What Is Considered An Elevated Psa After Prostatectomy
After radical prostatectomy, the doctors will perform a PSA test in order to determine whether there are some prostate cells left in the body. This usually happens when the disease is advanced at the time of surgery and could have already spread to other parts of the body. It is considered elevated PSA after prostatectomy a PSA greater than 0.2 ng/ml. If the prostate cells are grown enough to generate detectable levels of PSA, this could be an alarming point both for the patient and the doctor.
It is important to note that a level of PSA that is not alarming when first diagnosed with prostate cancer is a reason for concern when being tested after surgery. The reason is that usually, the prostate generates a certain level of PSA. But after being removed, the level of PSA is expected to be zero unless the prostate cells had already spread to other parts of the body.
According to the Prostate Cancer Foundation, about 20-30% of men have PSA recurrence after five years of initial prostate cancer treatment . As a patient, the prospect of PSA recurrence can be very worrisome. What many patients do not know is that not all modified levels of PSA after prostate cancer treatment indicate the same diagnosis. Some types of levels are much more troublesome than others and treatment approaches can vary tremendously case by case. Not all changes in the PSA mean a recurrence of prostate cancer after robotic surgery or other forms of treatment.
Can You Remove The Prostate For Prostate Cancer If You Have Had Radiation Wellyes And No
One of the most common reasons I am given by patients choosing to have their prostate removed is the argument that one can do radiation after surgery but you cant do surgery after radiation. It is a valid argument and I think something to consider in the decision-making process. The concept is, however, not that cut and dried. Here are some caveats.
So, the rationale for choosing surgery because you can do radiation later is a reasonable decision, but not one that will always make a difference in your ultimate outcome. I feel it does make a difference in the situations I mention above, but you really wont know until you have the radiation and over an extended period of time your PSA goes down and never goes up again.
| Salvage Prostatectomy with Bladder Neck Closure, Continent Catheterizable Stoma and Bladder Augmentation: Feasibility and Patient Reported Continence Outcomes at 32 Months |
Open Radical Prostatectomy Vs Minimally Invasive Radical Prostatectomy
In 2003, only 9.2% of radical prostatectomies were done using a minimally invasive procedure. By 2007, that number had jumped to 43.2%. In 2009, researchers in Boston reported on a study that compared outcomes, benefits, and complications of open surgery vs. minimally invasive surgery:
- No difference was found in deaths or in the need for additional cancer therapy between the two approaches.
- The median hospital stay was two days for minimally invasive surgery and three days for open surgery.
- 2.7% of men having laparoscopic surgery required a blood transfusion compared with 20.8% of men having open surgery.
- There was more anastomotic stricture — narrowing of the suture where internal body parts are rejoined — for open surgery than for minimally invasive surgery .
- There were fewer respiratory complications with minimally invasive surgery than with open surgery .
- There were lower rates of incontinence and erectile dysfunction with open surgery. The overall rate was 4.7% for laparoscopic surgery and 2.1% for open surgery.
Read Also: What Happens To The Prostate Later In Life
Are There Differences Between Orp Lrp And Ralrp
According to a 2010 of different surgery types for prostate cancer, the outcomes for open radical prostatectomy , laparoscopic , and robotic-assisted prostatectomy are not significantly different.
But people who choose LRP and RALRP may experience:
- less blood loss
- shorter hospital stay
- faster recovery time
Also, people who choose RALRP report faster recovery in continence and decreased hospital stay, in comparison to LRP. But the overall outcomes still depend on the surgeons experience and skill.
Immediately After A Prostatectomy
- You will stay in hospital for two to five days.
- Nurses will monitor your vital signs.
- Your pain will be managed with medication.
- You may be given antibiotics to reduce the risk of infection.
- You may have a drip inserted into your arm or hand for a few days.
- You will most likely have a drain tube out of your abdomen that will be removed in the first day or two after the surgery.
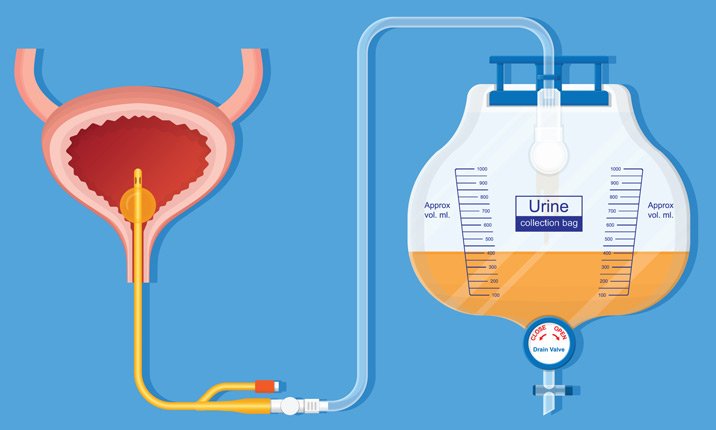
- You will be fitted with a small tube in your penis. The catheter drains urine into an attached bottle or bag. This catheter will be removed about one to three weeks after the operation. Your surgeon will tell you when it can be removed.
- In most cases, you will have to go home still wearing the catheter. You will be taught how to care for it.
Read Also: Urinozinc Prostate Side Effects
Surgery For Prostate Cancer
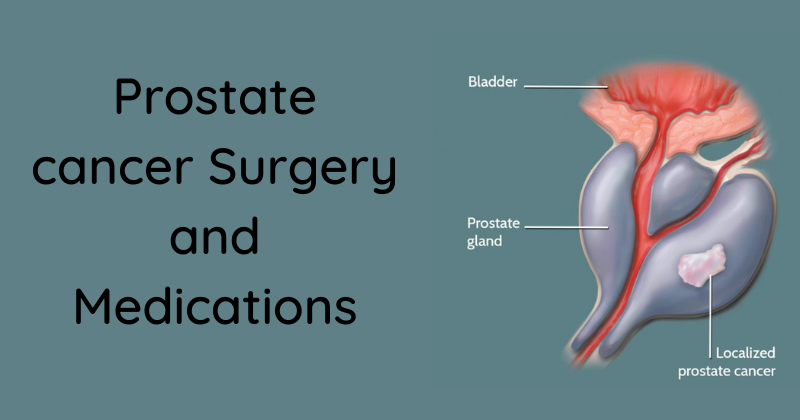
Surgery is a common choice to try to cure prostate cancer if it is not thought to have spread outside the prostate gland.
The main type of surgery for prostate cancer is a radical prostatectomy. In this operation, the surgeon removes the entire prostate gland plus some of the tissue around it, including the seminal vesicles.
Risks Of Prostate Surgery
The risks with any type of radical prostatectomy are much like those of any major surgery. Problems during or shortly after the operation can include:
- Reactions to anesthesia
- Blood clots in the legs or lungs
- Damage to nearby organs
- Infections at the surgery site.
Rarely, part of the intestine might be injured during surgery, which could lead to infections in the abdomen and might require more surgery to fix. Injuries to the intestines are more common with laparoscopic and robotic surgeries than with the open approach.
If lymph nodes are removed, a collection of lymph fluid can form and may need to be drained.
In extremely rare cases, a man can die because of complications of this operation. Your risk depends, in part, on your overall health, your age, and the skill of your surgical team.
You May Like: Can You Give Yourself A Prostate Massage
Types Of Prostate Surgery
There are several ways of removing the prostate keyhole surgery either by hand or robot-assisted, and open surgery.
Although robot-assisted keyhole surgery is the newest technique, the most recent research suggests all three techniques are as good as each other for treating prostate cancer, as long as the surgeon is experienced. They also have similar rates of side effects.
The advantages of keyhole surgery, both by hand and robot-assisted, are that you are likely to lose less blood, have less pain, spend less time in hospital, and heal more quickly than with open surgery.
Keyhole surgery
Keyhole surgery .
- Robot-assisted keyhole surgery Your surgeon makes five or six small cuts in your lower abdomen and a slightly bigger cut near your belly button, and removes the prostate using special surgical tools. These include a thin, lighted tube with a small camera on the tip. The image will appear on a screen so the surgeon can see what theyre doing. Your surgeon controls the tools from a console in the operating room via four or five robotic arms. Although its called robot-assisted, its still a surgeon who does the operation. You may hear the equipment called the da Vinci® Robot.
- Keyhole surgery by hand As with robot-assisted keyhole surgery, the surgeon will make four or five small cuts in your abdomen. But they will hold the surgical tools in their hands, rather than using robotic arms.
Open surgery
Other Possible Side Effects
Anorgasmia is the inability to achieve orgasm regardless of the level of stimulation.
2) Penile shrinkage
Removal of the prostate seems to initiate a phase of penile shrinkage that varies between 2 to 3 cm. For men with large organs, this may have little effect. But a man that starts on the small side might be very dismayed about it.
Early penile rehabilitation may avoid structural endothelial and smooth muscle damage by improving penile oxygenation.
3) Urine leakage or pain during intercourse
4) Urine leakage at orgasm
5) Pain or discomfort at orgasm
You May Like: How Effective Is Chemotherapy For Prostate Cancer
Open Or Laparoscopic Radical Prostatectomy
In the more traditional approach to prostatectomy, called anopen prostatectomy, the surgeon operates through a single long skin incision to remove the prostate and nearby tissues. This type of surgery is done less often than in the past.
In a laparoscopic prostatectomy, the surgeon makes several smaller incisions and uses special long surgical tools to remove the prostate. The surgeon either holds the tools directly, or uses a control panel to precisely move robotic arms that hold the tools. This approach to prostatectomy has become more common in recent years. If done by experienced surgeons, the laparoscopic radical prostatectomy can give results similar to the open approach.
How Soon After Prostate Cancer Treatment Can I Be Sexually Active Again
This will depend on what type of treatment you have had and how you feel. It could be several weeks, for others it may be a lot longer for erections to return. Some men will never be able to keep an erection without the help of artificial methods like medicines or medical devices . If you were having problems having erections before treatment, this will not get better after treatment.
Read Also: What Is Perineural Invasion In Prostate Cancer
Good Prostate Cancer Care
Your MDT will be able to recommend what they feel are the best treatment options, but ultimately the decision is yours.
You should be able to talk with a named specialist nurse about treatment options and possible side effects to help you make a decision.
You should also be told about any clinical trials you may be eligible for.
If you have side effects from treatment, you should be referred to specialist services to help stop or ease these side effects.
What The Research Shows About Radiation Vs Surgery
The ProtecT trial was a 10-year, randomized clinical study designed to compare radical prostatectomy, external-beam radiotherapy and active surveillance for the treatment of localized prostate cancer.
The results, published in 2016, showed that the rate of disease progression among men assigned to radiotherapy or radical prostatectomy was less than half the rate among men assigned to active monitoring. However, there was no significant difference in survival at the median 10-year mark for radiation therapy, surgery or active surveillance.
If youre interested in directly comparing treatment outcomes by treatment method and risk group , the Prostate Cancer Free Foundation provides an interactive graph on its website with information from data obtained from over 100,000 prostate cancer patients over a 15-year period.
As discussed earlier in the sections on the side effects of radiation therapy and surgery, the researchers conducting the ProtecT trial also looked at side effects and quality-of-life issues and found that the three major side effects of these two treatment options that affect quality of life after prostate cancer treatment are urinary incontinence, sexual dysfunction and bowel health.
The trial found that urinary leakage and erectile dysfunction were more common after surgery than after radiation therapy. Gastrointestinal bowel problems were more common after radiation therapy.
Recommended Reading: Cialis For Bph Dosage
Read Also: Flomax For Prostatitis
Radical Prostatectomy Perineal Approach
You’ll be placed in a supine position in which the hips and knees will be fully bent with the legs spread apart and elevated with the feet resting on straps. Stirrups will be placed under your legs for support.
An upside-down, U-shaped incision will be made in the perineal area .
The doctor will try to minimize any trauma to the nerve bundles in the prostate area.
The prostate gland and any abnormal-looking tissue in the surrounding area will be removed.
The seminal vesicles may be removed if there’s concern about abnormal tissue in the vesicles.
Your Cancer Care Team
People with cancer should be cared for by a multidisciplinary team . This is a team of specialists who work together to provide the best care and treatment.
The team often consists of specialist cancer surgeons, oncologists , radiologists, pathologists, radiographers and specialist nurses.
Other members may include physiotherapists, dietitians and occupational therapists. You may also have access to clinical psychology support.
When deciding what treatment is best for you, your doctors will consider:
- the type and size of the cancer
- what grade it is
- whether the cancer has spread to other parts of your body
Don’t Miss: Zinc Prostate Cancer
How Fast Will I Become Totally Continent After Prostate Surgery
During surgery for prostate cancer, the urethra is also affected and, depending on the experience of the surgeon, more or less of the continence function will be preserved. Due to the high precision of robotic surgery, the patient will have a catheter for roughly one week and the trauma to the urinary function will be minimum.
The discomfort that patients feel during this time is minimum, but you should expect the removal to make you feel uneasy. The catheter will be removed during a visit to your doctor, so do not try to do this at home, as it could cause infections. The degree of which the urinary function will be affected depends on how normal the function was before surgery, age and weight.
It is worth noting that most men will experience some degree of incontinence after prostate surgery, but control can be regained within several weeks or months to a year.
Read Also: Prognosis Of Prostate Cancer With Bone Metastases
Staging Of Prostate Cancer
Doctors will use the results of your prostate examination, biopsy and scans to identify the “stage” of your prostate cancer .
The stage of the cancer will determine which types of treatments will be necessary.
If prostate cancer is diagnosed at an early stage, the chances of survival are generally good.
Don’t Miss: Find Prostate Externally
How To Return To An Active Sex Life After Prostate Cancer Treatment
No matter the cancer, treatments often cause side effects that affect patients quality of life. But with prostate cancer, the potential side effects can be particularly concerning to men who are trying to decide which approach is right for them. Surgery, radiation therapy and other treatments may impact a patients sex life, causing challenges like low sex drive, loss of penis length, dry orgasm or low sperm counts. Despite the angst these issues may cause, experts say most of these side effects can be managed and many men have a good chance of returning to a full sex life after prostate cancer treatment.
Unfortunately, sexual dysfunction is a possibility for nearly all treatment options for prostate cancer, including surgery, says Scott Shelfo, MD, FACS, Medical Director of Urology at our hospital near Atlanta. The degree of dysfunction depends on many factors, including the patients overall health, co-existing medical problems, as well as the patients level of sexual function and ability before treatment.
Treating Advanced Prostate Cancer
If the cancer has reached an advanced stage, it’s no longer possible to cure it. But it may be possible to slow its progression, prolong your life and relieve symptoms.
Treatment options include:
- hormone treatment
- chemotherapy
If the cancer has spread to your bones, medicines called bisphosphonates may be used. Bisphosphonates help reduce bone pain and bone loss.
Don’t Miss: How Effective Is Chemotherapy For Prostate Cancer
Prostatectomy And Sexual Issues
As a man, your prostate gland plays several important roles in your bodys sexual and urinary function.
During sex, your prostate gland is responsible for releasing seminal fluid, or semen, into your urethra. As you reach orgasm and ejaculate, the muscle tissue of your prostate forces semen and sperm out from your penis.
The nerves that surround your prostate also play an important role in allowing blood to flow to the erectile tissue of your penis when youre sexually aroused.
Because prostate surgery involves removing the prostate gland, its normal to lose some parts of your normal sexual function after the surgery.
For example, radical prostatectomy involves cutting the connection between your urethra and your testicles. This means that sperm is no longer able to flow down your urethra and out the tip of your penis during sex.
As a result of this, men who undergo radical prostatectomy surgery can still reach orgasm, but arent able to ejaculate.
Several different approaches are used to remove your prostate gland during surgery. Some of these approaches particularly those used to treat prostate cancer may result in damage to the nerves that surround your prostate gland, testicles and penis.
Nerve damage caused by prostatectomy surgery may affect your erectile health. If your nerves need to be cut during the procedure , you may find it difficult or impossible to get and/or maintain an erection after surgery.
Questions You May Want To Consider Asking Your Doctor Include:
- What type of prostate problem do I have?
- Is more testing needed and what will it tell me?
- If I decide on watchful waiting, what changes in my symptoms should I look for and how often should I be tested?
- What type of treatment do you recommend for my prostate problem?
- For men like me, has this treatment worked?
- How soon would I need to start treatment and how long would it last?
- Do I need medicine and how long would I need to take it before seeing improvement in my symptoms?
- What are the side effects of the medicine?
- Are there other medicines that could interfere with this medication?
- If I need surgery, what are the benefits and risks?
- Would I have any side effects from surgery that could affect my quality of life?
- Are these side effects temporary or permanent?
- How long is recovery time after surgery?
- Will I be able to fully return to normal?
- How will this affect my sex life?
- How often should I visit the doctor to monitor my condition?
Related Resources
Also Check: Does Enlarged Prostate Affect Ejaculation
