What Is The Gleason Score
The Gleason score will be described using a number from 6 to 10. The pathologist will add the two most common grades together to make the Gleason score.
If the most common grade in the sample is 3, and the second most common grade in the sample is 4, then your Gleason score will be 7 . If only one grade is found, then this grade is added to itself. So if all the sample is only grade 3, then the Gleason score will be 6 .
- Lower grades are slower growing.
- Higher grades are faster growing.
The Tnm System For Prostate Cancer Stages
As they do for most cancers, doctors use the TNM system to describe prostate cancer stages. The system uses three different aspects of tumor growth and spread:
- Tumor. Whats the size of the main area of prostate cancer?
- Nodes. Has it spread to any lymph nodes? If so, how far and how many?
- Metastasis. How far has the prostate cancer spread?
What Does It Mean If In Addition To Cancer My Biopsy Report Also Says Acute Inflammation Or Chronic Inflammation
Inflammation of the prostate is called prostatitis. Most cases of prostatitis reported on a biopsy are not caused by infection and do not need to be treated. In some cases, inflammation may increase you PSA level, but it is not linked to prostate cancer. The finding of prostatitis on a biopsy of someone with cancer does not affect their prognosis or the way the cancer is treated.
Recommended Reading: What Herbs Are Good For Prostate Cancer
Physical Emotional And Social Effects Of Cancer
Cancer and its treatment cause physical symptoms and side effects, as well as emotional, social, and financial effects. Managing all of these effects is called palliative care or supportive care. It is an important part of your care that is included along with treatments intended to slow, stop, or eliminate the cancer.
Palliative care focuses on improving how you feel during treatment by managing symptoms and supporting patients and their families with other, non-medical needs. Any person, regardless of age or type and stage of cancer, may receive this type of care. And it often works best when it is started right after a cancer diagnosis. People who receive palliative care along with treatment for the cancer often have less severe symptoms, better quality of life, and report that they are more satisfied with treatment.
Palliative treatments vary widely and often include medication, nutritional changes, relaxation techniques, emotional and spiritual support, and other therapies. You may also receive palliative treatments similar to those meant to get rid of the cancer, such as chemotherapy, surgery, or radiation therapy.
Learn more about the importance of tracking side effects in another part of this guide. Learn more about palliative care in a separate section of this website.
What Does It Mean If In Addition To Cancer My Biopsy Report Also Mentions Acute Inflammation Or Chronic Inflammation
Inflammation of the prostate is called prostatitis. Most cases of prostatitis reported on biopsy are not caused by infection and do not need to be treated. In some cases, inflammation may increase your PSA level, but it is not linked to prostate cancer. The finding of prostatitis on a biopsy of someone with prostate cancer does not affect their prognosis or the way the cancer is treated.
Also Check: Do You Need A Prostate
What Are Prostate Cancer Survival Rates By Stage
Staging evaluation is essential for the planning of treatment for prostate cancer.
- A basic staging evaluation includes the patient examination, blood tests, and the prostate biopsy including ultrasound images of the prostate.
- Further testing and calculations may be performed to best estimate a patient’s prognosis and help the doctor and patient decide upon treatment options.
Prognosis refers to the likelihood that cancer can be cured by treatment, and what the patient’s life expectancy is likely to be as a consequence of having had a prostate cancer diagnosis.
If cancer is cured, your life expectancy is what it would have been had you never been diagnosed with prostate cancer. If cancer cannot be cured due to it recurring in distant locations as metastases, or recurs either locally or in an area no longer able to be treated in a curative manner, then estimates can be made of what is likely to be your survival-based again on group statistics for people who have been in the same situation.
Nomograms are charts or computer-based tools that use complex math from the analysis of many patients’ treatment results.
The prognosis for prostate cancer varies widely and depends on many factors, including the age and health of the patient, the stage of the tumor when it was diagnosed, the aggressiveness of the tumor, and cancer’s responsiveness to treatment, among other factors.
The 5 and 10-year survival rate of prostate cancer chart
| Stage and 5-Year Survival |
|---|
New Contemporary Prostate Cancer Grading System
Discrete Well-formed Glands
Gleason Patterns 1-3: from left to right1st Row: Closely packed uniform sized and shaped large glands Large variably sized and shaped glands, some with infolding Uniform medium sized glands Variably sized glands2nd Row: Occasional tangentially sectioned glands amongst well-formed small glands Occasional tangentially sectioned glands amongst well-formed glands with open lumina Back-to-back discrete glands Branching glands
Cribriform/Poorly-formed/Fused Glands
Gleason Pattern 4: from left to right3rd Row: Large irregular cribriform glands with well-formed lumina Irregular cribriform glands with slit-like lumina, glomeruloid structures, and fused glands Irregular cribriform glands with small round lumina Small round cribriform glands4th Row: Poorly-formed glands with peripherally arranged nuclei Small poorly-formed glands Small poorly-formed glands Fused poorly-formed glands
Sheets/Cords/Single Cells/Solid Nests/Necrosis
Gleason Pattern 5: from left to right5th Row: Sheets of cancer Sheets of cancer with rosette formation Small nests and cords of tumor with scattered clear vacuoles Individual cells6th Row: Nests and cords of cells with only vague attempt at lumina formation Solid nests of cancer Solid nests with comedonecrosis Cribriform glands with central comedonecrosis
Don’t Miss: Can Prostate Infection Cause Back Pain
Gleason Score And International Society Of Urological Pathology 2014 Grade
In the original Gleason grading system, 5 Gleason grades based on histological tumour architecture were distinguished, but in the 2005 and subsequent 2014 International Society of Urological Pathology Gleason score modifications Gleason grades 1 and 2 were eliminated . The 2005 ISUP modified GS of biopsy-detected PCa comprises the Gleason grade of the most extensive pattern, plus the second most common pattern, if two are present. If one pattern is present, it needs to be doubled to yield the GS. For three grades, the biopsy GS comprises the most common grade plus the highest grade, irrespective of its extent. The grade of intraductal carcinoma should also be incorporated in the GS . In addition to reporting of the carcinoma features for each biopsy, an overall GS based on the carcinoma-positive biopsies can be provided. The global GS takes into account the extent of each grade from all prostate biopsies. The 2014 ISUP endorsed grading system limits the number of PCa grades, ranging them from 1 to 5 .
Further sub-stratification of the intermediate-risk group can be made and specifically the National Cancer Center Network Guidelines subdivide intermediate-risk disease into favourable intermediate-risk and unfavourable intermediate-risk, with unfavourable features including ISUP grade 3, and/or > 50% positive biopsy cores and/or at least two intermediate-risk factors .
Table 4.2: EAU risk groups for biochemical recurrence of localised and locally advanced prostate cancer
Reporting Rules For Gleason Grading Reporting Secondary Patterns Of Higher Grade When Present To A Limited Extent
High-grade tumor of any quantity on needle biopsy, as long as it was identified at low to medium magnification should be included within the Gleason score. Any amount of high-grade tumor sampled on needle biopsy most likely indicates a more significant amount of high-grade tumor within the prostate due to the correlation of grade and volume and the problems inherent with needle biopsy sampling. Consequently, a needle biopsy that is entirely involved by cancer with 98% Gleason pattern 3 and 2% Gleason pattern 4 would be diagnosed as Gleason score 3+4=7.
In RP specimens with the analogous situation of a tumor nodule having 98% Gleason pattern 3 and 2% pattern 4, the current recommendation is to grade these foci in an analogous manner to that done on needle biopsy and interpret the case as Gleason score 3+4=7 and record the percentage of pattern 4.
Minor high-grade patterns do not change the Grade Groups with minor pattern 5). If Grade Groups 15 eventually were to replace Gleason scores 210, the 2014 Consensus Conference suggested options how to incorporate tertiary patterns with Grade Groups. Suggestions included, for example, Grade Group 2 with minor high-grade pattern or Grade Group 2+.
Also Check: Do All Men Get Prostate Cancer
Tertiary Grade On Needle Core Biopsy
In contrast to the original Gleason grading system, it is now recommended that on a needle core biopsy both the most common and highest grade are added together for the Gleason score . For example, if there is 60 % Gleason pattern 3, 35 % Gleason pattern 4, and 5 % Gleason pattern 5, the Gleason score would be 3+5=8. Needle core biopsy is an imperfect, non-targeted, random sampling of the prostate gland. Thus any amount of high-grade tumor sampled on needle biopsy most likely indicates a more significant amount of high-grade tumor within the prostate. In all specimens, in the setting of high-grade cancer, one should not report a lower grade if it occupies less than 5 % of the total tumor. For example, if there is 98 % Gleason pattern 4 and 2 % Gleason pattern 3, the Gleason score would be reported as 4+4=8 .
Grade And Risk Category
The biopsy results will show the grade of the cancer. This is a score that describes how quickly the cancer may grow or spread.
For many years, the Gleason scoring system has been used to grade the tissue taken during a biopsy. If you have prostate cancer, youll have a Gleason score between 6 and 10. A new system has been introduced to replace the Gleason system. Known as the International Society of Urological Pathologists Grade Group system, this grades prostate cancer from 1 to 5 .
Risk of progression
Based on the stage, grade and your PSA level before the biopsy, localised prostate cancer will be classified as having a low, intermediate or high risk of growing and spreading. This is known as the risk of progression. The risk category helps guide management and treatment.
Grading prostate cancer
| High risk. The cancer is likely to grow aggressive. |
Also Check: Does A Pet Scan Show Prostate Cancer
What Are The Five Stages Of Prostate Cancer
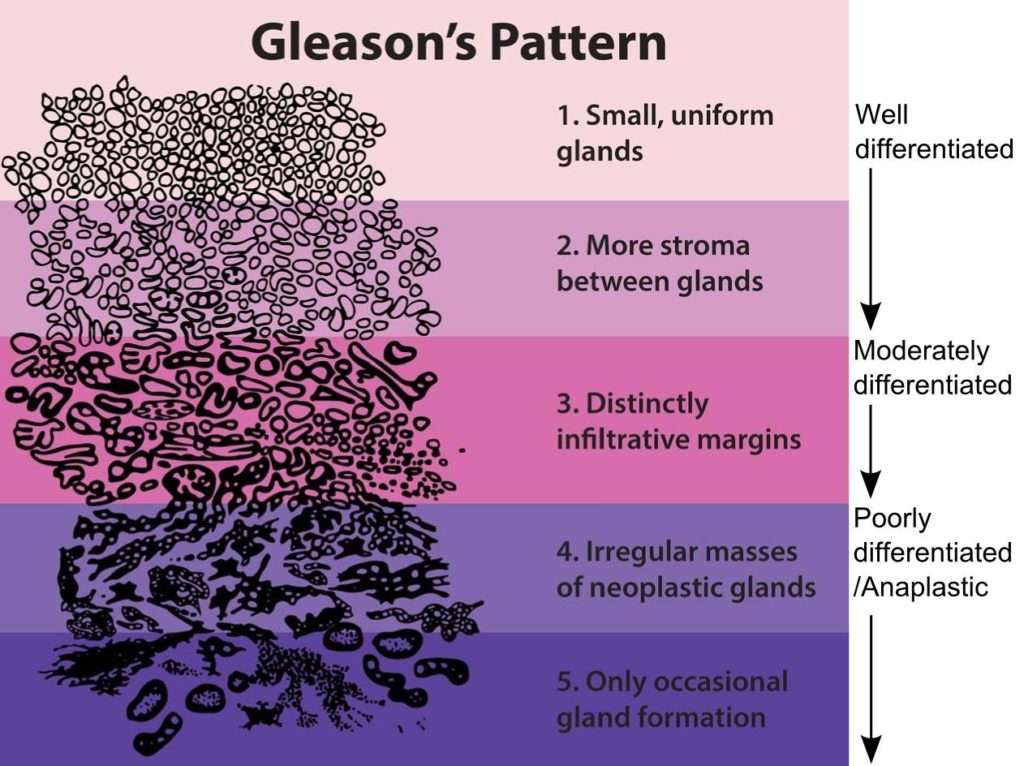
The Gleason grading system grades prostate cancer from 1 to 5. According to cells appearances under a microscope, this system grades the most common and second most common patterns of cells in a tissue sample collected via biopsy.
- Grade 1: The cells appear like normal prostate cells.
- Grades 2-4: Cells that score the lower look closest to normal and are suggestive of less aggressive cancer. Those that score higher look the furthest from normal and will probably grow faster.
- Grade 5: Most cells look vastly different from normal.
Depending on the Gleason score, the American Joint Committee on Cancer has classified prostate cancer into four stages.
Stage I cancer:
- This stage is known as localized cancer because the cancer has been found in only one part of the prostate .
- Stage I cancers cannot be felt during a digital rectal exam or seen with imaging tests.
- If the prostate-specific antigen is less than 10, it is most likely slow growing.
Stage II cancer:
- This stage of cancer is still localized but is more advanced than stage I.
- In stage II, the cells are less normal than stage I and may grow more rapidly.
- Stage IIA means that the cancer is found only on one side of the prostate, whereas stage IIB means that the cancer is found in both sides of the prostate.
Stage III cancer:
Stage IV cancer:
To summarize:
Prostate Cancer Grading And The Gleason Score Explained
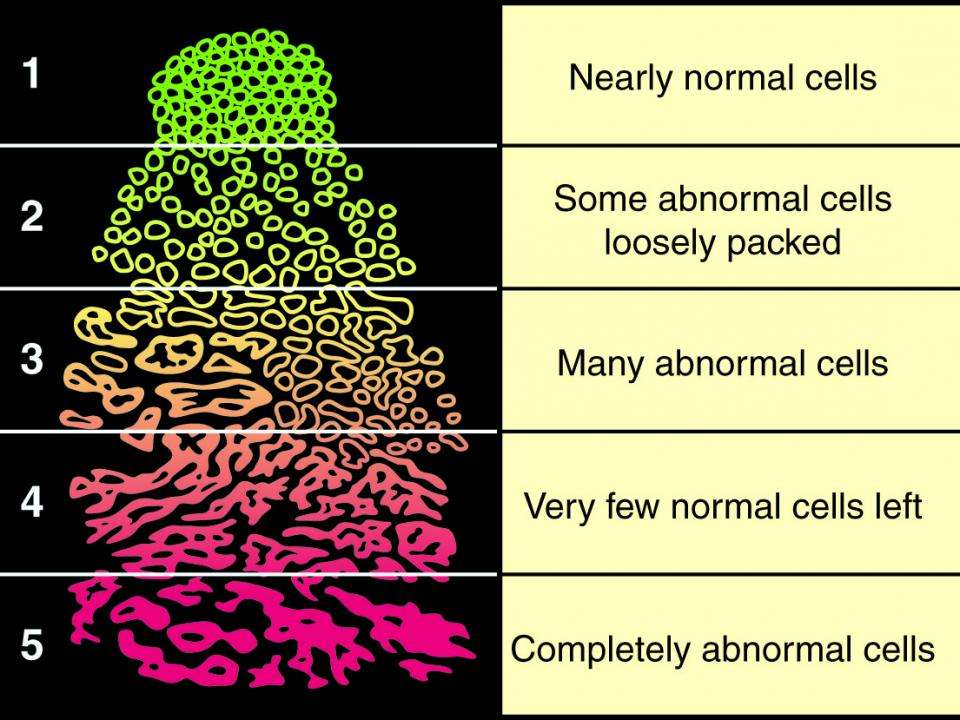
When prostate cancer is graded, a system is used known as the Gleason Score to determine how aggressive the cancer is. The Gleason Score ranges from 1-5 and describes how much of the tissue taken from a biopsy looks like healthy tissue or abnormal tissue.
When you are diagnosed with cancer, you may find that the doctors looking after you may talk about your Gleason score and what the stage of your prostate cancer is. Your doctors will try and explain things in easily understood language, but some of the terminology used can be somewhat confusing. The following will help to explain the terminology and clarify any questions you may have. If you do not understand what your doctor is saying, tell them and ask for further clarification.
Read Also: Are You Put To Sleep For A Prostate Biopsy
Use Of Contrast Agent
Our preprocessing scheme, specifically the individual denoising and intensity standardization protocols, enables us to dynamically account for individual differences in noise and contrast. Therefore, the contrast agent dose is not expected to introduce a major bias. This aspect is relevant when implementing a low-contrast dose protocol as by He et al. . Moreover, it might be possible to abbreviate the DCE-MRI protocol to only capture the first-pass phase, during which the peak FD was usually found. Abbreviating the DCE protocol and using a low amount of contrast agent might be an alternative approach to entirely skipping the DCE sequences, which constitutes a recent trend in prostate MRI and is also reflected in the recent PI-RADS version 2.1 .
How Important Is The Gleason Score
The Gleason score is very important in predicting the behavior of a prostate cancer and determining the best treatment options. Still, other factors are also important, such as:
- The blood PSA level
- How much of each core is made up of cancer
- The number of cores that contain cancer
- Whether cancer was found in both sides of the prostate
- Whether the cancer has spread outside the prostate
Also Check: What Happens When You Have Your Prostate Removed
What Are Some Of The Cancer Type
Breast and prostate cancers are the most common types of cancer that have their own grading systems.
Breast cancer. Doctors most often use the Nottingham grading system for breast cancer . This system grades breast tumors based on the following features:
- Tubule formation: how much of the tumor tissue has normal breast duct structures
- Nuclear grade: an evaluation of the size and shape of the nucleus in the tumor cells
- Mitotic rate: how many dividing cells are present, which is a measure of how fast the tumor cells are growing and dividing
Each of the categories gets a score between 1 and 3 a score of 1 means the cells and tumor tissue look the most like normal cells and tissue, and a score of 3 means the cells and tissue look the most abnormal. The scores for the three categories are then added, yielding a total score of 3 to 9. Three grades are possible:
- Total score = 35: G1
- Total score = 67: G2
- Total score = 89: G3
- Gleason X: Gleason score cannot be determined
- Gleason 26: The tumor tissue is well differentiated
- Gleason 7: The tumor tissue is moderately differentiated
- Gleason 810: The tumor tissue is poorly differentiated or undifferentiated
Psa Levels By Age Chart
The main difference between the PSA scores of prostatitis and an enlarged prostate, compared to prostate cancer, is the ratio of free vs bound PSA within your test sample.
- Prostate Cancer will have a higher bound PSA ratio.
- An enlarged prostate and prostatitis will have a higher free PSA ratio.
- If your free PSA results are less than 25%, your risk for developing prostate cancer is between 10% to 20%.
- If your free PSA results are less than 10%, your risk for developing prostate cancer jumps to around 50%.
Don’t Miss: Green Light Photovaporization Of The Prostate
Active Surveillance And Watchful Waiting
If prostate cancer is in an early stage, is growing slowly, and treating the cancer would cause more problems than the disease itself, a doctor may recommend active surveillance or watchful waiting.
Active surveillance. Prostate cancer treatments may seriously affect a person’s quality of life. These treatments can cause side effects, such as erectile dysfunction, which is when someone is unable to get and maintain an erection, and incontinence, which is when a person cannot control their urine flow or bowel function. In addition, many prostate cancers grow slowly and cause no symptoms or problems. For this reason, many people may consider delaying cancer treatment rather than starting treatment right away. This is called active surveillance. During active surveillance, the cancer is closely monitored for signs that it is worsening. If the cancer is found to be worsening, treatment will begin.
ASCO encourages the following testing schedule for active surveillance:
-
A PSA test every 3 to 6 months
-
A DRE at least once every year
-
Another prostate biopsy within 6 to 12 months, then a biopsy at least every 2 to 5 years
Treatment should begin if the results of the tests done during active surveillance show signs of the cancer becoming more aggressive or spreading, if the cancer causes pain, or if the cancer blocks the urinary tract.
General Applications Of The Gleason Grading System
As described by Gleason, the initial grading of prostate carcinoma should be performed at low magnification using a x4 or x10 lens. After one assesses the case at scanning magnification, one may proceed to use the x20 lens to verify the grade. For example, at low magnification one may have the impression of fused glands or necrosis, but may require higher magnification at x20 to confirm its presence. However, one should not initially use the x20 or x40 objectives to look for rare fused glands or a few individual cells seen only at higher power, which would lead to an overdiagnosis of Gleason pattern 4 or 5, respectively . If the tumor is borderline between lower- and higher-grade cancer, I assign the lower grade so as to not result in overtreatment. In cores with borderline grade, additional levels are often helpful to clarify the grade.
Figure 6
Gleason pattern 3 with a few glands that appear poorly formed but are likely tangential sections off of adjacent small well-formed glands. Original magnification, 40x.
Read Also: How To Find The Prostate Gland Externally
