Extended Systematic And Saturation Biopsies
The debate on the optimal number of biopsy core samples that should be taken is still open. Ploussard et al. have demonstrated that an increase from 12 to 21 cores significantly increases the detection rate of significant PC . Transperineal mapping biopsy aims for optimal staging and detection of all significant PC by using an external grid of 5 mm . Lecornet et al. have shown that TPMB detects nearly all significant PC lesions above 0.5 mL . However, TPMB is significantly more invasive than SB leading to urinary retention and the potential for oversampling of clinically insignificant PC, which often results in overtreatment. Valerio et al. report that, beside an accurate index lesion detection, insignificant PC was detected in up to 42.9% of TPMB . Additionally, the prostate is mobile, deformable and swells during biopsy, so real-time sampling errors in vivo might still occur . Thus, Ukimura et al. conclude that the specific clinical indication for TPMB, remains under debate .
Less Than Half Of Men Get Colon Cancer Tests
Data came from a 2002 national phone survey of more than 22,000 men aged 50 and older.
About 61% of the men had stayed current with the PSA tests or a digital rectal exam to screen for prostate cancer. But only 48% had followed colorectal cancer screening guidelines for fecal occult blood test, sigmoidoscopy, or colonoscopy.
That means that a third of men who were good about getting PSA tests didnt make the same effort with colon cancer screening, the study explains.
Older men and black men were more likely to follow colon cancer testing guidelines. Health insurance, bigger paychecks, and higher education levels also helped.
Adherence to prostate cancer screening had the biggest influence on whether men underwent colon cancer screening. Men who adhered to prostate cancer screening were two to three times more likely to have had a colon cancer screening.
Hispanic men, smokers, and those who reported general good health were less likely to follow colon cancer screening guidelines, says the study, which appears in Februarys Journal of the American College of Surgeons.
The study was conducted by the University of Michigans Ruth Carlos, MD, MS, and colleagues.
Show Sources
Permutations Of Twofold Cross
Owing to the limited number of higher Gleason grade lesions, we consider a twofold cross-validation to maximize the number of lesions of each Gleason grade in both training and testing. However, twofold cross-validation may not adequately demonstrate generalization of CAD systems. Prostate literature often considers more folds, such as 10-fold cross-validation. To compensate for these limitations, we formed five twofold cross-validation sets, all resulting from random permutations of the original data set. This helps better demonstrate generalization while leaving a large number of test lesions of various Gleason grades for analysis.
Read Also: How Can You Tell If You Have A Prostate Infection
Can Mri Detect Cancer
MRI scans can help medical professionals detect cancer. And whole-body magnetic resonance imaging has become available to the general public to screen for potential cancer.
If you find out early that you have a tumor or cancer, you can start treatment earlier, giving you a head start and improving your prognosis. This way, you also avoid more costly cancer treatment.
Oncologists use whole-body MRI more often to manage treatment for patients whose cancer is likely to metastasize to bone marrow, such as prostate and breast cancers. Oncologists and radiologists also use WB-MRI in lymphoma follow-up because of its superior diagnostics compared to positron emission tomography.
As an imaging tool, WB-MRI minimizes ionizing radiation exposure.
Read Also: Living With Metastatic Prostate Cancer
Biopsy During Surgery To Treat Prostate Cancer
If there is more than a very small chance that the cancer might have spread , the surgeon may remove lymph nodes in the pelvis during the same operation as the removal of the prostate, which is known as a radical prostatectomy .
The lymph nodes and the prostate are then sent to the lab to be looked at. The lab results are usually available several days after surgery.
Read Also: Prostate Cancer Nursing Care Plan
Excellence In Prostate Cancer Detection
The Sperling Prostate Center is a technologically-advanced, patient-oriented practice dedicated to providing the most effective techniques in prostate cancer detection and diagnosis. Unlike the PSA blood test or DRE, our approachutilizing BlueLaser 3T mpMRI imaging with the newest advances in Restricted Spectrum Imaging, powered Artificial Intelligenceoffers the best pathway to diagnostic superiority.
Bluelaser 3t Mpmri: Better Early Detection
If a high PSA raises suspicion of cancer, the next step before biopsy is to obtain an accurate 3D image of the gland that defines both normal and cancerous tissue. It is just as important to see what is healthy as what is unhealthy! Ultrasound doesnt do this because it cant reveal specific differences needed to detect what is and isnt cancer.
Our BlueLaser 3T mpMRI Plus features the latest advance in multiparametric imaging sequences. It is called Restricted Spectrum Imaging powered by AI, and it takes cancer detection to a whole new level. RSI was originally developed for brain imaging where it accurately picks up previously undetectable but telltale differences in neurological diseases. When applied to prostate imaging, potentially cancerous lesions literally stand out.
Studies now show that combining technological breakthroughs and expertise1 makes an essential difference. By offering the increased accuracy of both RSI2 powered by AI3 together with the pioneering experience of Dr. Sperling and his team, the Sperling Prostate Center remains at the forefront of prostate cancer imaging.
RSI-MRI+ leverages an advanced diffusion MRI technique called Restriction Spectrum Imaging, powered by AI, to enable faster, more accurate prostate cancer detection.
Remember: Early prostate cancer has NO SYMPTOMS. Early detection results in better diagnosis, better treatment decisions and better outcomes.
Read Also: Metastatic Castration Resistant Prostate Cancer Life Expectancy
Is Bluelaser 3t Mpmri Right For You
Knowledge is power only if man knows what facts not to bother with. -R.S. Lynd
Our BlueLaser 3T mpMRI empowers our patients by providing accurate knowledge about whats going on in their bodies, both normal and disease. You should consider BlueLaser 3T mpMRI for the earliest possible detection if:
- You have an elevated or rising PSA
- You have an abnormal DRE
- You were treated for a prostate infection or inflammation but your PSA is still high
- You are on Active Surveillance
- You are in a high-risk category to develop prostate cancer
- You have not had a PSA test but you have unusual urinary symptoms
Measuring The Accuracy Of An Mri In Prostate Cancer Diagnosis
To measure the accuracy of an MRI in detecting prostate cancer, studies are completed in contrast to another prostate cancer diagnosis procedure. In a study comparing the accuracy of an MRI scan to a biopsy, an MRI scan correctly diagnosed 93% whereas a biopsy correctly diagnosed 48% of the patients observed. In a separate study by Medline involving 2,585 patients, MRIs:
- Improved the detection of clinically significant prostate cancer by 57% when compared to a biopsy.
- Reduced the number of biopsy procedures by 33%.
- Reduced the number of core biopsies by 77%.
Its important to note that an MRI does not replace a biopsy, but is an ideal augment that can help doctors provide a more accurate diagnosis.
| TULSA Procedure
Read Also: Is It Prostatitis Or Prostate Cancer
How Does The Procedure Work
Unlike x-ray and computed tomography exams, MRI does not use radiation. Instead, radio waves re-align hydrogen atoms that naturally exist within the body. This does not cause any chemical changes in the tissues. As the hydrogen atoms return to their usual alignment, they emit different amounts of energy depending on the type of tissue they are in. The scanner captures this energy and creates a picture using this information.
In most MRI units, the magnetic field is produced by passing an electric current through wire coils. Other coils are inside the machine and, in some cases, are placed around the part of the body being imaged. These coils send and receive radio waves, producing signals that are detected by the machine. The electric current does not come into contact with the patient.
A computer processes the signals and creates a series of images, each of which shows a thin slice of the body. The radiologist can study these images from different angles.
MRI is often able to tell the difference between diseased tissue and normal tissue better than x-ray, CT, and ultrasound.
Tests To Diagnose And Stage Prostate Cancer
Most prostate cancers are first found as a result of screening. Early prostate cancers usually dont cause symptoms, but more advanced cancers are sometimes first found because of symptoms they cause.
If prostate cancer is suspected based on results of screening tests or symptoms, tests will be needed to be sure. If youre seeing your primary care doctor, you might be referred to a urologist, a doctor who treats cancers of the genital and urinary tract, including the prostate.
The actual diagnosis of prostate cancer can only be made with a prostate biopsy .
On this page
Also Check: What Does Prostate Cancer Mean
Is Prostate Mri With Or Without Mri
Background
Many prostate cancers are slow growing and may not have any harmful effects during a man’s lifetime. Meanwhile, clinically significant cancers can cause problems such as blockage of the urinary tract, painful bone lesions and death. The prostate-specific antigen test followed by tissue samples of the prostate with ultrasound guidance is often used to detect these cancers early. More recently, magnetic resonance imaging has also been used to help make the diagnosis.
What is the aim of this review?
The aim of this review was to compare MRI alone, MRI together with a biopsy, and a pathway that uses MRI to help decide whether to do a biopsy or not with the standard ultrasound guided biopsy in reference to template-guided biopsy.
What are the main results?
We examined evidence up to July 2018. The review included 43 studies, mainly from Western countries, of men aged 61 to 73 years.
In a population of 1000 men at risk for prostate cancer, where 300 men actually have clinically significant prostate cancer, MRI will correctly identify 273 men as having clinically significant prostate cancer but miss the remaining 27 men for the 700 men that do not have clinically significant prostate cancer, MRI will correctly identify 259 as not having prostate cancer but will misclassify 441 men as having clinically significant prostate cancer.
How reliable is the evidence?
What are the implications of this review?
The test accuracy analyses included 18 studies overall.
Choosing Where To Have Your Mri Is Key To Getting An Accurate Diagnosis
Until recently, a patient with abnormally high prostate-specific antigen level would be sent for a biopsy to determine if he had prostate cancer. This biopsy is guided by ultrasound, which urologists use to take twelve samples of the prostatein an attempt to find cancer regardless of where it is in the gland.
As a diagnostic tool for prostate cancer, however, ultrasound is limited. The ultrasound images show the prostate gland well enough to guide the twelve samples, but ultrasound often does not show the cancer inside the prostate. As a result, a biopsy may miss aggressive prostate cancer and may instead discover indolent prostate cancer that need not be treated.
Ultrasound may not find the bad cancer, and sometimes it identifies cancers that would be better left alone, says Dr. Hiram Shaish, assistant professor of radiology at Columbia University Irving Medical Center.
Now, men with high PSA levels are more and more frequently being offered a specialized test called multiparametric magnetic resonance imaging . MpMRI provides high-quality imaging that can visualize cancer in the prostate, distinguishing tumors that need to be treated from insignificant tumors that do not.
Given the insurance restrictions around this costly exam, patients basically have one chance to get it right.
Don’t Miss: What Is Removed During Prostate Surgery
What Are The Benefits Of Having An Mri At An Imaging Center Of Ngmc
- MRI is a noninvasive imaging technique that does not use ionizing radiation.
- MR images of soft-tissue structures are clearer and more detailed than those of other imaging methods.
- MRI a valuable tool in early diagnosis and evaluation of the extent of tumors, such as prostate cancer.
- MRI is valuable in diagnosing many conditions, including cancer. It is also useful in diagnosing non-cancerous conditions such as an enlarged prostate and infection.
- MRI helps distinguish between low-risk/slow-growing and high-risk/aggressive prostate cancers. It also helps determine if cancer has spread to other areas.
- MRI can detect abnormalities that might be obscured using other imaging methods.
- The MRI contrast is less likely to cause an allergic reaction than the iodinated contrast used for x-rays and CT scans.
- Your kidney function may be tested prior to the exam. This ensures that your kidneys are functioning adequately to filter out the MRI contrast. Our facilities use the level of MRI contrast that is the safest for your kidneys.
Use In Men Already Diagnosed With Prostate Cancer
The PSA test can also be useful if you have already been diagnosed with prostate cancer.
- In men just diagnosed with prostate cancer, the PSA level can be used together with physical exam results and tumor grade to help decide if other tests are needed.
- The PSA level is used to help determine the stage of your cancer. This can affect your treatment options, since some treatments are not likely to be helpful if the cancer has spread to other parts of the body.
- PSA tests are often an important part of determining how well treatment is working, as well as in watching for a possible recurrence of the cancer after treatment .
Don’t Miss: Is Beet Juice Good For Prostate
Understanding Your Mri Results
A doctor who specialises in imaging scans gives the MRI scan a score based on the results. This score helps your doctor decide on the next step and whether you need to have a biopsy. This is where your doctor takes a sample of your prostate gland.
This score is called the Likert or PI-RAD system. It estimates the risk that an area seen on the MRI scan may be a cancer or not. The score is from 1 to 5.
| Likert score | |
|---|---|
| Its highly unlikely that you have prostate cancer | |
| 2 | Its unlikely that you have prostate cancer |
| 3 | Its difficult to tell from the scan if a prostate cancer is present or not |
| 4 | Its likely that you have prostate cancer |
| 5 | Its very likely that you have prostate cancer |
Prostate Mpmri For Pc Detection And Localization
The first application of prostate MRI was published by Hricak et al. in 1983 . Since then, the field strength of MRI increased from 0.35 Tesla to 3T and standardized multiparametric sequences were established. MRI and TB detect more clinically significant PC compared to standard 12-core TRUS-biopsy . To establish a standardized MRI technique and a quantitative structured reporting system, the ESUR promoted the ESUR guidelines in 2012 . In 2015, a revised PIRADS version was published by the American College of Radiologists . The imaging techniques are described in the following sections.
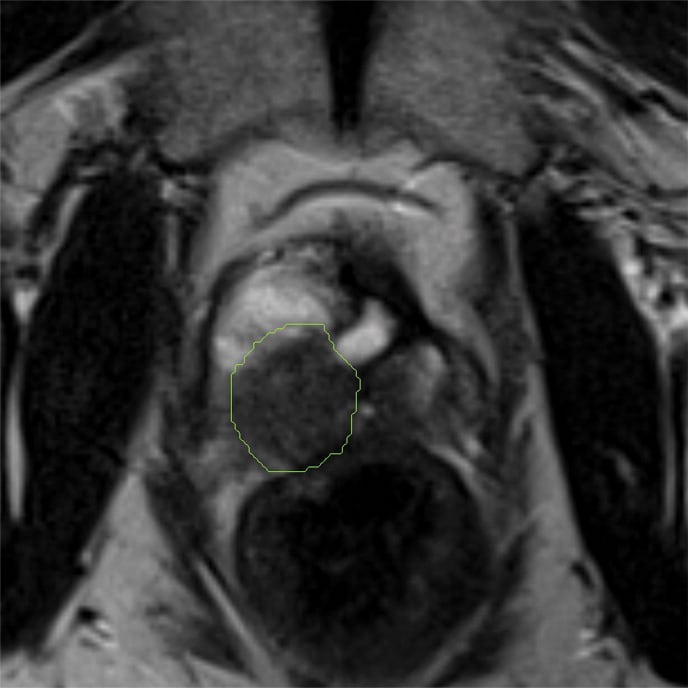
T2-weighted imaging
Figure 2et alet alTable 1
Diffusion-weighted imaging
Limitations of DWI include low signal-to-noise ratio and image distortion, both of which become more problematic at higher b values . Nonetheless, DWI is a widely available technique, and given its association with tumor aggressiveness, it may prove to be the primary sequence for tumor detection and characterization, especially in the peripheral zone, were it is recommended as the dominant sequence .
Dynamic contrast-enhanced imaging and role of biparametric MRI
You May Like: What Is An Enlarged Prostate Mean
The Current And Future Role Of Magnetic Resonance Imaging In Prostate Cancer Detection And Management
1 Department of Urology, Heidelberg University Hospital, Heidelberg, Germany Department of Radiology, German Cancer Research Center, Heidelberg, Germany
Correspondence to:
Purpose: Accurate detection of clinically significant prostate cancer and correct risk attribution are essential to individually counsel men with PC. Multiparametric MRI facilitates correct localization of index lesions within the prostate and MRI-targeted prostate biopsy helps to avoid the shortcomings of conventional biopsy such as false-negative results or underdiagnosis of aggressive PC. In this review we summarize the different sequences of mpMRI, characterize the possibilities of incorporating MRI in the biopsy workflow and outline the performance of targeted and systematic cores in significant cancer detection. Furthermore, we outline the potential of MRI in patients undergoing active surveillance and in the pre-operative setting.
Materials and methods: An electronic MEDLINE/PubMed search up to February 2015 was performed. English language articles were reviewed for inclusion ability and data were extracted, analyzed and summarized.
mpMRI and targeted biopsies are able to detect significant PC accurately and mitigate insignificant PC detection. As long as the negative predictive value is still imperfect, systematic cores should not be omitted for optimal staging of disease. The potential to correctly classify aggressiveness of disease in AS patients and to guide and plan prostatectomy is evolving.
Prostate Mri Can Help Differentiate Between Harmless And Aggressive Cancers Preventing The Overdiagnosis Of Low
There are two forms of prostate cancer: aggressive and harmless. Fortunately, out of all prostate cancer cases, only a fraction will be aggressive and clinically significant. The majority will never impact the well-being or life expectancy of a patient.
Prostate MRI can help reduce the number of men who are over-diagnosed by 5%.
A prostate MRI scan enables radiologists to better differentiate between aggressive and harmless cancers by providing information about a tumors size, density, and proximity to the bloodstream. One study comparing prostate MRI to biopsy found MRI scans to correctly diagnose 93% of tumors, whereas biopsy correctly diagnosed only 48%. Identifying non-threatening forms of prostate cancer helps decrease the risk of overdiagnosis and overtreatment.
But do keep in mind that MRIs can be complex images for radiologists to interpret. Coupling a prostate MRI with a subspecialty second opinion from a fellowship-trained radiologist can help maximize the advantages and efficacy of the screening. This can be done completely online and is especially recommended for scans that indicate the possibility of aggressive prostate cancer.
CONNECT WITH A SPECIALIST
Take Charge of Your Health
Get a second opinion from a radiology specialist in 3 easy steps.
Recommended Reading: Best Foods For Prostate Cancer Prevention
