Hormone Therapy For Prostate Cancer
Jump to a section
Hormone therapy is also called androgen suppression therapy. The goal is to reduce levels of male hormones, called androgens, in the body, or to stop them from fueling prostate cancer cells.
Androgens stimulate prostate cancer cells to grow. The main androgens in the body are testosterone and dihydrotestosterone . Most androgen is made by the testicles, but the adrenal glands as well as the prostate cancer itself, can also make a fair amount. Lowering androgen levels or stopping them from getting into prostate cancer cells often makes prostate cancers shrink or grow more slowly for a time. But hormone therapy alone does not cure prostate cancer.
Paracrine And Autocrine Signaling
Newer treatments for prostate disease have been based on regulating paracrine signaling within the tissue itself.
Paracrine signaling and mesenchymalepithelial cell interactions are an essential component of androgenic control of the prostate gland and AAT can also be effectively realized by targeting local androgen metabolism and signaling. Testicular testosterone is normally converted to the more potent androgen dihydrotestosterone by the 5-reductase type 2 enzyme that is located in the prostatic stroma. DHT then acts in a paracrine manner to subsequently activate the epithelial androgen receptor to maintain secretory function. Treatment with 5R inhibitors rapidly reduces DHT levels within the prostate, while AR antagonists effectively prevent any androgenic effects by blocking the androgen signaling pathway.
In a manner analogous, yet different, to androgens, estrogens also exert local effects in the prostate via paracrine mechanisms. An important difference is that estrogens are both adversely and beneficially implicated in the genesis and progression of PCa. This alters the application and complicates the use of estrogen-based therapies in the treatment of prostate disease.
Estrogen Imprinting & Epigenetic Modifications
There is reason to believe that some of the effects of estrogen on the prostate gland are the result of developmental exposures that predispose to prostate disease later in life, fitting into the emerging paradigm on the fetal basis of adult disease. A classic example is in utero exposure to DES, which has been linked to increases in breast and vaginal cancer of exposed offspring, although adult DES exposure presents limited risk for these cancers . The prostate gland is similarly dependent upon steroid hormones, and imbalances in these hormones during development can result in abnormalities in growth and differentiation . For example, in utero DES exposure has been associated with an increased rate of structural abnormalities of the prostatic utricle in newborn sons , while elevated maternal estrogen levels during pregnancy have been associated with increased prostate cancer risk in humans . In rodents, DES exposure during the perinatal period predisposes the offspring to prostate cancer . While it remains to be investigated if the overall risk of developing prostate cancer is increased in humans after in utero exposure to DES as exposed sons are just now entering the typical age of prostate cancer risk, the earlier onset of disease as seen with breast cancer in DES-exposed daughters has not been demonstrated with prostate cancer.
Don’t Miss: When To Get A Prostate Biopsy
Intermittent Versus Continuous Hormone Therapy
Most prostate cancers treated with hormone therapy become resistant to this treatment over a period of months or years. Some doctors believe that constant androgen suppression might not be needed, so they advise intermittent treatment. The hope is that giving men a break from androgen suppression will also give them a break from side effects like decreased energy, sexual problems, and hot flashes.
In one form of intermittent hormone therapy, treatment is stopped once the PSA drops to a very low level. If the PSA level begins to rise, the drugs are started again. Another form of intermittent therapy uses hormone therapy for fixed periods of time for example, 6 months on followed by 6 months off.
At this time, it isnt clear how this approach compares to continuous hormone therapy. Some studies have found that continuous therapy might help men live longer, but other studies have not found such a difference.
Mechanisms Of Estrogen Carcinogenesis: Genotoxic Activity Of Estrogen Metabolites
There is a growing body of evidence to suggest that estrogens might act as carcinogenic factors not only through the ER but also through a genotoxic mechanism. Estradiol can be converted to so-called catecholestrogen metabolites by P450-mediated hydroxylation. Unless they are detoxified, these catecholestrogens can undergo a process called redox-cycling. This process leads to the formation of reactive oxygen species that can lead to DNA damage and lipid peroxidation, as well as to the formation of reactive intermediates that can directly adduct to DNA, which might lead to mutagenesis. There is evidence that this happens in tissue culture and in animal models of estrogen-induced cancer, as well as a limited amount of evidence from studies with human breast cancer tissue.,
Read Also: What Is The Va Disability Rating For Prostate Cancer
Mapping Of Sequencing Data
Mapping of the Color Space sequencing reads to the reference genome was performed with the Lifetech Lifescope 2.5.1 bioinformatics software suite, after âa prioriâ error correction with the SAET procedure. The resulting alignment files in standard.bam format were analyzed for peak calling directly with the MACS software version 1.4.1 . In addition, the.bam alignments were converted to the.bed format with the bamToBed bedtools utility and used for peak calling with the SICER analysis software in order to take into account the heterogeneous nature of these DNA – protein interactions which may include quite long areas of interaction. All intersections between MACS and SICER bed files and genome-wide features was performed with the bedTools v2.17.0 software suite .
How Are Hormone Therapy Medicines Used
Hormone therapy medicines may be used alone, with another type of hormone therapy, or with another type of prostate cancer treatment.
Monotherapy
Monotherapy is when only one type of hormone therapy medicine is used to lower the amount of testosterone in your body. Monotherapy can be effective in shrinking a prostate cancer tumor, slowing the spread of your prostate cancer, and relieving pain caused by your prostate cancer. Monotherapy may be used with neoadjuvant therapy or adjuvant therapy. Please read When is Hormone Therapy Used for Prostate Cancer? to learn more about neoadjuvant and adjuvant therapy.
Combination therapy
Also Check: How Is Prostate Size Measured
Targeting Ers In Pc: Therapeutic Approaches
Androgen deprivation therapy, either medical or surgical, is the first line of treatment for PC. Although more potent AR antagonists have been designed, resistance to these drugs continues to develop, resulting in CRPC, which is almost untreatable . Alternative approaches to androgen ablation need to be considered to prevent progression and metastatic spreading of PC.
Selective ER modulators are synthetic estrogen receptor ligands that show both estrogenic and/or antiestrogenic effects, depending on cell type and the different expression and/or activation of transcriptional co-regulators. By inducing a conformational change in ERs, SERMs might influence the interaction between ER and co-regulatory proteins . Several SERMS, such as tamoxifen, toremifene, and raloxifene, are able to suppress PC growth in mouse models and cultured cells . However, clinical trials with high-dose tamoxifen or toremifene did not show significant effects , and the combinatorial use of toremifene and ADT in patients with advanced PC has only recently been found to have a relative beneficial effect . Further, clinical trials with larger cohorts are needed to confirm these promising phase IIA results.
New Directions In Hormonal Carcinogenesis
The idea that endogenous levels of circulating hormones are the primary determinants of cancer risk is troubling, since endogenous hormones are not an easily modifiable risk factor, like diet or smoking. We simply cannot remove or lower endogenous hormones to reduce cancer risk. Thus, we are forced to develop new strategies for early detection and prevention. These new strategies are just beginning to be explored. In the area of early detection, we must identify biomarkers of high risk, such as specific genotypes. In the area of prevention, new chemopreventives, such as tamoxifen, offer hope to high-risk individuals that cancer can be prevented.
Recommended Reading: How To Massage Own Prostate
Drugs That Stop Androgens From Working
Anti-androgens
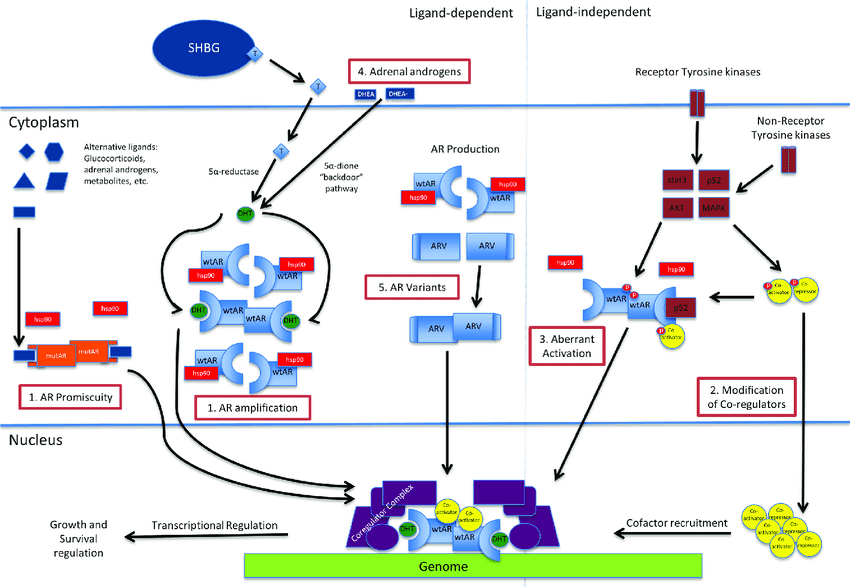
For most prostate cancer cells to grow, androgens have to attach to a protein in the prostate cancer cell called an androgen receptor. Anti-androgens are drugs that also connect;to these receptors, keeping the androgens from causing tumor growth. Anti-androgens are also sometimes called androgen receptor antagonists.
Drugs of this type include:
- Flutamide
They are taken daily as pills.
In the United States, anti-androgens are not often used by themselves:
- An anti-androgen may be added to treatment if orchiectomy or an LHRH agonist or antagonist is no longer working by itself.
- An anti-androgen is also sometimes given for a few weeks when an LHRH agonist is first started to prevent a tumor flare.
- An anti-androgen can also be combined with orchiectomy or an LHRH agonist as first-line hormone therapy. This is called combined androgen blockade . There is still some debate as to whether CAB is more effective in this setting than using orchiectomy or an LHRH agonist alone. If there is a benefit, it appears to be small.
- In some men, if an anti-androgen is no longer working, simply stopping the anti-androgen can cause the cancer to stop growing for a short time. This is called the anti-androgen withdrawal effect, although they are not sure why it happens.
Newer anti-androgens
Enzalutamide , apalutamide and darolutamide are newer types of anti-androgens.
These drugs are taken as pills each day.
Transient Transfection And Luciferase Assays
Transient transfections were done using Lipofectamine per the manufacturer’s protocol using an AR luc in the pGL3-Basic vector and an ER- luc in the pGL2-Basic vector reporter plasmids provided by Donald J. Tindall and Ronald J. Weigel, respectively. Cotransfections were done with 0.5 g of reporter plasmid and 15 ng of Renilla luciferase plasmid , and assays were done after 24 hours using dual-luciferase assay kit . Cells were cotransfected and normalized with Renilla luciferase plasmid . Following transfection, cells were treated with carnosol for 24 hours and samples were prepared per the manufacturer’s protocol.
Read Also: What Does A Prostate Massage Feel Like
Prostate Cancer Hormone Therapy
Prostate cancer depends on testosterone to grow. Hormone therapy blocks or lowers the amount of testosterone in the body.
This can lower the risk of an early prostate cancer coming back when you have it with other treatments. Or, it can shrink an advanced prostate cancer or slow its growth.
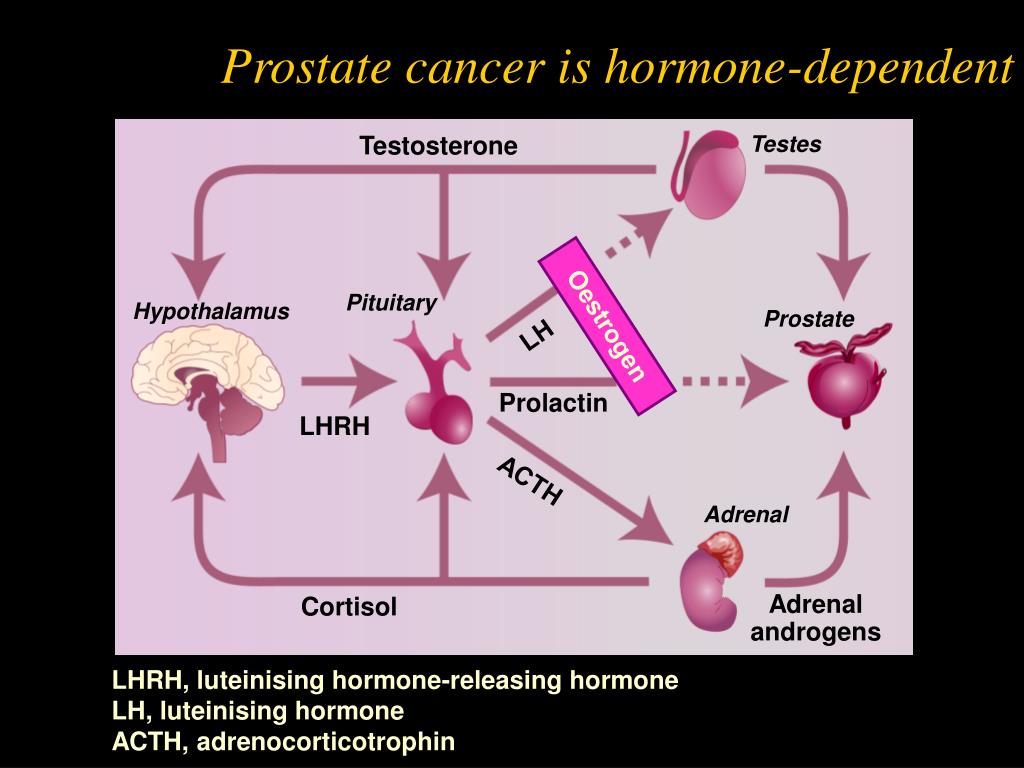
Luteinising hormone releasing hormone agonists or LH blockers
A gland in the brain called the pituitary gland produces luteinising hormone . This controls the amount of testosterone made by the testicles.
LH blockers are drugs that stop the production of luteinising hormone. They do this by blocking the signal from the pituitary gland to the testicles. So the testicles stop making testosterone.
Types for prostate cancer include goserelin , leuprorelin and triptorelin .
Anti androgens
Prostate cancer cells have areas called receptors. Testosterone attaches to these receptors and that can encourage the cells to divide so that the cancer grows.
Anti androgen drugs work by attaching themselves to these receptors. This stops testosterone from reaching the prostate cancer cells.
There are different types of anti androgens including bicalutamide , cyproterone acetate and flutamide .
Gonadotrophin releasing hormone blocker
Gonadotrophin releasing hormone blockers stop messages from a part of the brain called the hypothalamus that tell the pituitary gland to produce luteinising hormone.
Other hormone therapies;
There are other newer hormonal treatments for prostate cancer. These therapies include:
Questions To Ask Your Doctor Or Nurse
- What is the aim of treatment?
- What type of hormone therapy are you recommending for me and why?
- How often will I have my injections or implants?
- How will my treatment be monitored?
- How long will it be before we know if the hormone therapy is working?
- What are the possible side effects, and how long will they last?
- What will happen if I decide to stop my treatment?
- Are there any clinical trials that I could take part in?
Also Check: How Does Prostate Cancer Kill
Is Hormonal Cancer Hereditary
Cancer is not usually inherited, but some types mainly breast, ovarian, colorectal and prostate cancer can be strongly influenced by genes and can run in families. We all carry certain genes that are normally protective against cancer. These genes correct any DNA damage that naturally happens when cells divide.
Modulation Of Androgenar Axis In The Treatment Of Prostate Cancer
As androgens stimulate the growth and survival of prostate cancer cells, the goal of hormonal therapy in prostate cancer is to deprive these cancer cells of androgen so that they die due to apoptosis . Therefore, regression of an androgen-dependent prostate tumor is induced either medically with luteinizing hormone-releasing hormone analogues or surgically by orchiectomy, which reduces the intracellular concentration of DHT . This in turn results in the death of androgen-sensitive cancer cells . Thus, androgen deprivation slows the progression of the tumor and enhances the quality of life. However, with time the disease inevitably recurs, and importantly, CRPC still remains dependent on the AR as discussed above .
Recommended Reading: How Far In Is Your Prostate
Chromatin Immunoprecipitation Followed By Massively Parallel Dna Sequencing
Breast cancer PDEs cultured in complete medium containing vehicle , 17-estradiol , or synthetic PGR agonist R5020 for 72;h were harvested, crosslinked, and processed for ChIP-seq analysis as described previously . The estrogen receptor alpha HC-20 antibody was used for immunoprecipitation of ER from PDE tissue lysates. Sequences generated by an Illumina HiSeq 2000 were processed by the Illumina analysis pipeline version 1.6.1 and aligned to the Human Reference Genome using BWA version 0.5.5 . Reads were filtered by removing those with a BWA alignment quality score less than 15. Enriched ER binding regions were identified by comparing ER ChIP DNA samples to total ChIP input DNA. ER ChIP-sequencing was then performed from each PDE tissue and treatment. Peak calling was performed using MACS2 version 1.4.0rc2 .
How Does Hormone Therapy Work Against Prostate Cancer
Early in their development, prostate cancers need androgens to grow. Hormone therapies, which are treatments that decrease androgen levels or block androgen action, can inhibit the growth of such prostate cancers, which are therefore called castration sensitive, androgen dependent, or androgen sensitive.
Most prostate cancers eventually stop responding to hormone therapy and become castration resistant. That is, they continue to grow even when androgen levels in the body are extremely low or undetectable. In the past, these tumors were also called hormone resistant, androgen independent, or hormone refractory; however, these terms are rarely used now because the tumors are not truly independent of androgens for their growth. In fact, some newer hormone therapies have become available that can be used to treat tumors that have become castration resistant.;
Recommended Reading: What Is Super Beta Prostate
When Is Hormone Therapy Used For Prostate Cancer
On its own, hormone therapy can be a good way to control the growth of your prostate cancer. It can also be used with another prostate cancer treatment to help it work better. You should keep in mind that the following things will affect when you have hormone therapy and if you have hormone therapy along with another type of prostate cancer treatment:
- The grade of your prostate cancer
- Your Gleason score
- The stage of your prostate cancer
- Your PSA level
- Your age
- Your general health
Your stage, grade, and Gleason score are determined by a pathologist. A pathologist is a specially trained physician who reviews biopsy results in order to find changes in your body caused by cancer. When you had your prostate biopsy, the pathologist looked at the tissue samples taken from your prostate gland and prepared your biopsy report. The report tells you and your doctor the following information:
- The grade tells you what your prostate cancer cells look like.
- The Gleason score. The Gleason score tells you what your prostate cancer cells look like compared to healthy cells and gives you an idea of how quickly your cancer is growing. Your Gleason score will range from 2 to 10.
- The stage tells how much prostate cancer you have and where your cancer is located.
This information is used to help your doctor chose the most effective type of hormone therapy for you. The types of hormone therapy include:
Neoadjuvant hormone therapy
Adjuvant hormone therapy
Salvage hormone therapy
What Are The Side Effects Of Hormone Therapy
Like all treatments, hormone therapy can cause side effects. These are usually caused by low testosterone levels.
Hormone therapy affects men in different ways and you may not get all of the possible side effects. Some men only get a few side effects or dont get any at all. This doesnt mean that the treatment isnt working.
Some men find their side effects improve or get easier to manage the longer theyre on hormone therapy. But if side effects dont improve, there are usually ways to manage them.
Side effects will usually last for as long as youre on hormone therapy. If you stop using it, the side effects should improve as your testosterone levels start to rise again.
Your side effects wont stop straight away it may take several months or years. For some men, the side effects may never go away completely.
The risk of getting each side effect depends on your type of hormone therapy and how long you take it for. If you have hormone therapy alongside another treatment, you may get side effects from that treatment as well.
Surgery to remove the testicles cant be reversed, so the side effects will be permanent. But there are treatments to help manage them.
Discuss the possible side effects with your doctor or nurse before you start or change your hormone therapy, or call our;Specialist Nurses. If you know what side effects you might get, it can be easier to manage them.
Read more about;prostate cancer and your sex life.
Weight gain
Strength and muscle loss
Bone thinning
Recommended Reading: How To Treat Prostate Cancer That Has Spread To Bones
