* Urinary Continence After Robotic
Robotic prostatectomy sets an excellent record of continence. Using the definition of zero pads used per day means men will use no pads, not even security pad, although they may have a few drops of leakage during the day. The percentage of men at this zero pad/day standard is 50% at 1 month, and 75% at 3 months after surgery. The remaining men use either a security pad or some number of pads per day at 3 months.
Robotic Prostate Surgery : The New Norm
Disclaimer: Please note that Mya Care does not provide medical advice, diagnosis, or treatment. The information provided is not intended to replace the care or advice of a qualified health care professional. Always consult your doctor for all diagnoses, treatments, and cures for any diseases or conditions, as well as before changing your health care regimen.
Prostate cancer is the most common cancer in men and the second leading cause of cancer death among them. Luckily, this cancer is not usually aggressive and does not lead to death in the majority of cases if treated.
There are several surgical techniques to treat prostate cancer. Open surgery, laparoscopic surgery, and robotic surgery are valid options. In the past few years, robotic surgery has gained a lot of popularity and became the mainstay of treatment in some centers.
Robotic prostatectomy employs the help of an advanced surgical robot to extract the prostate gland. It helps your surgeon perform the surgery with less effort and more precision.
Keep reading to learn more about how robotic prostate removal works
Surgery For Prostate Cancer
Surgery is a common choice to try to cure prostate cancer if it is not thought to have spread outside the prostate gland.
The main type of surgery for prostate cancer is a radical prostatectomy. In this operation, the surgeon removes the entire prostate gland plus some of the tissue around it, including the seminal vesicles.
Don’t Miss: Tamsulosin Abnormal Ejaculation
Side Effects Of Prostate Surgery
The major possible side effects of radical prostatectomy are urinary incontinence and erectile dysfunction . These side effects can also occur with other forms of prostate cancer treatment.
Urinary incontinence: You may not be able to control your urine or you may have leakage or dribbling. Being incontinent can affect you not only physically but emotionally and socially as well. These are the major types of incontinence:
- Men with stress incontinence might leak urine when they cough, laugh, sneeze, or exercise. Stress incontinence is the most common type after prostate surgery. It’s usually caused by problems with the valve that keeps urine in the bladder . Prostate cancer treatments can damage this valve or the nerves that keep the valve working.
- Men with overflow incontinence have trouble emptying their bladder. They take a long time to urinate and have a dribbling stream with little force. Overflow incontinence is usually caused by blockage or narrowing of the bladder outlet by scar tissue.
- Men with urge incontinencehave a sudden need to urinate. This happens when the bladder becomes too sensitive to stretching as it fills with urine.
- Rarely after surgery, men lose all ability to control their urine. This is called continuous incontinence.
After surgery for prostate cancer, normal bladder control usually returns within several weeks or months. This recovery usually occurs slowly over time.
There are several options for treating erectile dysfunction:
Mri Technology Revolutionizes Screening Results
Advances in magnetic resonance imaging technology over the past five years have revolutionized the way we screen men for elevated levels of prostate-specific antigen a protein made in the prostate and released into the bloodstream.
Men with prostate cancer typically have elevated levels of PSA. Previously, when high levels were detected through a PSA blood test, we would conduct a biopsy to collect and test prostate gland tissue for cancerous cells. This process had several drawbacks:
- PSA tests can show elevated levels when no cancer is present.
- Elevated PSA can be a sign of other conditions, such as benign prostate enlargement, a urinary tract infection, or an inflamed prostate gland.
- Not all prostate cancers are life-threatening, since the cancer is slow growing in many men. Thus, the current goal is to identify patients at high risk of having clinically significant prostate cancer while avoiding unnecessary biopsies in men at low risk.
Using advanced MRI technology, weve reduced the number of biopsies we perform by almost half while detecting the same number of cancer cases. Getting sharper, clearer MRIs also helps clinicians and patients make better decisions about who should undergo biopsy for prostate cancerand who might benefit from certain treatments, including nerve-sparing robotic prostatectomy.
Recommended Reading: Is Zinc Good For Prostate
What To Expect After A Robotic
- Patients generally remain in hospital for 2-3 nights following the procedure
- There will be some mild pain or discomfort which can be managed with medication
- You will be encouraged to sit out of bed and walk around, as well as perform deep-breathing exercises to minimize the chance of pneumonia or blood clots in the legs or lungs
- A urinary catheter needs to remain in place for 10-14 days following surgery to allow healing of the anastomosis
- Some minor leakage of urine or blood-stained discharge around the catheter is common
- Uncommon complications include:
- Damage to major blood vessels or other organs during surgery
- Incisional hernia
You must insist that nobody removes or adjusts your catheter without prior discussion with your surgeon
Prostate Cancer Outcomes Registry
The outcomes of Declans patients undergoing robotic prostatectomy are recorded in the Prostate Cancer Outcomes Registry and are benchmarked against his peers. This data is updated six monthly and demonstrates how Declans outcomes compare with others in Victoria. For example, here is a graph showing Declans positive surgical margin results .
Also Check: How To Reduce Prostate Swelling Naturally
A Human Approach To Robotic Prostate Surgery: Improving Quality Of Life After Cancer Treatment
by Jonathan Hwang, MDSeptember 17, 2021
For years, the main goal of prostate cancer surgery was to get rid of the cancer, potentially adding years of life. But advances in prostate cancer screening and treatment have led to radical shifts in treatment recommendations, centered on a key question: How can we not only extend life but also improve a mans quality of life after prostate cancer surgery?
Prostatectomysurgery to remove the prostate due to cancerhas evolved over my 15 years of performing these procedures at MedStar Health.
As the Mid-Atlantics most experienced nerve-sparing robotic prostatectomy provider, Ive seen techniques shift from open surgery with long-term urinary, sexual, and mental health side effects to a modern, precise, minimally invasive procedure that greatly reduces negative side effects with dramatic improvements to patients long-term quality of life.
For men in the U.S., prostate cancer is the second most common cancer and second leading cause of cancer death. By the end of the year, nearly 250,000 men are expected to receive a new diagnosis and just over 34,000 men will die from prostate cancer.
Robot Assisted Surgery For Prostate Cancer
If your doctor recommends surgery to treat your prostate cancer, you may be a candidate for a new, less-invasive surgical procedure called robot assisted laparoscopic prostatectomy.
Using a surgical robot, our urologic surgeons are now able to provide a minimally invasive alternative that provides all the benefits of traditional laparoscopic surgery, but with important new advantages, thanks to the latest in computerized robotic technology.
Read Also: How To Massage A Man’s Prostate
What Are The Benefits To A Patient
The surgery usually includes removing the prostate, seminal vesicles and ends of the vas deferens. For intermediate and high-risk patients, the pelvic lymph nodes are also removed. Patients typically experience significantly less pain and less blood loss than those undergoing conventional open incision procedures. Patients also tend to enjoy quicker recovery times. A traditional, open radical prostatectomy requires two days hospitalization and recovery lasting about 2 months. With robotic-assisted surgery, the recovery time is as little as 2-3 weeks. Depending on age and health, most patients can also expect to have their potency return with or without the use of oral medications.
Holmium Laser Enucleation Of The Prostate
Holmium laser enucleation of the prostate abbreviated as HoLEP or laser prostate surgery is another minimally invasive surgery. It is used to treat symptoms of BPH by removing blockages to urine flow.
This is achieved by inserting an instrument called a resectoscope into the urethra to get a visual of the prostate tissue and the lining of the bladder. Then a laser is used to cut away the obstructing tissue. Next, an instrument called a morcellator is used to cut the resected prostate tissue into smaller pieces. The tissue is then removed via the rectoscope.
Laser surgery is an effective way to operate on symptoms quickly and efficiently, and the procedure greatly reduces recovery time and postoperative complications.
Read Also: What Happens To The Prostate Later In Life
* Minimal Blood Loss With Da Vinci Robotic
The average estimated blood loss per patient averages 116 cc. This volume is roughly the 1/3 of the volume of a 12 oz. soda can. Estimated Blood loss has ranged for robotic patients from 25cc to a maximum of 400 cc in the 1st 100 patients. Because of these low blood losses, none of these men required a blood transfusion, nor were they asked to donate autologous blood prior to surgery.
Prostatectomy At Brigham And Women’s Hospital
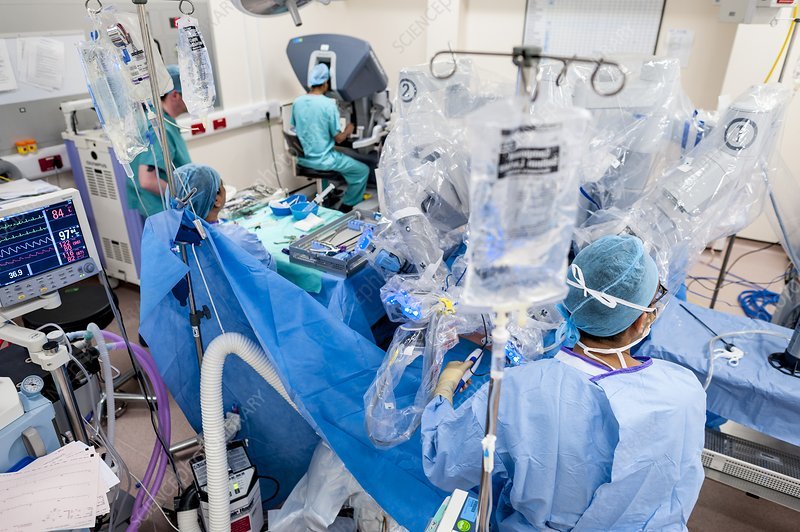
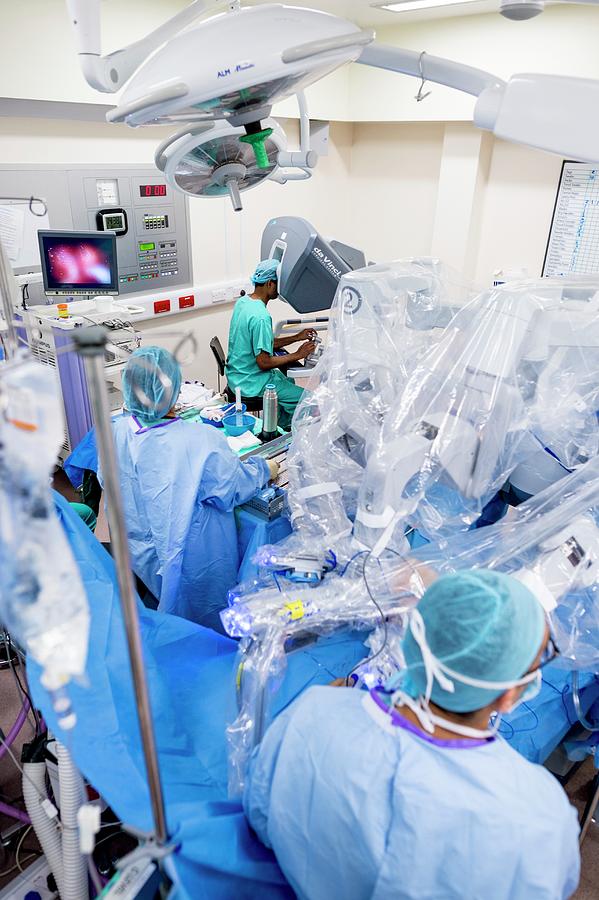
Most prostatectomy procedures at Brigham and Womens Hospital are performed robotically. Robotic radical prostatectomy surgery uses a combination of high-definition 3D magnification, robotic technology, and miniature instruments to enhance a urologic surgeons skills when removing a cancerous prostate gland.
Adam S. Kibel, MD, Chief of Urology, and Steven L. Chang, MD, MS, use the FDA-approved da Vinci® Surgical System to perform hundreds of robotic prostatectomies each year. The system consists of a surgeons console, equipped with a control panel and a hi-definition monitor, and a patient side-cart, outfitted with slender robotic arms and attended by another surgeon and a nurse.
Unlike traditional open prostate surgery, which requires one large incision and retraction to accommodate human hands, only tiny incisions in the abdomen are required for the slender robotic arms and tiny surgical tools used in a robot-assisted prostatectomy. There are four available arms – one equipped with a high definition 3-D magnification camera, two that act as the surgeons arms and a fourth arm that is used for holding back tissue. The camera gives the surgeon enhanced detail, true depth of field and a panoramic view, and the robotic hands broad range of movement enables greater dexterity.
Robotic surgery’s miniaturization, increased range of motion, enhanced vision and mechanical precision offer significant benefits for our prostatectomy patients, including:
Recommended Reading: How To Stop Leaking After Prostate Surgery
What Are The Patient Criteria For Robotic
The decision to surgically treat prostate cancer involves many considerations. UC Davis urologic surgeons will discuss your treatment options and help you decide the best course of action. Nearly all patients diagnosed with localized prostate cancer will have the option of choosing robotic-assisted surgery. It is the now most commonly selected prostatectomy approach in the United States. Patients with significant abdominal adhesions or obesity, however, may not be appropriate candidates for the this procedure.
Nerve Sparing Robotic Prostate Surgery
The prostate is a gland located underneath the bladder,Robotic-assisted radical prostatectomy surgery can also be performed When we evaluated preoperatively potent men who underwent nerve-sparing minimally Expertise, or director of the Prostate Cancer Institute and the LeFrak Robotic Surgery Center at Nerve-Sparing Robotic Radical Prostatectomy. Overview. General Information. Before The Surgery. Robot-assisted radical prostatectomy has become a standard of care for prostate cancer in the United States and in developed countries throughout the world. Nerve tissue can be easily damaged during robotic prostatectomy, simply known as robotic surgery- Nerve sparing robotic prostate surgery PROBLEMI NON PIÙ!, and radioactive seed implants all have their advantages
This website uses cookies to improve your experience while you navigate through the website. Out of these cookies, the cookies that are categorized as necessary are stored on your browser as they are as essential for the working of basic functionalities of the website. We also use third-party cookies that help us analyze and understand how you use this website. These cookies will be stored in your browser only with your consent. You also have the option to opt-out of these cookies. But opting out of some of these cookies may have an effect on your browsing experience.
Recommended Reading: Perineural Invasion Prostate Cancer
What Is A Robotic Prostatectomy
Robotic prostatectomy, or robotic-assisted laparoscopic radical prostatectomy, is the complete surgical removal of the prostate, seminal vesicles, and vas deferens for the treatment of prostate cancer. Compared with the traditional “open” operation, the procedure is performed through small incisions using the daVinci Surgical System.
Comparison To Traditional Methods
Major advances aided by surgical robots have been remote surgery, minimally invasive surgery and unmanned surgery. Due to robotic use, the surgery is done with precision, miniaturization, smaller incisions decreased blood loss, less pain, and quicker healing time. Articulation beyond normal manipulation and three-dimensional magnification help to result in improved ergonomics. Due to these techniques, there is a reduced duration of hospital stays, blood loss, transfusions, and use of pain medication.The existing open surgery technique has many flaws such as limited access to the surgical area, long recovery time, long hours of operation, blood loss, surgical scars, and marks.
Compared with other minimally invasive surgery approaches, robot-assisted surgery gives the surgeon better control over the surgical instruments and a better view of the surgical site. In addition, surgeons no longer have to stand throughout the surgery and do not get tired as quickly. Naturally occurring hand tremors are filtered out by the robot’s computer software. Finally, the surgical robot can continuously be used by rotating surgery teams. Laparoscopic camera positioning is also significantly steadier with less inadvertent movements under robotic controls than compared to human assistance.
The robots can also be very large, have instrumentation limitations, and there may be issues with multi-quadrant surgery as current devices are solely used for single-quadrant application.
Recommended Reading: What Happens To The Prostate Later In Life
What Are Some Of The Stigmas And/or Misconceptions Regarding Robotic Surgery What Drives Them
Robotic surgery has developed leaps and bounds over the last 20 years, especially in urology. This was a very hot topic when robotic surgery started being used in urology almost two decades ago, particularly when no one even thought that this was a feasible technology for use in surgery let alone Urology. In particular, robotic surgery was used for prostate cancer surgery and then slowly evolved for use in many other areas in urology, including kidney cancer, bladder cancer and reconstructive surgery. Today most major urologic surgical procedures are being done robotically.
Again, a lot of it is experience, the comfort level of the surgeon, and what we’re trying to accomplish. Going back to your original questionthe stigmathere’s always going to be a stigma of new technologies and new ways of doing things. I think as the surgeons and as the staff get more and more comfortable with these technologies, that’s where the stigma starts to go away. And, in fact, if enough surgeons do it, then it becomes “standard of care.” And so, the standard of care, like I said in 2021, does call for the robotic approach with many procedures.
Treating Prostate Surgery With Urology Specialist
Dr Arianayagam is a highly experienced urologist in Sydney and is an expert in all aspects of prostate surgery, particularly robotic radical prostatectomy.
Dr Arianayagam performs robotic radical prostatectomy at both Macquarie University Hospital and Nepean Public Hospital. Dr Arianayagam has performed over 300 robotic cases. In addition, he is a proctor for Device Technologies, which supply the Da Vinci Robotic System in Australia. Being a proctor means Dr Arianayagam is qualified to teach other surgeons to use this technique.
If you have any questions regarding prostate surgery or would like to book an appointment, please feel free to contact Urology Specialist here.
While youre here, learn some more about how we can help you:
You May Like: What Is The Definition Of Prostate Gland
Minimally Invasive Prostatectomy In San Diego
If your doctor has recommended you have a prostatectomy, its natural to have concerns. Our patients often ask if prostate surgery will affect their bladder control or sexual performance. But you can rest assured knowing prostatectomy is safer and less invasive than ever before and in many cases, it saves lives.
Scripps surgeons perform many prostate surgeries every year. Whenever possible we use the latest minimally invasive techniques, including robotic prostatectomy.
Urological Care At Brigham And Women’s Hospital
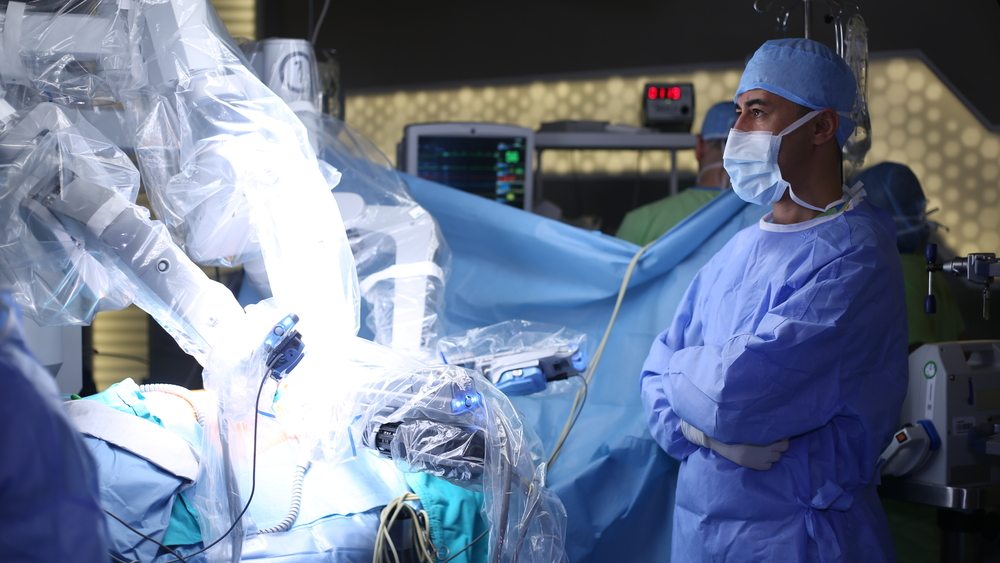
Urology at BWH continues to play a leadership role in developing new therapies for prostate cancer, benign prostate disease, and bladder dysfunction. Members of our clinical staff are all on the faculty of Harvard Medical School and are international leaders in treating prostate, bladder, testicle, and renal cancers and mens sexual dysfunction. Our services include urologic oncology, men’s sexual health, and urodynamics.
Our researchers are international leaders in molecular genetics, image-guided radiotherapy, tumor markers, and surgical robotics.
Much of our staff, under the direction of the Chief of Urology, Adam Kibel, MD, acts as the surgical oncology team for the Genitourinary Cancer Treatment Program at the Dana-Farber/Brigham and Womens Cancer Center. This integrated cancer center in adult oncology brings together genitourinary, radiation, and medical oncologists with urological surgeons to treat patients as one medical team.
Patient- and Family-focused Care
BWH has long been committed to not only the care of our patients but also the many other needs that they and their families have. This philosophy of patient- and family-focused care – involving systems and services that emphasize healing in a comfortable, relaxed environment is a guiding force behind the care we provide at the Department of Urology.
Quality of Patient Care
You May Like: Does Prostatitis Go Away Without Treatment
