Comparison Of Distribution Of Patient Characteristics Stratified By Whether Patient Was Upgraded To Prostatectomy Gleason 8 Or Higher
Clinicopathologic characteristics of the 136 included patients are presented in Table 1. The median age was 60.5 years, and the median pretreatment PSA was 5.8 ng/mL. Most men had clinical T1c disease. All of men had Gleason score 7, with 49.3% of these demonstrating Gleason 4 + 3 on biopsy. The median GPC was 70%. We observed that men who had pathologic upgrading at the time of RP were significantly older and had higher median GPC
When Is Brachytherapy Alone The Right Choice
For a patient with disease that is confined to the prostate and not too aggressive, brachytherapy alone is a good option. With the use of sophisticated real-time computer-based planning, we can use brachytherapy to deliver radiation in an extraordinarily precise way, with minimal exposure to the surrounding normal tissues. It is also convenient for the patient as it is done in an outpatient setting and most people are able to get back to work the next day.
But brachytherapy is not right for everyone. For some patients with less-aggressive disease, a watch-and-wait approach would also be very reasonable. At MSK, our philosophy is that when the disease is caught very early meaning a low PSA level, or nonaggressive disease as reflected by a Gleason score of 6 with evidence of cancer in only a few of the biopsy samples and no evidence from the MRI of a significant amount of disease then it would be very appropriate to do active surveillance and hold off on treatment.
Dont Miss: How To Get Rid Of Prostate Stones
Options For Treating Intermediate Risk Prostate Cancer
Finding out you or a loved one has been diagnosed with prostate cancer can be a scary thing to hear. The first thing many men ask is, what does this mean, and is my prostate cancer curable. Before I delve into treatment options with men, I like to discuss the specific risk group they belong to.
While many cancers are described as stage 1, 2, 3, or 4 cancers, localized prostate cancers are more typically described as low risk, intermediate risk, or high risk. Furthermore, many physicians group patients into sub-groups within each of these categories. These risk category groups are used to determine both how aggressive your prostate cancer is and what the best treatment may entail. Your specific risk group of prostate cancer is determined by a combination of factors, including, but not limited to, the PSA blood test value and the Gleason score determined by the prostate biopsy. This article will further discuss treatments for intermediate risk prostate cancer, specifically.
The Prostate Cancer Foundation has a nice, simple guide and video describing the prostate cancer risk groups here.
One of the best large studies to show the results of prostate brachytherapy in this population of men is NRG/RTOG 0232, a large randomized trial that included 588 men. In this trial, men with intermediate risk prostate cancer were randomized to 2 different treatments
The theory was that the combination therapy may increase the overall cure rate
Also Check: What Happens When You Get Your Prostate Taken Out
> > > One Crazy Prostate Trick All Men Over 40 Should Try
Symptomatic treatment of an enlarged prostate usually involves a combination of medication and lifestyle changes. A diet rich in fruits and vegetables may be the best option if you suffer from chronic urination. It will help the body adjust to the increased size of the prostate. Also, taking regular urination intervals will help retrain the bladder to function properly. Inactivity also contributes to urine retention, and cold temperatures can increase the urge to urinate.
Invasive treatment of enlarged prostate includes medication that relieves the pressure on the urethra and bladder. However, if the condition is severe, it may require surgical intervention. If treatment is not successful, the enlarged prostate can become a potentially life-threatening disease. As the hormone levels in the body change, the enlarged prostate can lead to various complications, including urinary retention and even cancer. This is why it is critical to see a doctor for further evaluation.
Validating This New Classification System
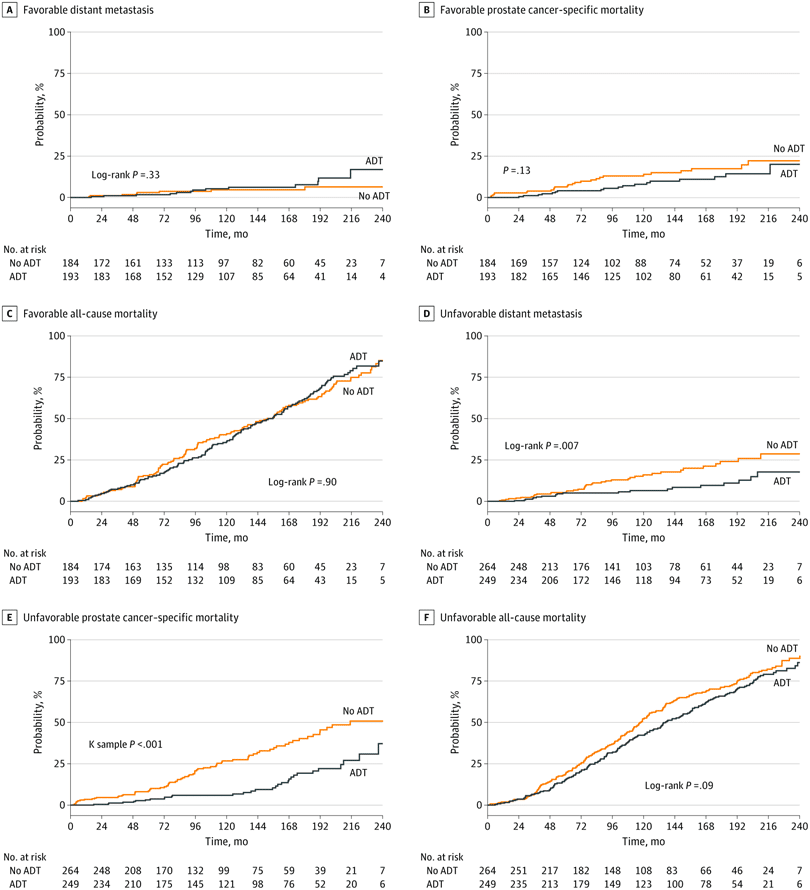
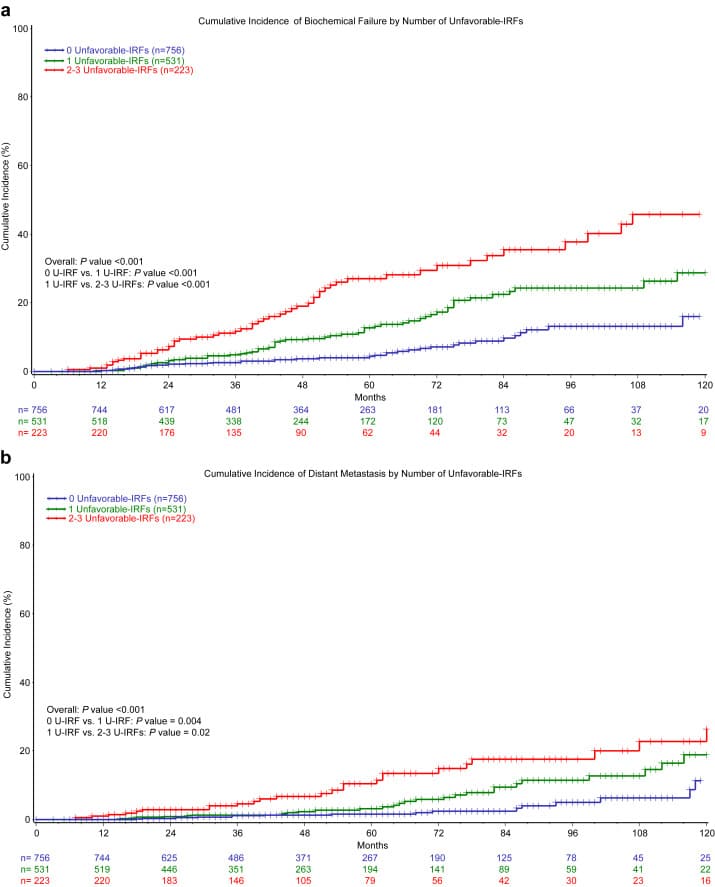
In order to validate the new classification system, the same authors retrospectively reviewed 1,024 men with intermediate-risk prostate cancer who underwent definitive DERT, defined as 81 Gy. They evaluated biochemical recurrencefree survival, incidence of distant metastasis, and PCSM in patients classified as FIR or UIR. They also examined the effect of ADT on the aforementioned endpoints. The investigators reported that primary Gleason pattern 4 , percent positive biopsy cores 50% , and multiple intermediate-risk factors were all significant predictors of increased distant metastasis in multivariate analyses. Primary Gleason pattern 4 and percent positive biopsy cores 50% both independently predicted an increased PCSM. They also reported that men with UIR disease had inferior biochemical recurrencefree survival , distant metastasis , and PCSM compared with those with FIR disease, despite the fact that UIR patients were more likely to receive ADT . Interestingly, they also found no difference in outcome between FIR patients and 511 low-risk patients treated with radiation doses of at least 81 Gy in terms of biochemical recurrencefree survival , distant metastasis , or PCSM .
Don’t Miss: How To Test For Prostate Cancer
Some Things To Consider When Choosing Among Treatments
Before deciding on treatment, here are some questions you may want to ask yourself:
- Are you the type of person who needs to do something about your cancer, even if it might result in serious side effects?
- Would you be comfortable with watchful waiting or active surveillance, even if it means you might have more anxiety and need more frequent follow-up appointments in the future?
- Do you need to know right away whether your doctor was able to get all of the cancer out ? Or are you comfortable with not knowing the results of treatment for a while if it means not having to have surgery?
- Do you prefer to go with the newest technology , which might have some advantages? Or do you prefer to go with better proven treatments that doctors might have more experience with?
- Which potential treatment side effects might be most distressing to you?
- How important for you are issues like the amount of time spent in treatment or recovery?
- If your initial treatment is not successful, what would your options be at that point?
Many men find it very stressful to have to choose between treatment options, and are very fearful they will choose the âwrongâ one. In many cases, there is no single best option, so itâs important to take your time and decide which option is right for you.
You May Like: Prognosis Of Prostate Cancer Spread To Bones
Considering Prostate Cancer Treatment Options
For most men diagnosed with prostate cancer, the cancer is found while its still at an early stage its small and has not spread beyond the prostate gland. These men often have several treatment options to consider.
Not every man with prostate cancer needs to be treated right away. If you have early-stage prostate cancer, there are many factors such as your age and general health, and the likelihood that the cancer will cause problems for you to consider before deciding what to do. You should also think about the possible side effects of treatment and how likely they are to bother you. Some men, for example, may want to avoid possible side effects such as incontinence or erection problems for as long as possible. Other men are less concerned about these side effects and more concerned about removing or destroying the cancer.
If youre older or have other serious health problems and your cancer is slow growing , you might find it helpful to think of prostate cancer as a chronic disease that will probably not lead to your death but may cause symptoms you want to avoid. You may think more about watchful waiting or active surveillance, and less about treatments that are likely to cause major side effects, such as radiation and surgery. Of course, age itself is not necessarily the best reason for your choice. Many men are in good mental and physical shape at age 70, while some younger men may not be as healthy.
Also Check: What Happens When You Have Prostate Removed
Focal Therapy For Prostate Cancer
With recent advances in MRI and targeted biopsy, we are better able to locate the exact area of prostate cancer. Men who do not have an enlarged prostate, who have prostate cancer that is detected only in a single region of the prostate and have intermediate grade cancer can be a candidate for focal therapy. This type of therapy treats only the cancerous tissue and spares the normal prostate, thereby preserving urinary and sexual function
Here at UCLA we commonly use cryotherapy or HIFU to focally treat prostate cancer. Given that this is a relatively new form of treatment, we have established rigorous post-treatment protocols using MRI and biopsies to ensure that the cancer has been adequately treated.
How Is Intermediate Prostate Cancer Treated
People with intermediate-risk prostate cancer should receive hormonal therapy for at least 4 to 6 months. Those with high-risk prostate cancer should receive it for 24 to 36 months. Hormonal therapy may also be given to those who have had surgery and microscopic cancer cells were found in the removed lymph nodes.
You May Like: Do You Have To Have A Prostate
Initial Treatment Of Prostate Cancer By Stage
The stage of your cancer is one of the most important factors in choosing the best way to treat it. Prostate cancer is staged based on the extent of the cancer and the PSA level and Gleason score when it is first diagnosed.
For prostate cancers that havent spread , doctors also use risk groups to help determine treatment options. Risk groups range from very low risk to very high risk, with lower risk group cancers having a smaller chance of growing and spreading compared to those in higher risk groups.
Other factors, such as your age, overall health, life expectancy, and personal preferences are also taken into account when looking at treatment options. In fact, many doctors determine a mans possible treatment options based not just on the stage, but on the risk of cancer coming back after the initial treatment and on the mans life expectancy.
You might want to ask your doctor what factors he or she is considering when discussing your treatment options. Some doctors might recommend options that are different from those listed here.
Recommended Reading: Likelihood Of Surviving Prostate Cancer
Treatment Of Unfavorable Intermediate Risk Prostate Cancer
Biographies:Related Content:Read the Full Video Transcript
Ashley Ross: Hi, I’m Ashley Ross speaking for UroToday. I’m a urologist at Northwestern at the AUA 2022. This year. We had some interesting discussions around the use of decipher in unfavorable, intermediate risk, prostate cancer. Genomics has played a larger role in our practices as urologists. Particularly at initial diagnosis. For a while, we were using its prognostic ability to help guide us on decisions regarding active surveillance or active treatment for men with localized prostate cancer, mostly in the low and favorable intermediate risk space. They published some retrospective, an analysis of prospective randomized data in the RTOG 0126 trial. And this was with intermediate risk patients getting radiation for their prostate cancer. Many of which were unfavorable, intermediate risk patients. And they showed that you could use a genomic classifier to stratify those patients into low risk or into high risk categories. And by that stratification determine whether or not they would have benefit from adding androgen deprivation therapy to their treatment. In those studies men without androgen deprivation therapy, who were genomic high risk had metastasis rates of about 20%.
Katie Murray: Thank you.
Recommended Reading: Best Treatment For Prostate Enlargement
Favorable Vs Unfavorable Intermediate
The DAmico risk groups, initially published in 1998, were designed to stratify patients according to the likelihood of biochemical recurrencefree survival after radical prostatectomy or radiotherapy. The current NCCN guidelines are a slight modification of this classification system. However, in 2005 an International Society of Urological Pathology conference was held in order to reach a consensus regarding the grading of prostate cancer. A consensus statement was published in 2005, and as a result of the adoption of this new grading system, the reporting of secondary pattern Gleason grade 4 disease became more prevalent. Several investigators have reported on their observation of grade migration from GS 3+3 to GS 3+4 . This grade migration could cause a number of men who previously would have been categorized as low-risk to be assigned to the NCCN intermediate-risk category because of their GS, thereby improving the prognosis of both groups . Thus, it has been hypothesized that some men with GS 3+4 intermediate-risk prostate cancer may have a low risk of PCSM and higher rates of overall survival , similar to what is seen in patients with low-risk prostate cancer.
Only one intermediate-risk factor .
GS of 3+4=7 or less.
Less than 50% of biopsy cores positive for cancer.
Those who were classified as unfavorable could have any of the following:
More than one intermediate-risk factor.
GS of 4+3=7.
Greater than 50% positive biopsy cores.
Gene And Protein Tests For Prostate Cancer
For men with prostate cancer that is localized , a major issue is that its often hard to tell how quickly the cancer is likely to grow and spread. This can make it hard to decide if the cancer needs to be treated right away, as well as which types of treatment might be good options.
Some types of lab tests, known as genomic, molecular, or proteomic tests, can be used along with other information to help better predict how quickly a prostate cancer might grow or spread, and as a result, help decide what treatment options might be best and when they should be given. These tests look at which genes or proteins are active inside the prostate cancer cells. Examples of such tests include:
These tests continue to be studied to find more areas where they can be useful in prostate cancer risk and treatment decisions.
Also Check: What Is The Risk Of Prostate Cancer
Treatment For Intermediate Risk Prostate Cancer
Intermediate risk prostate cancers are the most frequently treated prostate cancers. They are cancers that are confined to the prostate, often are Gleason 7 and have a PSA of less than 20. These cancers are treated in men with life expectancy greater than 10 years to prevent spread of the cancer in the long-term. There are a number of different effective treatment options for intermediate risk prostate cancer and the decision is often a personal one. Here at UCLA we recommend consultation with both Urologist and Radiation Oncologist to help men decide which treatment option is best for them.
You May Like: Fiducial Markers For Prostate Cancer
Why Is Risk Level Important
Risk level is all about matching the right treatment to the right patient, so its very important!
The idea of classifying PCa according to risk was originally based on the relative risk of PSA failure after prostatectomy or radiation. Until the late 1990s, the only conceivable treatment options were either whole gland surgery or radiation, and watchful waiting . The standard risk classification was the DAmico system:
- Low risk defined as stage T1c, T2a and PSA level 10 ng/mL and Gleason score 6
- Intermediate risk defined as stage T2b or Gleason score of 7 or PSA level > 10 and 20 ng/mL
- High risk defined as stage T2c or PSA level > 20 ng/mL or Gleason score 8.
Read Also: Is Fish Good For Prostate
Brachytherapy For Prostate Cancer
Brachytherapy is a form of internal radiation therapy. With this type of therapy, radiation is delivered to the prostate tumor inside the body via a catheter or another implantable device.
High-dose rate brachytherapy uses radioactive Iridium-192 to deliver high doses of radiation to the prostate tumor. Treatments are short, sometimes requiring as few as five sessions. Brachytherapy radiation more tightly surrounds the tissues were targeting, which may help spare normal tissues.
About Dr Dan Sperling
Dan Sperling, MD, DABR, is a board certified radiologist who is globally recognized as a leader in multiparametric MRI for the detection and diagnosis of a range of disease conditions. As Medical Director of the Sperling Prostate Center, Sperling Medical Group and Sperling Neurosurgery Associates, he and his team are on the leading edge of significant change in medical practice. He is the co-author of the new patient book Redefining Prostate Cancer, and is a contributing author on over 25 published studies. For more information, contact the Sperling Prostate Center.
Search the spc blog
Also Check: Green Light Photovaporization Of The Prostate
Matching Treatment For Favorable Risk Prostate Cancer
Today, the majority of PCa cases are diagnosed early thanks to PSA screening coupled with noninvasive multiparametric MRI tumor detection. It therefore makes sense that for those with Gleason 3+3 and some with Gleason 3+4, the conditions are favorable for a successful minimalist approach to managing the disease, including treatment and AS. These are considered favorable low-risk and favorable intermediate-risk prostate cancers. When carefully diagnosed and qualified, these patients may safely hold off on such aggressive radical treatments provided they protect themselves by adhering to monitoring protocols.
Modifying Risk Level Classification
The new millennium brought changes as 1) more epidemiological and demographic data accumulated, 2) the nature of PCa was better understood, and 3) sub-radical therapies such as focal ablation or hemi-ablation were developed to offer comparable cancer control but with far fewer side effect risks. A need was seen to add qualifiers to low risk PCa. Thus, the National Comprehensive Cancer Network subdivided this category into very-low and low-risk types to help doctors and patients determine for which men Active Surveillance or a sub-radical treatment would be safe choice.
The NCCN system did not qualify intermediate risk PCa. It differs a bit from DAmico, defining it as stage T2b or T2c, Gleason score of 7, and PSA level 10-20 ng/mL. However, by 2015 it was clear that this category was the largest group of PCa cases with the most heterogeneous disease characteristics. There was a wide range of PCa-specific mortality as well as biochemical or clinical recurrence after radical treatment by prostatectomy, beam radiation, and brachytherapy . Studies began to show that all Gleason 7 is not created equal men with Gleason 3+4=7 had better outcomes than those with Gleason 4+3=7, Therefore, In order to better understand this risk group, new classification systems have been proposed that help reduce its heterogeneity by subdividing men with intermediate-risk prostate cancer into favorable and unfavorable subgroups.
Read Also: How To Shrink Your Prostate Without Drugs
