Cancer Vaccines Modified By Oncolytic Newcastle Disease Virus
Cancer vaccines can be modified by virus infection in order to increase their immunogenicity. This has been exemplified with NDV. Two types of such vaccine were developed over many years: ATV-NDV, an autologous tumor cell vaccine modified by infection with a lentogenic strain of NDV , and IO-VACR, a dendritic cell vaccine modified by loading with oncolysate from patient-derived tumor cells infected with a mesogenic oncolytic strain of NDV .
6.3.1. Mechanism of Action
In a pre-clinical animal tumor model, post-operative vaccination with ATV-NDV but not with ATV without virus infection caused long-term protective anti-tumor immunity . ATV-NDV strongly augmented a tumor-specific T cell response as a result of CD4+ and CD8+ immune T cell interaction . In addition to the response activation via T-T cooperation, NDV of the vaccine caused induction of type I interferons which play an important role in the generation of a CTL response .
In a clinical study, post-operative vaccination with ATV-NDV of primary glioblastoma multiforme patients caused: increase of skin anti-tumor delayed-type hypersensitivity reactivity, an increase in the numbers of cancer-reactive memory T cells in the peripheral blood, and an increase of CD8+ tumor-infiltrating lymphocytes in recurrent brain tumor tissue .
6.3.2. Side Effects
Kenworth W900 For Sale
Managing the sideeffects of hormone therapy 14 Loss of sex drive and erectile dysfunction 15 Hot flushes 20 Bone thinning 24 Breast swelling and tenderness 26 For men with prostatecancer, hormone therapy can be used to control the balance of the male hormone testosterone. Mar 15, 2021 · The standard treatmentfor prostate cancer that has come back after prostatectomy is radiation therapy, either alone or with the addition of hormonetherapy. Because hormonetherapy can cause distressing sideeffectsincluding hot flashes, loss of energy, and loss of sexual desirethe treatment is typically reserved for patients with . Hormonetherapyfor prostatecancer can cause weight gain. You may notice that body fat starts to increase in certain areas, particularly around the breast. This may give your body a more feminine look that can be upsetting for some men. Discuss any changes in your body shape with your doctor or nursing team, particularly if they are worrying .
Also Check: Sleeping Pills And Enlarged Prostate
High Intensity Focused Ultrasound
High intensity focused ultrasound was first used in the 1940s and 1950s in efforts to destroy tumors in the central nervous system. Since then, HIFU has been shown to be effective at destroying malignant tissue in the brain, prostate, spleen, liver, kidney, breast, and bone.
HIFU for prostate cancer utilizes ultrasound to ablate/destroy the tissue of the prostate. During the HIFU procedure, sound waves are used to heat the prostate tissue, thus destroying the cancerous cells. In essence, ultrasonic waves are focused on specific areas of the prostate to eliminate the prostate cancer, with minimal risks of affecting other tissue or organs. Temperatures at the focal point of the sound waves can exceed 100 °C . However, many studies of HIFU were performed by manufacturers of HIFU devices, or members of manufacturers advisory panels.
Contraindications to HIFU for prostate cancer include a prostate volume larger than 40 grams, which can prevent targeted HIFU waves from reaching the anterior and anterobasal regions of the prostate, anatomic or pathologic conditions that may interfere with the introduction or displacement of the HIFU probe into the rectum, and high-volume calcification within the prostate, which can lead to HIFU scattering and transmission impairment.
Recommended Reading: Hormone Resistant Prostate Cancer Treatment
Common Side Effects Of Immunotherapy
Immunotherapy side effects can vary according to the type of treatment and can also be influenced by the location and type of cancer as well as a patients overall health. Before treatment, patients should consult their oncologist and care team to gain a better and fuller understanding of the potential side effects and potential risks associated with specific immunotherapies.
In general, the side effects most commonly experienced across the spectrum of the current FDA-approved immunotherapies may include but are not limited to:
- Infusion-related reaction / injection site pain
Explore side effects specific to certain types of immunotherapies
Chimeric Antigen Receptor T
Another emerging field that has shown promise is chimeric antigen receptor T-cell therapy. CAR-T therapy involves taking a patients T cells, engineering them to express a T cell receptor directed against a certain antigen, expanding the cells, and reinfusing them back into the patient. CAR-Ts directed against CD19 have been approved for the treatment of relapsed/refractory acute lymphoblastic leukemia and diffuse large B-cell lymphoma. CAR-Ts are also designed to express costimulatory domains, which may interact with ligands or receptors on antigen-presenting cells, tumor cells, or on the T cell itself .
Read Also: First Line Treatment For Prostate Cancer
Table : Survival Benefits Of Early Treatment
An analysis of 98 men with prostate cancer that had spread to the lymph nodes, who were randomly assigned to receive immediate hormone therapy or to forgo it until the disease spread further to bones or lungs, found that early treatment saved lives.
Deaths from prostate cancer 21 Source: Lancet Oncology 2006 7:4729. PMID: 16750497.
Other studies have shown that starting hormone therapy early on increases survival times, delays cancer progression, and results in better quality of life. However, in a review of four studies involving 2,167 men with metastatic prostate cancer, the Cochrane Collaboration concluded that early hormone therapy had offered only a small overall survival advantage over deferred treatment, and cautioned that more research on the issue needs to be done.
Although debate on this issue continues, in most cases I advise my patients with metastatic disease to begin hormone treatment early on. This is particularly important for someone with spine metastases, because a bone fracture or extension of the cancer into the spinal cord area could lead to impaired mobility and even paralysis. Fortunately, this is a rare event.
Side Effects Of Targeted Therapy
Some men may experience side effects such as diarrhea, nausea and low red blood cell counts. Other possible side effects include:
Liver blood tests may also be abnormal.
One of the targeted therapies for prostate cancer, Lynparza® , may increase the risk for blood clots in the lungs and legs. These drugs may also cause a blood cancer such as myelodysplastic syndrome or acute myeloid leukemia, but this is rare.
You May Like: Does Prostate Massage Help Ed
Risk Of Heart Problems
Hormone therapy for prostate cancer might increase the risk of heart problems if you have certain medical conditions.
This may be because some of the side effects of hormone therapy, such as weight gain, can make heart disease worse.
-
Gynecomastia in Patients with Prostate Cancer: A Systematic Review
A Fagerlund and others
Recommended Reading: Pi Rads 4 Lesion Prostate
T Cell In Oc Development
T cells have a dual role in OC development.
- T cells as foes in OC development
- T cells as friends in OC development
On the one hand, T cells can kill cancer cells through antibody dependent cellular cytotoxicity . ADCC occurs when CD16 is present on T cells. CD16 binds to the Fc region of IgGs, which is another T cell target recognition method besides TRAIL and FasL. Binding to target cells may trigger cytotoxicity or other effector functions . The researchers cloned the extracellular domain of V9 V2 T cell receptor from tumor infiltrating lymphocyte in OC and combined it with the Fc domain of human IgG1. This chimeric antibody mediates cell killing through ADCC in a dose-dependent manner. In vivo, this TCR V9 V2-Fc significantly inhibits cancer cell growth and improves survival rate in a human OC xenograft model.
On the other hand, T17 cells are the main source of IL-17 and play an immunosuppressive effect in tumors. T17 cells secrete IL-17, which induces the production of vascular endothelial growth factor and other angiogenesis-related factors. Studies have shown that the OC microenvironment may mobilize and recruit T cells, which secrete large amounts of inflammatory cytokine IL-17A, which reduces cytotoxicity, enhances immunosuppressive activity, establishes an effective immunosuppressive microenvironment, and promotes tumor progression and immune escape.
Fig.1 Antitumor and protumor functions of T cells.
You May Like: What Kind Of Surgery Is Done For An Enlarged Prostate
More Research Needed On Immunotherapy
Knowledge gained from decades of treating autoimmune disorders has informed the ways that doctors identify and manage immune-related side effects, noted Dr. Sharon.
But he pointed out that immunotherapy-related side effects may develop through different biological mechanisms than autoimmune disorders, which suggests that the treatment of these side effects may also differ.
A wide-spread rash on a man with advanced melanoma following combination immune checkpoint inhibitor treatment.
To more effectively explore such questions, doctors and researchers need to establish definitions of immunotherapy-related side effects and develop standards for reporting these side effects as they are observed in patients, Dr. Sharon noted.
Doctors could use definitions of immune-related side effects to identify patients who may need to be referred to specialists for treatment, he added.
In addition to definitions, new biomarkers and tests for diagnosing immune-related side effects are needed, and that will require collaboration from experts across disciplines, he said.
Dr. Sharon was one of the organizers of a scientific workshop on cancer, autoimmunity, and immunology held last year that brought together experts from different fields to discuss a range of topics, including immune-related side effects.
During a keynote presentation at the meeting, Jeffrey Bluestone, Ph.D., of the University of California, San Francisco, said: We still have a lot to learn.
If Youre Having Radiation Therapy To The Pelvis
Radiation therapy to the pelvis can cause side effects such as:
- Bladder problems
- Fertility problems
- Changes in your sex life
You might also have some of the same problems people get from radiation to the abdomen, such as nausea, vomiting, diarrhea, or constipation.
Bladder problems
Radiation to the pelvis can cause problems with urination, including:
- Pain or burning sensations
- Blood in the urine
- An urge to urinate often
Most of these problems get better over time, but radiation therapy can cause longer-term side effects as well:
You May Like: Is Sex Good For Enlarged Prostate
Support Programs And Services
All cancer patients at Mount Sinai have access to specialized support programs and services. These services include palliative care, treatment for pain, and integrative medicine. Integrative medicine involves using complementary and traditional medicine together. Our social workers, psychiatrists, dietitians, chaplains, and experts in palliative care are here to help. We focus on you with individual needs that may change over time. We work with you and your loved ones to evaluate your concerns and develop a personal plan. This plan may include counseling, practical help, education, symptom management, and wellness programs.
Donât Miss: Prognosis Of Prostate Cancer Spread To Bones
What Immunotherapies Are Available As Prostate Cancer Therapy Options

Back in 2011, the FDA approved Sipuleucel-T to treat asymptomatic or minimally symptomatic metastatic castrate-resistant prostate cancer.
Many immunotherapies are on their way to approval, such as PROSTVAC and GVAX.
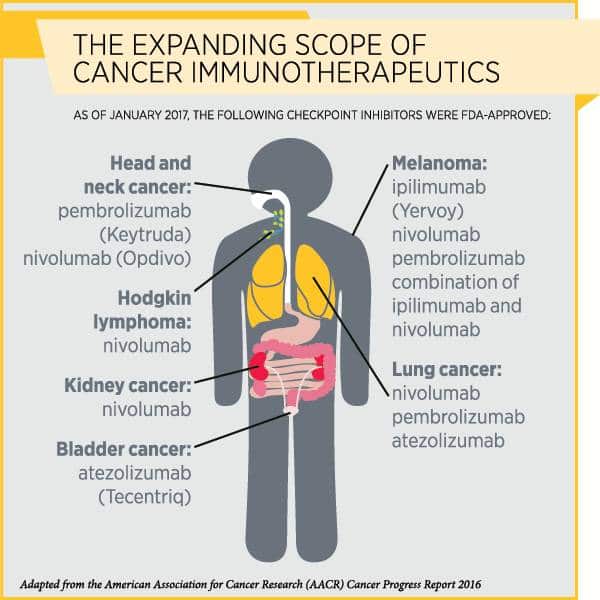
As of right now, the FDA has approved several checkpoint inhibitors for melanoma, Hodgkin lymphoma, and kidney, lung, and bladder cancer. Unfortunately, there are none approved for prostate cancer. However, some of GRUs experts believe we could see checkpoint inhibitors approved for prostate cancer in the near future.
You May Like: Best Treatment For Prostate Enlargement
Prostate Cancer Treatment Options
Conventional treatments for early-stage prostate cancer include surgery and radiation. Hormonal therapy, which can reduce levels of the male hormones that lead to tumor growth, is also used to treat early-stage tumors. For advanced or metastatic prostate cancer, chemotherapy is also a treatment option.
Immunotherapy is class of treatments that take advantage of a persons own immune system to help kill cancer cells. There are currently three FDA-approved immunotherapy options for prostate cancer.
Cancer Vaccines
- Sipuleucel-T : a vaccine composed of patients own immune cells, which have been stimulated to target the PAP protein highly expressed on prostate cancers approved for subsets of patients with advanced prostate cancer
Immunomodulators
- Dostarlimab : a checkpoint inhibitor that targets the PD-1/PD-L1 pathway approved for subsets of patients with advanced prostate cancer that has DNA mismatch repair deficiency
- Pembrolizumab : a checkpoint inhibitor that targets the PD-1/PD-L1 pathway approved for subsets of patients with advanced prostate cancer that has high microsatellite instability , DNA mismatch repair deficiency , or high tumor mutational burden
In cases where the patients prostate cancer is resistant to testosterone level reduction via hormone therapy, treatment options are few. Several immunotherapy options are currently in clinical trials for patients with advanced prostate cancer.
The Right Way To Do It
For immunotherapies to deliver the greatest value, they will need to be targeted to the right people. Prostate is going to be an immunologically responsive disease, says Haas. We just need to better divide the patient populations. This sort of personalization is already common in treatment of breast, kidney and skin cancers, but is lagging in prostate cancer.
Drake, however, thinks that it shouldnt be necessary to limit treatments to small groups of people whose tumours fit a narrow set of criteria. We dont select patients for chemo for prostate cancer it just works, he says. If we had an effective combination regimen with immunotherapy, we could probably help the majority of patients.
There is growing consensus that the timing of an immunological intervention could be crucial. Most immunotherapy approaches have been taken in patients with quite advanced disease, says Haas. But the longer a cancer fights off a patients immune system, the more entrenched it can become. In advanced tumours, there arent a lot of T cells, says McNeel. Maybe weve been targeting the wrong stage of the disease. He suggests that it might be better to deploy immunotherapy immediately after surgery or radiation therapy, to prevent the disease coming back. There are also hints that radiotherapy might prime the immune system, perhaps by cracking open cancer cells and inducing an immune response.
More from Nature Outlooks
Nature609, S42-S44
Don’t Miss: Prostate Cancer And Thigh Pain
A Biopsy Is Done To Diagnose Prostate Cancer And Find Out The Grade Of The Cancer
A transrectal biopsy is used to diagnose prostate cancer. A transrectal biopsy is the removal of tissue from the prostate by inserting a thin needle through the rectum and into the prostate. This procedure may be done using transrectal ultrasound or transrectal MRI to help guide where samples of tissue are taken from. A pathologist views the tissue under a microscope to look for cancer cells.
Sometimes a biopsy is done using a sample of tissue that was removed during a transurethral resection of the prostate to treat benign prostatic hyperplasia.
If cancer is found, the pathologist will give the cancer a grade. The grade of the cancer describes how abnormal the cancer cells look under a microscope and how quickly the cancer is likely to grow and spread. The grade of the cancer is called the Gleason score.
To give the cancer a grade, the pathologist checks the prostate tissue samples to see how much the tumor tissue is like the normal prostate tissue and to find the two main cell patterns. The primary pattern describes the most common tissue pattern, and the secondary pattern describes the next most common pattern. Each pattern is given a grade from 3 to 5, with grade 3 looking the most like normal prostate tissue and grade 5 looking the most abnormal. The two grades are then added to get a Gleason score.
Hormone Treatment Side Effects
While hormone therapy is among the most effective forms of systemic therapy for prostate cancer, any man considering hormone therapy should weigh the risks and benefits of the treatment, including possible side effects.
Most hormone therapies cause similar side effects due to changes in the levels of hormones . The side effects of medicine-based hormone therapy and the time it takes to get over some of them depend on the type of medicine, the dose, the length of time itâs given and your overall health.
Similar side effects can occur with surgical removal of the testicles . Though orchiectomy is a simple outpatient procedure, it also has the typical side effects and risks associated with surgery, including risks for bleeding and infection.
Read Also: How To Ejaculate From Prostate Massage
How Long Do Immunotherapy Side Effects Last
The long-term side effects of immunotherapy vary from patient to patient. While the majority of immunotherapy side effects often can be temporary and reversible, some of side effects may persist after treatment because immunotherapy can influence the activity of immune cells that remain in the body long after the drug has been cleared from the patients system. In rare cases, the consequences of immunotherapy side effects may be permanent.
How Effective Is Immunotherapy
Success rates for any cancer treatment, including immunotherapy, depend on individual factors, including the cancer type and stage. In general, immunotherapy is effective against many cancers. While some cancers are more immunogenic than others, in general, immunotherapy is effective across a wide variety of cancers. Immunotherapy can produce durable responses unlike chemotherapy or radiation, however, these occur only in around 25% patients.
Some research suggests that the immune system may remember cancer cells after immunotherapy ends.
You May Like: Metastatic Hormone Sensitive Prostate Cancer
Inflammatory Responses In The Prostate
Inflammation is an innate response to harmful stimuli, such as infections, tissue damage, or tissue malfunction . The main goal with the inflammatory process is to clear the potential threat and restore tissue homeostasis. This normally occurs in two phases the recognition and elimination phase and the resolution and repair phase . If the acute response fails in eliminating the inflammatory agents, the inflammation shifts toward a chronic state. Instead of initiating the resolution phase, additional macrophages and lymphocytes are recruited and, depending on the inflammatory inducer, act to remodel the local microenvironment to adapt to an altered tissue homeostasis.
Cancer has been described as a wound that refuses to heal , and today many cancers have been tightly correlated with preceding inflammatory responses . Several lines of evidence support the theory that inflammation also precedes PCa . Proliferative inflammatory atrophy lesions are areas in the prostate with an increased infiltration of inflammatory cells. These regions can merge with prostatic intraepithelial neoplasia, which is considered to be a risk factor for the development of PCa . Also, a correlation with regular intake of non-steroidal anti-inflammatory drugs and reduced PCa risk has been observed .
