Recent Findings About Regaining Potency After Radical Prostatectomy
It is important to remember that regaining erectile function takes time after radical robotic prostatectomy. Most studies in the literature use endpoints of 18-36 months after prostate cancer surgery. Nerve tissue can be easily damaged during robotic prostatectomy, regardless of the skill of the surgeon, and takes a long time to regenerate. It is believed that early postoperative medical therapy can aid an earlier return to potency.
Dr. Ahlering, a physician with UC Irvine Medical in Orange County, CA. has pioneered the use of electrocautery-free preservation of the neurovascular bundles which are essential for the return of potency after prostate surgery. A recent study by Dr. Patrick Walsh and associates at John Hopkins has shown that mono and bipolar cautery near the potency nerves severely impact the erectile function of dogs. Mono and bipolar cautery are routinely used by many institutions to limit the bleeding during surgery by heat-sealing or ‘cauterizing’ the bleeding vessels.
The nerves for potency are intertwined with a bundle of blood vessels, which must be controlled during prostate cancer surgery to prevent large blood losses. Thus to preserve the nerves of potency, a surgeon also must prevent the bleeding of these vessels also. Cautery is considered a standard method of sealing the blood vessels, allowing the nerve bundles to now be properly visualized.
For comparison we show the standard data on open prostatectomy potency :
How Your Doctor Monitors You After Treatment
After treatment you have follow up appointments, which usually include regular blood tests to check the levels of a protein called prostate specific antigen . They check to see if your PSA level rises. And they also look at how quickly it rises.
An increase in PSA can mean there are prostate cancer cells in your body. The cells might be in or around the prostate. Or they might have spread to other parts of your body. You might need treatment if it rises.
Prostate cancer that comes back after treatment is called recurrent prostate cancer.
Read Also: What Is Perineural Invasion In Prostate Cancer
Are There Any Surgical Techniques That Have Been Developed To Improve Erectile Function Outcomes
At this time, there are several different surgical approaches to carry out the surgery, including retropubic or perineal approaches as well as laparoscopic procedures with freehand or robotic instrumentation. Much debate but no consensus exists about the advantages and disadvantages of the different approaches. Further study is needed before obtaining meaningful determinations of the success with different new approaches.
Recommended Reading: How To Decalcify The Prostate
What Can Be Done
If your prostate cancer has recurred, your healthcare provider will likely order some imaging tests to better determine where in your body the cancer has returned. Bone scans, CT scans, and MRIs are the most common tests ordered to find where in the body prostate cancer has recurred.
Many treatment options are available for prostate cancer that has returned. The one that you and your healthcare provider choose depends on individual factors such as what treatment you have already received, where in the body your prostate cancer has returned, how your cancer has spread, your general health, and your age.
If your prostate cancer is thought to have recurred in only a small area and has not spread to other areas of the body, then radiation therapy to that area may be an option.
If your prostate cancer has most likely spread to multiple areas of the body, then hormonal therapy would likely be an option. Chemotherapy can also be used when the cancer has spread to multiple sites.
Surgically Removing The Prostate Gland
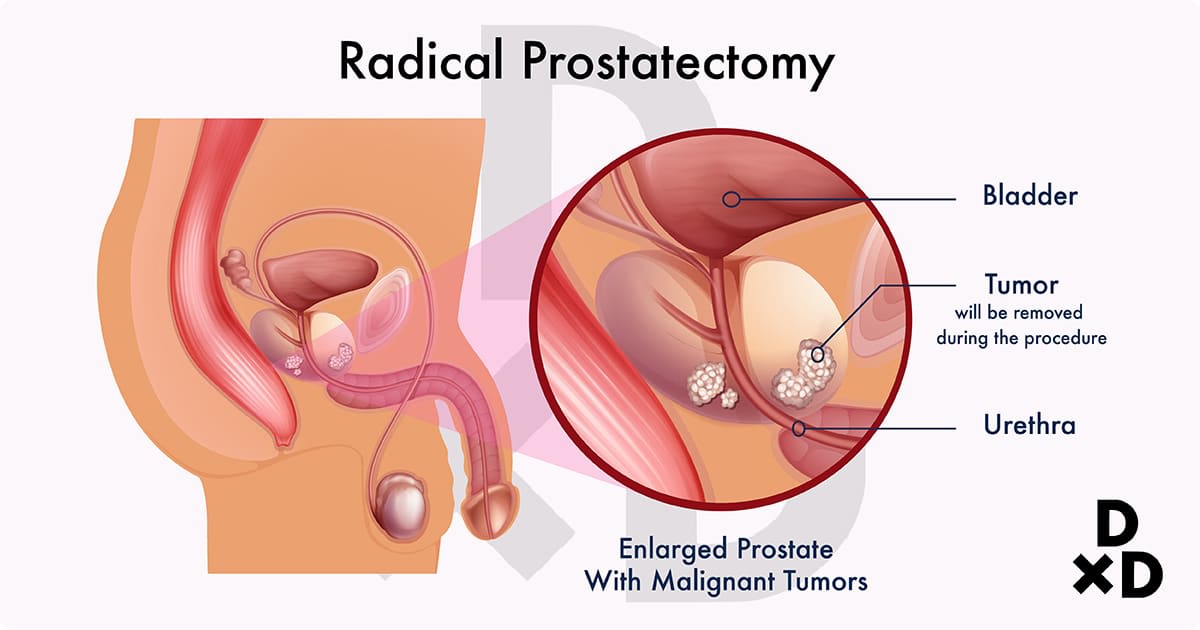
A radical prostatectomy is the surgical removal of your prostate gland. This treatment is an option for curing prostate cancer that has not spread beyond the prostate or has not spread very far.
Like any operation, this surgery carries some risks.
A recent trial showed possible long-term side effects of radical prostatectomy may include an inability to get an erection and urinary incontinence.
Before having any treatment, 67% of men said they could get erections firm enough for intercourse.
When the men who had a radical prostatectomy were asked again after 6 months, this had decreased to 12%. When asked again after 6 years, it had slightly improved to 17%.
For urinary incontinence, 1% of men said they used absorbent pads before having any treatment.
When the men who had a radical prostatectomy were asked again after 6 months, this had increased to 46%. After 6 years, this had improved to 17%.
Out of the men who were actively monitored instead, 4% were using absorbent pads at 6 months and 8% after 6 years.
In extremely rare cases, problems arising after surgery can be fatal.
Its possible that prostate cancer can come back again after treatment. Your doctor should be able to explain the risk of your cancer coming back after treatment, based on things like your PSA level and the stage of your cancer.
After a radical prostatectomy, youll no longer ejaculate during sex. This means you will not be able to have a child through sexual intercourse.
Also Check: Can Zytiga Cure Prostate Cancer
What Is The Recovery Time After Radical Prostatectomy
You may feel tired for a few weeks after surgery. Light exercise such as walking can help with the healing process. You should avoid heavy lifting for several weeks.
You may have urinary incontinence or leakage for weeks to months after the surgery, although most people recover continence after surgery. Recovery of sexual function is expected to take months. Your doctor may start you on a medication to help with recovery of erections.
Youll need regular follow-ups with your healthcare provider to monitor for evidence of cancer recurrence and manage effects from the surgery. They can work with you to improve any problems with erectile dysfunction or bladder control.
Recommended Reading: Methods Of Treating Prostate Cancer
Common Side Effects Of Turp
Common side effects after surgery include:
- bleeding after the operation this usually reduces over time and should stop after four weeks
- retrograde ejaculation most men are able to have erections and orgasms after surgery to treat an enlarged prostate. However, they may not ejaculate because the bladder neck is removed along with prostate tissue. This causes the ejaculate to collect with urine and pass out of the body in the next urination.
Read Also: Fiducials Prostate Cancer
What Is Prostate Cancer
Prostate cancer develops in the prostatea small gland that makes seminal fluid. It is the second most common type of cancer in men. Prostate cancer usually grows over time and in the beginning stays within the prostate gland, where it may not cause serious harm. While some types of prostate cancer grow slowly and may need minimal or no treatment, other types are aggressive and can spread quickly.
Prostate cancer that is caught early has a better chance of successful treatment.
What Are The Side Effects Of Hormone Therapy For Prostate Cancer
Testosterone is the primary male hormone and plays an important role in establishing and maintaining the male sex characteristics, such as body hair, muscle mass, sexual desire, and erectile function. Most men who are on hormone therapy experience at least some effects related to the loss of testosterone, but the degree to which you will be affected by any one drug regimen is impossible to predict. Side effects from testosterone-lowering therapies include hot flashes, breast enlargement or tenderness, loss of bone mineral density and fractures, increased weight gain , higher cholesterol, a higher risk of diabetes, and a slightly higher risk of heart problems like heart attacks and chest pains. Some men complain of mood problems and depression during this time as well. Dont be afraid to discuss these issues with your doctors. For all of these reasons, maintaining a healthy overall lifestyle is vital to doing well with hormonal therapies over time.
Recommended Reading: How Long Can You Take Lupron For Prostate Cancer
Your Emotions And Sex
Your prostate cancer and its treatment wonât just affect your body. Theyâll also have a serious impact on your emotions. Stress and anxiety can trigger your body to make adrenaline, which gets in the way of having sex. The more you worry, the worse the struggle. If youâre in a relationship, your partner will be going through many of the same feelings.
One of the most important things you can do is to talk to your partner. Have an honest conversation about your fears and expectations when it comes to sex. Dont assume they know how you feel. Being open with each other will help you both feel supported and help you work together to make any adjustments that you may need to stay intimate.
Talking with a mental health professional either one-on-one or with your partner can be a powerful way to help manage your emotions. A therapist can also prescribe medications that may ease stress and anxiety. A professional sex therapist can help you and your partner find ways to improve your sex life. It may also be helpful to join a support group where you can talk with others who share your experience.
Prostate Cancer Foundation: Erectile Dysfunction.
UCLA Urology: Prostate Cancer: Dealing with Erectile Dysfunction.
Albaugh, J. Reclaiming Sex & Intimacy After Prostate Cancer: A Guide for Men and Their Partners. Anthony J. Jannetti, Inc., 2012.
Harvard Prostate Knowledge: Achieving orgasm after radical prostatectomy.
What Happens If Prostate Cancer Comes Back
The prostate is a small gland about the size of a walnut that helps make seminal fluid. Its intertwined with your urinary tract system, resting below your bladder and surrounding the urethra. As you age, this gland continues to grow, sometimes resulting in benign prostatic hyperplasia. While this growth is normal, cancerous growth is not. Cancer occurs when the cells in your prostate gland begin to grow out of control.
While prostate cancer is common, especially among older men, its got a fairly positive outcome. When caught early and treated, most men survive and continue on with remission after five years. Unfortunately, for a small percentage of men, the cancer returns. To give you some clarity on this situation, heres what happens if prostate cancer comes back.
Read Also: Expressed Prostatic Secretion
Other Medications And Devices
Although medications like sildenafil and tadalafil are effective for many men with post-surgery erectile dysfunction, they arent the best choice for everyone.
If your prostatectomy causes damage to the nerves near your penis, or if you take medication for hypertension, angina or other health conditions, using an oral ED medication may not be a suitable option for you.
In this case, your healthcare provider may recommend a different type of medication or a device to help you achieve an erection. Your options may include:
-
Penile injection therapy. This involves using injectable medications to stimulate blood flow and improve your erections. These medications are typically administered using a very small needle to minimize discomfort.Although this treatment method may sound unpleasant, its relatively simple to use and has a success rate of 70 percent to 80 percent.
-
Vacuum constriction devices . Also known as a penis pump, a VCD works by creating a vacuum around your penis. This draws blood into your penis and allows it to become erect.
Prostate Cancer Recurrence After Prostatectomy: Why Does It Happen And How Do We Treat It
Filed in Life After Treatment
The concept of prostate cancer recurrence after prostatectomy puzzles many patients. A frequently asked question is how can the cancer come back if the prostate has been removed? The explanation is that, as with any cancer, if cancerous cells migrate out of the organ in which they arose before the organ is removed , they can settle and grow elsewhere. These migrating cells are called metastases, secondary deposits or secondaries.
You May Like: Prostatic Neoplasms
Before Surgery Start Your Pelvic Floor Exercises
- These should be started before surgery and only stopped once you are completely continent after the operation.
- Youll be shown how to do the exercises during your pre-operative assessment visit, but essentially these pelvic floor muscles are the ones that you use to interrupt your urine stream. A strong pelvic floor therefore allows you greater control over your continence after the operation.
- More precisely, the muscles aid urinary control whilst your valve of continence recovers from the operation. This valve essentially switches your urine stream on and off, and is affected during surgery. Stitches in the valve take 6 weeks to dissolve and the scar tissue surrounding it takes up to a year to soften, so we need to help it after the operation. By creating a strong pelvic floor with your exercises, the muscles are able to squeeze around this valve and help it to close during the recovery period.
Ill be covering how to perform the exercises in a later article as its slightly out of the scope of this article, but for now there is an excellent guide from Prostate Cancer UK here, as well as a video to watch here.
The Natural History Of Bcr
Although a rising PSA level universally precedes metastasis and PCa-specific mortality , BCR is not a surrogate for PCa-specific mortality or OS, and may pre-date local recurrence or metastasis by several years. On average, BCR precedes the appearance of clinical metastasis by 8 years after RP and by 7 years after primary definitive RT .
The natural history of BCR and the risk of subsequent metastasis may be predicted by pre- and post-treatment clinical features . These prognostic indicators are used as a means to assess the patients level of risk, and therefore, help physicians to determine whether to initiate early treatment or to adopt a strategy of active surveillance. Treatment decisions following BCR must balance the risk of metastatic disease or death with the impact of treatment, and necessitate involvement of a multi-disciplinary team, as well as informing the patient of the potential for a prolonged natural history of PSA-only recurrence .
Table 1.
Pre- and post-treatment prognostic factors in PSA-recurrent prostate cancer
Don’t Miss: Prostate Massage Dangerous
What Treatment Options Are Best For Recurrent Prostate Cancer
The most suitable treatment for prostate cancer, if it becomes an issue once again after a prostatectomy, will vary on a patient-by-patient basis. These differences are usually contingent on a combination of factors, including the increased risk markers , the area of the body where recurrence manifests, the age of the patient, personal medical history, and more.
In many cases, hormone treatment may be recommended and carried out. This option for addressing recurrent prostate cancer works by blocking the cellular and physiological effects of certain male hormones. This kind of mitigation may further be supplemented with specialized drugs that play a significant role in preventing metastatic processes and curbing the cancers rate of growth.
Other options that can effectively eradicate or adequately address prostate cancer recurrence include high-intensity focused ultrasound , radiation therapies, and certain drug-based or chemotherapeutic approaches.
How Common Is Recurrence
The recurrence of prostate cancer depends on when it was caught and treated the first time. If your doctor was able to remove the cancer while it was still confined in the prostate gland, your chances of recurrence are fairly low. If your cancer spread before treatment, such as in the case of about 10% of men, recurrence is more likely to occur. Recurrence, therefore, occurs if not all of the cancer cells were treated the first time or if the cancer was more advanced than originally believed.
Recommended Reading: Define Prostate
Can Erection Rehabilitation Be Applied To Improve Erection Recovery Rates
A relatively new strategy in clinical management after radical prostatectomy has arisen from the idea that early induced sexual stimulation and blood flow in the penis may facilitate the return of natural erectile function and resumption of medically unassisted sexual activity. There is an interest in using oral PDE5 inhibitors for this purpose, since this therapy is noninvasive, convenient, and highly tolerable. However, while the early, regular use of PDE5 inhibitors or other currently available, “on-demand” therapies is widely touted after surgery for purposes of erection rehabilitation, such therapy is mainly empiric. Evidence for its success remains limited.
What Changes Can You Expect
- Ejaculation will cease:Without a prostate gland or seminal vesicles, you will no longer experience ejaculation. Even though your orgasm may feel different, it will still be pleasurable.
- Leaking urine during sex:This is possible but does not happen to all men. Its harmless and temporary.
- Performance anxiety:Dont underestimate the emotional roller coaster of prostate cancer surgery and recovery. Its normal to worry about sex after prostate cancer. Being open and honest with your partner will help.
Keep in mind that your overall health, age, and present ED status are all factors in your recovery to sex after prostate surgery.
Less commonly, the prostate cancer tumor may bulge to one or both sides of the prostate gland, making nerve-sparing surgery extremely difficult or impossible.
Dr. Samadi will help you understand your exact prostate cancer status and the position and size of your tumor. In some cases, a nerve graft can be performed to regenerate the penile nerves for sex after prostate surgery.
- Changes in mood and libido:The psychological impact of surgery can be significant this will leave you tired and irritable, not in the mood for sex so you will need to move towards intimacy slowly and your desire will return back to normal.
You May Like: How Are Fiducial Markers Placed In The Prostate
Why Is A Simple Prostatectomy Performed
There are varying degrees of prostate enlargement.
If your prostate grows only slightly, many minimally-invasive surgeries can remove part of the gland, such as transurethral resection of the prostate .
However, if your prostate becomes very large , your surgeon will need to perform a simple prostatectomy. This involves removing the inner core of your prostate gland. Most men who undergo this type of surgery are age 60 or older.
Special diets, changes in drinking habits, and medications are often tried before surgery is recommended.
Your doctor may recommend a simple prostatectomy if your prostate is very large and you are suffering from:
- extremely slow urination
