Gleason 6 Prostate Cancer: Serious Malignancy Or Toothless Lion
Nicholas M. Donin, MDOncology
There is strong evidence from longitudinal cohort studies of men with both treated and untreated Gleason 6 prostate cancer to suggest that Gleason 6 disease, when not associated with higher-grade cancer, virtually never demonstrates the ability to metastasize and thus represents an indolent entity that does not require treatment.
Autopsy studies of men without known prostate cancer suggest that a substantial reservoir of prostate cancer that does not cause symptoms or death exists within the population. The majority of these cancers are Gleason 6 tumors and are frequently detected by prostate-specific antigenbased prostate cancer screening. There is strong evidence from longitudinal cohort studies of men with both treated and untreated Gleason 6 prostate cancer to suggest that Gleason 6 disease, when not associated with higher-grade cancer, virtually never demonstrates the ability to metastasize and thus represents an indolent entity that does not require treatment. Whether Gleason 6 has a propensity to progress to higher-grade cancer is still under investigation. Because the term cancer has historically been used to represent a disease state that leads to progressive illness that is uniformly fatal without treatment, we believe Gleason 6 disease should not be labeled with this term. Our challenge now is to develop the technology to differentiate true Gleason 6 disease from the higher grades of dysplasia with which it can be associated.
Understanding Your Pathology Report: Prostate Cancer
When your prostate was biopsied, the samples taken were studied under the microscope by a specialized doctor with many years of training called a pathologist. The pathologist sends your doctor a report that gives a diagnosis for each sample taken. Information in this report will be used to help manage your care. The questions and answers that follow are meant to help you understand medical language you might find in the pathology report from your prostate biopsy.
Also Check: How To Cure Prostate Enlargement
Initial Treatment Of Prostate Cancer By Stage And Risk Group
The stage of your cancer is one of the most important factors in choosing the best way to treat it. Prostate cancer is staged based on the extent of the cancer and the PSA level and Gleason score when it is first diagnosed.
For prostate cancers that haven’t spread , doctors also use risk groups to help determine if more tests should be done and to help guide treatment options. Risk groups range from very-low-risk to very-high-risk, with cancers in the lower risk groups having a smaller chance of growing and spreading compared to those in higher risk groups.
Other factors, such as your age, overall health, life expectancy, and personal preferences are also important when looking at treatment options. In fact, many doctors determine a mans possible treatment options based not just on the stage, but on the risk of cancer coming back after the initial treatment and on the mans life expectancy.
You might want to ask your doctor what factors he or she is considering when discussing your treatment options. Some doctors might recommend options that are different from those listed here. Taking part in a clinical trial of newer treatments is also an option for many men with prostate cancer.
Jump to
Don’t Miss: What Color Represents Prostate Cancer
The Gleason Grading System
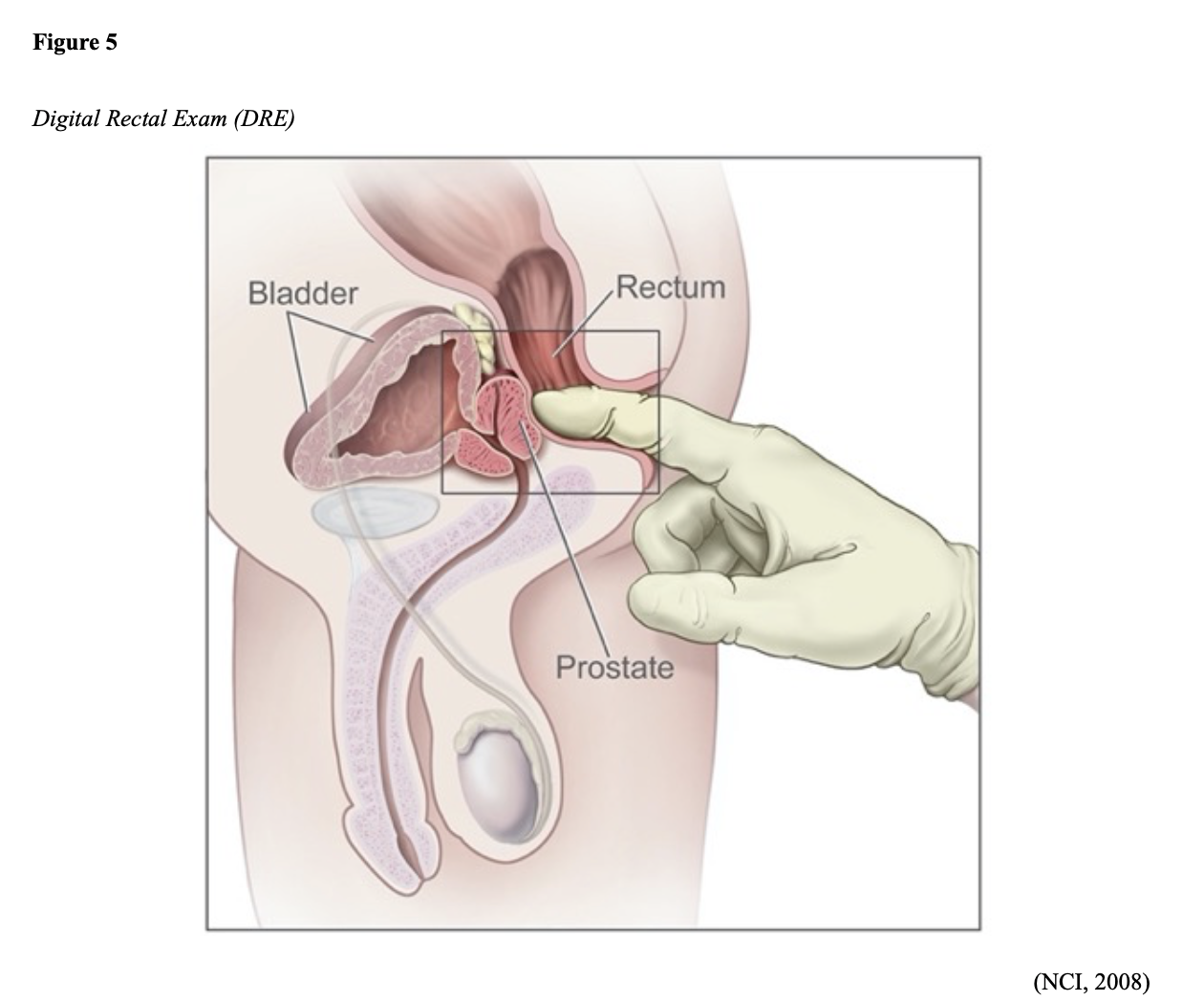
Screening for prostate cancer involves the prostate-specific antigen test and a digital rectal exam. If results are suspect, your doctor may recommend a prostate biopsythe only way to confirm the diagnosis.
During a prostate biopsy, a urologist uses a small needle to remove tissue samples from different parts of the prostate. These samplesalso called coresare then sent to a pathologist so they can review each one under a microscope.
The pathologist uses a pattern scale, developed by Donald Gleason, MD, PhD in 1966, to give each sample a grade from 1 to 5. Grade 1 cells are well-differentiated and look like normal tissue. Grade 5 cells, on the other hand, are “poorly differentiated” or even unrecognizable from normal tissue.
Your Gleason score is the sum of the two numbers that represent the most common types of tissue found in your biopsy. The first number in the equation is the most common grade present, the second number is the second most common grade. For example, if seven of your cores are grade 5 and five are grade 4, your Gleason score would be 5+4, or a Gleason 9.
Today, pathologists typically only flag tissue samples that are grade 3 or higher, making 6 the lowest Gleason score.
In 2014, a revised grading system for prostate cancercalled Grade Groupswas established. This system builds on the Gleason scoring system and breaks prostate cancer into five groups based on risk. This can help make it easier to understand the Gleason score scale.
What Does It Mean When There Are Different Core Samples With Different Gleason Scores
Cores may be samples from different areas of the same tumor or different tumors in the prostate. Because the grade may vary within the same tumor or between different tumors, different samples taken from your prostate may have different Gleason scores. Typically, the highest Gleason score will be the one used by your doctor for predicting your prognosis and deciding on treatment options.
Don’t Miss: How To Tell If You Have Prostate Infection
Is Gleason 6 Cancer
The Gleason score has been the universal grading system for prostate cancer for half a century. In the late 1960s, Donald Gleason developed his classic grading system, which was solely based on the classification of tumor growth patterns and is unique in taking account of tumor heterogeneity.
In 2005 the International Society of Urologic Pathology significantly modified the Gleason grading system. This modification resulted from alterations in clinical presentation and pathological diagnosis of prostate cancer in the preceding 40 years in Gleasons day prostate cancer was commonly discovered at a late stage or incidentally at transurethral resection for hyperplasia, since Prostate Specific Antigen was only introduced in the late 1980s. Immunohisto-chemistry for basal cells was not included in the pathologic diagnosis of lesions suspicious for prostate cancer at that time. Many closely packed, slightly atypical glands originally classified as Gleason grade 1 or 2 probably represented atypical adenomatous hyperplasia since immunohistochemical staining for basal cells is a prerequisite for differentiating these lesions. In November 2014, the ISUP updated the Gleason grading system again with relatively minor changes in relation to the 2005 modification.
Figure 1: Gleason score 6 prostate cancer glands with expansion into extra-prostatic fat tissue . Hematoxylin & Eosin, 200x
Prostate Cancer Risk Groups
In addition to stage, doctors may use other prognostic factors to help plan the best treatment and predict how successful treatment will be. Examples of these include the National Comprehensive Cancer Network risk group categories and the Cancer of the Prostate Risk Assessment risk score from University of California, San Francisco.
Information about the cancers stage and other prognostic factors will help the doctor recommend a specific treatment plan. The next section in this guide is Types of Treatment. Use the menu to choose a different section to read in this guide.
Don’t Miss: Can A Man Have Sex If His Prostate Is Removed
Eggener Et Al Respond:
Matthew R. Cooperberg, MD, MPH
Scott Eggener, MD
Gladell Paner, MD
Andrew Vickers, PhD
Berlin is a member of the Cancer Clinical Research Unit at Princess Margaret Cancer Centre and an affiliate scientist at Techna Institute for Advancement of Technology for Health in Toronto, Canada. Cooperberg is a professor of urology epidemiology & biostatistics and Helen Diller Family Chair in Urology at the University of California, San Francisco. Eggener is the Bruce and Beth White Family Professor of Surgery anddirector of the High Risk and Advanced Prostate Cancer Clinic at the University of Chicago, Illinois. Paner is a professor of pathology at the University of Chicago. Vickers is an attending research methodologist at Memorial Sloan Kettering Cancer Center in New York City, New York.
To the editor,
We would like to thank Harris et al for their interest in our work. The authors provide an excellent summary of the main counterarguments to eliminating the term cancer when describing a prostate tumor with only pattern 3 disease . Indeed, many of these arguments have been made before in the published literature.1 We address these below. We also encourage readers to review the entirety of our proposal.2
1. Argument: You have to call Gleason 6 cancer because of the possibility of misgrading due to inadequate sampling: Patients from low-grade grade group 1 to higher grade 3/4/5 sampling errorat biopsy.
References
Related Content:
What Is A Bad Gleason Score For Prostate Cancer
Gleason scores aren’t good or bad, per se. They predict how quickly your prostate cancer might grow. Tumors with higher Gleason scores are likely to grow quickly. And Gleason scores aren’t the only factors healthcare providers consider when creating your treatment plan.
What other factors do healthcare providers consider?
Providers consider the results of other tests and additional biopsy information. For example, when you had your biopsy, your healthcare provider obtained several samples or cores from your prostate. They checked how many cores contained cancer and whether most of the cells in the cores were cancerous cells.
Other factors may include:
Don’t Miss: Enlarged Prostate Blocking Urine Flow
A Roundtable Discussion With Brian F Chapin Md Jonathan I Epstein Md And Maha Hussain Md Facp Fasco
Physician-Patient Communication Oncologist counsels patient about options for treatment of prostate cancer. Photo courtesy of Thinkstock.
Prior to ASCOs 2016 endorsement of the Cancer Care Ontario guideline on active surveillance in the management of localized prostate cancer,1 most menover 90%diagnosed with low-risk localized disease were treated with active therapy.2 Today, about 50% of American men with low-risk disease opt for active surveillance instead of therapy. In Sweden, nearly 80% of men with low-risk prostate cancer undergo surveillance rather than treatment.3
This year, approximately 165,000 men in the United States will be diagnosed with prostate cancer,4 and half of those men will have low-risk tumors that pathologists rate as Gleason 6 disease. Changes to the Gleason score grading system in 2014 by the International Society of Urological Pathology classified Gleason 6 as grade 1, putting the cancer in the very lowrisk category.
Strong evidence suggests that Gleason 6 disease, when not associated with higher-grade cancer, almost never develops into aggressive cancer requiring treatment. Thus, many patients with Gleason 6 cancer are able to sidestep therapy, such as surgery and radiation therapy, and its attendant side effects, including sexual, urinary, and bowel dysfunction, for active surveillance, which is increasingly being adopted as the standard of care for men with a Gleason 6 score.
Defining Gleason 6 Cancer
Managing Localized Prostate Cancer
Active Surveillance For Gleason 6 Cancer
Per the Cancer Care Ontario guideline,1 active surveillance for patients with Gleason 6 disease should include:
- PSA testing every 3 to 6 months
- Annual digital rectal exam
- 12- to 14-core confirmatory transrectal ultrasound biopsy, including anterior-directed cores, within 6 to 12 months of starting surveillance, and then a serial biopsy every 3 to 5 years thereafter
REFERENCES
1. Chen RC, Rumble RB, Loblaw DA, et al: Active surveillance for the management of localized prostate cancer : American Society of Clinical Oncology Clinical Practice Guideline Endorsement. J Clin Oncol 32:2182-2190, 2016.
2. Cooperberg MR, Broering JM, Carroll PR: Time trends and local variation in primary treatment of localized prostate cancer. J Clin Oncol 28:1117-1123, 2010.
3. Loeb S, Folkvaljon Y, Curnyn C, et al: Uptake of active surveillance for very low-risk prostate cancer in Sweden. JAMA Oncol 3:1393-1398, 2016.
4. American Cancer Society: Key statistics for prostate cancer. Available at www.cancer.org/cancer/prostate-cancer/about/key-statistics.html. Accessed June 26, 2018.
5. Morash C, Tey R, Agbassi C, et al: Active surveillance for the management of localized prostate cancer. Available at www.cancercareontario.ca/en/guidelines-advice/types-of-cancer/2286. Accessed June 26, 2018.
6. Hamdy FC, Donovan JL, Lane JA, et al: 10-Year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N Engl J Med 375:1415-1424, 2016.
Also Check: Can Prostate Cancer Be Hereditary
Does Untreated Clinical Gleason 6 Disease Cause Symptoms Or Death
Several studies that examined the natural history of untreated prostate cancer diagnosed in the prePSA screening era have suggested that men with Gleason 6 cancers are at risk for prostate cancerspecific mortality beyond 10 years of follow-up. The majority of the Gleason 6 disease was T1a/b disease, which was identified at the time of transurethral resection of the prostate for benign disease. Today, it is extremely rare to diagnose T1a/b disease because fewer TURPs are performed and those undergoing TURP have been prescreened with PSA testing. The results of the natural history studies in the PSA screening era are also problematic because many of the cases were likely misclassified at the outset because of the aforementioned limitations attributable to the random-systematic tissue sampling guided by TRUS.
With reported median follow-up ranging from 22 to 82 months, current active surveillance cohorts remain immature at this time, and longer follow-up will be necessary to draw definitive conclusions. Thus far, cancer-specific survival among these cohorts has been > 97%, and there are no data to suggest inferior outcomes after delayed radical therapy, as compared with immediate therapy.
Molecular Progression Of Gleason 6 Prostate Cancer: Tracking Of Specific Clones By Image
![[1/3] AI based Gleason Grading for Prostate Cancer [1/3] AI based Gleason Grading for Prostate Cancer](https://img.healthyprostateclub.com/wp-content/uploads/13-ai-based-gleason-grading-for-prostate-cancer-by-zsfvishnu-medium.jpeg)
Abstract: PD08-07
Introduction
Magnetic resonance imaging/ultrasound fusion biopsy may be used to follow men during active surveillance . Repeat sampling of the same biopsy site is theoretically possible . However, the ability to sample the same clonal focus of cancer over time is unknown. Using next generation sequencing , we sought to determine if a clonal focus can be tracked serially and if so, is there evidence that cancer progression at the molecular level can occur.
Methods
31 men with Gleason 6 prostate cancer were enrolled in an IRB-approved registry for AS. Subjects underwent MRI/US fusion biopsy at study entry and re-sampling of the tracked biopsy site 1 year later. Immunohistochemistry and targeted RNA/DNA NGS on routine formalin-fixed paraffin-embedded prostate biopsy tissues obtained at both time points were performed. ETS gene fusion status, a marker of CaP clonality and common oncogenic alterations associated with human cancer were assessed.
Results
Read Also: Does An Enlarged Prostate Affect Pooping
Can Gleason 6 Progress To Higher
Currently available data regarding the potential for progression of Gleason 6 disease during its untreated natural history are conflicting. Epidemiologic evidence exists to support the concept of a nonprogressive and benign indolent course as well as a progressive course in which more aggressive disease can develop from initially low-risk lesions.
Its Not Aggressive And May Never Need Treatment But Then Again It Might
- Prostate Cancer Basics
- Patient Resources
Dont worry about Gleason 3+3=6 ! Its harmless! We shouldnt even call it cancer! In fact, lets call it IDLE !
Many patients have heard reassurances like these, and yes, if you have to have prostate cancer, Gleason 6 is the best kind to have.
But wait: Lets not call it not cancer, says Johns Hopkins urologic pathologist Jonathan Epstein, M.D. There are some very good reasons to keep the cancer designation for Grade Group 1. Epstein should know he is the originator of the Grade Group system of prostate cancer grading, a system that has been adopted worldwide.
Gleason Score and Grade Group
Under the microscope, he explains, Grade Group 1 cancer has some of the same behaviors as higher-grade cancer. Even though it is not aggressive, it can still invade nerves, go out of the prostate, and rarely, can invade the seminal vesicles. Molecularly, it has many of the hallmarks associated with higher-grade cancer, and has certain features that you do not see in benign prostate glands.
Finally, a name change may not even be that meaningful today, Epstein continues. Grade Group 1 is more intuitive to patients as lowest-grade cancer. With greater acceptance of active surveillance, patients are understanding that not all cancers are the same, that not everyone needs treatment right away or ever and that low-grade cancer can be followed carefully and safely.
Gleason Score and Grade Group
- Prostate Cancer Basics
Read Also: Which Lymph Nodes Does Prostate Cancer Spread To
What Are Grade Groups
Grade Groups are a new way to grade prostate cancer to address some of the issues with the Gleason grading system.
As noted above, currently in practice the lowest Gleason score that is given is a 6, despite the Gleason grades ranging in theory from 2 to 10. This understandably leads some patients to think that their cancer on biopsy is in the middle of the grade scale. This can compound their worry about their diagnosis and make them more likely to feel that they need to be treated right away.
Another problem with the Gleason grading system is that the Gleason scores are often divided into only 3 groups . This is not accurate, since Gleason score 7 is made up of two grades , with the latter having a much worse prognosis. Similarly, Gleason scores of 9 or 10 have a worse prognosis than Gleason score 8.
To account for these differences, the Grade Groups range from 1 to 5 :
- Grade Group 1 = Gleason 6
- Grade Group 2 = Gleason 3+4=7
- Grade Group 3 = Gleason 4+3=7
- Grade Group 4 = Gleason 8
- Grade Group 5 = Gleason 9-10
Although eventually the Grade Group system may replace the Gleason system, the two systems are currently reported side-by-side.
Movement Builds To Classify Gleason 6 Prostate Lesions As Nonmalignant
In prostate cancer, as in life, you roll the dice.
In craps, 3+3 is called a âhard six.â Itâs hard because you can only win if you repeat with a combination of 3+3. Any other sixes you roll â 4+2, 5+1 â are losers.
Gleason 3+3 is a hard six in prostate cancer. It is the lowest grade cancer in the traditional Gleason scoring system. Still, to the eye of a pathologist, a Gleason 6 looks like a malignancy.
Now, a few experts are questioning whether this hard six is a cancer at all. Some urologists see a Gleason 6 as a noncancerous growth that has the potential to be invasive, but most likely will never spread to other organs or end up killing a man.
To a patient like me, who has been on active surveillance for 10 years, a Gleason 6 can create a big medical fuss lasting years with regular prostate-specific antigen blood tests, digital rectal exams , biopsies, and MRIs. It can cause âanxious surveillanceâ that prompts them to drop AS and undergo unnecessary radical prostatectomy, which poses a potential risk of impotence and urinary incontinence.
The Gleason 6 diagnosis can yield polar opposite recommendations from urologists. Ten years ago, I found this to be the case in the matter of a day.
On December 14, 2010, a local urologist recommended I undergo a radical prostatectomy within the week. When asked, he said he didnât support active AS, then a relatively new approach for monitoring low-grade prostate cancer.
âThe right thing to doâ
Mixed reactions
Also Check: Is Cranberry Juice Good For Prostate Infection
