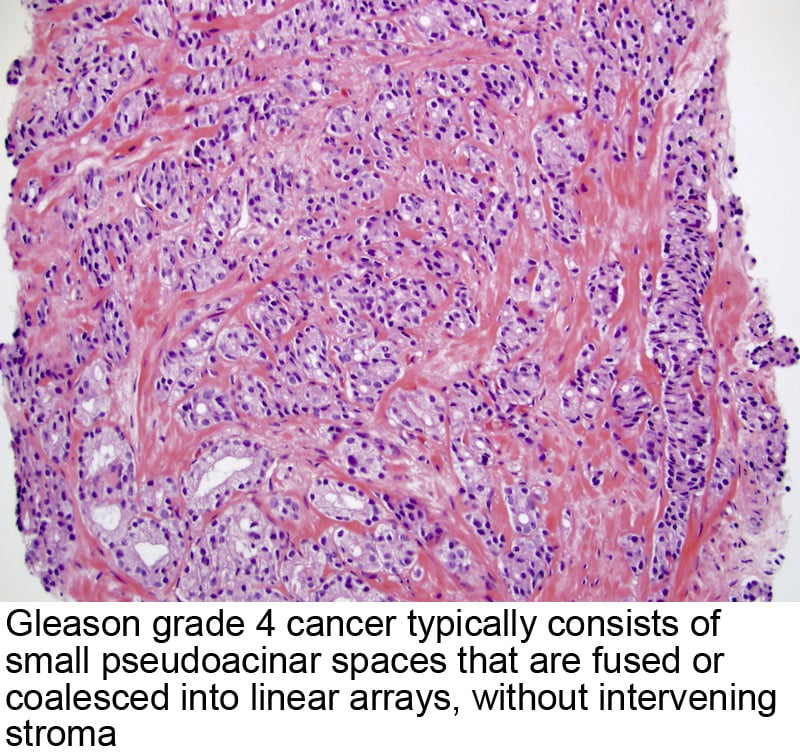
Movement Builds To Classify Gleason 6 Prostate Lesions As Nonmalignant
In prostate cancer, as in life, you roll the dice.
In craps, 3+3 is called a “hard six.” It’s hard because you can only win if you repeat with a combination of 3+3. Any other sixes you roll — 4+2, 5+1 — are losers.
Gleason 3+3 is a hard six in prostate cancer. It is the lowest grade cancer in the traditional Gleason scoring system. Still, to the eye of a pathologist, a Gleason 6 looks like a malignancy.
Now, a few experts are questioning whether this hard six is a cancer at all. Some urologists see a Gleason 6 as a noncancerous growth that has the potential to be invasive, but most likely will never spread to other organs or end up killing a man.
To a patient like me, who has been on active surveillance for 10 years, a Gleason 6 can create a big medical fuss lasting years with regular prostate-specific antigen blood tests, digital rectal exams , biopsies, and MRIs. It can cause “anxious surveillance” that prompts them to drop AS and undergo unnecessary radical prostatectomy, which poses a potential risk of impotence and urinary incontinence.
The Gleason 6 diagnosis can yield polar opposite recommendations from urologists. Ten years ago, I found this to be the case in the matter of a day.
On December 14, 2010, a local urologist recommended I undergo a radical prostatectomy within the week. When asked, he said he didn’t support active AS, then a relatively new approach for monitoring low-grade prostate cancer.
‘The right thing to do’
Mixed reactions
What Are Grade Groups
Grade Groups are a new way to grade prostate cancer to address some of the issues with the Gleason grading system.
As noted above, currently in practice the lowest Gleason score that is given is a 6, despite the Gleason grades ranging in theory from 2 to 10. This understandably leads some patients to think that their cancer on biopsy is in the middle of the grade scale. This can compound their worry about their diagnosis and make them more likely to feel that they need to be treated right away.
Another problem with the Gleason grading system is that the Gleason scores are often divided into only 3 groups . This is not accurate, since Gleason score 7 is made up of two grades , with the latter having a much worse prognosis. Similarly, Gleason scores of 9 or 10 have a worse prognosis than Gleason score 8.
To account for these differences, the Grade Groups range from 1 to 5 :
- Grade Group 1 = Gleason 6
- Grade Group 2 = Gleason 3+4=7
- Grade Group 3 = Gleason 4+3=7
- Grade Group 4 = Gleason 8
- Grade Group 5 = Gleason 9-10
Although eventually the Grade Group system may replace the Gleason system, the two systems are currently reported side-by-side.
What Does It Mean
A Gleason score of 6 is low grade, 7 is intermediate grade, and a score of 8 to 10 is high grade cancer.
Get More Information
Its also important to know whether any cells rated at Gleason grade 5 are present, even in just a small amount, and most pathologists will report this. Having any Gleason grade 5 in your biopsy or prostate puts you at a higher risk of recurrence.
But because many prostate cancer cases are extremely slow-growing, the Gleason system didnt necessarily do a good job of communicating the risks for these cases. Patients with scores of 6 and 7 didnt have a clear picture of the nature of their particular cancer.
Read Also: How Do You Find Your Prostate
How Is A Gleason Score Determined
Dr. Gleason graded prostate cancer cells based on how closely they resembled normal cells. This ranged from Grade 1 to Grade 5 . After a patient had been diagnosed with prostate cancer, Dr. Gleason would analyze the two most common cell patterns in the patients tissue sample, assign each of them a grade and then combine those grades to come up with a total Gleason score.
In other words, to calculate a prostate cancer patients Gleason score, a pathologist must:
For example, if a pathologist grades a prostate cancer patients primary cell pattern as a 3 and their secondary cell pattern as a 4, then the patients Gleason score would be a 7.
Table 1 Why A Low Psa Does Not Mean You Are Cancer
The Prostate Cancer Prevention Trial included a provision that men randomized to receive placebo undergo a prostate biopsy at the end of the study, even if they had normal PSA levels and digital rectal exams. To their surprise, investigators found that many of these men had prostate cancer in some cases, high-grade prostate cancer.
PSA level 13 *Note: A PSA level over 4.0 ng/ml traditionally triggers a biopsy. Adapted with permission from I.M. Thompson, et al. Prevalence of Prostate Cancer Among Men with a Prostate-Specific Antigen Level 4.0 ng per Milliliter. New England Journal of Medicine, May 27, 2004, Table 2.
This study inadvertently provided evidence not only that prostate cancer occurs more often than once believed, but also that PSA levels may not be a reliable indicator of which cancers are most aggressive. Both findings add weight to the growing consensus that many prostate tumors currently being detected may not need to have been diagnosed or treated in the first place.
Read Also: How To Prepare For Prostate Radiation Therapy
Proposal For A New Grading System
To address the above deficiencies, a new 5 Grade Group system has been developed based on a study of > 20,000 prostate cancer cases treated with radical prostatectomy and > 5,000 cases treated by radiation therapy .
For cases with > 95% poorly-formed/fused/cribriform glands or lack of glands on a core or at RP, the component of < 5% well-formed glands is not factored into the grade Poorly-formed/fused/cribriform glands can also be a more minor component
Cancer Staging May Miss Errant Cells
Once a pathologist confirms that cancer is present, the doctor will next determine how far the cancer extends a process known as cancer staging and discuss the implications with you. This is perhaps the most important information of all for you to obtain, as it determines whether the cancer is likely to be curable, or whether it has already spread to additional tissues, making prognosis much worse.
If you were my patient, I would ask you to consider two important points. First, cancer staging actually occurs in two phases: clinical and pathological . Of the two, pathological staging is more accurate.
A second point to understand, however, is that even pathological staging can be inaccurate . A cancer spreads, or metastasizes, once a primary tumor sheds cancer cells that travel elsewhere in the body and establish other tumor sites. Metastasis is a complex process that researchers do not fully understand. What is clear is that this process involves multiple genetic mutations and steps, and that each type of cancer spreads in a unique way.
Don’t Miss: How To Get Tested For Prostatitis
What Does Gleason 6 Mean
A Gleason score of 6 is different from other prostate cancer diagnoses because it means all the biopsy samples are grade 3 . Though the samples dont look like normal tissue, no grade 4 or 5 samples were found.
Gleason 6 prostate tumors are:
- Confined to the prostate
- Not causing any symptoms
There are changes at the cellular level, but the prostate cancer is likely slow-growing and has a low-risk of metastasizing, or spreading to other areas of the body.
This knowledge allows your doctor to monitor you and see how your tumor changes over time.
Problems With The Current Gleason System
Don’t Miss: Treatment For Non Aggressive Prostate Cancer
What Is The Gleason Score
The Gleason grading system estimates the aggressiveness of the cancer by assigning a pattern to the cancer cells depending on their appearance under the microscope. A number from 1 to 5 is used as a measure of how aggressive the cancer looks under the microscope.
- If the cancerous tissue looks much like normal prostate tissue, a grade of 1 is assigned.
- If the cancer cells and their growth patterns look very abnormal, a grade of 5 is assigned.
- Grades 2 through 4 have features in between these extremes.
The most common type of prostate biopsy is a core needle biopsy. For this procedure, the doctor inserts a thin, hollow needle into the prostate gland. When the needle is pulled out it removes a small cylinder of prostate tissue called a core. This is typically repeated several times to sample different areas of the prostate.
Since multiple core biopsy samples are evaluated and prostate cancers in a single patient often have areas with different grades the pathologist assigns two grades to the examined prostate tissue. The first grade is the most common pattern seen after review of all the biopsy specimens and the 2nd grade is assigned to the next most common pattern.
What Does It Mean To Have A Gleason Score Of 6 Or 7 Or 8
The lowest Gleason Score of a cancer found on a prostate biopsy is 6. These cancers may be called well-differentiated or low-grade and are likely to be less aggressive – they tend to grow and spread slowly.
Cancers with Gleason Scores of 8 to 10 may be called poorly differentiated or high grade. These cancers tend to be aggressive, meaning they are likely to grow and spread more quickly.
Cancers with a Gleason Score of 7 may be called moderately differentiated or intermediate grade. The rate at which they grow and spread tends to be in between the other 2.
Read Also: How To Reduce Prostate Inflammation
What Is A Normal Gleason Score For Prostate Cancer
Your Gleason score doesn’t rank potential ranges like ranges set for elevated PSA tests. Instead, providers break Gleason scores into three categories:
- Gleason 6 or lower: The cells look similar to healthy cells, which is called well differentiated.
- Gleason 7: The cells look somewhat similar to healthy cells, which is called moderately differentiated.
- Gleason 8, 9 or 10: The cells look very different from healthy cells, which is called poorly differentiated or undifferentiated.
What are grade groups?
Healthcare providers established grade groups to clarify the Gleason score system. Those grade groups are:
- Grade Group 1 = Gleason 6 .
- Grade Group 2 = Gleason 3+4=7.
- Grade Group 3 = Gleason 4+3=7.
- Grade Group 4 = Gleason 8.
- Grade Group 5 = Gleason 9-10.
Grading In Different Prostatic Tissue Samples
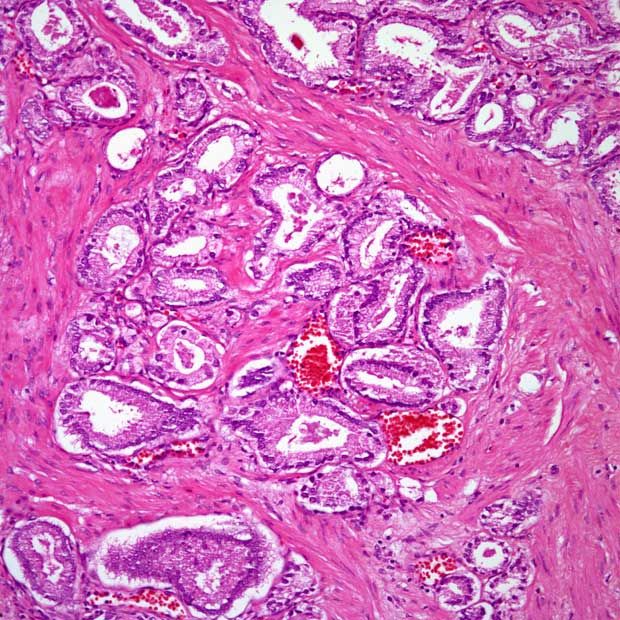
Gleason grading should be performed in all prostatic tissue samples, including needle core biopsy specimens. Indeed, of Gleason’s original series of 2911 patients, 60% were graded solely on the basis of a needle biopsy. A Gleason grade should be assigned even to needle biopsy cases with minimal prostatic carcinoma, defined as less than 1mm of tumor., Of importance, a small amount of carcinoma in needle biopsy tissue should not be equated with well-differentiated Gleason score 24 adenocarcinoma. Most minimal adenocarcinomas in needle biopsy tissue are intermediate Gleason grade, usually of a score of 6. Comparisons of Gleason grade in needle biopsy with Gleason grade in the matched whole prostate gland indicate exact correlation in 43% of cases and agreement to within±1 score unit in 77% of 3789 cases . Undergrading of tumor in the needle biopsy, with a higher Gleason score in the matched whole gland, is the most common problem, occurring, on average, in 42% of all cases. Overgrading of carcinoma in needle biopsy tissue also takes place, but with a much lower mean of 15% of all cases. For needle biopsy cases, there are several sources of grading error, including difficulty in appreciation of an infiltrative growth pattern, tissue sampling error , tissue distortion, pathologist experience, and observer variability.
Also Check: What Is The Normal Level For Prostate
Biopsy Gleason Score Underestimates Disease Grade And Extent
On the basis of the intermediate end points of pathologic grade and stage, biopsy Gleason score underestimates both grade and extent of disease. Among men at a median age of 58 years who had at least a 10-core prostate biopsy, 36% of Gleason score 5 to 6 tumors were upgraded at radical prostatectomy if tertiary patterns were considered, and 25% were if tertiary patterns were not considered.20 The rate of upgrading was 35% for Gleason scores 5 to 6 on biopsy to Gleason score 7 at radical prostatectomy when studies that had evaluated at least 100 patient cases since 1992 were included.20
In addition to upgrading, men who are thought to harbor Gleason score 6 on biopsy may have more extensive nonorgan-confined disease. In a study evaluating men who met different criteria for enrollment in active surveillance, 70% to 80%, depending on inclusion criteria, were organ confined and Gleason score 6 on pathologic review of radical prostatectomy specimens.21 Furthermore, among men chosen for active surveillance based on a Gleason score 6 and treated surgically after a median of 1.3 years after enrollment, 80% had organ-confined disease.22 Thus, one could argue that if one in three to one in five men thought to harbor Gleason score 6 tumors actually have high-grade or nonorgan-confined disease, assigning a noncancer moniker to these low-grade cancers would disadvantage a substantial proportion of men by delaying curative therapy.
What Does It Mean If My Biopsy Report Mentions The Word Core
The most common type of prostate biopsy is a core needle biopsy. For this procedure, the doctor inserts a thin, hollow needle into the prostate gland. When the needle is pulled out it removes a small cylinder of prostate tissue called a core. This is often repeated several times to sample different areas of the prostate.
Your pathology report will list each core separately by a number assigned to it by the pathologist, with each core having its own diagnosis. If cancer or some other problem is found, it is often not in every core, so you need to look at the diagnoses for all of the cores to know what is going on with you.
Recommended Reading: Can Inflamed Prostate Cause Back Pain
The Updated Gleason Grading System Is Misleading For Patients And Physicians
The Gleason grading system, based on five architectural patterns of a tumor, has evolved over time.4 For practical purposes, Gleason patterns 1 and 2, or scores 2 to 4 noted in the classic system, are not diagnosed on needle biopsies because of poor correlation with radical prostatectomy grade and poor reproducibility among expert pathologists.5 The Gleason system has been modified based on a 2005 consensus conference,4 whereby lesions previously referred to as Gleason scores 2 to 4 in the classic system are now assigned a higher grade in the modified system however, those previously graded as Gleason score 6 in the classic system are often graded as Gleason score 7 tumors in the modified system. Although this modification of grading could improve the prognosis of some men who have cancer-specific outcomes intermediate between the modified Gleason score 6 and the classical Gleason score 3 + 4 cancers,6 the larger effect of the 2005 modification has been to improve the perceived cancer-specific survival by 26% through the Will Rogers phenomenon.7
What Does It Mean If My Biopsy Report Also Mentions Atrophy Adenosis Or Atypical Adenomatous Hyperplasia
All of these are terms for things the pathologist might see under the microscope that are benign , but that sometimes can look like cancer.
Atrophy is a term used to describe shrinkage of prostate tissue . When it affects the entire prostate gland it is called diffuse atrophy. This is most often caused by hormones or radiation therapy to the prostate. When atrophy only affects certain areas of the prostate, it is called focal atrophy. Focal atrophy can sometimes look like prostate cancer under the microscope.
Atypical adenomatous hyperplasia is another benign condition that can sometimes be seen on a prostate biopsy.
Finding any of these is not important if prostate cancer is also present.
You May Like: What Does An Infected Prostate Feel Like
Monitoring And Treatment Decisions
In the past, men with prostate cancerregardless of whether it was aggressive or notwere almost always treated right away with a targeted therapy like surgery or radiation. However, in recent years, experts have revisited this one-size-fits-all approach to prostate cancer.
Experts now understand that low-risk prostate cancerlike Gleason 6 tumorsmay not need treatment right away. In fact, major medical associations, including the American Urological Association and the Society for Urologic Oncology, now recommend the use of active surveillance for low-risk prostate cancer.
