Prospects For Improving The Perspectives In Prostatitis
While the initiatives described above are exciting, practicing urologists are treating patients today. If the urologist, who has become frustrated with this disease, decides to use the classification system, diagnostic plan, and therapeutic algorithm proposed in this review, he or she may find that the management of prostatitis will be just another enjoyable aspect of his urologic practice.
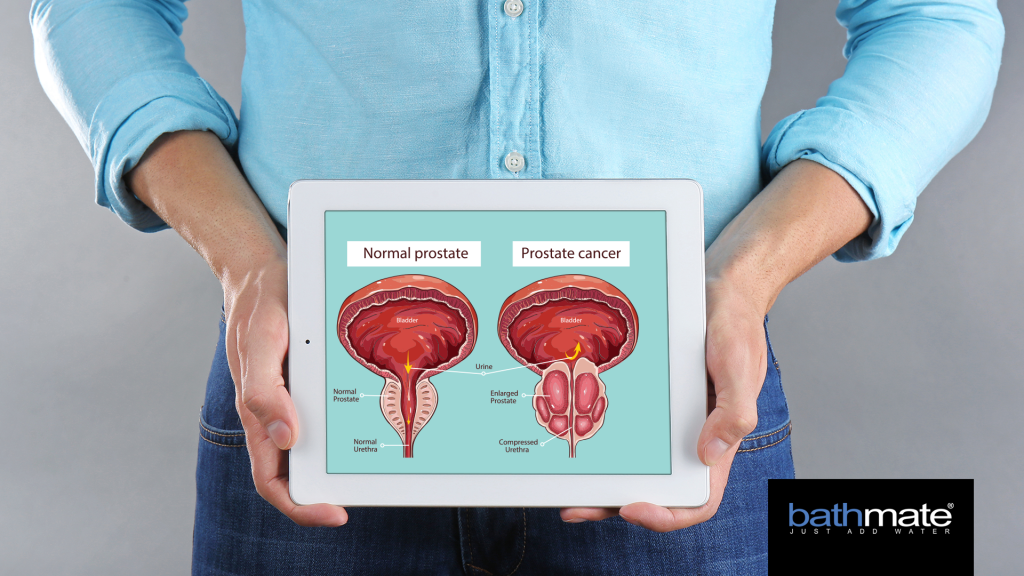
What Causes An Enlarged Prostate
It’s not known what causes many cases of prostatitis. A bacterial infection is only sometimes responsible.
In many cases of chronic prostatitis, doctors can’t find any infection in the prostate gland, although they may still prescribe a course of antibiotics. In these cases, the cause is poorly understood.
Chronic prostatitis is thought to be caused by a number of suggested factors, including partial blockage of the flow of urine and underlying problems with the immune system, pelvic floor or nervous system.
What Is Prostatitis And What Causes It
4.4/5Prostatitiscaused byprostatefull detail here
Acute bacterial prostatitis is often caused by common strains of bacteria. The infection can start when bacteria in urine leak into your prostate. Antibiotics are used to treat the infection. In many cases of prostatitis, the cause isn’t identified.
One may also ask, what is prostatitis and how is it treated? Antibiotics. Taking antibiotics is the most commonly prescribed treatment for prostatitis. If you have severe symptoms, you might need intravenous antibiotics. You’ll likely need to take oral antibiotics for four to six weeks but might need longer treatment for chronic or recurring prostatitis.
Additionally, is prostatitis serious?
Prostatitis. Prostatitis is the inflammation of the prostate gland. acute prostatitis where the symptoms are severe and develop suddenly; it’s rare, but can be serious and requires immediate treatment, and is always caused by an infection.
Can prostatitis be transmitted to a woman?
Prostatitis is frequently caused by bacterial infections, but it’s usually not caused by something that can be passed on to your partner during sex. In rare cases, prostatitis is caused by a sexually transmitted infection .
Also Check: How To Reduce Prostate Swelling Naturally
Practical Answers To Our Problems
Epidemiology of ProstatitisA Beginning. Recent epidemiologic studies confirmed that prostatitis is a major male health issue. In the early 1990s, 2 million office visits per year were recorded in the United States for prostatitis. Eight percent of urologists office visits and 1% of family physicians office visits were for prostatitis. Urologists in Wisconsin saw an average of 173 patients with prostatitis per year, while Canadian urologists treated 262 such patients per year. Thirty-eight percent of these were patients in their practice newly diagnosed with prostatitis. The incidence and prevalence of prostatitis ranges between 5% and 8%. The quality of life of a patient with chronic prostatitis is similar to that of a patient with a recent myocardial infarction, unstable angina, or active Crohns disease. While the effect on society of this very common disease of young, productive men has not been calculated, it must be enormous.
A New Classification SystemA Good Start. In 1995, the National Institutes of Health convened a con-census conference to determine future directions in the management of prostatitis. It was decided that before any further work could be done, a generally accepted classification system based on no preconceived notions would be used for further examination of this disease. The classification system that was decided on is one that could be useful in clinical practice as well. It divides the prostatitis syndrome into 4 categories.
Can Treating Gum Disease Cure Prostatitis

However, before I dive into the meat of the research, I think its a good idea to start with an issue that everyone reading this can control for, and thats dental hygiene.
As youll see reading this post, we get into issues of PH and which bacteria thrive in more acidic environments. For example, the PH of urine can dictate whether bacteria like E. coli can grow in the urinary tract. Similarly, the state of our dental hygiene also plays a role in the pathogenic load placed on the body. The issue first came on my radar when visiting with a holistic dentist recently. He developed a product that raises the PH of the mouth to make it more alkaline.
At first, I was skeptical , but then I did some reading.
I was surprised to see saliva referred to as containing many host defense factors, and the PH of saliva is a biomarker for gum disease. 2 More acidic saliva correlates with more advanced gum disease, whereas more alkaline saliva is associated with better gum health.
But, heres the kicker gum disease and prostatitis go hand in hand. In fact, there are studies demonstrating significant improvement in prostate inflammation just by treating the gums alone. So, if youre reading this and you have prostatitis, the first step is to visit with a holistic dentist, make sure your gums are healthy, and pay attention the acidity of your saliva.
Also Check: Does Prostate Stimulation Increase Testosterone
Prostatitis: Is It Curable By Itself Or Not
leo over a year ago
Loading…
Guest over a year ago
Guest over a year ago
There are different kinds of prostatitis; bacterial, non-bacterial, and inflammatory. The prostatitis treatment you need depends on the kind of prostatitis you have. While you can certainly explore natural treatments in some cases , you shouldn’t just leave it alone and hope for the best, that’s for sure.;
Anyway, may want to explore prostate drainage, Traditional Chinese Medicine, acupuncture, herbal supplements such as saw palmetto, and also a regimen of vitamin supplements that will help you some. These are not necessarily a substitute for other medical treatment, and if you have bacterial prostatitis you will definitely need antibiotics, but they can help you some for sure.;
Rob over a year ago
over a year ago
In reply to Rob on 2012-09-16 – click to read
Symptoms Of Chronic Bacterial Prostatitis
Bacterial infections in the prostate can be very painful.
The symptoms begin slowly and last 3 months or longer. Seek medical attention if you have any of the following symptoms:
Serious complications can arise if an infection isnt properly treated. Complications include:
- urinary retention, which is an inability to urinate
- , which occurs when bacteria spread into the bloodstream
- a prostate abscess, which is a collection of pus that causes inflammation
A bacterial infection causes chronic bacterial prostatitis. Even when the primary symptoms of infection have been treated, bacteria may continue to thrive in the prostate.
Causes of infection include:
- sexually transmitted infections , such as chlamydia and gonorrhea
- E. coli after having an infection of the testicles, urethritis , or a UTI
Certain factors put people at risk for developing this condition, such as:
Also Check: What Can Be Done For An Enlarged Prostate
Can Prostatitis Come Back
Men who have had prostatitis once are more likely to get it again. Antibiotics may not get into the prostate gland well. Small amounts of bacteria might hide in the prostate and not be killed by the antibiotic. Once you stop taking the antibiotic, the infection can get bad again. If this happens, you might have to take antibiotics for a long time to prevent another infection. Prostatitis that is not caused by infection is often chronic. If you have this kind of prostatitis, you might have to take medicine for a long time.
Providing Your Medical History
At first, the doctor will probably ask you about your medical history. Do you have any chronic illnesses? What illnesses and operations have you had in the past? What medications are you taking, if any? Your doctor is also likely to ask about your psychological well-being and lifestyle: Do you suffer from depression? Are you under a lot of stress? Do you drink alcohol? Smoke? Use illegal drugs? Have you felt a loss of affection for your partner? Have you recently grown interested in a new partner?
As part of this health history, be prepared to tell your doctor specific details about the symptoms that brought you to the office and when they began. Your doctor might want to know how often you had sex before the problem started and if there have been weeks or months in the past when youve had erectile dysfunction. Your doctor may conduct a written or verbal screening test.
If the cause is clear a recent operation for prostate cancer, for example the conversation may move directly to your treatment options. Otherwise, you may need to answer more questions to help the doctor narrow down the possible causes and avoid unnecessary testing.
You May Like: Is Prostate Cancer Estrogen Dependent
When Should You Call Your Doctor
if you have sudden fever, chills, and urinary symptoms, such as pain or burning with urination or blood or pus in the urine. These symptoms may point to acute prostatitis.
- Urinary symptoms and persistent pain in the low back, scrotum, penis, or the area between the scrotum and anus, or if you have pain with ejaculation or with a bowel movement.
- Recurring urinary tract infections .
- Discharge from your penis or sores on your genitals.
- Problems urinating, such as excessive nighttime urination, trouble starting urinating, decreased urinary stream, or frequent urination that isn’t related to drinking lots of fluids.
What Is Painful Ejaculation
Ejaculation is the release of semen from the penis during the male orgasm. It is normally a pleasurable experience and shouldnt be uncomfortable.
Yet ejaculation can sometimes be painful, and its not an uncommon problem. A review article published in the journal,;Translational Andrology and Urology, reported that up to 10% of men have had painful ejaculation at some point in their lives. Among those with prostate issues, that rate climbed to 30% to 75%.
The sensations of painful ejaculation vary. It may feel like pain or burning in the perineum , the urethra, or scrotum. The pain may begin during sex and become more severe when you climax, or it may be painful only when you ejaculate.
Painful ejaculation can be a symptom of an infection, inflammation, or blockage of the lower urinary tract . One of the most common causes is prostatitis, an inflammation of the prostate.
Ejaculation could also be painful because of psychological and emotional factors. Discuss painful ejaculation, and any other symptoms, such as discharge or pain, with your doctor.
Read Also: How Do They Test For Prostate Infection
What Are The Symptoms
Symptoms of long-term prostatitis are often mild and start slowly over weeks or months. They may include:
- An urge to urinate often. But you may pass only small amounts of urine.
- A burning pain when you urinate.
- A problem starting the urine stream, urinating in waves rather than in a steady stream, urine flow that is weaker than normal, and dribbling after urinating.
- Waking up at night to urinate often.
- A feeling of not completely emptying your bladder.
- Pain in your lower back, in the area between the testicles and anus, in the lower belly or upper thighs, or above the pubic area. Pain may be worse during a bowel movement.
- Some pain during or after ejaculation.
- Pain in the tip of your penis.
Symptoms of acute prostatitis are the same, but they start suddenly and are severe. They may also include a fever and chills.
Some men may have no symptoms.
Ruling Out Fungal Infection
Consider this study;which appeared in the Central European Journal of Urology. The authors found that most young men presenting with prostatitis, who also had low prostate specific antigen numbers , were suffering from a yeast infection, not bacterial prostatitis, although E. Coli was thought to be the bridge that brought yeast to the prostate region in the first place.
Also Check: Is Prostate Cancer A Disability
What Are The Types Of Prostatitis
- Acute bacterial prostatitis;is the least common of the four types and is potentially life-threatening, but it is the easiest to diagnose and treat effectively. Men with this disease often have chills; fever; pain in the lower back and genital area; urinary frequency and urgency, often at night; burning or painful urination; body aches; and a demonstrable infection of the urinary tract as evidenced by white blood cells and bacteria in the urine.
- Chronic bacterial prostatitis, also relatively uncommon, occurs when bacteria find a spot on the prostate where they can survive. Men have urinary tract infections that seem to go away but then come back with the same bacteria.
- Chronic prostatitis/chronic pelvic pain syndrome;is the most common but least understood form of prostatitis. It may be found in men of any age. Its symptoms go away and then return without warning, and it may be inflammatory or non-inflammatory. In the inflammatory form, urine, semen, and prostatic fluid contain the kinds of cells the body usually produces to fight infection, but no bacteria can be found. In the non-inflammatory form, not even the infection-fighting cells are present.
- Asymptomatic inflammatory prostatitis;is the diagnosis given when the patient does not complain of pain or discomfort but has infection-fighting cells in his prostate fluid and semen. Doctors usually find this form of prostatitis when looking for causes of infertility or testing for prostate cancer.
Is Prostatitis A Sexually Transmitted Disease
Yes, prostatitis can be contracted through sex, so the more sexual partners a man has, the higher his odds of developing the condition. 34567
Interestingly, Trichomonas vaginalis, a parasite and STD, has been found in prostate biopsies of men with prostatitis, and although it seems that E. Coli is a much more regular culprit, the prostates susceptibility to;Trichomonas vaginalis colonization has been linked to zinc levels. The prostate is the number one home for zinc in a mans body, and when levels get low, studies have shown these types of pathogens can take a greater foothold.
Mineral deficiencies are common in the U.S., which means supplementing with small amounts of zinc to see whether conditions improve could be worthwhile. As far as food is concerned, pumpkin seeds and oysters are both high in zinc.
As an added benefit, zinc supplementation has also shown some promise in maintaining the cell lining of the gut, which can prevent or help to heal leaky gut, a condition that often accompanies prostatitis, and that is marked by a breakdown of the epithelial wall of the gut lining, which allows pathogens and undigested food particles to enter the blood stream. 89 I will touch more on leaky gut later in this post.
Read Also: How To Stop Leaking After Prostate Surgery
Chronic Pelvic Pain Syndrome
CPPS is the most common type of prostatitis around 19 out of every 20 men with prostatitis have it. You might also hear it called chronic non-bacterial prostatitis, chronic abacterial prostatitis or prostate pain syndrome. Chronic means long-lasting.
Men with CPPS usually have symptoms for three months or longer. Even after treatment, you may still have prostatitis for a long time. It might come and go, causing occasional episodes of severe pain, sometimes known as flare-ups.
What causes it?
Nobody knows for certain what causes CPPS. Unlike other types of prostatitis it isnt usually caused by a bacterial infection. There could be a number of causes, which makes it difficult to diagnose and treat.
There are also a number of things that might trigger it, including:
- urine getting into the prostate
- previous infections in or around the prostate
- an infection that doesnt show up in tests
- problems with nerves, so that they send pain signals to the brain even when theres nothing physically wrong
- stress, anxiety or depression
- problems with the pelvic floor muscles .
Some research shows a link between stress, anxiety and depression and CPPS. But this doesnt mean that CPPS is all in your head. If youre feeling stressed or depressed, this may cause physical symptoms that trigger CPPS, or make symptoms worse.
Diagnosing Chronic Bacterial Prostatitis
To make a diagnosis, your doctor will review your medical history and perform a physical exam to look for swollen lymph nodes near the groin or fluid discharge from the urethra.
Your doctor will also perform a digital rectal exam to examine the prostate. During this test, they will insert a lubricated and gloved finger into your rectum to look for signs of infection, such as a soft or enlarged prostate.
Your doctor may also use the following tests and techniques:
Antibiotics are the main course of treatment for this condition. Theyre usually taken for 4 to 12 weeks. For many people, treatment will last for 6 weeks.
First-line treatment is typically a fluoroquinolone antibiotic, such as ciprofloxacin , ofloxacin, or levofloxacin.
However, fluoroquinolones can increase your risk for a ruptured Achilles tendon, which is why they are no longer considered a preferred treatment.
Other commonly prescribed antibiotics include:
- sulfamethoxazole/trimethoprim , another first-line treatment
- tetracycline antibiotics, such as doxycycline or azithromycin
Tetracyclines are commonly used in cases where a doctor identifies or suspects chlamydia or mycoplasma genitalium. Like chlamydia, mycoplasma genitalium is an STI.
The antibiotic that youre prescribed will ultimately depend on which bacterium is causing your prostatitis.
Also Check: Can An Mri Detect Prostate Cancer
Can Prostatitis Be Cured By Itself
Many prostatitis patients feel embarrassed to see a doctor and have a timely treatment, they think this disease can be cured by itself. In fact, this misunderstanding will cause further damages to the body since prostatitis will lead to other complications if left untreated.
- Shop 1-3, Nan Hu Xin Cheng, Wenchang Road, Hongshan District, Wuhan, Hubei Province, China
Q&A
Treatments For Symptom Relief
The preferred treatment regimen for chronic bacterial prostatitis is a combination of antibiotics and anti-inflammatory medications, such as nonsteroidal anti-inflammatory drugs .
Although NSAIDs can provide relief from the pain of prostatitis, theyre primarily used to reduce inflammation.
Other medications you may receive are:
- stool softeners to avoid constipation
- alpha-blocker medications, such as tamsulosin , to help treat urinary retention
Certain home remedies may be able to ease your symptoms too. Home remedies include:
- warm baths
- avoiding alcohol, caffeine, citrus juices, and hot and spicy food
Don’t Miss: Can You Ejaculate With An Enlarged Prostate
