Survival Outcomes By Treatment Strategies
As shown in Table and Figure , patients treated with EBRT + BT had significantly better cancerspecific survival, compared with patients treated with surgery or EBRT alone . No difference was found between EBRT and surgery by CSS outcome. When allcause mortality is considered, surgery had a significantly better OS than EBRT and a similar OS as EBRT + BT . These results suggested substantially elevated competing causes of death other than prostate cancer in patients treated with radiation over time. We then examined if salvage RT impacted the surgery vs RT comparisons by removing salvage RT patients from the surgery group. The conclusions were not substantially changed, although the statistical significance was lost in comparison of cancerspecific mortality between EBRT + BT and surgery .2). Since patients who forwent prostatectomy for RT were more likely to be older and susceptible to other causes of death, we performed stratified analyses by age . In patients 65 years, EBRT was significantly inferior to surgery in both cancerspecific mortality and allcause mortality. In patients > 65 years, EBRT was still inferior to surgery in allcause mortality, but EBRT and EBRT + BT showed a nonsignificant reduced cancerspecific mortality compared with surgery. When combined, RT was statistically significantly associated with a better cancerspecific mortality .
What About The Data On The Relative Side Effects Of Proton Therapy Vs Imrt
We pooled our data with various cancer centers in order to study about 1,000 patients who had been treated for prostate cancer with Proton Beam Therapy and compared their Quality of Life scores with those of a control group of men who had no treatment .
The EPIC questionnaire was completed by all men every three months from the beginning of treatment until at least one year after treatment. The results showed that men who were treated with proton therapy for prostate cancer had the same urinary and rectal quality of life scores as men who didn’t even have prostate cancer.
Don’t let anyone rush you into making a decision that will have consequences for the rest of your life.
Prostate Cancer Surgery Vs Prostate Cancer Radiation
After being diagnosed with prostate cancer, many men are confused about their treatment options. They probably wonder: Do I go for radiation? Do I go for surgery? Well-intended people may give certain suggestions or recommendations. But, because prostate cancer may be a life threat, prostate cancer patients need to have accurate, scientific information about their options.
Dr. David Samadi, prostate cancer expert, highlights the benefits of robotic prostatectomy surgery over radiation for prostate cancer. A study from Memorial Sloan Kettering showed a 65 percent reduced risk of prostate cancer metastasis after surgery compared to radiation.
Also, there is an analysis of more than a dozen studies which shows that prostate cancer patients do better with surgery versus radiotherapy, especially for men who have localized prostate cancer.
Patients who were treated with radiation over surgery were twice as likely to die from prostate cancer than those treated by surgery. As with any cancer, surgery is the first line of treatment.
Read Also: How To Shrink Prostate Mayo Clinic
Quality Of Life Is Better After Modern Radiotherapy Compared With Surgery
For decades, organ preservation has been an abiding principle of radiotherapy, with the underlying belief being that a person with preserved native anatomy has better physical functioning than one who has undergone surgical removal of organs followed by reconstruction. Comparing modern radiotherapy vs surgery for prostate cancer, we argue the following points: Head-to-head comparisons have shown modern radiotherapy to be much better than surgery in terms of urinary and sexual function.
While bowel toxicity has historically been moderately worse after radiotherapy, this decline in function can now be mitigated largely by using modern radiotherapy techniques, such as image guidance and possible additional rectal spacing.
Quality of life following radiotherapy has continued to improve as advances have been made in radiotherapeutic techniques, whereas prostate surgery-despite the availability of newer, once-promising techniques such as laparoscopic or robot-assisted radical prostatectomy-remains largely unchanged in regard to long-term impacts on quality of life. Thus, radiotherapy is the better choice for treatment of prostate cancer.
Financial Disclosure: Dr. Yu and Dr. Hamstra have served as paid consultants to Augmenix, Inc. Dr. Hamstra has also received grant funding from Augmenix, Inc.
How Can I Choose From Among The Options
In addition to talking with family and friends, you will need a team of physicians to help advise you. You should meet with everyone involved in your treatment planning before choosing a treatment, including:
- your primary care doctor
- a urologist to discuss surgery
- a radiation oncologist to discuss radiation therapy
- a medical oncologist to discuss hormone suppression, if your cancer is more advanced
After you meet with these doctors, you can make an informed decision regarding your treatment options. You may have an early-stage or moderately advanced cancer with no evidence of spread to other organs . If so, your two major treatment options are active surveillance , surgery or radiation therapy .
You may have advanced cancer and require hormonal suppression therapy or chemotherapy. If so, you will need a medical oncologist to administer these drugs. Doctors use hormone-ablation therapy to treat advanced prostate cancer. It suppresses androgen because these hormones stimulate most prostate cancer growth. Your internist, urologist, radiation oncologist or medical oncologist may administer the treatment. Depending on the stage of the cancer, your doctor may use hormone suppression therapy and radiation therapy to help control your disease. You may receive hormone suppression therapy for as little as four to six months, or for as long as two to three years.
Don’t Miss: Fiducial Marker Prostate
Remission And The Chance Of Recurrence
A remission is when cancer cannot be detected in the body and there are no symptoms. This may also be called having no evidence of disease or NED.
A remission can be temporary or permanent. This uncertainty causes many people to worry that the cancer will come back. Although there are treatments to help prevent a recurrence, such as hormonal therapy and radiation therapy, it is important to talk with your doctor about the possibility of the cancer returning. There are tools your doctor can use, called nomograms, to estimate someones risk of recurrence. Understanding your risk of recurrence and the treatment options may help you feel more prepared if the cancer does return. Learn more about coping with the fear of recurrence.
In general, following surgery or radiation therapy, the PSA level in the blood usually drops. If the PSA level starts to rise again, it may be a sign that the cancer has come back. If the cancer returns after the original treatment, it is called recurrent cancer.
When this occurs, a new cycle of testing will begin again to learn as much as possible about the recurrence, including where the recurrence is located. The cancer may come back in the prostate , in the tissues or lymph nodes near the prostate , or in another part of the body, such as the bones, lungs, or liver . Sometimes the doctor cannot find a tumor even though the PSA level has increased. This is known as a PSA-only or biochemical recurrence.
What The Research Shows About Radiation Vs Surgery
The ProtecT trial was a 10-year, randomized clinical study designed to compare radical prostatectomy, external-beam radiotherapy and active surveillance for the treatment of localized prostate cancer.
The results, published in 2016, showed that the rate of disease progression among men assigned to radiotherapy or radical prostatectomy was less than half the rate among men assigned to active monitoring. However, there was no significant difference in survival at the median 10-year mark for radiation therapy, surgery or active surveillance.
If youre interested in directly comparing treatment outcomes by treatment method and risk group , the Prostate Cancer Free Foundation provides an interactive graph on its website with information from data obtained from over 100,000 prostate cancer patients over a 15-year period.
As discussed earlier in the sections on the side effects of radiation therapy and surgery, the researchers conducting the ProtecT trial also looked at side effects and quality-of-life issues and found that the three major side effects of these two treatment options that affect quality of life after prostate cancer treatment are urinary incontinence, sexual dysfunction and bowel health.
The trial found that urinary leakage and erectile dysfunction were more common after surgery than after radiation therapy. Gastrointestinal bowel problems were more common after radiation therapy.
Don’t Miss: How Long Can You Stay On Lupron For Prostate Cancer
Table 1 Why A Low Psa Does Not Mean You Are Cancer
The Prostate Cancer Prevention Trial included a provision that men randomized to receive placebo undergo a prostate biopsy at the end of the study, even if they had normal PSA levels and digital rectal exams. To their surprise, investigators found that many of these men had prostate cancer in some cases, high-grade prostate cancer.
PSA level 13 *Note: A PSA level over 4.0 ng/ml traditionally triggers a biopsy. Adapted with permission from I.M. Thompson, et al. Prevalence of Prostate Cancer Among Men with a Prostate-Specific Antigen Level 4.0 ng per Milliliter. New England Journal of Medicine, May 27, 2004, Table 2.
This study inadvertently provided evidence not only that prostate cancer occurs more often than once believed, but also that PSA levels may not be a reliable indicator of which cancers are most aggressive. Both findings add weight to the growing consensus that many prostate tumors currently being detected may not need to have been diagnosed or treated in the first place.
Tools To Help You Decide
The Predict Prostate tool can help you decide between monitoring and more radical treatment. It is for men whose prostate cancer hasn’t spread.
It can’t tell you exactly what is going to happen in the future, but it gives you an idea about the differences in survival between the different treatment options. The tool works less well for men with a very high PSA or those with a fast growing or large tumour.
To be able to use the tool you need to know the following about your cancer:
- PSA level
- stage of cancer
- grade of cancer
Read Also: How Are Fiducial Markers Placed In The Prostate
Surgery For Prostate Cancer
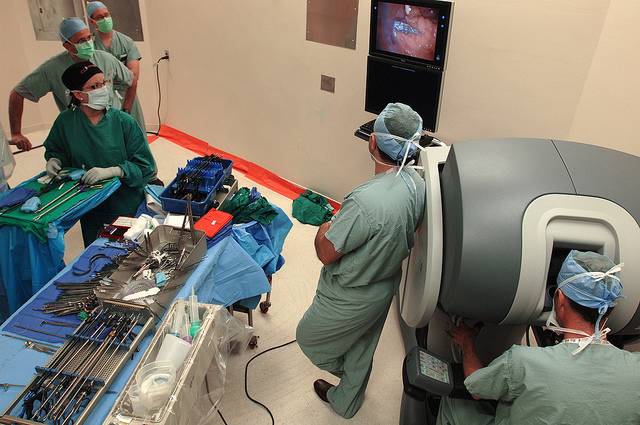
A radical prostatectomy is the surgical removal of the prostate. This procedure may be performed through traditional open surgery, which involves one large incision in the abdomen. Laparoscopic surgery using the robotic daVinci® Surgical System is a minimally invasive alternative. Robotic surgery only requires a few small incisions in the abdomen, which may result in reduced pain, lower risk of infection and a shorter hospital stay after surgery.
The technology associated with the robotic surgical system is designed to give the surgeon greater precision and control, which may help spare healthy tissue and one or two of the nerve bundles on the sides of the prostate. This often allows the patient to have better erectile functionin both the short term and long term.
Watchful Waiting And Active Surveillance
Watchful waiting is an adequate approach in patients who are at low risk of death from prostate cancer because of their limited life expectancy due to severe comorbidities., Watchful waiting resulted in similar overall survival when compared with radical prostatectomy, but disease-specific survival was better in patients who had undergone surgery. For some patients it turns out to be hard to persist on a watchful waiting policy, and many men drop out and seek active treatment within several years, mostly when PSA elevation is noted.
Active surveillance is a novel and fascinating approach to distinguish between patients who are at higher risk and need active therapy and patients who are at low risk for disease progression., This approach avoids the risks of therapy while allowing early detection of those patients who are prone to progress. In these high-risk individuals, delayed active treatment is offered. Periodic monitoring of the PSA serum level, digital rectal exam, and repeated prostate biopsies are performed in patients who are on active surveillance, and active therapy is started when predefined threshold values are reached. This concept makes it possible to offer curative treatment to individuals who are at high risk for disease progression as indicated by active surveillance parameters.
Recommended Reading: Define Prostate
Choosing Between Radical Prostatectomy And Radiation Therapy
The main advantage of radical prostatectomy is that it is arguably a one time procedure. It takes just a few hours to completely remove the affected prostate and the patient is likely to recover fully, albeit gradually and with the monitoring of a urologist. The main disadvantage is that it is appropriate only where the cancer has not spread to other organs outside the prostate. If it has spread, then removing the prostate and leaving behind other affected organs will have no effect at all. In cases where the cancer has spread, radiation therapy may be the more reasonable choice.
Other factors that urologists and surgeons consider before suggesting either procedure include:
1. Age of the patient Radical prostatectomy is offered mostly to men under 70 years of age because they are more likely to live longer and be able to survive any long term effects of the disease.
2. The natural progression of the disease Slow progression of a non-aggressive tumor does not lend itself to surgery. This is a case that can be managed by what is called watchful waiting where the disease is monitored constantly but treatment is deferred for a while.
3. The possibility of cure The goal of radical prostatectomy is to cure the patient of prostate cancer. If for whatever reason it appears that it is unlikely that this objective will be achieved, then radiation therapy or other forms of treatment should be preferred.
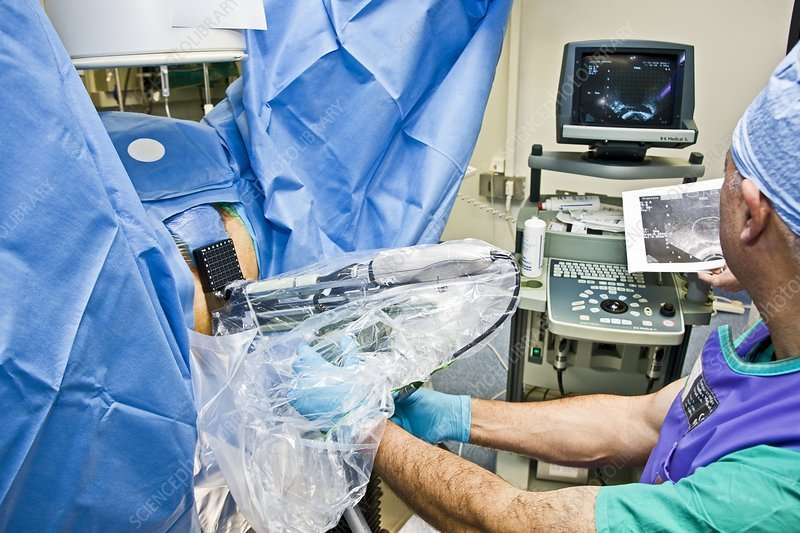
What Happens During Radiation Therapy
Radiation therapy uses high-energy x-rays or a stream of particles . High doses of radiation can destroy abnormal cancer cells. Each treatment destroys some of the cancer cells at a microscopic level. Patients do not feel the radiation during treatment. They will only hear some electrical noise and may see light from the machine.
Don’t Miss: Seminal Vesicle Massage
Treatments May Have Side Effects
The treatment options for early-stage prostate cancer fall into three broad categories: surgery, radiation therapy, and active surveillance. Your doctor will make a treatment recommendation based on your numbers as well as a mathematical tool known as a nomogram, which can help you and your doctor better assess how extensive your cancer is likely to be and whether it is likely to become active in the future.
Yet clinical studies have not provided any evidence that one treatment is better than another or that any treatment at all actually prolongs life: The average 5-, 10-, and 15-year survival rates are virtually the same for all treatment options in early-stage prostate cancer, including active surveillance. Its also important to understand that no mathematical model is foolproof, and some men diagnosed with early-stage, locally confined disease will later find out that their cancer was more extensive than originally believed.
If you are diagnosed with early-stage prostate cancer, you have a number of treatments to choose from. A brief comparison is listed in Table 2.
Survival Rates For Bladder Cancer
Survival rates can give you an idea of what percentage of people with the same type and stage of cancer are still alive a certain amount of time after they were diagnosed. They cant tell you how long you will live, but they may help give you a better understanding of how likely it is that your treatment will be successful.
Keep in mind that survival rates are estimates and are often based on previous outcomes of large numbers of people who had a specific cancer, but they cant predict what will happen in any particular persons case. These statistics can be confusing and may lead you to have more questions. Talk with your doctor about how these numbers may apply to you, as he or she is familiar with your situation.
Read Also: Prostate Biopsy Cost In Usa
Recommended Reading: Expressed Prostatic Secretion
Comparison Of Oncological Outcomes Between Radical Prostatectomy And Radiotherapy By Type Of Radiotherapy In Elderly Prostate Cancer Patients
- Department of Urology, Beijing Hospital, National Center of Gerontology, Beijing, China
Objective: We aimed compare the oncologic outcomes of radical prostatectomy with those of external beam radiotherapy , brachytherapy , or EBRT + BT in elderly patients with localised prostate cancer .
Methods: Localised PCa patients aged 70 years who underwent RP, EBRT, BT, or EBBT between 2004 and 2016 were identified from the Surveillance, Epidemiology, and End Results database. Multivariable competing risks survival analyses were used to estimate prostate cancer-specific mortality and other-cause mortality . Subgroup analyses according to risk categories were also conducted.
Results: Overall, 14057, 37712, 8383, and 5244 patients aged 70 years and treated with RP, EBRT, BT, and EBBT, respectively, were identified. In low- to intermediate-risk patients, there was no significant difference in CSM risk between RP and the other three radiotherapy modalities . The corresponding 10-year CSM rates for these patients were 1.2%, 2.3%, 2.0%, and 1.8%, respectively. In high-risk patients, EBRT was associated with a higher CSM than RP , whereas there was no significant difference between RP and BT or RP and EBBT . The 10-year CSM rates of high-risk patients in the RP, EBRT, BT, and EBBT groups were 7.5%, 10.2%, 8.3%, and 7.6%, respectively. Regarding OCM, the risk was generally lower in RP than in the other three radiotherapy modalities .
How To Decide Between Radiation And Surgery For Localized Prostate Cancer
If youre like most men whove been diagnosed with prostate cancer, youve been told you have early-stage, localized prostate cancer, meaning the disease hasnt spread beyond the prostate. You may have also been told that you have choices about what you want to do next.
Unless your cancer is aggressive, youve probably been presented with three treatment options: active surveillance, radiation therapy or surgery. If you arent comfortable with active surveillance, or if its not an advisable option for you, you may have to decide between radiation therapy and surgery to treat your cancer.
Many men want to know whats the best treatment for their localized prostate cancer. But its a misconception that you have only one better or safer choice. In most cases, either radiation therapy or surgery is an equally good choice when we look at long-term survival.
Weve heard of some physicians telling men of their prostate cancer diagnosis and asking them to make a treatment decision at the same appointment. But prostate cancer progresses slowly, so most men have time to think about their options and shouldnt feel pressured into making an immediate decision.
How you feel about the big three possible side effects of treatmenturinary incontinence, sexual dysfunction and bowel healthmay be the deciding factor for you.
To help you through the process of making this decision, this article covers:
Also Check: Does Cialis Shrink An Enlarged Prostate
