Lhrh/gnrh Agonists And Antagonists
LHRH/GnRH agonists, such as leuprorelin/leuprolide, goserelin, and triptorelin, are by far the most commonly utilized forms of ADT in clinical practice in the treatment of PCa, targeting the LHRH/GnRH receptor in the anterior pituitary gland and administered as an intramuscular or subcutaneous injection. They stimulate the receptor, creating a temporary surge in LH and testosterone levels followed by downregulation of the receptor over the next 23 weeks with a subsequent reduction in LH and suppression of testosterone production by the testes.19 They achieve serum testosterone levels below castration within 46 weeks with a subsequent reduction in the PSA level.20 The most common adverse effects associated with treatment are hot flashes, fatigue, sexual/erectile dysfunction, testicular atrophy, cognitive decline, increased risk of diabetes and cardiovascular events, and decreased bone mineral density associated with joint disorders and/or osteoporosis that needs to be monitored periodically with bone density scanning.21
Hormone Therapy For Prostate Cancer
Jump to a section
Hormone therapy is also called androgen suppression therapy. The goal of this treatment is to reduce levels of male hormones, called androgens, in the body, or to stop them from fueling prostate cancer cell growth.
Androgens stimulate prostate cancer cells to grow. The main androgens in the body are testosterone and dihydrotestosterone . Most androgens are made by the testicles, but the adrenal glands as well as the prostate cancer cells themselves, can also make androgens.
Lowering androgen levels or stopping them from getting into prostate cancer cells often makes prostate cancers shrink or grow more slowly for a time. But hormone therapy alone does not cure prostate cancer.
Get The Facts: Things To Know About Prostate Cancer And A Treatment Option
This content is sponsored and provided by Myovant Sciences and Pfizer Inc.
Did you know that men are less likely to go to the doctor than women? A study conducted by the U.S. Centers for Disease Control in 2018 found that nearly a quarter of men had not seen a doctor in the past year while only half as many women reported the same. Some men may try to tough it out when they have an issue, rather than seeking help, but it is important to receive regular preventative care and manage any new or existing conditions in order to stay healthy. In addition to taking stock of your own health, its also a good idea to check in with the men in your life to make sure theyre taking care of themselves.
Take a few moments to review the following five frequently asked questions about prostate cancer to ensure you have a few key facts about this surprisingly common and potentially serious disease including what you can do if you or a loved one is diagnosed.
1. How common is prostate cancer?
Approximately one in eight men will be diagnosed with prostate cancer in their lifetime. Prostate cancer is the most common form of cancer in American men, other than skin cancer, and is the second leading cause of cancer death for men in the U.S. The American Cancer Society estimates that there will be about 268,000 new cases of prostate cancer in 2022.
Risk factors for prostate cancer include older age , race, family history and genetic factors.
2. Who should be screened for prostate cancer?
Don’t Miss: How Do I Know If I Got Prostate Cancer
Hormone Therapy With Radiation
Hormone therapy is often given together with radiation therapy for localized disease .
Hormone therapy usually consists of a shot that lowers your testosterone, given every 1 to 6 months, depending on the formulation. Sometimes, it is prescribed as a daily pill that blocks testosterone from reaching the cancer cells. Clinical trials show a benefit in patients who receive hormonal treatment in combination with external beam radiation. Hormone therapy has been shown to improve cure rates of prostate cancer for men receiving radiation therapy and is part of the standard of care for men with certain types of intermediate-risk prostate cancer and nearly all high-risk prostate cancer. It is often given for intermediate-risk cancer for 4 to 6 months , and for 2 to 3 years in men with high-risk localized prostate cancer, although some doctors may recommend as little as 18 months of hormone therapy.
Hormone therapy should not be given to men with low-risk prostate cancer and is not a standalone treatment for localized prostate cancer in any risk category.
Want more information about a prostate cancer diagnosis and treatment options? Download or order a print copy of the Prostate Cancer Patient Guide.
Treatment To Lower Androgen Levels From Other Parts Of The Body
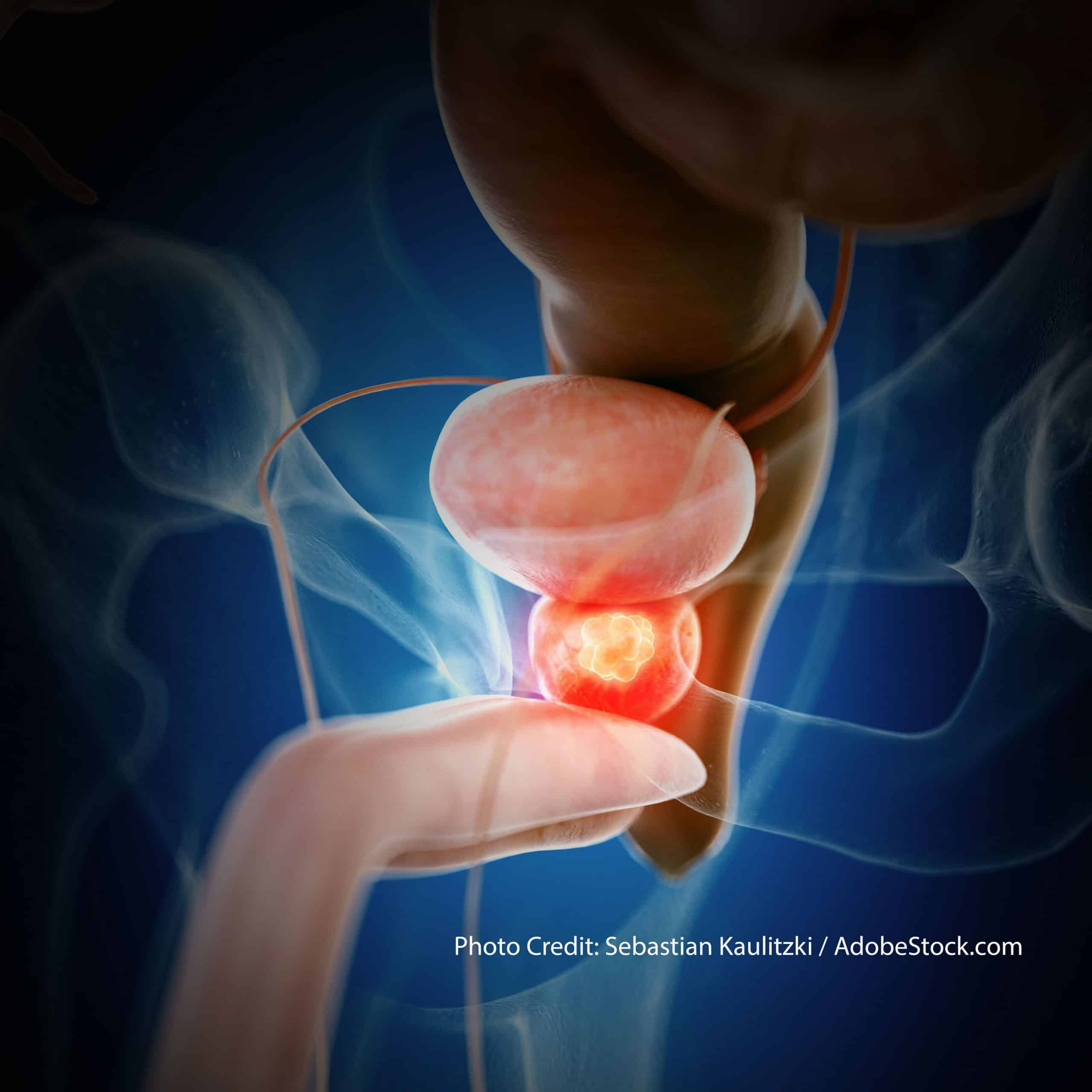
LHRH agonists and antagonists can stop the testicles from making androgens, but cells in other parts of the body, such as the adrenal glands, and prostate cancer cells themselves, can still make male hormones, which can fuel cancer growth. Some drugs can block the formation of androgens made by these cells.
Abiraterone blocks an enzyme called CYP17, which helps stop these cells from making androgens.
Abiraterone can be used in men with advanced prostate cancer that is either:
- Castration-resistant
This drug is taken as pills every day. It doesnt stop the testicles from making testosterone, so men who havent had an orchiectomy need to continue treatment with an LHRH agonist or antagonist. Because abiraterone also lowers the level of some other hormones in the body, prednisone needs to be taken during treatment as well to avoid certain side effects.
Ketoconazole , first used for treating fungal infections, also blocks production of androgens made in the adrenal glands, much like abiraterone. It’s most often used to treat men just diagnosed with advanced prostate cancer who have a lot of cancer in the body, as it offers a quick way to lower testosterone levels. It can also be tried if other forms of hormone therapy are no longer working.
Ketoconazole also can block the production of cortisol, an important steroid hormone in the body, so men treated with this drug often need to take a corticosteroid .
Also Check: What Age Can You Get Prostate Cancer
Adt And Prostate Cancer: Who Really Needs It
Part One of Four
The only people who really like androgen deprivation therapy are the drug companies that make billions of dollars a year selling the drugs. Doctors dont like it, and men dont like being on these drugs. So why do it? There are few specific situations when ADT therapy is the right thing to do. These are the most common:
* Intermediate-risk men who are given six months of ADT plus external-beam radiation
* High-risk men who are getting radiation therapy. This is a finite course of ADT, and this combination two or three years of ADT plus external-beam radiation has been proven to cure cancer in many men.
* Men with metastatic prostate cancer. ADT can make a big difference in these men, in relieving their symptoms and dramatically improving their quality of life. It can also extend life some men have been on ADT for 20 years and are still going strong.
Who should not get ADT? Anybody else with prostate cancer. If you just have a rising PSA after radiation therapy or radical prostatectomy, that is not a good enough reason for a doctor to put you on ADT. If your doctor wants to put you on ADT to shrink your prostate before brachytherapy, thats not a good enough reason.
ADT has never been shown to extend life if its given too soon, as opposed to taking it when you need it. Johns Hopkins urologist Patrick Walsh, M.D., with whom I have written several books on prostate cancer, has been saying this for many years.
©Janet Farrar Worthington
How Can I Manage These Side Effects
It is important to manage any side effects you are having so that you can continue treatment. Listed below are tips on how to manage the side effects of androgen deprivation medications.
Sexual Dysfunction & Body Image Problems
ADT causes a loss of libido in most men. This tends to happen within the first few months of therapy, followed by erectile dysfunction . Libido often comes back a few months after androgen deprivation therapy has been finished. Depending on other cancer treatments and other medical problems, erectile function also can come back for many men.
Talk with your partner and your healthcare providers. Learn about ED. Ask for help from your urologist, who is trained in the treatment of ED. Finally, think about seeing a sex therapist, which can be helpful for couples facing these side effects.
Osteoporosis
Osteoporosis is when you have thinning of the bones that can lead to fractures . There are things you can do to lower your risk of a fracture and to strengthen your bones.
Don’t Miss: Best Way To Screen For Prostate Cancer
Risk Assessment Tool Stratifies Major Osteoporotic Fracture Risk In Prostate Cancer
The Fracture Risk Assessment Tool is an easy to complete questionnaire for identifying fracture risk among patients initiating androgen deprivation therapy for prostate cancer. These findings were published in Archives of Osteoporosis.
In prostate cancer, ADT is associated with increased risk for osteoporosis and skeletal fractures. As such, the National Institute for Health and Care Excellence recommends patients with prostate cancer be evaluated for bone-related health, but fracture risk is often overlooked in this population.
The goal of this study was to evaluate the utility of the fracture risk tool in the setting of prostate cancer. A total of 200 men starting long-term ADT between 2020 and 2022 at The Royal Bolton Hospital in the United Kingdom completed the FRAX questionnaire and were assessed for serum vitamin D and calcium levels. The primary outcome was the 10-year probability of sustaining a major osteoporotic fracture .
The patients were median age 73.5 years .
Ten-year probability of sustaining a MOF ranged between 3.1% and 54% and the 10-year probability of sustaining a hip fracture ranged between 0.2% and 52%.
Risk for sustaining a MOF was low for 91% of patients, intermediate for 6%, and high for 3%. In the high-risk group, all 6 patients had a previous fracture, 4 had a parental fracture history, and 3 consumed 3 or more units of alcohol per day.
Reference
Calcium And Vitamin D
The National Osteoporosis Foundation recommends a daily calcium intake of 1200 mg and vitamin D supplement of 8001000 IU/d for all men over the age of 50.122 A 2015 study analyzed whether the recommended vitamin D supplementation of 800IU/d increased blood levels of 25-OH vitamin D in patients receiving ADT. Regression analysis showed vitamin D supplementation was associated with increased 25-OH vitamin D serum levels supporting the current recommendation of 800 IU/d for men receiving ADT.123
Also Check: How Accurate Is Blood Test For Prostate Cancer
Surgery Or Radiation Delayed Initiation Of Systemic Therapy By 18 Months
byCharles Bankhead, Senior Editor, MedPage Today November 29, 2022
Metastasis-directed therapy in selected patients with recurrent oligometastatic prostate cancer led to PSA responses in a majority of patients and delayed initiation of hormonal therapy by 18 months, a retrospective study showed.
Overall, 77 of 124 patients had PSA declines of more than 50% with surgery or stereotactic body radiation therapy . In particular, surgery led to PSA responses in 80.5% of patients, and almost a third of patients remained progression free after 3 years.
The results showed that local treatment of oligometastatic prostate cancer without androgen deprivation therapy is feasible and warrants prospective investigation of the strategy, reported Jack R. Andrews, MD, of the Mayo Clinic in Phoenix, and colleagues, in the Journal of Urology.
“To our knowledge, this is the first report evaluating the impact of MDT alone in solitary metastatic prostate cancer and is one of the largest studies to evaluate surgical and radiotherapy MDT in the absence of ADT,” the authors said. “These results indicate that further investigation is needed to define the role of MDT in oligometastatic prostate cancer.”
A single-center retrospective analysis of almost 500 patients with oligometastatic prostate cancer showed that MDT with surgery or external beam radiation therapy led to better outcomes in patients with lymph node metastasis as compared with ADT but not in those with bony metastasis.
Can You Live 10 Years With Metastatic Prostate Cancer
Of the 794 evaluable patients, 77% lived < 5 years, 16% lived 5 up to 10 years, and 7% lived > or = 10 years. Factors predicting a statistical significant association with longer survival included minimal disease, better PS, no bone pain, lower Gleason score, and lower PSA level.
Read Also: Radiation Beam Therapy For Prostate Cancer
Complications Of Androgen Deprivation Therapy In Men With Prostate Cancer
This article summarizes the key side effects associated with ADT for the treatment of prostate cancer and discusses strategies to optimize management.
The standard treatment for men with metastatic prostate cancer is androgen deprivation therapy . This therapy is associated with a multitude of side effects that can impact quality of life. These include vasomotor complications , sexual dysfunction and gynecomastia, osteoporosis, metabolic syndrome, and depression. Additionally, ADT has been associated with neurocognitive deficits, thromboembolic disease, and cardiovascular disease, although the data regarding the latter associations are mixed. This article summarizes the key side effects associated with ADT and discusses strategies to optimize management.
Concurrent Adt Radiation Therapy Improves Outcomes In Localized Prostate Cancer
Disclosures: We were unable to process your request. Please try again later. If you continue to have this issue please contact .
Androgen deprivation therapy sequencing had a considerable effect on outcomes among men with prostate cancer who received prostate-only radiotherapy, according to study results published in Journal of Clinical Oncology.
Historically, men with prostate cancer begin ADT before they start radiation.
However, the findings of this study in which researchers analyzed more than 7,000 men treated across 12 randomized trials suggest most men should begin ADT when starting radiation.
Healio spoke with Amar U. Kishan, MD, vice chair of clinical and translational research and chief of the genitourinary oncology service in the department of radiation oncology at UCLA Jonsson Comprehensive Cancer Center, about the results and their potential clinical implications.
Recommended Reading: What Are The 5 Early Signs Of Prostate Cancer
Prostate Cancer: Androgen Deprivation Therapy With Dr Kristen Scarpato
Our guest is Dr. Kristen Scarpato, a urologic oncologist at Vanderbilt University Medical Center in Nashville, TN. She is here to talk with us about Androgen Deprivation Therapy, or ADT, for prostate cancer. She covers information such as what is ADT, questions to ask your doctor and what to expect after treatment.
Short on time? Use the below timestamps to jump to any topic section:0:48 – Introduction3:30 – What is Androgren Deprivation Therapy ?4:30 – Why is ADT important?6:43 – When during treatment would ADT be considered?9:32 – What patients benefit the most from ADT?10:45 – What administers ADT?12:10 – What can patients expect after ADT?15:30 – Talking with your doctor17:16 – Final thoughts
Supported by an independent educational grant provided by Myovant Sciences LTD and Pfizer Inc.
For more information, please subscribe to our free digital magazine, UrologyHealth extra.
****
Ep 3a: Androgen Deprivation Therapy Failure And Second
is really the backbone of systemic therapy for advanced prostate cancer, and it has been for decades. Importantly, we now know that in many situations of advanced prostate cancer, it’s ADT intensification or ADT combinations that are really now standard of care.
When ADT or a combination therapy starts to fail the patient, and the is rising, and the disease looks like it may be spreading or growing on scans, we absolutely need to think about next steps. And, in most cases, I try to think about next steps in our treatment journey before we get to that point, just to make sure I understand what our options are so that I’m ready to move forward, especially if it’s an emergent situation. Some of that preplanning, of course, requires that we do additional testing. And particularly for things like PARP inhibitors, where we need to do genetic germline or somatic testing, that is going to need to happen in advance of when we need that treatment.
I think that the next few years are going to be incredibly rich when it comes to prostate cancer clinical trials, and the advances are going to be coming fast and furious. It’s been only 6 months or even less since we learned the results of the VISION trial. I do expect that the ongoing trials investigating lutetium PSMA are going to probably move it forward, and we will be able to see its benefits be even more pronounced as we move it earlier in the disease spectrum.
Read Also: What Are The Chances Of Prostate Cancer Returning After Radiation
Reducing The Impact Of Adt
For men who experience a PSA recurrence after radiation therapy for prostate cancer, hormone therapy given intermittently appears to be as effective as hormone therapy given continuously.14
Androgen deprivation therapy is designed to block testosterone from stimulating the growth of hormone-dependent types of prostate cancer. Because continuous androgen deprivation therapy produces side effects such as osteoporosis, hot flashes, and loss of libido, and because many prostate cancers eventually become resistant to hormonal therapy, researchers continue to explore alternatives. Intermittent androgen suppression is one such alternative. It involves the administration of hormonal therapy until a sufficient treatment response has been achieved, followed by a period of no treatment. The cycle is repeated as needed. IAS may reduce side effects and delay hormone resistance. In order to assess the effects of IAS among men who experience an increase in PSA after radiation therapy for prostate cancer, researchers evaluated 1,386 men. Half the patients were treated with continuous androgen deprivation and half were treated with IAS. IAS was delivered for eight months at a time, and was restarted if PSA levels off treatment exceeded 10 ng/ml. During follow-up, patients assigned to IAS were on treatment 27% of the time. The trial was stopped early when it became apparent that overall survival with IAS was no worse than with continuous androgen deprivation therapy.
References:
