What Is The Life Expectancy After The Removal Of The Prostate Gland
Prostate removal prolongs life with about three years in men with prostate cancer. However, prognosis depends on many factors. A doctor should know the patients medical history in detail and put this information together with survival statistics in order to offer an informed answer.
Option treatments have evolved over the years and life after prostate removal is now associated with less complications and a higher success rate.
Should I Poop Before A Prostate Exam
You dont need to change any bathroom habits prior to your appointment. If you feel like you need to poop before your exam, then its fine to do so. But dont worry if you just dont have the urge. The prostate exam shouldnt make you feel like you need to go.
Theres no need to be embarrassed about fecal matter during your prostate exam. Your healthcare provider is experienced in performing this exam and will do everything to ensure your comfort during the process.
How Fast Will I Become Totally Continent After Prostate Surgery
During surgery for prostate cancer, the urethra is also affected and, depending on the experience of the surgeon, more or less of the continence function will be preserved. Due to the high precision of robotic surgery, the patient will have a catheter for roughly one week and the trauma to the urinary function will be minimum.
The discomfort that patients feel during this time is minimum, but you should expect the removal to make you feel uneasy. The catheter will be removed during a visit to your doctor, so do not try to do this at home, as it could cause infections. The degree of which the urinary function will be affected depends on how normal the function was before surgery, age and weight.
It is worth noting that most men will experience some degree of incontinence after prostate surgery, but control can be regained within several weeks or months to a year.
Don’t Miss: How Does Prostate Cancer Affect You Sexually
Minimally Invasive Procedures For Bph
Minimally invasive surgical therapies for BPH, such as free-beam laser therapy, radiofrequency ablation, transurethral needle ablation, prostatic urethral stents , and alcohol injection, are relatively simple procedures that can usually be performed in an outpatient setting, often with decreased postoperative catheterization time.
For patients at very high medical risk who cannot safely undergo significant anesthesia or surgery, these minimally invasive treatments may offer some benefit. Prostatic urethral stents, for example, have been suggested as a reasonable BPH treatment alternative when medical therapy has failed and the medical risks of surgery are unacceptably high. Stent migration, dysuria, and pain are relatively common complications but are easily reversible with stent removal.
These minimally invasive methods do not allow tissue to be saved for pathological analysis and do not remove the entire adenomatous prostate thus, retreatment and even TURP is sometimes required later. Up to 25% of patients who receive these minimally invasive treatment alternatives ultimately undergo a TURP within 2 years.
Prior to surgical intervention for LUTS attributed to BPH, clinicians should do the following:
- Consider assessment of prostate size and shape via abdominal or transrectal ultrasound, cystoscopy, or by preexisting cross-sectional imaging
- Assess post-void residual
- Consider pressure flow studies when diagnostic uncertainty exists
Surgical Therapy
Simple prostatectomy:
Side Effects Of Prostate Surgery
The major possible side effects of radical prostatectomy are urinary incontinence and erectile dysfunction . These side effects can also occur with other forms of prostate cancer treatment.
Urinary incontinence: You may not be able to control your urine or you may have leakage or dribbling. Being incontinent can affect you not only physically but emotionally and socially as well. These are the major types of incontinence:
- Men with stress incontinence might leak urine when they cough, laugh, sneeze, or exercise. Stress incontinence is the most common type after prostate surgery. Its usually caused by problems with the valve that keeps urine in the bladder . Prostate cancer treatments can damage this valve or the nerves that keep the valve working.
- Men with overflow incontinence have trouble emptying their bladder. They take a long time to urinate and have a dribbling stream with little force. Overflow incontinence is usually caused by blockage or narrowing of the bladder outlet by scar tissue.
- Men with urge incontinencehave a sudden need to urinate. This happens when the bladder becomes too sensitive to stretching as it fills with urine.
- Rarely after surgery, men lose all ability to control their urine. This is called continuous incontinence.
After surgery for prostate cancer, normal bladder control usually returns within several weeks or months. This recovery usually occurs slowly over time.
There are several options for treating erectile dysfunction:
Don’t Miss: What Causes Prostate To Swell
What Are The Limitations Of Prostate Ultrasound Imaging
Men who have had the tail end of their bowel removed during prior surgery are not good candidates for ultrasound of the prostate gland because this type of ultrasound typically requires placing a probe into the rectum. However, the radiologist may attempt to examine the prostate gland by placing a regular ultrasound imaging probe on the perineal skin of the patient, between the legs and behind the scrotum of the patient. Sometimes the gland can be examined by ultrasound this way, but the images may not be as detailed as with the transrectal probe. An MRI of the pelvis may be obtained as an alternative imaging test, because it may be obtained with an external receiver coil.
Read Also: What Causes Your Prostate To Enlarge
Less Common Side Effects Of Turp
Less common unwanted effects of surgery include:
- urinary symptoms do not change sometimes surgery does not cure your urinary problems. Even though the blockage has been cleared, the bladder irritability may continue and you may still have symptoms such as being unable to empty your bladder completely, and nocturia
- erectile dysfunction some men are unable to get or maintain an erection sufficient for sexual intercourse after surgery. This is more of a problem for men who had erectile difficulties before their operation. This problem may be treated by medication
- urethral strictures when scarring occurs in and around the urinary tract, it can cause further blockage to urine flow. Strictures may need to be dilated or need further surgery
- urinary incontinence sometimes surgery results in being unable to hold or control the flow of urine. This may be due to continuing bladder problems or, less often, to sphincter muscle damage
Recommended Reading: Is Zinc Bad For The Prostate
Open Or Laparoscopic Radical Prostatectomy
In the more traditional approach to prostatectomy, called anopen prostatectomy, the surgeon operates through a single long skin incision to remove the prostate and nearby tissues. This type of surgery is done less often than in the past.
In a laparoscopic prostatectomy, the surgeon makes several smaller incisions and uses special long surgical tools to remove the prostate. The surgeon either holds the tools directly, or uses a control panel to precisely move robotic arms that hold the tools. This approach to prostatectomy has become more common in recent years. If done by experienced surgeons, the laparoscopic radical prostatectomy can give results similar to the open approach.
Why Is A Simple Prostatectomy Performed
There are varying degrees of prostate enlargement.
If your prostate grows only slightly, many minimally-invasive surgeries can remove part of the gland, such as transurethral resection of the prostate .
However, if your prostate becomes very large , your surgeon will need to perform a simple prostatectomy. This involves removing the inner core of your prostate gland. Most men who undergo this type of surgery are age 60 or older.
Special diets, changes in drinking habits, and medications are often tried before surgery is recommended.
Your doctor may recommend a simple prostatectomy if your prostate is very large and you are suffering from:
- extremely slow urination
Recommended Reading: Can Prostate Cancer Metastasis To Lungs
Preparation For Prostatectomy Surgery
During the weeks before the surgery, patients should stop taking anything that prevents blood clotting, including aspirin, ibuprofen, warfarin, vitamin E, and fish oil. Ideally, they should also stop smoking several weeks before surgery so as to help speed recovery.
Patients may also be asked to take a laxative or use an enema on the morning of the surgery to clean out their colon. In addition, the doctor may administer an antibiotic to prevent infection.
Surgery To Treat Problems Passing Urine
Prostate cancer can press on the tube that carries urine from the bladder. This can make it difficult for you to empty your bladder. Your doctor might suggest that you have an operation to remove some of the cancer so that you can pass urine more easily. This is called trans urethral resection of the prostate .
This operation is more common in men with a non cancerous swelling of the prostate. This is called benign prostatic hypertrophy .
Surgeons can also use laser surgery to remove the prostate tissue. It works just as well as a TURP, but isn’t available in every hospital.
You May Like: What Is Better For Prostate Cancer Surgery Or Radiation
Questions To Ask The Doctor
- Why is an open prostatectomy recommended?
- What form of open prostatectomyretropubic or suprapubicwill be used?
- What forms of anesthesia and pain relief will be given?
- Where will the incision be located?
- What are the risks of the procedure?
- Is the surgeon a board certified urologist?
- Is there an alternative to open prostatectomy?
- What are the chances of after effects, including erectile problems?
Why Is Radical Prostatectomy Done
Radical prostatectomy is a treatment for prostate cancer that prevents cancer from spreading outside the prostate gland. It may cure prostate cancer by removing it completely.
For patients diagnosed with prostate cancer, additional tests may be needed to determine the how far the cancer has spread. These tests help your provider decide if you are a candidate for radical prostatectomy:
Also Check: Prostate Cancer Seeds Vs Surgery
Also Check: Will Every Man Get Prostate Cancer
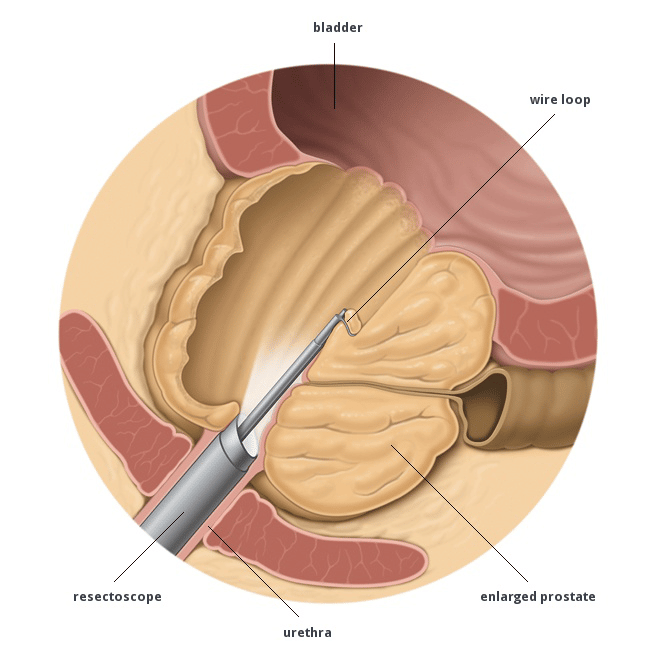
What Happens During Surgery
The aim of surgery is to make the prostate gland smaller so that it no longer pushes against the bladder and urethra. In most of the approaches, tiny instruments are guided through the urethra until they reach the prostate, where they are used to remove tissue or widen the urethra. This kind of procedure is known as keyhole surgery. If the prostate gland is very large, it may be operated on from the outside, through a cut in the abdominal wall . This is rarely necessary, though.
Many different surgical techniques and many different instruments and devices can be used to remove prostate tissue in different ways.
How Does The Procedure Work
After anesthesia, a surgeon will insert a tool called a resectoscope into the urethra. In some cases, a separate device will be used to flush sterile fluid through the surgical site.
Once the surgeon has positioned the resectoscope, they will use it to cut away abnormal prostate tissues and seal broken blood vessels.
Finally, the surgeon will insert a long plastic tube called a catheter into the urethra and flush destroyed prostate tissues into the bladder where they are excreted through urine.
Read Also: How To Shrink Your Prostate
What Is A Prostate Exam
A prostate exam is a screening method used to look for early signs of prostate cancer. In general, a prostate exam includes a PSA blood test and a digital rectal exam .
During the digital rectal exam portion, your healthcare provider carefully inserts their gloved finger into your rectum. This allows them to feel the edges and surface of your prostate gland to detect any potential abnormalities.
What To Expect After Surgery
Following surgery, most men spend one to two days in the hospital. Patients typically receive intravenous pain medication during their first day after surgery , then transition to oral pain medications by the second day. Once pain is under control and bowel function has begun to return, the patient is ready for discharge.
Also Check: What Does The Prostate Look Like After Radiation
Reducing Your Risk Of Complications
You can help reduce the chance of certain complications by:
- following activity, dietary, and lifestyle restrictions and recommendations before surgery and during recovery
- notifying your doctor immediately of any concerns, such as bleeding, bloody urine, fever, an increase in pain, or a change in urination
- seeing your doctor as instructed before and after surgery
- taking your medications exactly as directed
- telling all members of your care team if you have any allergies
Other Forms Of Treatment For Benign Prostate Disease
Other forms of treatment may include:
- monitor symptoms the condition is monitored closely. Treatment only begins once the condition has progressed and is causing problems
- medical treatment symptoms of benign enlargement can be treated by medications that relax the muscles around the bladder or that shrink the prostate and delay the need for surgery.
Also Check: Types Of Advanced Prostate Cancer
How Do I Prepare For A Simple Prostatectomy
Your doctor will do a thorough check of your health. If you have health conditions such as diabetes, heart disease, lung problems, or high blood pressure, they need to be under control before surgery. If youre in poor health and cant undergo anesthesia or surgery, a simple prostatectomy is probably not your best option.
Your doctor will order many tests and scans before your surgery to learn as much as possible about your condition. These will likely include:
- blood tests to check for other health conditions
- an ultrasound to get images of your prostate gland and nearby organs
- a biopsy of the prostate, to obtain a small sample for analysis
- a CT scan or MRI of your abdomen and pelvis
Be sure to tell your doctor if you take any drugs or vitamins, especially any medicines that thin your blood. Blood-thinning medications can cause complications and excessive bleeding during surgery. Examples of these drugs and vitamins include:
- newer blood thinners, such as eliquis, pradaxa, and xarelto
Do not eat or drink after midnight on the night before surgery. This will ensure you avoid complications with the anesthesia. You may need to drink only clear liquids and take a laxative the day before surgery to clear your digestive system.
What Happens During Turp
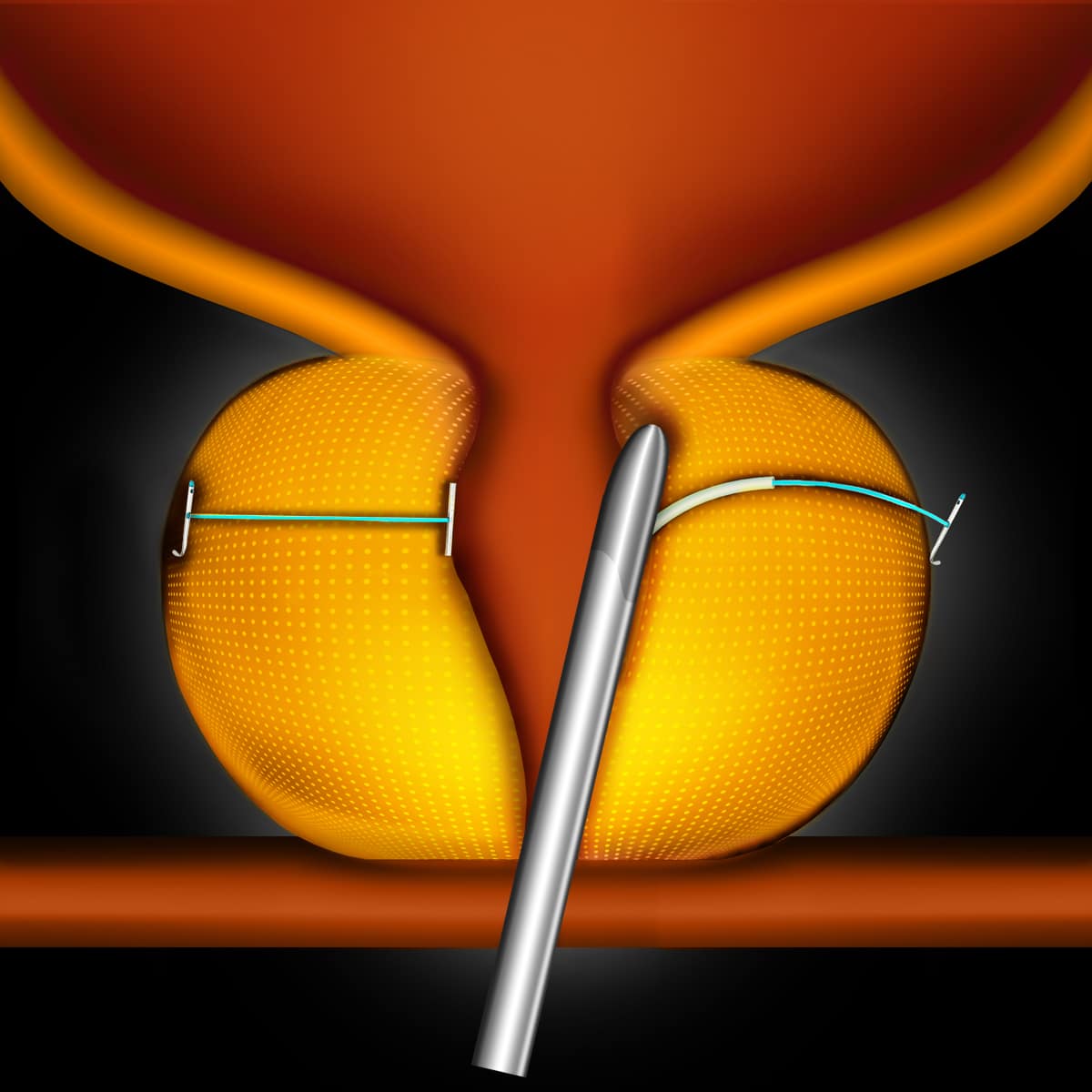
TURP requires a hospital stay. Procedures may vary depending on yourcondition and your healthcare providers practices.
Generally, a TURP follows this process:
Recommended Reading: New Prostate Cancer Treatment 2021
Prostate Size And Blockage Of The Urethra
If the inner part of the prostate gland obstructs the urethra during urination, this will irritate the bladder and cause urinary symptoms.Urinary symptoms may include:
- frequent urination, particularly at night
- urgency and possible urgency incontinence
- passing drops of urine involuntarily after you think you’ve finished
- blood in the urine although this can never be assumed to be due to the prostate until other causes have been excluded.
The actual size of the prostate does not appear to determine whether or not there is a blockage. Some men with large prostates never develop obstruction, but some men with small prostates can have severe bladder obstruction, which causes difficulty with urinating.Around one in three Victorian men over the age of 50 years have some urinary symptoms. In most cases, these symptoms are due to a blockage caused by an enlarged prostate, but they may be due to other causes.
How Do These Surgical Options Compare
| Prostate Artery Embolization | |
| Risks | |
|
|
|
|
|
|
|
|
Don’t Miss: When Should You Have A Prostate Exam Uk
Questions To Ask Before Surgery
As you think over the options for surgery, ask your doctor these questions:
- Is there a good chance my condition will get better?
- How much will it improve?
- What are the chances of side effects from a treatment?
- How long will the effects last?
- Will I need to have this treatment repeated?
With newer technologies, doctors can do some minimally invasive procedures with tiny cuts or use tube-style instruments that they insert into you. These procedures may not treat the symptoms to the same degree or durability as more invasive surgical options, they do have faster recoveries, less pain afterward and have reduced risks.
Other times, the traditional and more invasive surgery may be needed. It all depends on your case and what you and your doctor decide is best for you.
Doctors can choose from these minimally invasive procedures, endoscopic, or open surgeries to treat moderate to severe symptoms. These procedures are also used if tests show that your ability to pee is seriously affected.
