant.
Certain brands or strengths of leuprolide are used to treat only men and should not be used in women or children. Always check your medicine to make sure you have received the correct brand and strength. Ask the pharmacist if you have any questions about the medicine you receive at the pharmacy.
To make sure Lupron Depot is safe for you, tell your doctor if you have ever had:
-
depression, mental illness or psychosis;
-
heart disease, congestive heart failure, long QT syndrome;
-
an electrolyte imbalance ; or
-
risk factors for bone loss .
Do not give this medicine to any child without medical advice.
Lupron Depot usually causes women to stop ovulating or having menstrual periods. However, you may still be able to get pregnant. Use a condom or diaphragm with spermicide to prevent pregnancy. Lupron Depot can make hormonal birth control less effective .
You should not breast-feed while using Lupron Depot.
Dosage For Central Precocious Puberty
For central precocious puberty, Lupron Depot-Ped can be given as a once-monthly dose thats based on body weight:
- 7.5 mg for children 55 lb or less
- 11.25 mg for children more than 55 lb up to 83 lb
- 15 mg for children more than 83 lb
Lupron Depot-Ped can also be given once every 3 months. The dosage options for taking it every 3 months are 11.25 mg or 30 mg.
Lupron Depot And Lab Tests
You may have reduced levels of certain hormones in your body during your treatment with Lupron Depot. If you have any lab tests that look for hormones, the results of the tests may be incorrect.
Its recommended that you wait 3 months until after youre done with Lupron Depot treatment before having these tests. This way, the results are less likely to be incorrect. Talk with your doctor about any tests you have scheduled while taking Lupron Depot to ensure your lab results will be accurate.
When To Consider Hormone Therapy
Hormone therapy is a treatment option for men with prostate cancer in any of the following situations:
- when cancer has metastasized beyond the prostate
- when cancer is confined to the prostate, but hormone therapy is used to boost the effectiveness of radiation therapy or to shrink the size of a tumor before brachytherapy
- when PSA begins to rise sometime after initial treatment with surgery or radiation therapy, indicating the cancer may have recurred.
Not all doctors agree on when to use hormone therapy, or how to administer it. Indeed, this is an area that requires a physician to exercise as much art as science in clinical practice. You should also be aware that side effects can be daunting, although most men tolerate treatment reasonably well .
When Is Hormone Therapy Used
Hormone therapy may be used:
- If the cancer has spread too far to be cured by surgery or radiation, or if you cant have these treatments for some other reason
- If the cancer remains or comes back after treatment with surgery or radiation therapy
- Along with radiation therapy as the initial treatment, if you are at higher risk of the cancer coming back after treatment
- Before radiation to try to shrink the cancer to make treatment more effective
What Are The Side Effects Of Hormone Therapy For Prostate Cancer
Because androgens affect many other organs besides the prostate, can have a wide range of side effects , including:
- loss of interest in sex
Studer UE, Whelan P, Albrecht W, et al. Immediate or deferred androgen deprivation for patients with prostate cancer not suitable for local treatment with curative intent: European Organisation for Research and Treatment of Cancer Trial 30891. Journal of Clinical Oncology 2006; 24:18681876.
Zelefsky MJ, Eastham JA, Sartor AO. Castration-Resistant Prostate Cancer. In: Vincent T. DeVita J, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles & Practice of Oncology, 9e. Philadelphia, PA: Lippincott Williams & Wilkins; 2011.
Smith MR, Saad F, Chowdhury S, et al. Apalutamide and overall survival in prostate cancer. European Urology 2021; 79:150158.
Almost The Same Thing: Eligard
Ob, I am on Eligard that sounds like “On-your-gard!!!
Mitch, I have all those symptoms you list above, maybe a few more on Eligard but its the same basic stuff as Lupron.
I have discussed quitting the shot with my wife a number of times, and with a few friends, and the oncologist at Loma Linda where I got proton and radiation treatments. The doctor told me I am the patitent and I don’t have to take anything I’m not comfortable with or don’t want- its my call as a patient. What would he recommend? I wanted to know. He favored the two year treatment plan I am on because it has a statisical advantage over less or no hormone treatment he told me. He was a very sharp doctor.
From a nursing textbook I learned that the hormone treatment, by stopping testostrone, actually interrupts cancer cell development, when the hormone drug is working as it should. Combined with radiation, hormone treatment might be the deciding factor to turn the growth of cancer cells in your favor.
And 2nd Base, Personally, if I had a PSA of 100 or higher, I would be scared to death every day. Something is going on with a PSA that high and oncology docs see this stuff and they push what they see as giving their patients an edge over cancer.
What Things Should I Think About Before Starting Hormone Therapy
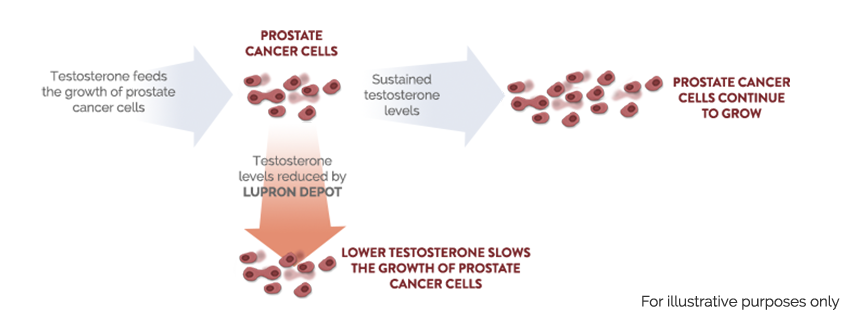
If you and your doctor are talking about hormone therapy as a way to control your prostate cancer, you should think about the following things:
- There are several kinds of hormone therapy. They work in different ways and have different side effects.
- Hormone therapy does not cure prostate cancer. It controls the growth of prostate cancer cells for a period of time. Speak with your doctor or health care team about what kind of hormone therapy is best for you.
The Future Of Hormone Therapy For Prostate Cancer
Some experts aren’t sure how much further we can improve hormone therapy for prostate cancer.
“I’m not saying that we’ve reached the end of what we can do with hormonal therapy,” Thrasher tells WebMD, “but there are only so many ways to shut down the hormonal effects. The cancer will still eventually escape.”
Brooks argues that, overall, prostate cancer is only moderately affected by hormones. “You can only do so much manipulating the levels of hormones,” says Brooks. “We have to find better ways to fight the basis of the cancer cells.”
Thrasher and Brooks have more hope that the next breakthroughs will come with different approaches, like chemotherapy or vaccines.
But Holden remains optimistic about the future of hormone therapy for prostate cancer.
“Cancer cells eventually figure out how to survive, how to overcome a specific hormone therapy,” he says. “But if we have enough types of drugs and can keep changing the hormone therapy, we might be able to keep the cancer cells in a state of confusion. We could change therapies before they have a chance to adapt.”
“It’s like an endless chess game,” he says. “You may not ever win, but you might be able to prolong the game indefinitely. I think that hormone therapy still has a lot of promise. We just need to develop better anti-androgens, and more varieties of them.”
Frequent Urination Burning With Urination And Difficulty Urinating
These are the most common complaints. Occasionally the urinary stream will weaken. Generally these symptoms are managed with medications to help the bladder function better or eliminate burning. Rarely, your doctor may order a urine test. Symptoms will resolve after the end of treatment. Contact your doctor if you see blood in your urine or if you are unable to urinate.
What Is Hormone Therapy
The idea that hormones have an effect on prostate cancer is not new. The scientist Charles Huggins first established this over 60 years ago in work that led to his winning the Nobel Prize. Huggins found that removing one of the main sources of male hormones from the body — the testicles — could slow the growth of the disease.
“This procedure worked dramatically,” says Holden, who is also director of the Prostate Cancer Center at Cedar Sinai Medical Center in Los Angeles. “Before, these men were confined to bed and wracked with pain. Almost immediately afterwards, they improved.”
Huggins found that some types of prostate cancer cells need certain male hormones — called androgens — to grow. Androgens are responsible for male sexual characteristics, like facial hair, increased muscle mass, and a deep voice. Testosterone is one kind of androgen. About 90% to 95% of all androgens are made in the testicles, while the rest are made in the adrenal glands located on top of the kidneys.
Hormonal Therapy For Aggressive Prostate Cancer: How Long Is Enough
Men weighing treatment options for intermediate- or high-risk cancer that is still localized to the prostate can face a tricky question. A standard approach in these cases is to give radiation to the prostate along with drugs that block testosterone, a hormone that makes the cancer cells grow faster. For how long should this hormone therapy last? Thats not entirely clear. The drugs have side effects, such as fatigue, impotence, and a loss of muscle mass. But radiation doesnt control prostate cancer effectively without them. Doctors therefore aim to give hormone therapy only for as long as it takes to help their patients, without causing any undue harm.
Now, newly published results from a phase 3 clinical trial are providing some needed guidance.
Hormone Treatment Fights Prostate Cancer
Hormone therapy for prostate cancer has come a long way in the past few decades. Not so long ago, the only hormonal treatment for this disease was drastic: an orchiectomy, the surgical removal of the testicles.
Now we have a number of medications — available as pills, injections, and implants — that can give men the benefits of decreasing male hormone levels without irreversible surgery.
“I think hormonal therapy has done wonders for men with prostate cancer,” Stuart Holden, MD, Medical Director of the Prostate Cancer Foundation.
Hormone therapy for prostate cancer does have limitations. Right now, it’s usually used only in men whose cancer has recurred or spread elsewhere in the body.
But even in cases where removing or killing the cancer isn’t possible, hormone therapy can help slow down cancer growth. Though it isn’t a cure, hormone therapy for prostate cancer can help men with prostate cancer feel better and add years to their lives.
On average, hormone therapy can stop the advance of cancer for two to three years. However, it varies from case to case. Some men do well on hormone therapy for much longer.
Theres More Hope All The Time
Metastatic prostate cancer can turn on a dime. For too long, a sudden shift in the disease has meant bad news. But now, more and more men are seeing a sudden turn in the right direction. Jeff Finerman is one of them.
In a very short time, Jeff has gone from being nearly bedridden after weeks of debilitating bone pain to feeling great. He feels so good, in fact, that hes planning on joining his family on a long-awaited trip to Asia a trip he thought he would probably have to miss. Two months ago, I wasnt going to be part of that, he says. My wife and I knew I probably wouldnt be going.
In September of 2017, Jeff was in such pain that I was soaking in the bathtub two to three hours a day. He had just changed doctors to UCLA medical oncologist and PCF Young Investigator John K. Lee, M.D., Ph.D. Dr. Lee was ready to write me a prescription for some heavy pain medicine; meanwhile, I was loading up with Advil. Then, I started Zytiga with prednisone ; along with Xgeva, a drug that specifically targets and strengthens cancer-riddled areas in the bone; and Lupron, a form of androgen deprivation therapy that helps control cancer by lowering testosterone. His quality of life was pretty bad, agrees Lee, and he was not able to do much physically. He was writhing in pain.
Jeffs doctor at UC Davis suggested starting a clinical trial, in addition to androgen deprivation therapy and radiation.
How The Study Was Performed
During the study, scientists randomized 1,071 men with intermediate- or high-risk localized prostate cancer into four groups. One group received radiation and six months of an anti-testosterone drug called leuporelin, and the second group received radiation plus 18 months of leuporelin therapy. Two other groups were treated with the same regimens of either radiation plus six or 18 months of leuporelin therapy, along with another drug called zoledronic acid, which helps to limit skeletal pain and related complications should cancer spread to the bones. Study enrollment occurred between 2003 and 2007 at 23 treatment centers across New Zealand and Australia.
When Hormone Therapy Stops Working
After some months or years the hormone treatment usually stops working and the cancer starts to grow again. Your doctor might recommend stopping or changing hormone treatment at this stage.
If you’re having anti androgens and your PSA level has started to rise again your doctor might get you to stop taking them. In some cases this can cause the cancer to shrink and stop growing for some time. This is called anti androgen withdrawal response .
There are different treatment options for when hormone therapy stops working, such as chemotherapy or steroids.
Swelling Bruising Or Tenderness Of The Scrotum
Symptoms generally resolve on their own within three to five days. Oral anti-inflammatory medications such as ibuprofen are usually sufficient for pain relief, if necessary. You should avoid hot tubs and Jacuzzis for at least two to three days after the procedure. Postpone bike riding until the tenderness is gone.
Hormone Therapy: Immediate Versus Delayed
Medical Research Council Prostate Cancer Working Party Investigators Group. Immediate Versus Deferred Treatment for Advanced Prostatic Cancer. British Journal of Urology 1997;79:23546. PMID: 9052476.
Messing EM, Manola J, Sarosdy M, et al. Immediate Hormonal Therapy Compared with Observation after Radical Prostatectomy and Pelvic Lymphadenectomy in Men with Node-Positive Prostate Cancer. New England Journal of Medicine 1999;341:17818. PMID: 10588962.
Messing EM, Manola J, Yao J, et al. Immediate Versus Deferred Androgen Deprivation Treatment in Patients with Node-Positive Prostate Cancer after Radical Prostatectomy and Pelvic Lymphadenectomy. Lancet Oncology 2006;7:4729. PMID: 16750497.
Nair B, Wilt T, MacDonald R, Rutks I. Early Versus Deferred Androgen Suppression in the Treatment of Advanced Prostatic Cancer. Cochrane Database of Systematic Reviews 2002;CD003506. PMID: 11869665.
Types Of Hormonal Therapies
There are 3 types of hormonal therapies for the treatment of prostate cancer. They may be used alone or together.
- Luteinizing hormone-releasing hormone agonists block the signal from your pituitary gland that tells your testicles to make testosterone. Leuprolide and goserelin are LHRH agonists. Theyre given by injection either once a month or every 3, 4, or 6 months.
- Anti-androgens are medications that block testosterone from attaching to cancer cells. This keeps it from helping cancer cells grow. One example of an anti-androgen is bicalutamide . This is a pill you take once a day.
- If youre taking bicalutamide, make sure you take it at the same time every day, with or without food.
- Your healthcare team will tell you when to start taking this medication.
If youre getting hormonal therapy by injection, read the section at the end of this resource called Your Injection Schedule.
How Does Hormone Therapy Work
Hormone therapy for prostate cancer works by either preventing the body from making these androgens or by blocking their effects. Either way, the hormone levels drop, and the cancer’s growth slows.
“Testosterone and other hormones are like fertilizer for cancer cells,” Holden tells WebMD. “If you take them away, the cancer goes into shock, and some of the cells die.”
In 85% to 90% of cases of advanced prostate cancer, hormone therapy can shrink the tumor.
However, hormone therapy for prostate cancer doesn’t work forever. The problem is that not all cancer cells need hormones to grow. Over time, these cells that aren’t reliant on hormones will spread. If this happens, hormone therapy won’t help anymore, and your doctor will need to shift to a different treatment approach.
Drugs That Stop Androgens From Working
Anti-androgens
For most prostate cancer cells to grow, androgens have to attach to a protein in the prostate cancer cell called an androgen receptor. Anti-androgens are drugs that also connect to these receptors, keeping the androgens from causing tumor growth. Anti-androgens are also sometimes called androgen receptor antagonists.
Drugs of this type include:
- Flutamide
They are taken daily as pills.
In the United States, anti-androgens are not often used by themselves:
- An anti-androgen may be added to treatment if orchiectomy or an LHRH agonist or antagonist is no longer working by itself.
- An anti-androgen is also sometimes given for a few weeks when an LHRH agonist is first started to prevent a tumor flare.
- An anti-androgen can also be combined with orchiectomy or an LHRH agonist as first-line hormone therapy. This is called combined androgen blockade . There is still some debate as to whether CAB is more effective in this setting than using orchiectomy or an LHRH agonist alone. If there is a benefit, it appears to be small.
- In some men, if an anti-androgen is no longer working, simply stopping the anti-androgen can cause the cancer to stop growing for a short time. This is called the anti-androgen withdrawal effect, although they are not sure why it happens.
Newer anti-androgens
Enzalutamide , apalutamide and darolutamide are newer types of anti-androgens.
These drugs are taken as pills each day.
