Early Versus Delayed Treatment
For men who need hormone therapy, such as men whose PSA levels are rising after surgery or radiation or men with advanced prostate cancer who dont yet have symptoms, its not always clear when it is best to start hormone treatment. Some doctors think that hormone therapy works better if its started as soon as possible, even if a man feels well and is not having any symptoms. Some studies have shown that hormone treatment may slow the disease down and perhaps even help men live longer.
But not all doctors agree with this approach. Some are waiting for more evidence of benefit. They feel that because of the side effects of hormone therapy and the chance that the cancer could become resistant to therapy sooner, treatment shouldnt be started until a man has symptoms from the cancer. This issue is being studied.
Relevance Of Trial Data In Real
After decades without significant progress in the treatment landscape of mHSPC, the results of the above-mentioned trials are welcome. Nevertheless, we need to cautiously interpret these results, taking into consideration the between-study heterogeneity in study populations, and how well they reflect our patient population .
Dont Miss: How To Relieve Stress Hormones
Are There Any Complementary Therapies I Should Consider While In Treatment For Metastatic Prostate Cancer
Absolutely! Whenever we can avoid adding a medication butstill provide a benefit, were doing something right.
Acupuncture has been studied by several groups as a way toalter the vasomotor response of the body that causes the hotflash. Some studiessuggest up to a 40 percent reduction in symptoms with an acupuncture treatmentcourse of 5 to 12 weeks.
There has been some interest in using soy products, due toestrogen-like substances they contain. But results generally showed nosignificant improvement.
Multiple additional natural products and herbs have beensuggested, but quality research on these is lacking. You should discuss anysupplement with your doctor before adding it to your regimen.
Also Check: How Long Is Radiation Treatment For Prostate Cancer
Ethics Approval And Consent To Participate
Data collection was undertaken in line with the European Pharmaceutical Marketing Research Association guidelines . The questionnaires used in the Prostate Cancer DSP were reviewed and given exemption by the Western Institutional Review Board . The survey was performed in full accordance with relevant legislation at the time of data collection, including the US Health Insurance Portability and Accountability Act 1996 and the Health Information Technology for Economic and Clinical Health Act legislation . Data were collected according to market research guidelines hence, no source validation was possible or required. Data were collected in such a way that patients and physicians could not be identified directly all data were aggregated, de-identified and anonymized before receipt by Adelphi Real World and therefore informed consent from individual patients was not required.
Treatment To Lower Testicular Androgen Levels
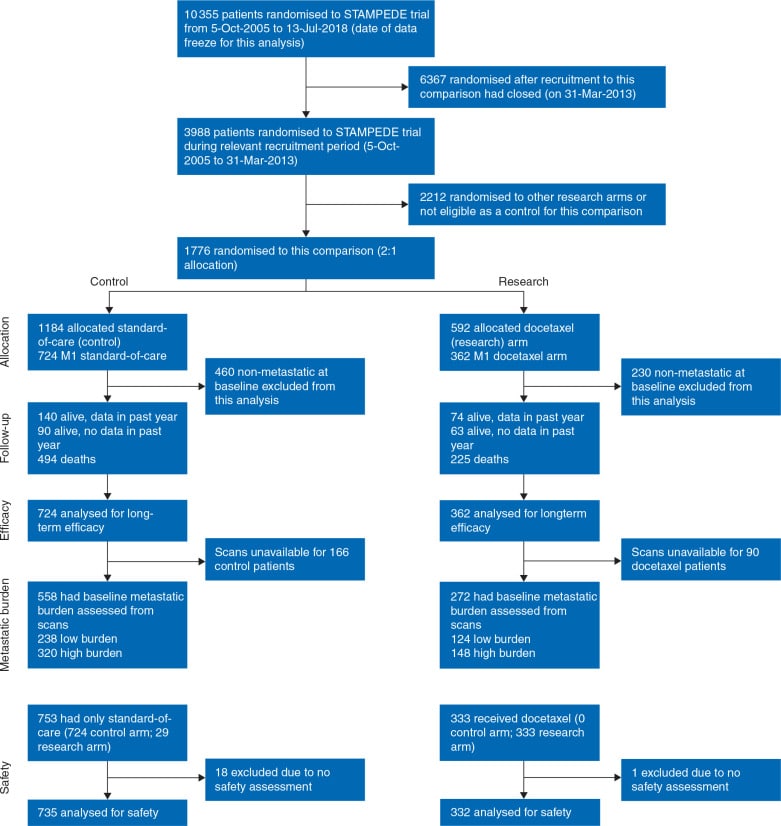
Androgen deprivation therapy, also called ADT, uses surgery or medicines to lower the levels of androgens made by the testicles.
Orchiectomy
Even though this is a type of surgery, its main effect is as a form of hormone therapy. In this operation, the surgeon removes the testicles, where most of the androgens are made. This causes most prostate cancers to stop growing or shrink for a time.
This is done as an outpatient procedure. It is probably the least expensive and simplest form of hormone therapy. But unlike some of the other treatments, it is permanent, and many men have trouble accepting the removal of their testicles. Because of this, they may choose treatment with drugs that lower hormone levels instead.
Some men having this surgery are concerned about how it will look afterward. If wanted, artificial testicles that look much like normal ones can be inserted into the scrotum.
LHRH agonists
Luteinizing hormone-releasing hormone agonists are drugs that lower the amount of testosterone made by the testicles. Treatment with these drugs is sometimes called medical castration because they lower androgen levels just as well as orchiectomy.
With these drugs, the testicles stay in place, but they will shrink over time, and they may even become too small to feel.
- Leuprolide mesylate
LHRH antagonists
Possible side effects
Many side effects of hormone therapy can be prevented or treated. For example:
Read Also: Is Prostate Cancer Estrogen Dependent
How Will I Know That My Hormone Therapy Is Working
Doctors cannot predict how long hormone therapy will be effective in suppressing the growth of any individual mans prostate cancer. Therefore, men who take hormone therapy for more than a few months are regularly tested to determine the level of PSA in their blood. An increase in PSA level may indicate that a mans cancer has started growing again. A PSA level that continues to increase while hormone therapy is successfully keeping androgen levels extremely low is an indicator that a mans prostate cancer has become resistant to the hormone therapy that is currently being used.
How Does Hormone Therapy Work Against Prostate Cancer
Early in their development, prostate cancers need androgens to grow. Hormone therapies, which are treatments that decrease androgen levels or block androgen action, can inhibit the growth of such prostate cancers, which are therefore called castration sensitive, androgen dependent, or androgen sensitive.
Most prostate cancers eventually stop responding to hormone therapy and become castration resistant. That is, they continue to grow even when androgen levels in the body are extremely low or undetectable. In the past, these tumors were also called hormone resistant, androgen independent, or hormone refractory however, these terms are rarely used now because the tumors are not truly independent of androgens for their growth. In fact, some newer hormone therapies have become available that can be used to treat tumors that have become castration resistant.
Recommended Reading: Does Keytruda Treat Prostate Cancer
Definitions And Treatment Landscape
Men who present with mHSPC represent a heterogenous group of patients. Many patients will present with relapse after local treatment, while a minority present with de novo metastatic disease . Metastatic sites and burden of disease will also vary between patients, as will their functional status and presence of cancer-related symptoms.
There are vastly different outcomes between patients, with some prognostic features established at diagnosis while others determined over the course of the treatment. Many of the clinical trials described in this review have attempted to develop prognostic systems for the different subtypes of mHSPC, and the results of individual trial results will need to be interpreted in the context of their study population. The key definitions used in this review are listed in Table 1.
Table 1 Definition of key terminology relating to metastatic hormone-sensitive prostate cancer
Are There Any Lifestyle Changes I Should Consider While In Treatment For Metastatic Prostate Cancer
The most important thing you can do is to stay physicallyactive and strong. This includes following a heart-healthy diet and exercising.
Cardiovascular exercise is the most important. The degree,or intensity and duration, of cardio exercise depends on the individual person.
Several studies have pointed to a link between obesity and aggressive prostate cancer, although the mechanism is still being worked out.
Weight loss is generally encouraged if youre overweight, but excessive or unintentional weight loss can be a sign of disease progression and should be discussed with your doctor.
Finally, if youre a smoker, stop! If youre finding it hardto quit, ask your doctor about products and medications that might help you.
Also Check: Can Cycling Irritate The Prostate
What Factors Will My Oncologist Consider When Recommending A Treatment For Metastatic Prostate Cancer
Doctors consider several factors when determining the right treatment for each patient.
First, the disease is staged, usually with imaging like a:
Second, the symptomatic status of the patient is assessed. Somepeople can have significant pain, mobility limitations, or urinary symptoms dueto metastases or local spread.
Third, the sensitivity of the disease to HMT is determined. This is usually done by measuring PSA and testosteronelevels.
Finally, a discussion between the patient and doctor should focus on the goals of care and treatment options available based on the above factors.
Case : Metastatic Hormone
Alicia Morgans, MD, MPH: Let’s move on to case 2. Case 2 is another patient. This time we’ll have you introduce that patient. Would you mind taking it away, Tanya?
Tanya Dorff, MD: This patient is a 72-year-old gentleman who presented with an initial prostate-specific antigen of 47.5, with potential symptoms of nocturia and low back pain. A bone scan was done due to the high PSA level, 3 bone metastases in the spine and 2 bone metastases in the pelvis. Treatment was started with androgen deprivation therapy as well as up-front docetaxel. He had a good response. His PSA dropped down to 0.3. However, 22 months later, the PSA began to rise again, and there was a progression of his disease noted, so he’s now metastatic castrate-resistant and enzalutamide is initiated.
Alicia Morgans, MD, MPH: Now, Ulka, from your perspective, what do you think about the way the treatments have progressed to this point?
Alicia Morgans, MD, MPH: Thank you for bringing up the triplet. I think that’s really such a new aspect of our treatment paradigm, but for patients who are fit for chemotherapyand we’re proceeding with thatit seems like it’s really such a low burdenas long as there’s not an issue with financials and copaysto just do the simultaneous treatment with the AR -targeted agent and then that maintenance phase.
Alicia Morgans, MD, MPH: Given that, Ulka, what testing and imaging would you order at this point?
Recommended Reading: Is Garlic Good For Prostate Enlargement
What Are The Side Effects Of Hormone Therapy For Prostate Cancer
Because androgens affect many other organs besides the prostate, ADT can have a wide range of side effects , including:
- loss of interest in sex
Studer UE, Whelan P, Albrecht W, et al. Immediate or deferred androgen deprivation for patients with prostate cancer not suitable for local treatment with curative intent: European Organisation for Research and Treatment of Cancer Trial 30891. Journal of Clinical Oncology 2006 24:18681876.
Zelefsky MJ, Eastham JA, Sartor AO. Castration-Resistant Prostate Cancer. In: Vincent T. DeVita J, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles & Practice of Oncology, 9e. Philadelphia, PA: Lippincott Williams & Wilkins 2011.
Smith MR, Saad F, Chowdhury S, et al. Apalutamide and overall survival in prostate cancer. European Urology 2021 79:150158.
Risk Of Bias Assessment
Two investigators independently assessed risk of bias using predefined criteria. Disagreements were resolved by consensus. For randomized trials and cohort studies, methodologists adapted criteria for assessing risk of bias from the U.S. Preventive Services Task Force. Criteria for randomized trials included use of appropriate randomization and allocation concealment methods, baseline comparability of groups, blinding, attrition, and use of intention-to-treat analysis. For cohort studies on prognostic factors, criteria included methods for assembling cohorts, attrition, blinding assessment of outcomes, and adjustment for potential confounding.
The methodology team assessed systematic reviews using AMSTAR 2 criteria. Criteria included use of pre-specified methods, appropriate search methods, assessment of risk of bias, and appropriate synthesis methods. Studies were rated as âlow risk of bias,ââmedium risk of bias,â or âhigh risk of biasâ based on the presence and seriousness of methodological shortcomings.
Studies rated âlow risk of biasâ are generally considered valid. âLow risk of biasâ randomized trials include clear descriptions of the population, setting, interventions, and comparison groups a valid method for allocation of patients to treatment low dropout rates and clear reporting of dropouts blinding of patients, care providers, and outcome assessors and appropriate analysis of outcomes.
Also Check: How Long Do Side Effects Last After Prostate Radiation
Orteronel Misses Goal In Metastatic Hormone
Significant improvement seen in progression-free survival, but not overall survival, with addition of orteronel to androgen deprivation therapy
- HealthDay
You’ve saved your first item
You can find your saved items on your dashboard, in the “saved” tab.
You’ve recommended your first item
Your recommendations help us improve our content suggestions for you and other PracticeUpdate members.
You’ve subscribed to your first topic alert
What does that mean?
In Five Years A Major Treatment Shift
In men diagnosed with metastatic hormone-sensitive prostate cancer, the cancer is typically driven to grow and spread by androgens that are produced largely in the testes. For many years, treatments that block androgen production have been a mainstay for men initially diagnosed with metastatic prostate cancer.
Starting in 2014, that began to change after a large clinical trial showed that adding the chemotherapy drug docetaxel to ADT improved how long men with hormone-responsive disease lived. Shortly after, another clinical trial showed that adding abiraterone to ADT also improved survival in these men, although primarily in men with many metastatic tumors, known as high-volume disease.
However, docetaxel, which works by directly killing cancer cells, can have substantial side effects, and some patients arent healthy enough to tolerate it. And abirateronewhich blocks androgen production throughout the bodycan also cause side effects, including those that affect the liver. It also has to be given in combination with the steroid prednisone, which carries its own toxicity.
Doing so, Dr. Chi said during a presentation of the TITAN data at the ASCO meeting, might help stave off the typically inevitable development of hormone-resistant cancer, which is more difficult to treat and a key driver of prostate cancer deaths.
Recommended Reading: Womens Hormones At 50
Also Check: Do You Need A Prostate
Drugs That Stop Androgens From Working
Anti-androgens
For most prostate cancer cells to grow, androgens have to attach to a protein in the prostate cancer cell called an androgen receptor. Anti-androgens are drugs that also connect to these receptors, keeping the androgens from causing tumor growth. Anti-androgens are also sometimes called androgen receptor antagonists.
Drugs of this type include:
They are taken daily as pills.
In the United States, anti-androgens are not often used by themselves:
- An anti-androgen may be added to treatment if orchiectomy or an LHRH agonist or antagonist is no longer working by itself.
- An anti-androgen is also sometimes given for a few weeks when an LHRH agonist is first started. This can help prevent a tumor flare.
- An anti-androgen can also be combined with orchiectomy or an LHRH agonist as first-line hormone therapy. This is called combined androgen blockade . There is still some debate as to whether CAB is more effective in this setting than using orchiectomy or an LHRH agonist alone. If there is a benefit, it appears to be small.
- In some men, if an anti-androgen is no longer working, simply stopping the anti-androgen can cause the cancer to stop growing for a short time. This is called the anti-androgen withdrawal effect, although it is not clear why it happens.
Newer anti-androgens
Enzalutamide , apalutamide and darolutamide are newer types of anti-androgens. They can sometimes be helpful even when older anti-androgens are not.
These drugs are taken as pills each day.
What Are Some Of My Options To Manage Those Side Effects
Hot flashes tend to be the most bothersome.
Non-medication strategies like keeping cool drinks with you, dressing comfortably, relaxation techniques, and breathing exercises might be helpful.
Medications, such as megestrol, estrogen therapies, antidepressants, and neuroleptic agents like gabapentin can improve hot flashes but often come with dose-limiting side effects.
Pain, although usually not a side effect of treatment, is managed with non-narcotic or narcotic pain medications. We sometimes have to manage the side effects of pain medication, such as constipation.
Using the mildest medication is always best.
Don’t Miss: Is Prostate And Pancreatic Cancer The Same
Physical Emotional And Social Effects Of Cancer
Cancer and its treatment cause physical symptoms and side effects, as well as emotional, social, and financial effects. Managing all of these effects is called palliative care or supportive care. It is an important part of your care that is included along with treatments intended to slow, stop, or eliminate the cancer.
Palliative care focuses on improving how you feel during treatment by managing symptoms and supporting patients and their families with other, non-medical needs. Any person, regardless of age or type and stage of cancer, may receive this type of care. And it often works best when it is started right after a cancer diagnosis. People who receive palliative care along with treatment for the cancer often have less severe symptoms, better quality of life, and report that they are more satisfied with treatment.
Palliative treatments vary widely and often include medication, nutritional changes, relaxation techniques, emotional and spiritual support, and other therapies. You may also receive palliative treatments similar to those meant to get rid of the cancer, such as chemotherapy, surgery, or radiation therapy.
Learn more about the importance of tracking side effects in another part of this guide. Learn more about palliative care in a separate section of this website.
Breaking News: Fda Approves Darolutamide For Metastatic Hormone
Today, the FDA approved darolutamide in combination with docetaxel chemotherapy for patients with metastatic hormone-sensitive prostate cancer . This means that patients with mHSPC have an additional treatment option.
Darolutamide is a novel hormone therapy that works by blocking the androgen receptor. Androgens are the hormones that act as prostate cancers fuel. The approval is based on the results of a large Phase 3 clinical trial called ARASENS. This trial compared outcomes among 1300 patients who received docetaxel + standard ADT + darolutamide vs. patients who received docetaxel + standard ADT + placebo. 86% of the patients were newly diagnosed with prostate cancer that had metastasized to the bones or other organs.
Patients treated with the addition of darolutamide were 32% less likely to die during the study follow-up period compared to patients treated with docetaxel + ADT alone. These patients also had improved time to castration resistance , time to pain progression, time to symptomatic skeletal related events , and time to next cancer therapy. Importantly, these improved outcomes of triplet therapy intensification were associated with only a modest increase in adverse events.
Read more about treatment intensification in mHSPC here.
Also Check: Does Incontinence Go Away After Prostate Surgery
