Question 1 Of : What Does Prostate Pain Feel Like
Recommended Reading: Zinc Prostate
What Is The Prostate
The prostate is a walnut-shaped gland that is part of the male reproductive system. The main function of the prostate is to make a fluid that goes into semen. Prostate fluid is essential for a mans fertility. The gland surrounds the urethra at the neck of the bladder. The bladder neck is the area where the urethra joins the bladder. The bladder and urethra are parts of the lower urinary tract. The prostate has two or more lobes, or sections, enclosed by an outer layer of tissue, and it is in front of the rectum, just below the bladder. The urethra is the tube that carries urine from the bladder to the outside of the body. In men, the urethra also carries semen out through the penis.
The Revival Of Fosfomycin
Considering that the evolving changes in resistance rates for fluoroquinolones have a serious impact on treatment, alternative antibiotic therapies are urgently needed. Studies have demonstrated fosfomycin has a strong killing effect in vitro against antimicrobial-resistant E. coli . This new discovery inspires the treatment of refractory bacterial prostatitis . Fosfomycin, an old drug used before for therapy of females uncomplicated cystitis and transrectal prostate biopsy prophylaxis, has been recently rediscovered as a treatment for MDR infections with an effective rate > 90% in lowering UTIs . In addition, fosfomycin-susceptibility rate of ESBL-producing E. coli, ESBL-producing K. pneumoniae, and E. faecalis reported lately by a systemic review was 95%, 83.8%, and 96.8%, respectively . Clinically, a case report of the successful administration of oral fosfomycin on patients with CBP who were infected by a complicated vancomycin-resistant Enterococci demonstrated that fosfomycin is available .
Recommended Reading: Super Beta Prostate Advanced Side Effects
You Have A Yeast Infection
Your painful peeing experience might be the product of a yeast infection. In people AFAB, a yeast infection occurs when the natural balance of microorganisms in the vagina are disrupted, leading to an overgrowth of fungus, according to the Mayo Clinic.
“Vaginal infections like yeast can cause the vagina to become swollen and inflamed, making the area very sensitive,” Dr. Horton says. In people AFAB, the urethra is located just above the vagina, and when you pee, the urine may encounter the irritated skin of the vagina and cause burning, she explains.
Other symptoms of a vaginal yeast infection involve, per the Mayo Clinic:
- Itching and irritation in the vagina and vulva
- Redness and swelling of the vulva
- Vaginal pain and soreness
- Thick, white, odor-free vaginal discharge with a cottage cheeseappearance
- Watery vaginal discharge
People AMAB may also get yeast infections, which can cause the head of the penis to become inflamed, a condition known as balanitis, according to the Mayo Clinic. Redness, scaling and a painful rash may also occur in penile yeast infections, per Johns Hopkins Medicine.
Fix it: Most yeast infections are treatable with antifungal topical creams and gels , Dr. Horton says. But if over-the-counter options don’t relieve your symptoms, you should see your doctor right away.
How Do Doctors Diagnose A Prostate Infection
The diagnosis of both acute and chronic prostate infections begins with the history of the symptoms described above, the physical exam, including the digital exam of the prostate and often confirmed by culture and identification of the infecting organism.
Acute bacterial prostatitis diagnosis
- Usually an enlarged, firm, and tender prostate is enough to make a presumptive diagnosis and start treatment .
- Because there is usually a low level of bacteria in urine, the doctor will perform a urinalysis to quantitate and identify infecting bacteria by urine culture.
- If the person has symptoms suggesting the infection has spread outside the prostate , blood cultures and other blood tests are likely to be ordered.
- If a spread of the infection is suspected, a doctor will often perform an ultrasound to help confirm the diagnosis and to rule out an abscess. If this ultrasound is not available, the doctor may perform a CT scan or MRI of the pelvis.
Chronic bacterial prostatitis diagnosis
One of two tests are sometimes performed to help with the diagnosis:
The classic test is a Meares-Stamey 3-glass test. Three separate urine samples are collected and examined during this test. The last sample is taken after prostatic massage.
Premassage and postmassage test
Men with recurrent urinary tract infections should have ultrasound imaging of their upper urinary tract and a plain abdominal X-ray or an intravenous urography to exclude a possible structural problem or a kidney stone.
Also Check: Ejaculation Problems With Tamsulosin
You Have Bacterial Vaginosis
Bacterial vaginosis a kind of vaginal inflammation caused by an overgrowth of bacteria in the vagina could be the source of your stinging pee.
In addition to burning during urination, you may also experience itching, a gray, frothy discharge and a foul or fishy odor when you have bacterial vaginosis, Dr. Horton says.
Fix it: See your doctor, who can prescribe oral antibiotics or a vaginal suppository, Dr. Horton says.
If you have recurrent bouts of BV, try taking over-the-counter boric acid capsules and suppositories, which can help restore a normal vaginal pH, Dr. Horton says. “Taking probiotics daily can also prevent vaginal infections like yeast and bacterial vaginosis,” she adds.
Nih Classification And Definition Of Prostatitis
The National Institutes of Health classification and definition of the categories of prostatitis are as follows:
-
Category I Acute bacterial prostatitis
-
Category II Chronic bacterial prostatitis
-
Category III Chronic abacterial prostatitis/chronic pelvic pain syndrome
-
Category IIIA Inflammatory chronic pelvic pain syndrome
-
Category IIIB Noninflammatory chronic pelvic pain syndrome
-
Category IV Asymptomatic inflammatory prostatitis
You May Like: Does Retrograde Ejaculation Go Away
Classic Drug Choice For Complicated Abp
An acutely ill patient with a clinical picture of sepsis or a systemic inflammatory response syndrome must be accepted for hospitalization with parenteral antibiotics that broadly cover fluoroquinolone plus an aminoglycoside or a combination of the above with a penicillin or second/third-generation cephalosporin . Once the clinical condition of the patient is stable without fever and urinary retention, oral antibiotic therapy should replace intravenous medication for 2â4 weeks, based on the results of blood and urine culture and drug sensitivity. It is necessary to plan repeat urine culture during and 1 week after therapy to ensure bacterial eradication.
Sexually active men younger than 35 years old and men older than 35 years old with high-risk sexual behavior suspected of N. gonorrhoeae and C. trachomatis infection should receive a standard treatment with cephalosporins and azithromycin or doxycycline, respectively . The treatment of ABP associated with genitourinary tuberculosis is recommended by the WHO with 2 months of daily isoniazid, rifampicin, and pyrazinamide with or without ethambutol or streptomycin and immediately followed by four months of treatment with isoniazid and rifampicin two or three times a week. For complicated cases of genitourinary tuberculosis with HIV or AIDS, antituberculosis therapy should be extended to 9â12 months . In addition, treatment for HIV patients is based on initiation of highly active antiretroviral therapy to restore immunity .
The Shift In Bacterial Etiology
As early as 2003, Bundrick et al, have described that E. faecalis and E. coli were the most common isolates the former was the major infection among cohorts of patients with CBP . An epidemiological investigation of the uropathogens among 6221 Italian patients with CBP from January 1997 to December 2008, showed that incidence of gram-positive was higher than gram-negative bacteria, and E. faecalis prevalence increased within 2006â2008 . Moreover, E. faecalis prevalence has also been reported in North America not just to Italy. Recently, a clinical and microbiological survey of 332 cases of CBP showed that E. faecalis was the main etiologic agent , followed by E. coli among patients diagnosed microbiologically with CBP . These results indicate that the predominant etiologic determinant of CBP is gradually transferring to E. faecalis, which belongs to gram-positive microorganisms. Wagenlehner indicated that the improved clinical use of fluoroquinolones for CBP patients increased the trend of gram-positive infections .
The evaluation of microbiological characteristic for each CBP patients to perform a correct, appropriate, and personalized treatment schedule is essential . Therefore, Magri, V et al. proposed to dismiss empirical therapy to avoid catastrophic consequences in terms of chemoresistance and poor clinical practice .
Don’t Miss: Urinozinc Prostate Plus
Treatment Options For Bph
BPH is treated with medications that shrink the prostate and reduce urinary symptoms.
Drugs called 5-alpha-reductase inhibitors block conversion of testosterone to a substance that contributes to the benign prostate growth, called dihydrotestosterone . These drugs include dutasteride and finasteride .
Drugs called alpha-blockers can help relax the prostate and bladder neck, and improve urine flow. These drugs include doxazosin , tamsulosin , and terazosin .
Your doctor may prescribe one of these drugs or a combination of them.
If medications dont help or your symptoms are severe, your urologist may recommend a less invasive procedure to destroy the extra prostate tissue and widen the urethra within the prostate. The procedure may use one of the following:
- heat with radiofrequency ablation
- high-intensity ultrasound waves
- electric current vaporization
Surgery is a longer-term solution. During BPH surgery, the doctor uses a cutting wire loop or laser to cut away the excess prostate tissue.
Donât Miss: What Percentage Of Prostate Nodules Are Cancerous
The Possible Treatment Options
The treatment you get will vary based on the type of prostatitis you have. The ideal management strategy depends on how severe the infections risk factors and symptoms are, including whether the patient has resistance to local antibiotic therapy.
Every patient responds differently to prostatitis treatment. So, if one option doesnt work, the doctor will recommend that you try another. Each treatment opportunity will focus on various stressors that will ease the symptoms. Treatment for bacterial prostatitis relies on:
You May Like: Female Prostate Equivalent
What Is The Prostate Gland What Does It Look Like
The prostate gland is part of the male reproductive system, and it is a walnut-sized gland found in men that is located below the bladder and in front of the rectum. It surrounds the urethra, the tube through which urine and semen exit the body. Its main function is to produce seminal fluid in order to transport sperm through the urethra.
When To Seek Medical Care For Prostate Infections

Contact a doctor for any of the following symptoms. These symptoms are even more significant if accompanied with high fever and chills:
- Urinary burning or pain
- Difficulty or pain when starting urination
- Pain in the genital area
- Pain with ejaculation
Doctors usually diagnose and treat prostate infections on an outpatient basis. If a person develops high fever with chills or a new onset of difficulty in urinating, seek medical care immediately or go to a hospitalâs emergency department because the infection may be spreading to other areas of the body.
Also Check: External Prostate Massage Prostatitis
Chronic Pelvic Pain Syndrome
CPPS is the most common type of prostatitis around 19 out of every 20 men with prostatitis have it. You might also hear it called chronic non-bacterial prostatitis, chronic abacterial prostatitis or prostate pain syndrome. Chronic means long-lasting.
Men with CPPS usually have symptoms for three months or longer. Even after treatment, you may still have prostatitis for a long time. It might come and go, causing occasional episodes of severe pain, sometimes known as flare-ups.
What causes it?
Nobody knows for certain what causes CPPS. Unlike other types of prostatitis it isnt usually caused by a bacterial infection. There could be a number of causes, which makes it difficult to diagnose and treat.
There are also a number of things that might trigger it, including:
- urine getting into the prostate
- previous infections in or around the prostate
- an infection that doesnt show up in tests
- problems with nerves, so that they send pain signals to the brain even when theres nothing physically wrong
- stress, anxiety or depression
- problems with the pelvic floor muscles .
Some research shows a link between stress, anxiety and depression and CPPS. But this doesnt mean that CPPS is all in your head. If youre feeling stressed or depressed, this may cause physical symptoms that trigger CPPS, or make symptoms worse.
Bacterial Prostatitis Starting With The Basics
Bacterial prostatitis is the result of a bacteria thats infecting the prostate. The bacteria may reach the prostate if the urine carrying the infection is flowing backward from the urethra. An ongoing prostate irritation resulting from bacteria is referred to as chronic nonbacterial prostatitis.
Chronic prostatitis can persist for 3 months or for an extended time. While acute prostatitis has a relatively quick onset. But, bacterial prostatitis is not something that can be transmitted to a sexual partner. Instead, it remains inside the prostate fluid and urine.
Also Check: Chemo Pill For Prostate Cancer
How I Cured My Prostatitis
If we go deeper into the definition of prostatitis, we find that inflammation is a protective response of body tissues to toxic stimuli such as pathogens, injured cells, or any other organic or non-organic irritants. Inflammation involves a variety of defense mechanisms such as the local or general rise of body temperature, immune response, and molecular mediators to localize the injured site and ultimately restore the tissue functionality.
Not surprising that our prostate contacting to the bladder and urethra carrying liquid wastes from one side and the colon carrying fecal wastes from another side, exposed to the influence of these irritants throughout the mens life. Even if we do not know the mechanism of prostatitis, we can assume the right causes of prostate inflammation leading to the symptoms mentioned earlier. In this regard, our lifestyle, what we eat, and what we drink or smoke play a primary role in the development of inflammatory processes in the prostate.
On this basis, and bearing in mind the fact that the exact mechanism of prostatitis has not yet been found, any treatment to reduce symptom hardness should be focused on total or, at least, partial removal of inflammation. I wont analyze the pros and cons of available approaches in this post, but their low or medium efficacy and a vast number of side effects make you wonder whether to apply them or not.
The recipe for inflamed prostate treatment.
Pharmacological Interventions For Bacterial Prostatitis
- 1Department of Urology, The First Affiliated Hospital of Nanchang University, Nanchang, China
- 2Jiangxi Institute of Urology, Nanchang, China
Prostatitis is a common urinary tract condition but bring innumerable trouble to clinicians in treatment, as well as great financial burden to patients and the society. Bacterial prostatitis accounting for approximately 20% among all prostatitis have made the urological clinics complain about the genital and urinary systems all over the world. The international challenges of antibacterial treatment and the transformation of therapeutic strategy for classic therapy have attracted worldwide attention. To the best of our knowledge currently, there is not a single comprehensive review, which can completely elaborate these important topics and the corresponding treatment strategy in an effective way. This review summarizes the general treatment choices for bacterial prostatitis also provides the alternative pharmacological therapies for those patients resistant or intolerant to general treatment.
You May Like: Can Zytiga Cure Prostate Cancer
How Do You Treat Prostatitis
There are many different methods for treating prostatitis. Generally, there is no best cure because the conditions of individuals are different. Its up to you, the patient, to decide what works best for you. Patients usually have to suffer from the annoying symptoms of prostatitis for years before they can get a radical cure. Some patients with chronic prostatitis may even live with it for decades. How do you treat prostatitis? Is you method efficient in prostatitis?
In USA, patients with prostatitis are usually prescribed antibiotics by their doctors for this medicine have the properties of antibiosis and anti-inflammation. Its effective on prostatitis that is caused by bacteria. That is to say, its useless for patients with non-bacterial prostatitis. This is a reason why many non-bacterial prostatitis cant have be cured completely. Moreover, the causes of non-bacterial prostatitis are not exactly clear is another reason for the difficulty in treating.
Sometimes doctors will recommend surgery or other high tech methods to heal prostatitis. However, the track record of these methods in prostatitis is poor, because the pain often persists and it will increase the risk of a new infection.
- Shop 1-3, Nan Hu Xin Cheng, Wenchang Road, Hongshan District, Wuhan, Hubei Province, China
Q& A
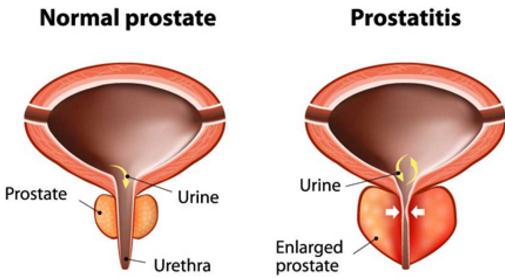
How Does An Enlarged Prostate Affect The Bladder
As the prostate begins to swell it can start to affect different parts of the urinary system. It can begin to tighten around the urethra, making it harder for urine to flow through the narrow tube. It can also start to press on the underside of the bladder and can even reduce the amount of space available in the bladder.
Due to the narrowing of the urethra, some of the common symptoms of an enlarged prostate include a difficulty starting urination, and a weak stream or poor flow when you do start. You may also find that your bladder doesnt quite feel empty afterwards. In serious cases, the urethra can become completely blocked, causing urinary retention.
As a result of the prostate pushing on the bladder, youll probably also find that you need to urinate more often, and that the urge to urinate can come quickly and suddenly.
Don’t Miss: Is Cranberry Juice Good For The Prostate
