Prostate Cancer Risk Groups
In addition to stage, doctors may use other prognostic factors to help plan the best treatment and predict how successful treatment will be. Examples of these include the National Comprehensive Cancer Network risk group categories and the Cancer of the Prostate Risk Assessment risk score from University of California, San Francisco.
Information about the cancers stage and other prognostic factors will help the doctor recommend a specific treatment plan. The next section in this guide is Types of Treatment. Use the menu to choose a different section to read in this guide.
Radical Prostatectomy Versus Radiation Therapy
The natural history of the disease, life expectancy of the patient, and potential for cure provide compelling reasons to treat the patient presented in this point-counterpoint discussion aggressively, with the intent to cure the prostate cancer. The next question, and the primary subject of this point-counterpoint discussion, is whether to offer radical prostatectomy or radiation therapy. The decision to offer one treatment or the other must reflect a critical analysis of benefits and risks.
As cancer diagnoses go, prostate cancer is often a less serious one. Prostate cancer is frequently slow-growing and slow to spread. For many men, prostate cancer is less serious than their other medical conditions.
For these reasons, and possibly because of earlier detection of low-grade prostate cancers, prostate cancer has one of the highest survival rates of any type of cancer. WebMD takes a look at prostate cancer survival rates and what they mean to you.
You May Like: What To Expect During Chemo
Seminal Vesicle And Lymph Node Positive
The determination of risk is not straightforward. As discussed earlier, the three standard prognostic factors are Gleason score, PSA and stage. There are subgroups in each that appear to have a very high risk of recurrence. So the first place to start is whether there are any single factors that portend such a great risk that they alone would indicate the need for adjuvant treatment. One that easily falls into this category is that of positive lymph node metastasis. The risk of failure in these patients is non-controversial and we wont discuss it further. We would submit that the second of these is that of seminal vesicle involvement, which has been extensively studied .
Table 1
| 56% |
Definition of failure and disease free survival: based on biochemical failure and includes biopsy proven local recurrence and radiologically detected distant metastasis
* 2 year endpoint for all groups. Mar+ is margin positive Mar- is margin negative EPE+ is extraprostatic extension present EPE- is extraprostatic extension absent foc is focal Ext is extensive Est is established Gl is Gleason score
The limitations of the small numbers of patients in the more favorable subgroups make selecting those patients for avoidance of intervention a risky proposition. In a subgroup analysis of the SWOG adjuvant study , all the subgroups benefitted from adjuvant radiation to the same degree .
You May Like: Best Lotion For Chemo Skin
Don’t Miss: How Do You Milk A Prostate
The Most Common Symptoms Of Stage 3 Mesothelioma Include:
- Shortness of breath
As the tumors continue to grow and spread throughout the chest, symptoms will become more problematic. Stage 3 symptoms vary from patient to patient depending on where the cancer is spreading and if the tumor mass damages vital organs. Some patients may experience referred pain felt in the neck, back or shoulders.
A tumor invading the chest wall may cause increased chest pain, while tumors forming around the lung may lead to increased breathing difficulties. Pleural mesothelioma tumors also cause increased pleural fluid, which puts pressure on the lungs. Symptoms and characteristics of stage 3 mesothelioma vary based primarily on cancer type.
Connect with a Top Mesothelioma Specialist
Dont Miss: Targeted Therapy For Breast Cancer
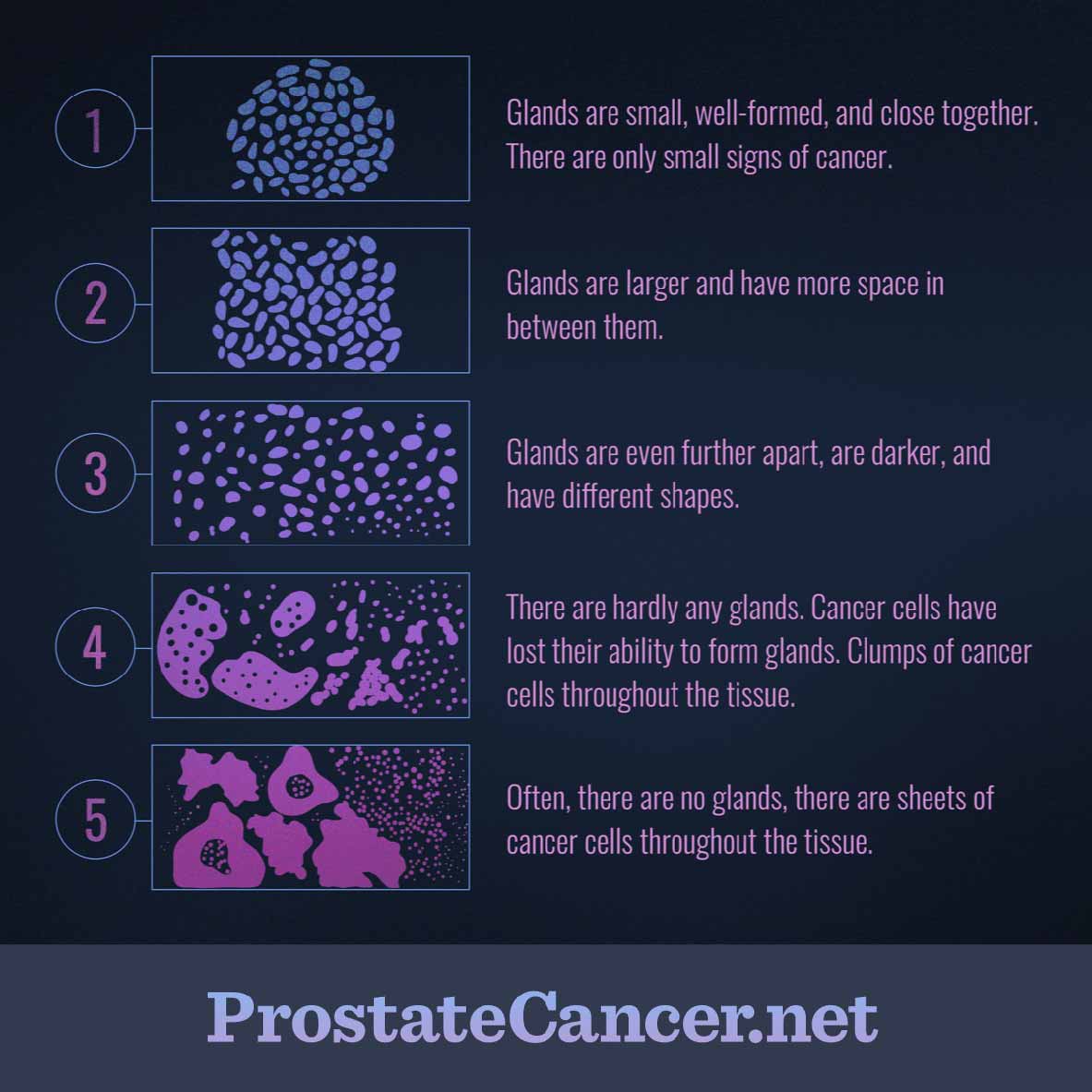
How To Interpret A Gleason Score
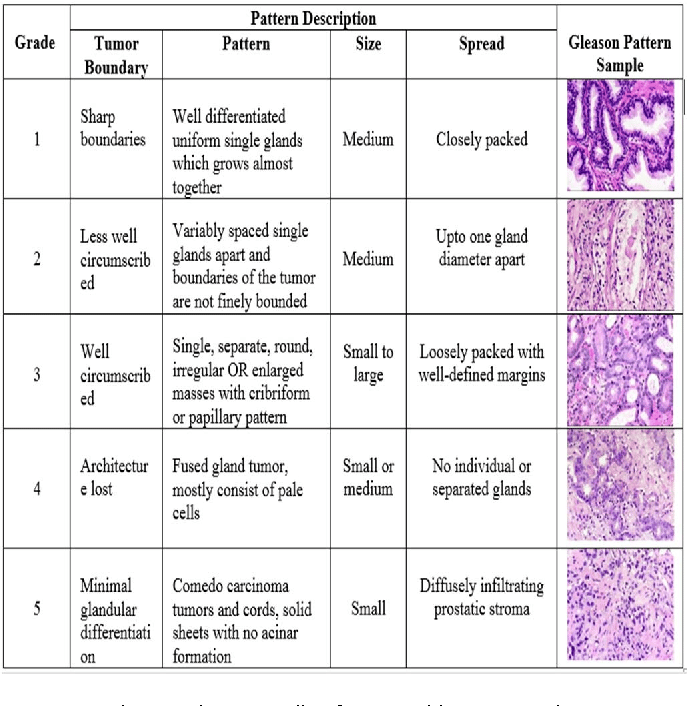
A high Gleason score suggests that prostate cancer is more likely to progress and spread to other areas of the body. A low Gleason score, on the other hand, suggests that a malignancy is growing more slowly.
Technically, Gleason scores can range from 2 to 10 . However, Gleason scores usually range from 6 to 10:
- Gleason scores of 6 and lower indicate low-grade prostate cancer.
- A Gleason score of 7 indicates intermediate- or medium-grade prostate cancer.
- Gleason scores of 8 to 10 indicate high-grade prostate cancer.
Also Check: What Is Unfavorable Intermediate Risk Prostate Cancer
Movement Builds To Classify Gleason 6 Prostate Lesions As Nonmalignant
In prostate cancer, as in life, you roll the dice.
In craps, 3+3 is called a âhard six.â Itâs hard because you can only win if you repeat with a combination of 3+3. Any other sixes you roll â 4+2, 5+1 â are losers.
Gleason 3+3 is a hard six in prostate cancer. It is the lowest grade cancer in the traditional Gleason scoring system. Still, to the eye of a pathologist, a Gleason 6 looks like a malignancy.
Now, a few experts are questioning whether this hard six is a cancer at all. Some urologists see a Gleason 6 as a noncancerous growth that has the potential to be invasive, but most likely will never spread to other organs or end up killing a man.
To a patient like me, who has been on active surveillance for 10 years, a Gleason 6 can create a big medical fuss lasting years with regular prostate-specific antigen blood tests, digital rectal exams , biopsies, and MRIs. It can cause âanxious surveillanceâ that prompts them to drop AS and undergo unnecessary radical prostatectomy, which poses a potential risk of impotence and urinary incontinence.
The Gleason 6 diagnosis can yield polar opposite recommendations from urologists. Ten years ago, I found this to be the case in the matter of a day.
On December 14, 2010, a local urologist recommended I undergo a radical prostatectomy within the week. When asked, he said he didnât support active AS, then a relatively new approach for monitoring low-grade prostate cancer.
âThe right thing to doâ
Mixed reactions
Grade Groups Of Prostate Cancer
The Grade Group is the most common system doctors use to grade prostate cancer. It is also known as the Gleason score.
The grade of a cancer tells you how much the cancer cells look like normal cells. This gives your doctor an idea of how the cancer might behave and what treatment you need.
To find out the Grade Group, a pathologist
Read Also: How Fast Does Prostate Cancer Progress
What Does It Mean If In Addition To Cancer My Biopsy Report Also Mentions Acute Inflammation Or Chronic Inflammation
Inflammation of the prostate is called prostatitis. Most cases of prostatitis reported on biopsy are not caused by infection and do not need to be treated. In some cases, inflammation may increase your PSA level, but it is not linked to prostate cancer. The finding of prostatitis on a biopsy of someone with prostate cancer does not affect their prognosis or the way the cancer is treated.
Does Untreated Clinical Gleason 6 Disease Cause Symptoms Or Death
Several studies that examined the natural history of untreated prostate cancer diagnosed in the prePSA screening era have suggested that men with Gleason 6 cancers are at risk for prostate cancerspecific mortality beyond 10 years of follow-up. The majority of the Gleason 6 disease was T1a/b disease, which was identified at the time of transurethral resection of the prostate for benign disease. Today, it is extremely rare to diagnose T1a/b disease because fewer TURPs are performed and those undergoing TURP have been prescreened with PSA testing. The results of the natural history studies in the PSA screening era are also problematic because many of the cases were likely misclassified at the outset because of the aforementioned limitations attributable to the random-systematic tissue sampling guided by TRUS.
With reported median follow-up ranging from 22 to 82 months, current active surveillance cohorts remain immature at this time, and longer follow-up will be necessary to draw definitive conclusions. Thus far, cancer-specific survival among these cohorts has been > 97%, and there are no data to suggest inferior outcomes after delayed radical therapy, as compared with immediate therapy.
You May Like: Survival Rate For Stage 4 Prostate Cancer
What Does It Mean When There Are Different Core Samples With Different Gleason Scores
Cores may be samples from different areas of the same tumor or different tumors in the prostate. Because the grade may vary within the same tumor or between different tumors, different samples taken from your prostate may have different Gleason Scores. Typically, the highest Gleason Score will be the one used by your doctor for predicting your prognosis and deciding treatment.
Similar Articles Being Viewed By Others
Carousel with three slides shown at a time. Use the Previous and Next buttons to navigate three slides at a time, or the slide dot buttons at the end to jump three slides at a time.
22 June 2022
Rita Alaggio, Catalina Amador, Wenbin Xiao
volume 8, Article number: 12054
An to this article was published on 23 November 2021
An to this article was published on 16 May 2019
This article has been
Recommended Reading: What Do Doctors Look For In A Prostate Exam
How Is The Gleason Score Derived
The pathologist looking at the biopsy sample will assign one Gleason grade to the most predominant pattern in your biopsy and a second Gleason grade to the second most predominant pattern. For example: 3 + 4. The two grades will then be added together to determine your Gleason score. Theoretically, Gleason scores range from 2-10. However, since Dr. Gleasons original classification, pathologists almost never assign scores 2-5, and Gleason scores assigned will range from 6 to 10, with 6 being the lowest grade cancer.
Staging Of Prostate Cancer
The stage of a cancer describes its size and how far it has spread. The results of your tests help your doctors decide on the stage and plan your treatment.
We understand that waiting to know the stage and grade of your cancer can be a worrying time. Were here if you need someone to talk to. You can:
Macmillan is also here to support you. If you would like to talk, you can:
|
Any T, any N, M1 Any Grade Group Any PSA |
The cancer might or might not be growing into tissues near the prostate and might or might not have spread to nearby lymph nodes . It has spread to other parts of the body, such as distant lymph nodes, bones, or other organs . The Grade Group can be any value, and the PSA can be any value. |
Prostate cancer staging can be complex. If you have any questions about your stage, please ask someone on your cancer care team to explain it to you in a way you understand.
While the stage of a prostate cancer can help give an idea of how serious the cancer is likely to be, doctors are now looking for other ways to tell how likely a prostate cancer is to grow and spread, which might also help determine a mans best treatment options.
Also Check: What Does Your Prostate Do
How Is Active Surveillance Done
Although the protocol can vary, recommendations for active surveillance generally call for routine PSA tests and prostate biopsies to check for any indication that the cancer might be growing.
For example, patients at Montefiore Health System in New York City get a PSA test every 36 months, at least initially, and an MRI-guided biopsy a year after diagnosis, said Kara Watts, M.D., a urologist at the hospital who specializes in treating prostate cancer but was not involved in the study.
After the initial PSA tests and biopsy, how often they are performed depends largely on the patients particular situation, Dr. Watts explained.
We have a flexible protocol, particularly for people at both ends of the spectrum, she continued. For a man in his 70s and a life expectancy of 510 years , she said, additional PSA tests or biopsies may only be conducted every few years or only if he has symptoms. An otherwise healthy man in his 50s, on the other hand, will usually continue to have PSA tests and MRI-guided biopsies on a schedule similar to the initial protocol.
At the NIH Clinical Center, where Dr. Parnes sees patients, in addition to routine PSA testing, MRI-guided biopsies are used to help inform decisions around whether to pursue active surveillance and as part of the surveillance protocol.
Prostate Cancer Grading & Prognostic Scoring
The Gleason Score is the grading system used to determine the aggressiveness of prostate cancer. This grading system can be used to choose appropriate treatment options. The Gleason Score ranges from 1-5 and describes how much the cancer from a biopsy looks like healthy tissue or abnormal tissue . Most cancers score a grade of 3 or higher.
Since prostate tumors are often made up of cancerous cells that have different grades, two grades are assigned for each patient. A primary grade is given to describe the cells that make up the largest area of the tumor and a secondary grade is given to describe the cells of the next largest area. For instance, if the Gleason Score is written as 3+4=7, it means most of the tumor is grade 3 and the next largest section of the tumor is grade 4, together they make up the total Gleason Score. If the cancer is almost entirely made up of cells with the same score, the grade for that area is counted twice to calculated the total Gleason Score. Typical Gleason Scores range from 6-10. The higher the Gleason Score, the more likely that the cancer will grow and spread quickly.
Recommended Reading: What Is The Gleason Score For Prostate Cancer
What The Numbers Mean
The pathologist who examines the cellstaken during your biopsywill look at their patterning in the samples. Each area is graded on a scale of 1 to 5, and the two numbers are added together to get the Gleason score.
If a Gleason score is written in your pathology report as 3+4=7, this means most of your tumor is grade 3 and less of it is grade 4. These numbers are then added together for a total Gleason score of 7.
Grades 1 and 2 are not usually used to describe cancer these grades are for tissue that almost looks normal and isn’t considered cancerous. The lowest possible Gleason score of a cancer found in a prostate biopsy is 6cancer with the least risk of spreading quickly. The highest score is 10cancer with the most risk of being aggressive.
Because a scoring system that starts with the number 6 can be confusing, recently the Gleason Grade Grouping were introduced. This group number is based on the numbers used to create a samples Gleason score, but start with 1 instead of 6 and range from 1 to 5 .
What Are The Side Effects Of A Biopsy
Having a biopsy can cause side effects. These will affect each man differently, and you may not get all of the possible side effects.
Pain or discomfort
Some men find the biopsy painful, but others have only slight discomfort. Your nurse or doctor may suggest taking mild pain-relieving drugs, such as paracetamol, to help with any pain.
If you have any pain or discomfort that doesnt go away, talk to your nurse or doctor.
Short-term bleeding
A small number of men who have a TRUS biopsy may have more serious bleeding in their urine or from their back passage . This can also happen if you have a transperineal biopsy but it isn’t very common. If you have severe bleeding or are passing lots of blood clots, this is not normal. Contact your doctor or nurse at the hospital straight away, or go to the accident and emergency department at the hospital.
Infection
Some men get an infection after their biopsy. This is more likely after a TRUS biopsy than after a transperineal biopsy. It’s very important to take any antibiotics youre given, as prescribed, to help prevent this. But you might still get an infection even if you take antibiotics.
Symptoms of a urine infection may include:
- pain or a burning feeling when you urinate
- dark or cloudy urine with a strong smell
- needing to urinate more often than usual
- pain in your lower abdomen .
If you have any of these symptoms, contact your doctor or nurse at the hospital straight away. If you cant get in touch with them, call your GP.
Don’t Miss: Long-term Side Effects Of Seed Implants For Prostate Cancer
Gleason Score For Prostate Cancer
In the 1960s, VA researcher Donald Gleason and his colleagues at the Minneapolis VA Hospital developed a grading system to classify the stage and prognosis of prostate cancer. Today, the Gleason score is almost universally used to rate prostate cancer. It is considered the most reliable measure of prostate cancer’s chances of growing and spreading.
To find a Gleason score, doctors take a biopsy of a patient’s prostate and look at the cells under a microscope. The pattern of cancer cells are ranked from 1 to 5. A score of 1 means cells resemble a normal prostate, with areas of cancer cells small and closely packed. Higher scores mean that the cancer cells are more widespread. Doctors add the score for the most common cell pattern with the next pattern with the highest score.
Total scores range from 2 to 10, with a higher score meaning more advanced cancer and a worse prognosis. Cancers with scores of 2-4 are usually considered benign or slow-growing. Scores of 5-7 are the most common, and are highly treatable. Scores of 8-10 show an advanced stage of cancer ad are unlikely to be cured.
Gleason served in the U.S. Army Medical Corps before going to work at the Minneapolis VA Hospital. He became the head pathologist in 1986. He died in 2008.
Principal investigator: Donald Gleason, M.D. Minneapolis VA Hospital
Selected publications:
