What Are The Leading Risk Factors Of Prostate Cancer
While the word cancer instills fear in most, prostate cancer is actually a very common disease that affects many men. However, some people are at a higher risk than others. Prostate cancer risk factors include:
- Age: Risk directly increases with age. The average age of diagnosis is between age 66 and 67.
- Race: African American men are at a higher risk than men of other races.
- Family history: Those who have a first-degree relative, father or a brother, with prostate cancer are at greater risk. There is a genetic mutation that may make it more likely to occur among family members with breast or ovarian cancer, like in those who have Lynch syndrome or BRCA1 or BRCA2.
- Geographic location: Prostate cancer is more common in North America, northwest Europe, Australia and the Caribbean. It is unclear whether that is because these areas screen more frequently for prostate cancer.
Exceptions And Barriers To Active Surveillance
In his UCSF program, Dr. Cooperberg said, about 95% of men diagnosed with low-risk prostate cancer are put on active surveillance. As an academic center that began implementing and studying active surveillance in the mid-1990s, thats likely higher than what is typically seen in the United States, he acknowledged.
But a reasonable target for the time being is around 80%, he said. Thats consistent with where rates top out in countries like Sweden and in other large, integrated health care systems in Europe where active surveillance has long been standard practice.
The bottom line, Dr. Cooperberg said, is that even though the vast majority of men with low-risk prostate cancer should be put on active surveillance, there will always be exceptions.
Those exceptions, for example, can include men with a strong family history of prostate cancer or who have urological symptoms related to the disease that immediate treatment can help to alleviate.
There can also be considerations that go beyond clinical or biological factors. For patients in rural areas or those who lack reliable transportation, anything that requires regular visits to the hospital or doctors office over a long period could push some men toward choosing immediate treatment, Dr. Watts said.
In addition, she noted, it can be challenging to explain the medical basis for active surveillance. In some patients minds, opting for active surveillance means missing a window of opportunity for cure, she said.
British Columbia Specific Information
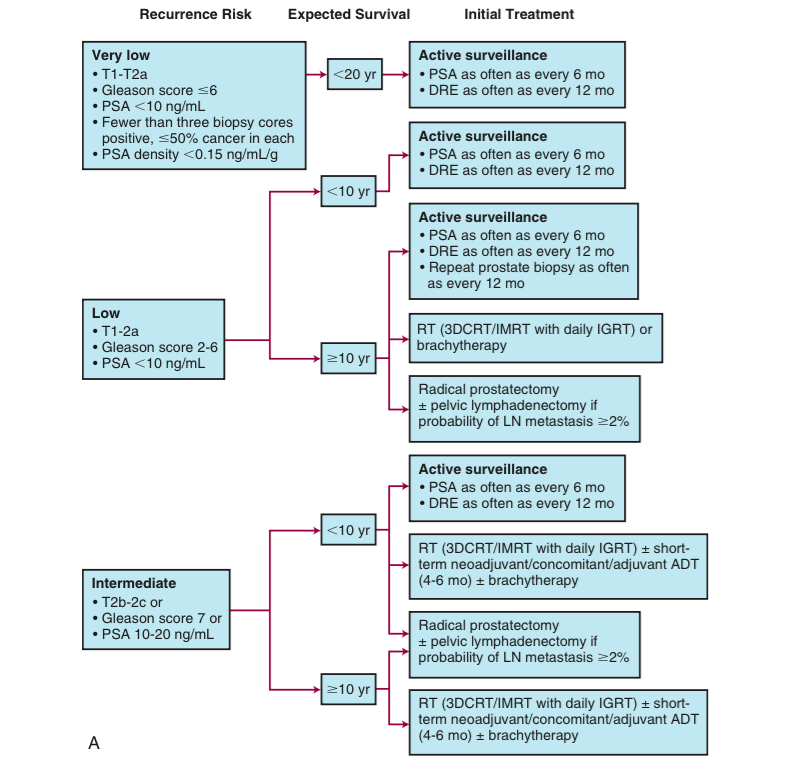
You are considered a low-risk patient if you have a PSA value that is equal or less than 10 nanograms per millilitre , a Gleason score that is equal or less than 6, and your cancer stage is T1c/T2a. PSA is your prostate specific antigen measured by a blood test, the Gleason score indicates how aggressive the cancer is by looking at tissue biopsy results, and the cancer stage describes how much the cancer has spread.
Active surveillance has been developed to allow for careful management of men with low-risk prostate cancer. For more information, visit BC Cancer Agency Prostate.
Top of the pageDecision Point
You may want to have a say in this decision, or you may simply want to follow your doctors recommendation. Either way, this information will help you understand what your choices are so that you can talk to your doctor about them.
Read Also: How Do They Check Your Prostate
Dont Rush To Get Treatment
If you are diagnosed with prostate cancer, you should discuss treatments and quality-of-life issues with your cancer care team.
Your team should include a urologist and a radiation oncologist. You can also get helpful advice from a medical oncologist.
Common treatments are surgery and radiation. However, there is another approach to learn about. Its called active surveillance or watchful waiting. Its for men with low-risk prostate cancer. In active surveillance, your team watches your condition closely. If tests show that its getting worse, you will get treatment. Discuss active surveillance with your team. Heres why:
Prostate Cancer: Avoidance Of Overuse Of Bone Scan For Staging Low Risk Prostate Cancer Patients
| 0389e | |
| Description |
Percentage of patients, regardless of age, with a diagnosis of prostate cancer at low risk of recurrence receiving interstitial prostate brachytherapy, OR external beam radiotherapy to the prostate, OR radical prostatectomy who did not have a bone scan performed at any time since diagnosis of prostate cancer |
|---|---|
| Initial Population |
All patients, regardless of age, with a diagnosis of prostate cancer |
| Denominator |
Equals Initial Population at low risk of recurrence receiving interstitial prostate brachytherapy, OR external beam radiotherapy to the prostate, OR radical prostatectomy |
| Denominator Exclusions |
None |
| Numerator |
Patients who did not have a bone scan performed at any time since diagnosis of prostate cancer |
| Numerator Exclusions |
Not Applicable |
| Denominator Exceptions |
Documentation of reason for performing a bone scan |
| Measure Steward | |
|
Higher score indicates better quality |
|
| Guidance |
A higher score indicates appropriate treatment of patients with prostate cancer at low risk of recurrence. Only patients with prostate cancer with low risk of recurrence will be counted in the performance denominator of this measure. This eCQM is a patient-based measure. This version of the eCQM uses QDM version 5.5. Please refer to the eCQI resource center for more information on the QDM. |
| MIPS Quality ID | |
| No Version Available |
Also Check: How Deadly Is Prostate Cancer
Stay Active To Support Prostate Health
In addition to eating a healthy diet, you should stay active. Regular exercise pares down your risk of developing some deadly problems, including heart disease, stroke, and certain types of cancer. And although relatively few studies have directly assessed the impact of exercise on prostate health, those that have been done have concluded, for the most part, that exercise is beneficial. For example:
Get more information and the latest news about prostate health at www.HarvardProstateKnowledge.org.
The Gleason Grading System
Screening for prostate cancer involves the prostate-specific antigen test and a digital rectal exam. If results are suspect, your doctor may recommend a prostate biopsythe only way to confirm the diagnosis.
During a prostate biopsy, a urologist uses a small needle to remove tissue samples from different parts of the prostate. These samplesalso called coresare then sent to a pathologist so they can review each one under a microscope.
The pathologist uses a pattern scale, developed by Donald Gleason, MD, PhD in 1966, to give each sample a grade from 1 to 5. Grade 1 cells are well-differentiated and look like normal tissue. Grade 5 cells, on the other hand, are poorly differentiated or even unrecognizable from normal tissue.
Your Gleason score is the sum of the two numbers that represent the most common types of tissue found in your biopsy. The first number in the equation is the most common grade present, the second number is the second most common grade. For example, if seven of your cores are grade 5 and five are grade 4, your Gleason score would be 5+4, or a Gleason 9.
Today, pathologists typically only flag tissue samples that are grade 3 or higher, making 6 the lowest Gleason score.
In 2014, a revised grading system for prostate cancercalled Grade Groupswas established. This system builds on the Gleason scoring system and breaks prostate cancer into five groups based on risk. This can help make it easier to understand the Gleason score scale.
Also Check: Can Prostate Infection Spread Partner
Treatment For Low Risk Prostate Cancer
Widespread screening with PSA and DRE leads to the detection of prostate cancer at an early stage. However, a significant number of prostate cancers diagnosed are slow to develop and do not pose a threat to a mans longevity. Once diagnosed with prostate cancer, at UCLA we use information such as your PSA, Gleason grade, MRI findings and biomarkers to determine the overall risk of your cancer spreading. If you have low risk prostate cancer , we know that you are not likely to die of prostate cancer. As a result, we will often not recommend treatment for these cancers.
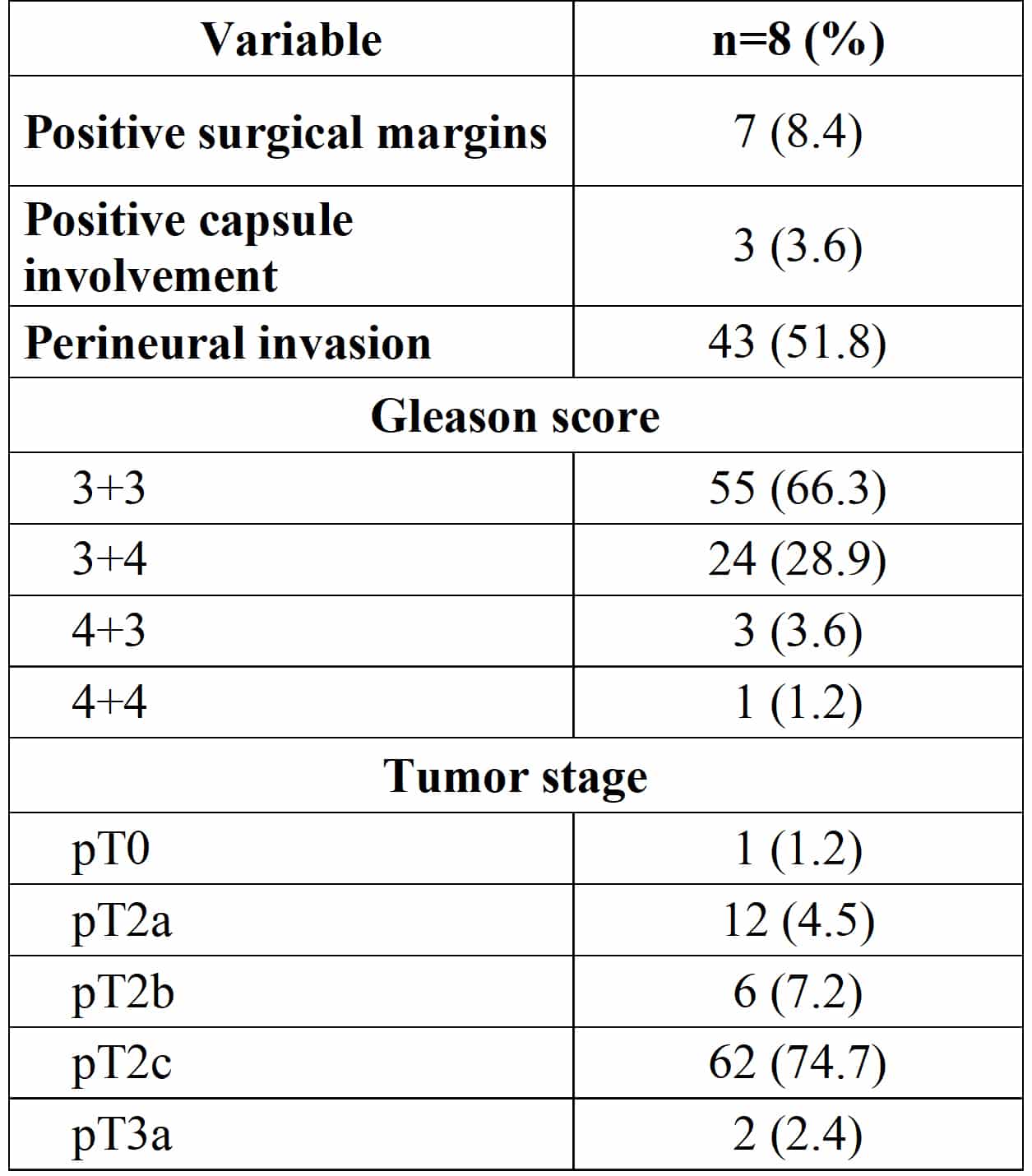
Efficacy Of The Treatment
Three patients developed biochemical failure, thus providing a 7-year actual biochemical failure-free survival rate of 99.1% . Biochemical failure was observed exclusively in cases with distant metastasis: two cases with lymph node metastasis and one case with bone metastasis, thus yielding a 7-year freedom from clinical failure rate of 99.1% . We observed eight deaths, but there was no death from prostate cancer, thus yielding a 7-year cause-specific survival rate of 100%, and an OS rate of 98.4% .
Kaplan-Meier BFFS, FFCF, CSS and OS. A Kaplan-Meier BFFS: BFFS rate is 99.1% at 7 years. B Kaplan-Meier FFCF: FFCF rate is 99.1% at 7 years. C Kaplan-Meier CSS: CSS rate is 100% at 7 years. D Kaplan-Meier OS: OS rate is 98.4%.
Recommended Reading: External Beam Radiation Treatment For Prostate Cancer
You May Like: Is Black Pepper Bad For Prostate
How Is Prostate Cancer Diagnosed
Screenings are the most effective way to catch prostate cancer early. If you are at average cancer risk, youll probably have your first prostate screening at age 55. Your healthcare provider may start testing earlier if you have a family history of the disease or are Black. Screening is generally stopped after age 70, but may be continued in certain circumstances.
Screening tests for prostate cancer include:
- Digital rectal exam: Your provider inserts a gloved, lubricated finger into the rectum and feels the prostate gland, which sits in front of the rectum. Bumps or hard areas could indicate cancer.
- Prostate-specific antigen blood test: The prostate gland makes a protein called protein-specific antigen . Elevated PSA levels may indicate cancer. Levels also rise if you have BPH or prostatitis.
- Biopsy: A needle biopsy to sample tissue for cancer cells is the only sure way to diagnose prostate cancer. During an MRI-guided prostate biopsy, magnetic resonance imaging technology provides detailed images of the prostate.
When Should You Get Immediate Treatment For Prostate Cancer
If your cancer is advanced or higher-risk, you will probably need treatment right away. Signs of higher-risk cancer include:
- PSA value that is high or rapidly rising.
- Test results show that the tumor is outside the prostate gland. Or the tumor is growing rapidly and is likely to spread outside the gland.
- Gleason score is high-risk.
Ask your team if your cancer shows any of these signs. If so, active surveillance may not be a good choice.
Also Check: Can You Get An Erection If Your Prostate Is Removed
More Active Surveillance But Not Enough
To conduct their study, Dr. Cooperberg and his colleagues looked at data from all men newly diagnosed with prostate cancer in the AUA Quality Registry. This registry collects real-time data from more than 240 participating US urology practices and more than 2,100 urologists.
Overall, of the more than 84,000 patients covered by the study, 20.3% were diagnosed with low-risk disease. The number of men diagnosed with low-risk disease actually fell during the study period, from about 24.6% in 2014 to 14.0% in 2019. That finding is consistent with other recent studies showing a decline in low-risk diagnoses, which researchers have attributed to fewer men being screened via PSA testing.
But even as diagnoses of low-risk disease have dropped, more men with low-risk disease are opting for active surveillance, Dr. Cooperberg reported. In 2014, 26.5% of men with low-risk prostate cancer chose active surveillance. By the end of 2021, 59.6% did.
Rates of active surveillance also increased among men diagnosed with intermediate-risk prostate cancer, which is considered to have a modestly greater likelihood than low-risk prostate cancer of progressing to the point where it could be fatal.
The variability in the use of active surveillance is alarming, Dr. Parnes said. It likely reflects, at least to some degree, entrenched patterns of care among some urologists. For some, I suspect their feeling is, I treat cancer, and this is cancer. Im not having this conversation , he said.
Selenium And Vitamin E
The medical community once considered selenium and vitamin E to be opponents of cancer.
However, more recent research suggests that these compounds, when taken together or in isolation, can increase the risk of prostate cancer in some people.
Anyone concerned about prostate cancer should avoid supplements containing vitamin E or selenium.
Recommended Reading: Is Ginger Good For Prostate
Talk To Your Cancer Care Team
Your team is an important source of advice. Some men may benefit from having a low-risk tumor treated right away, even if they might have side effects. Discuss your treatment options and quality-of-life issues with your team.
This report is for you to use when talking with your health-care provider. It is not a substitute for medical advice and treatment. Use of this report is at your own risk.
04/2014
What Exactly Is The Prostate
Here are some basics about the prostate:
The prostate is the size of a walnut and weighs about an ounce.
It can be found just below your bladder and in front of your rectum.
However, prostate cancer can sometimes be aggressive and fast-moving. It can spread beyond your prostate to other parts of your body. First, it may reach your prostates neighbors, like the seminal vesicles, the bladder, or your rectum. It can then move on to your lymph nodes, organs, and, commonly, your bones. Once it has traveled from the prostate, it becomes tougher to treat.
Recommended Reading: What Is A Prostate Specialist Called
Read Also: How Do They Do Radiation For Prostate Cancer
Treating Stage Iv Bladder Cancer
These cancers have reached the pelvic or abdominal wall , may have spread to nearby lymph nodes , and/or have spread to distant parts of the body . Stage IV cancers are very hard to get rid of completely.
Chemotherapy is usually the first treatment if the cancer has not spread to distant parts of the body . The tumor is then rechecked. If it appears to be gone, chemo with or without radiation or cystectomy are options. If there are still signs of cancer in the bladder, chemo with or without radiation, changing to another kind of chemo, trying an immunotherapy drug, or cystectomy may be recommended.
Chemo is typically the first treatment when bladder cancer has spread to distant parts of the body . After this treatment the cancer is rechecked. If it looks like its gone, a boost of radiation to the bladder may be given or cystectomy might be done. If there are still signs of cancer, options might include chemo, radiation, both at the same time, or immunotherapy.
In most cases surgery cant remove all of the cancer, so treatment is usually aimed at slowing the cancers growth and spread to help people live longer and feel better. If surgery is a treatment option, its important to understand the goal of the operation whether its to try to cure the cancer, to help a person live longer, or to help prevent or relieve symptoms from the cancer.
Because treatment is unlikely to cure these cancers, many experts recommend taking part in a clinical trial.
Differential Diagnosis Of Adenocarcinoma In Needle Biopsy Tissue
Numerous entities, both benign and malignant, should be considered in the differential diagnosis of prostatic adenocarcinoma. Indepth discussion of these entities is beyond the scope of this review.
Recent reviews have highlighted the benign lesions or pseudoneoplasms that may mimic prostatic adenocarcinoma., Atypical adenomatous hyperplasia and atrophy are the benign conditions that are most likely to be misdiagnosed as prostatic carcinoma.,, Crowded benign glands may also be mistaken for prostatic adenocarcinoma. The pathologist should always consider the possibility of a benign mimicker of prostatic carcinoma, particularly atrophy, but also all other entities , before making a diagnosis of adenocarcinoma of the prostate.
A descriptive diagnosis which may be rendered if the histological or immunohistochemical findings are thought to be worrisome but not fully diagnostic of carcinoma, is atypia,, also known as atypical suspicious for carcinoma or atypical small acinar proliferation. Such a diagnosis is given in about 45% of all prostate needle biopsy specimens.,
The main nonprostatic, secondary malignancy to think about before diagnosing prostatic carcinoma in needle biopsy of the prostate is urothelial carcinoma involving the prostate.,
Recommended Reading: What Is Treatment For Prostate Cancer With Bone Metastases
What Are The Treatment Options For Low
Men with low-risk prostate cancer have four treatment options: active surveillance, external radiotherapy, internal radiotherapy and surgery to remove the prostate.
- Active surveillance involves monitoring the prostate cancer, and only treating it if there are signs that it is progressing. This approach is based on the fact that low-risk prostate cancer often grows very slowly or doesn’t grow at all, so treatment often isnt needed.
- In external radiotherapy, the cancer is exposed to radiation from outside the body, through the skin.
- In internal radiotherapy , the cancer is exposed to radiation from slightly radioactive seeds that are implanted inside the body.
- The aim of surgery wird is to remove the tumor, together with the whole prostate, seminal vesicles and outer capsule.
Radiation and the surgical removal of the prostate are also referred to as “curative” treatments because the aim is to remove all of the tumor cells. But a few cancer cells may stay in the body, or new cancer cells might develop. For this reason, men who have had radiotherapy or surgery are still advised to have regular PSA tests.
