What Causes Chronic Bacterial Prostatitis
Chronic bacterial prostatitis is a type of infective prostatitis. It is caused by a persistent infection with a germ of the prostate gland. A man with chronic bacterial prostatitis will usually have had recurring urine infections. Chronic bacterial prostatitis is usually caused by the same type of germs that causes the urine infections. The prostate gland can harbour infection and therefore recurring infections can occur. Chronic bacterial prostatitis is not a sexually transmitted infection.
If Youre The Receiving Partner
Youll want to be as relaxed and aroused as possible, because itll make the experience easier and more enjoyable.
The whole poop-comes-out-of-the-butt thing gives some people a case of the heebie-jeebies even when its their own butt.
Remedy this by taking a shower and paying a little extra attention back there to get it squeaky clean. Some people like to use an enema before engaging in butt play, but it isnt necessary.
Use the bathroom before getting started. Prostate stimulation can make you feel like you need to pee, and anal penetration can cause the sensation of needing to poop.
Even though you wont actually do either, worrying that you might can interfere with your ability to let go and enjoy yourself. Knowing your bladder and bowels are empty can help.
Getting used to the sensation of having your prostate touched can help, too. Practice with an anal sex toy, like a butt plug, or your fingers.
Be sure to set the mood so that youre turned on and primed for action. Light candles, watch porn, or engage in some good old-fashioned masturbation or foreplay to get there.
Finally, be sure to lube up real good. Applying a water-based lubricant will allow for easier penetration and make for some easy gliding if stimulating your prostate externally.
What If My Prostatitis Is Not Caused By Infection
Because we do not understand what causes prostatitis without infection, it can be hard to treat. Your doctor might try an antibiotic to treat a hidden infection. Other treatments are aimed at making you feel better. Nonsteroidal anti-inflammatory medicines, such as ibuprofen or naproxen, and hot soaking baths may help you feel better. Some men get better by taking medicines that help the way the bladder or prostate gland work. These medicines include oxybutynin, doxazosin, prazosin, tamsulosin and terazosin.
Also Check: Cranberry Juice Good For Prostate
What Is A Prostate Infection
A prostate infection occurs when your prostate and the surrounding area become inflamed. The prostate is about the size of a walnut. Its located between the bladder and the base of the penis. The tube that moves urine from the bladder to the penis runs through the center of your prostate. The urethra also moves semen from the sex glands to the penis.
Several types of infections can affect the prostate. Some men with prostatitis experience no symptoms at all, while others report many, including intense pain.
Treatments That A Specialist May Suggest
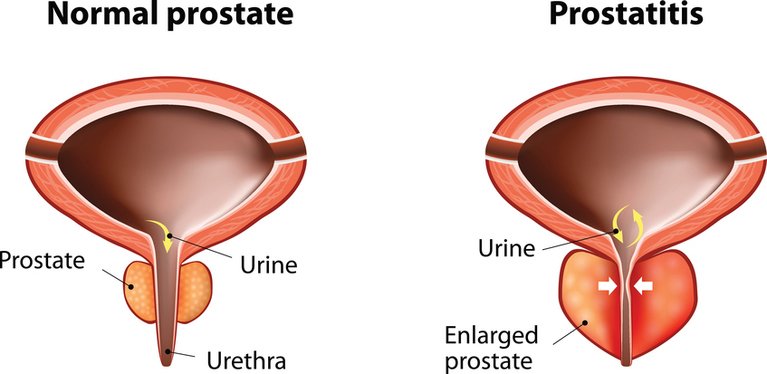
Various treatments have been tried for chronic prostatitis. They may benefit some people but so far there are few research studies to confirm whether they help in most cases. They are not ‘standard’ or routine treatments but a specialist may advise that you try one.
For chronic bacterial prostatitis, possible treatments may include the following:
- A longer course of antibiotics. If the specialist suspects that you have chronic bacterial prostatitis and your symptoms have not cleared after a four-week course of antibiotics, they may suggest a longer course. Sometimes a course of up to three months is used.
- Removal of the prostate may be considered if you have small stones in the prostate. It is not clear how much this may help but it has been suggested that these small stones may be a reason why some people have recurrent infections in chronic bacterial prostatitis. However, this is not commonly carried out and is not suitable in everyone. Your specialist will advise.
For chronic prostatitis/CPPS, possible treatments may include the following:
You May Like: Female Prostate Equivalent
How Durable Are The Benefits Of Urolift Procedure For Enlarged Prostate
Studies show that most men who experience benefit from Urolift procedurecontinue to benefit for up to 5 years and longer. Some men may experience a natural progression of BPH symptoms over time.
Should the benefits of Urolift treatment decrease over time, a few options are available. One option is the REZUM procedure for BPH, which is an office, minimally invasive procedure. Another option is to add medications such as Flomax which will often improve symptoms in combination with Urolift.
One of the major advantages of the Urolift procedure is that it does not preclude other treatment options such as Greenlight laser, laser enucleation of the prostate, Rezum procedure of the prostate, or TURP.
For men who have a significant progression of BPH and worsening of urinary symptoms after Urolift surgery and who desire significant improvement in urinary symptoms, prostate enucleation with a laser is an effective treatment option.
What Are The Types Of Prostatitis
Types of prostatitis include:
- Acute bacterial prostatitis : A UTI causes an infection in the prostate gland. Symptoms include fever and chills. You may experience painful and frequent urination or have trouble urinating. Acute bacterial prostatitis requires immediate medical treatment.
- Chronic bacterial prostatitis : Bacteria become trapped in the prostate gland, causing recurrent UTIs that are difficult to treat.
- Chronic pelvic pain syndrome, or CPPS : CPPS is the most common prostatitis type. Prostate gland inflammation occurs in approximately 1 out of 3 men. As the name implies, this type causes chronic pain in the pelvis, perineum and genitals.
- Asymptomatic inflammatory prostatitis : This condition causes prostate gland inflammation but no symptoms. You may learn you have this condition after getting tests to find the cause of other problems. For example, a semen analysis for infertility may detect asymptomatic inflammatory prostatitis. This type doesnt need treatment.
Read Also: Ejaculation Problems With Tamsulosin
How Is Acute Prostatitis Diagnosed
Your doctor will likely start by asking questions about your medical history. Theyll also conduct a physical examination.
Theyll probably conduct a digital rectal examination . During this procedure, theyll gently insert a gloved and lubricated finger into your rectum. Your prostate is located in front of your rectum, where your doctor can easily feel it. If you have acute bacterial prostatitis, it will likely be swollen and tender.
During a DRE, your doctor may also massage your prostate to squeeze a small amount of fluid into your urethra. They can collect a sample of this fluid for testing. Laboratory technicians can check it for signs of infection
Your doctor may also feel the lymph nodes in your groin, which may be enlarged and tender.
They may also conduct or order additional tests, such as:
- a blood culture to rule out bacteria in your blood
- a urinalysis or a urine culture to test your urine for blood, white cells, or bacteria
- a urethral swab to test for gonorrhea or chlamydia
- urodynamic tests to learn if you have problems emptying your bladder
- a cystoscopy to examine the inside of your urethra and bladder for signs of infection
Acute Prostatitis: Causes Symptoms And Diagnosis
What is acute prostatitis?
Acute prostatitis happens when your prostate gland becomes suddenly inflamed. The prostate gland is a small, walnut-shaped organ located at the base of the bladder in men. It secretes fluid that nourishes your sperm. When you ejaculate, your prostate gland squeezes this fluid into your urethra. It makes up a large portion of your semen.
Acute prostatitis is usually caused by the same bacteria that cause urinary tract infections or sexually transmitted diseases . Bacteria can travel to your prostate from your blood. It can enter your prostate during or after a medical procedure, such as a biopsy. It can also be caused by infections in other parts of your genitourinary tract.
If you have acute prostatitis, you may develop:
- chills
- pain above your pubic bone
- pain in your genitals, testicles, or rectum
Any bacteria that causes UTIs can cause prostatitis. Bacteria that commonly cause UTIs and prostatitis include:
- Proteus species
- Klebsiella species
- Escherichia coli
Some bacteria that cause STDs, such as chlamydia and gonorrhea, can also cause acute bacterial prostatitis. Other conditions that can lead to acute bacterial prostatitis include:
Factors that increase your risk of UTIs, STDs, and urethritis also increase your risk of acute prostatitis. For example, these risk factors include:
- not drinking enough fluids
- having unprotected vaginal or anal intercourse
Other risk factors include:
You May Like: How Are Fiducial Markers Placed In The Prostate
When Should You Call Your Doctor
if you have sudden fever, chills, and urinary symptoms, such as pain or burning with urination or blood or pus in the urine. These symptoms may point to acute prostatitis.
- Urinary symptoms and persistent pain in the low back, scrotum, penis, or the area between the scrotum and anus, or if you have pain with ejaculation or with a bowel movement.
- Recurring urinary tract infections .
- Discharge from your penis or sores on your genitals.
- Problems urinating, such as excessive nighttime urination, trouble starting urinating, decreased urinary stream, or frequent urination that isn’t related to drinking lots of fluids.
Diagnosing Chronic Bacterial Prostatitis
To make a diagnosis, your doctor will review your medical history and perform a physical exam to look for swollen lymph nodes near the groin or fluid discharge from the urethra.
Your doctor will also perform a digital rectal exam to examine the prostate. During this test, they will insert a lubricated and gloved finger into your rectum to look for signs of infection, such as a soft or enlarged prostate.
Your doctor may also use the following tests and techniques:
Antibiotics are the main course of treatment for this condition. Theyre usually taken for 4 to 12 weeks. For many people, treatment will last for 6 weeks.
First-line treatment is typically a fluoroquinolone antibiotic, such as ciprofloxacin , ofloxacin, or levofloxacin.
However, fluoroquinolones can increase your risk for a ruptured Achilles tendon, which is why they are no longer considered a preferred treatment.
Other commonly prescribed antibiotics include:
- sulfamethoxazole/trimethoprim , another first-line treatment
- tetracycline antibiotics, such as doxycycline or azithromycin
Tetracyclines are commonly used in cases where a doctor identifies or suspects chlamydia or mycoplasma genitalium. Like chlamydia, mycoplasma genitalium is an STI.
The antibiotic that youre prescribed will ultimately depend on which bacterium is causing your prostatitis.
Also Check: How Effective Is Chemotherapy For Prostate Cancer
If Youre The Giving Partner
Cleanliness and safety are a must, even for the giver.
Cut and file your nails smooth to help avoid scratching or tearing the delicate skin in and around the anus.
Wash your hands thoroughly, even if youre planning to use a condom over your finger to penetrate your partner. For extra comfort, stuff cotton balls inside the condom or glove.
You can also get the party started in the shower together, which serves as foreplay and gets you both all nice and clean for the big show.
Youll probably need to try a few different moves and experiment with speed and pressure to find what feels best.
Here are some techniques to try, whether youre using fingers or toys.
What Are The Symptoms Of Prostatitis
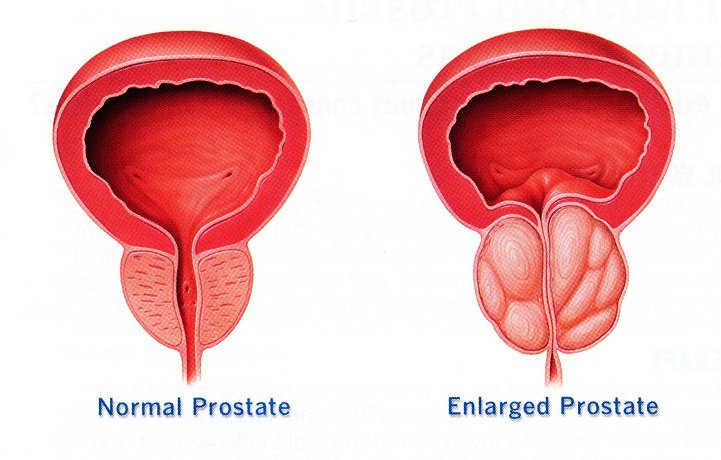
Each type of prostatitis has a range of symptoms that vary depending on the cause and may not be the same for every man. Many symptoms are similar to those of other conditions.
Chronic prostatitis/chronic pelvic pain syndrome. The main symptoms of chronic prostatitis/chronic pelvic pain syndrome can include pain or discomfort lasting 3 or more months in one or more of the following areas:
- between the scrotum and anus
- the central lower abdomen
- the scrotum
- the lower back
Pain during or after ejaculation is another common symptom. A man with chronic prostatitis/chronic pelvic pain syndrome may have pain spread out around the pelvic area or may have pain in one or more areas at the same time. The pain may come and go and appear suddenly or gradually. Other symptoms may include
- pain in the urethra during or after urination.
- pain in the penis during or after urination.
- urinary frequencyurination eight or more times a day. The bladder begins to contract even when it contains small amounts of urine, causing more frequent urination.
- urinary urgencythe inability to delay urination.
- a weak or an interrupted urine stream.
Acute bacterial prostatitis. The symptoms of acute bacterial prostatitis come on suddenly and are severe. Men should seek immediate medical care. Symptoms of acute bacterial prostatitis may include
You May Like: Is Cranberry Juice Good For The Prostate
What Is The Prostate Gland
The prostate is a gland that lies just below a man’s urinary bladder. It surrounds the urethra like a donut and is in front of the rectum. The urethra is the tube that carries urine out of the bladder, through the penis and out of the body. Your doctor may check your prostate by putting a finger into your rectum to feel the back of your prostate gland.
The prostate gland makes a fluid that provides nutrients for sperm. This fluid makes up most of the ejaculate fluid. We do not yet know all of the ways the prostate gland works.
The Longevity Of Treatment With Urolift Depends On Prostate Size Anatomy And Severity Of Initial Symptoms
Urolift Can Replace Medications for Many Men.
Urolift can often replace medications with similar or better efficacy for many men who are considered ideal candidates for Urolift after evaluation. For these men, Urolift is likely to work well for many years as the severity of prostate obstruction is mild-moderate. Prostate typically grows slowly over the years and these men can expect benefits to last 3-5 years or longer.
Recommended Reading: Is Zinc Good For Prostate
How Is Chronic Pelvic Pain Syndrome Managed Or Treated
Prostatitis treatments vary depending on the cause and type. Asymptomatic inflammatory prostatitis doesnt require treatment.
For chronic pelvic pain syndrome , your healthcare provider may use a system called UPOINT to classify symptoms into six categories. Your provider uses multiple treatments at the same time to treat only the symptoms youre experiencing.
Approximately 80% of men with CPPS improve with the UPOINT system. The system focuses on these symptoms and treatments:
- Urinary: Medications, such as tamsulosin and alfuzosin , relax muscles around the prostate and bladder to improve urine flow.
- Psychosocial: Stress management can help. Some men benefit from counseling or medications for anxiety, depression and catastrophizing .
- Organ: Quercetin and bee pollen supplements may relieve a swollen, inflamed prostate gland.
- Infection:Antibiotics kill infection-causing bacteria.
- Neurologic: Prescription pain medicines, such as amitriptyline and gabapentin , relieve neurogenic pain. This pain can include fibromyalgia or pain that extends into the legs, arms or back.
- Tenderness: Pelvic floor physical therapy may include myofascial release . This therapy can reduce or eliminate muscle spasms.
When To Get Medical Advice
See a GP if you have symptoms of prostatitis, such as pelvic pain, difficulty or pain when peeing, or painful ejaculation.
They’ll ask about the problems you’re having and examine your tummy.
You may also have a rectal examination. This is where a doctor inserts a gloved finger into your bottom to feel for anything unusual. You may have some discomfort during this examination if your prostate is swollen or tender.
Your urine will usually be tested for signs of infection, and you may be referred to a specialist for further tests to rule out other conditions.
See a GP straight away if you get sudden and severe symptoms of prostatitis.
You may have acute prostatitis, which needs to be assessed and treated quickly because it can cause serious problems, such as suddenly being unable to pee.
If you have persistent symptoms , you may be referred to a doctor who specialises in urinary problems .
You May Like: How Long Can You Take Lupron For Prostate Cancer
When To See A Doctor
See your primary care provider if youre having pain, burning, or trouble urinating. They may refer you to a urologist, a doctor who treats urinary health disorders in both men and women. This specialist also treats issues of the male genital system, including prostate problems.
During the exam, the doctor may insert a gloved, lubricated finger into your rectum. This test is called a digital rectal exam . It helps your doctor feel if part of your prostate is swollen or enlarged.
During the DRE, your doctor may massage your prostate to cause fluid from the prostate to be secreted into your urine in order to check for a cause of prostatitis, such as an infection. They may also test your blood, semen, and urine.
Your doctor may order an ultrasound, which is a scan that uses sound waves to create a picture of your prostate. They may also perform urodynamic tests, which measure your ability to empty your bladder.
Treatments For Symptom Relief
The preferred treatment regimen for chronic bacterial prostatitis is a combination of antibiotics and anti-inflammatory medications, such as nonsteroidal anti-inflammatory drugs .
Although NSAIDs can provide relief from the pain of prostatitis, theyre primarily used to reduce inflammation.
Other medications you may receive are:
- stool softeners to avoid constipation
- alpha-blocker medications, such as tamsulosin , to help treat urinary retention
Certain home remedies may be able to ease your symptoms too. Home remedies include:
- warm baths
- avoiding alcohol, caffeine, citrus juices, and hot and spicy food
Read Also: Do Females Have Prostate Cancer
What Does A Prostate Orgasm Feel Like
P-spot orgasms are said to feel similar to penile orgasms, only way more intense and felt through the entire body.
There are reports of people having super orgasms, which are a stream of fast, continuous orgasms that cause the body to shudder.
Not everyone ejaculates during a prostate orgasm, but some release a dribble of milky fluid from the urethra.
A little bit of prep can help make the experience a good one whether youre flying solo, or on the giving or receiving end of things.
