Predictive Genetic Tests For Cancer Risk Genes
Cancer is not usually inherited, but some types mainly breast, ovarian, colorectal and prostate cancer can be strongly influenced by genes and can run in families.
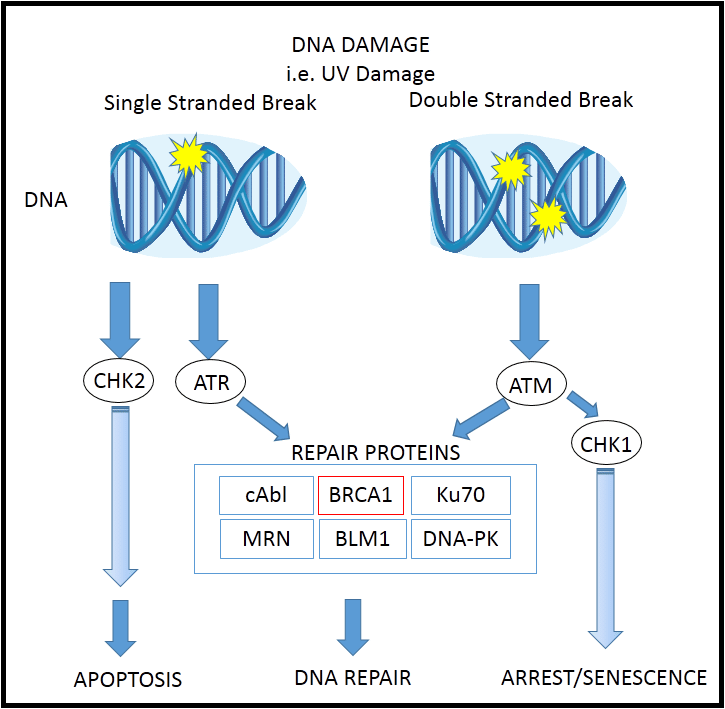
We all carry certain genes that are normally protective against cancer. These genes correct any DNA damage that naturally happens when cells divide.
Inheriting faulty versions or “variants” of these genes significantly raises your risk of developing cancer, because the altered genes cannot repair the damaged cells, which can build up and form a tumour.
BRCA1 and BRCA2 are examples of genes that raise your cancer risk if they become altered. Having a variant BRCA gene greatly increases a woman’s chance of developing breast cancer and ovarian cancer. They also increase a man’s chance of developing male breast cancer and prostate cancer.
BRCA genes are not the only cancer risk genes. Researchers recently identified more than 100 new gene variants associated with an increased risk of breast, prostate and ovarian cancer. Individually, these new gene variants only slightly increase the risk of cancer, but a combination could mean a high risk overall.
If you or your partner have a high-risk cancer gene, such as an altered version of BRCA1, it can be passed on to any children you have.
Lowering Risk Of Death
There are two different management approaches for people with BRCA2 mutations, both of which are designed to reduce the chance that a person will die from one of the cancers of risk:
- Early detection: Early detection is the process of trying to find a cancer which has formed at the earliest stage possible. With many cancers, we know that survival is higher when its found at an early stage than if it is discovered at a later stage . With early detection, the goal is to find cancer before it would otherwise cause the symptoms that would lead to its discovery. We dont have methods to detect all cancers at these early stages, and the tests we do have are not perfect. For example, despite having had a normal mammogram, some women are diagnosed with breast cancer shortly thereafter.
- Risk reduction: Risk reduction strategies work to reduce the risk that a cancer will develop in the first place. They are designed to prevent cancer from occurring. Methods of reduction may include surgery or medications .
Most approaches to a genetic predisposition to cancer include either screening or risk reduction, but there is one test that can do both. Colonoscopy can be used to detect colon cancer in the earliest stages. It can also be used to reduce the risk of a person getting cancer if a pre-cancerous polyp is found and removed before it becomes malignant.
What Are Brca1 And Brca2
BRCA1 and BRCA2 are genes that produce proteins that help repair damaged DNA. Everyone has two copies of each of these genesone copy inherited from each parent. BRCA1 and BRCA2 are sometimes called tumor suppressor genes because when they have certain changes, called harmful variants , cancer can develop.
People who inherit harmful variants in one of these genes have increased risks of several cancersmost notably breast and ovarian cancer, but also several additional types of cancer. People who have inherited a harmful variant in BRCA1 and BRCA2 also tend to develop cancer at younger ages than people who do not have such a variant.
A harmful variant in BRCA1 or BRCA2 can be inherited from either parent. Each child of a parent who carries any mutation in one of these genes has a 50% chance of inheriting the mutation. Inherited mutationsalso called germline mutations or variantsare present from birth in all cells in the body.
Even if someone has inherited a harmful variant in BRCA1 or BRCA2 from one parent, they would have inherited a normal copy of that gene from the other parent . But the normal copy can be lost or change in some cells in the body during that persons lifetime. Such a change is called a somatic alteration. Cells that dont have any functioning BRCA1 or BRCA2 proteins can grow out of control and become cancer.
Also Check: How Long Hormone Treatment For Prostate Cancer
Parp Inhibitors And Immune Checkpoint Inhibitors
There is also growing evidence into the synergy between PARP inhibitors and immune checkpoint inhibitors . The ligand programed death ligand-1 maintains an immunosuppressive tumor microenvironment and is activated in prostate cancer inhibition of PD-L1 may allow effective T-cell responses against tumor cells . Furthermore, PARP inhibition increases PD-L1 expression in cells with reduced BRCA2 expression . PD1 blockers, such as pembrolizumab and nivolumab, and PD-L1 blockers such as durvalumab, are being combined with PARP inhibitors in clinical trials . Karzai et al. showed efficacy of combining olaparib with durvalumab in mCRPC with 53% of patients having an over 50% decline in PSA, and median radiographic PFS in patients with DDR defects being 16.1 months compared to 4.8 months in patients without . There are ongoing trials investigating use of PARP inhibitors with immune checkpoint inhibitors in mCRPC .
Overall PARP inhibitors are a revolutionary treatment in the management of mCRPC in the era of targeted therapies with the future view of enabling personalized therapy with effective treatment results by determining prognostic and predictive factors as well as individual gene contributions . Several trials are in place to assess PARP inhibitor efficiency at different tumor stages as a monotherapy or polytherapy regime, and these will change the future of use of PARP inhibitors in years to come .
Testing For Gbrca In People With Cancer
Importance in Breast, Ovarian, Pancreatic, and Prostate Cancer
Testing for germline BRCA1/2 mutations, also known as gBRCA testing, is important in making treatment decisions for people with some types of cancer. While many people are familiar with genetic testing as a method to find people at risk for developing cancer in the first place, people who have recurrent or metastatic cancers of the breast, ovary, pancreas, or prostate may benefit from testing as a way to guide treatment choices as well.
For example, with metastatic breast cancer, the presence of a BRCA mutation might mean that a certain type of therapy is more likely to be effective or may suggest which type of chemotherapy will work best.
The importance of testing for gBRCA mutations in some metastatic cancers cannot be overemphasized. For example, gBRCA testing in metastatic breast cancer is considered a significant unmet need since there are now approved therapies for these tumors that traditionally carry a relatively poor prognosis. The situation is similar with some metastatic ovarian, prostate, and pancreatic cancers.
Testing for gBRCA is important not only in determining the risk of developing cancer, but in helping guide and predict the response to treatment for people living with some types of cancer.
You May Like: Best Treatment For Swollen Prostate
Atm And The Risks Of Radiotherapy
A study of prostate cancer patients with heterozygous ATM mutations found an increased risk of late complications of external beam radiotherapy,. Others have demonstrated that there is potential for increased therapeutic efficacy of radiotherapy among ATM carriers, but care must be taken to minimize radiation dose to prevent toxicity and second malignancies. At this time, the NCCN guidelines state that carrying a single ATM mutation should not lead to a recommendation to avoid radiation therapy. There is little evidence regarding late toxicity and second malignancy of radiotherapy for carriers of other germline mutations.
What Is A Mammogram
A mammogram is a low-dose X-ray procedure that produces images of the inside of the breasts. Mammography can detect some suspicious breast changes that are too small or too deep to be felt on breast examination.
A newer technology, called 3-dimensional mammography, or breast tomosynthesis, can be done as part of mammography screening. Although some studies have suggested that breast tomosynthesis may find more breast cancers and have fewer false positives than standard mammography, it remains unclear whether this is a better approach. All men should discuss this screening option in more detail with their doctor.
Typically beginning at 35 to 40, male BRCA mutation carriers should begin yearly clinical breast exams with a physician.
Don’t Miss: What Is Perineural Invasion In Prostate Cancer
What The Studies Showed
Clinical trial results showed the drugs were well-tolerated, with side effects similar to mild chemotherapy. Rucaparib was tested in a single-arm clinical trial , enrolling nearly 400 men with BRCA-positive metastatic prostate cancer who were no longer responding to other treatments. Results showed that tumors shrank in 44% of the enrolled subjects, in some cases for up to two years. Olaparib was tested in a similar population and delayed disease progression by an average of 7.4 months, which was just over two times longer than a type of hormonal therapy used in the control arm of that study.
Both drugs have their shortcomings. As personalized therapies, they work only for men with BRCA-positive prostate cancer, and just half the treated men will benefit. Furthermore, the experience with PARP-inhibitors so far is that tumors become resistant to therapy within six to 12 months. Whether PARP-inhibitors actually lengthen survival for men with metastatic prostate cancer is still being investigated. And many other questions remain about how to use the drugs most effectively to maximize their benefits.
Active Surveillance For Low
A historical overview of treatment outcomes of men with screen-detected, low-grade prostate cancer has led to the adoption of active surveillance for some low-risk prostate cancer patients. The choice of active surveillance relies on a combination of factors, including the PSA level, Grade group, clinical stage, and biopsy results . Active surveillance consists of PSA test every 36 months, digital rectal exam once per year, a confirmatory biopsy within 612 months, then serial biopsy a minimum of every 35 years thereafter with or without mpMRI. In the event of a rising PSA or grade progression active treatment is offered. Between 36% to 73% of patients will transition to treatment over 10 years but the development of metastatic disease is rare,.
Also Check: What Is Bad For Prostate Health
What About Early Prostate Cancer Screenings
If you’re aged 55 to 69, the U.S. Preventive Services Task Force suggests you talk to your doctor about prostate cancer screening. But if you have a BRCA1 or BRCA2 mutation, guidelines from the National Comprehensive Cancer Network guidelines recommend you think about prostate screenings by age 40.
Most people with prostate cancer live a long time. But the disease can be cured if you catch it before it spreads to other parts of your body.
Your doctor can check for signs of prostate cancer before you have symptoms. That usually includes a prostate-specific antigen blood test. Your prostate makes more PSA when you have prostate cancer. But other health problems can raise your PSA, including an infected or enlarged prostate.
Your doctor will go over the pros and cons of early PSA testing. Theyâll consider your overall health and any other risk factors.
According to the USPSTF, higher-risk groups include the following:
- Ages 55 or older
- Non-Hispanic Black people
- Those with a family history of prostate cancer
Risks of testing outweigh the benefits of screening for prostate cancer in the elderly , those who have major health problems, or those who expect to live less than 10 years.
Talk to your doctor about prostate cancer screenings if youâre in the gender-diverse community. Thereâs some evidence that transgender women who take gender-affirming hormone therapy have a lower risk of prostate cancer, but we need more research in this area.
Stabilization Of Stalled Forks
During replication stress, cells undergo arrest to allow time for repair and re-entry into the cell cycle . BRCA1 and BRCA2 are responsible for the protection of stalled replication forks . In the absence of BRCA1/2, nucleases such as MRE11 and MUS81 attack stalled replication forks, leading to fork collapse and chromosomal abnormality. PARP inhibitors sensitivity is affected by factors involved in recruiting these nucleases to the stalled replication fork, such as EZH2 and PTIP . The cytotoxicity of PARP inhibitors treatment results from fork degradation of deprotected replication forks in BRCA1 or BRCA2-mutated cells. There are at least three mechanisms that mediate fork degradation, and therefore loss of these mechanisms leads to protection of the fork and thereby PARP inhibitors resistance. The degradation is affected by factors involved directly or indirectly in fork remodelling and replication stress, such as chromatin-remodelers SMARCAL1, ZRANB3, HLTF, PTIP and SLFN11. The depletion of these factors will consequently lead to PARP inhibitors resistance .
Don’t Miss: Stage 4 Advanced Prostate Cancer Life Expectancy
What If A Man Reading This Article Has Already Been Diagnosed With Prostate Cancer But He Doesn’t Know His Brca Gene Status Is It Still Important For Him To Undergo Genetic Testing
CURRAN: At GBU, we think it’s important for two reasons. The first reason has to do with the previous point: if they have the BRCA gene mutation, they could have a more aggressive form of prostate cancer than a biopsy indicates.
The second reason involves treatment. We’ll likely treat a man with prostate cancer and who has the BRCA gene mutation differently from someone without the BRCA gene mutation. For example, we probably wouldn’t keep somebody with a BRCA gene mutation on active surveillance. And if they have advanced prostate cancer, there are different types of medical drug therapies that we can give the patients with BRCA gene mutations as opposed to the other prostate cancer patients.
Does A Germline Mutation Influence Prognosis
It is a central question whether or not the presence of a mutation predisposes men to more aggressive disease. There are several indicators of prostate cancer aggressivity that can be used in the evaluation. These include:
Mutation prevalence among men with metastatic disease versus localized disease.
It is important to ask if the prognosis of a man with an inherited pathogenic variant is influenced by the presence of the variant, independent of stage, grade and PSA level. It should also be noted that a pathogenic variant may not increase the risk of prostate cancer overall but may influence the probability of high-grade disease and prognosis to metastatic disease. Based on limited studies to date, it appears that men with BRCA2, ATM and PALB2 pathogenic variants face increased risks of progression and death that cannot be accounted for by traditional clinical parameters. Further work is needed in this area.
Don’t Miss: Beginning Signs Of Prostate Cancer
Can You Prevent Prostate Cancer
Most of the time, doctors dont know what causes prostate cancer. You cant always prevent prostate cancers, and some risk factors are out of your control.
Research is mixed about whether being overweight or consuming a very high calcium diet increases your risk of prostate cancer. According to the , the best preventative advice, for now, is to:
- get to and maintain a moderate weight
- stay physically active throughout your life
- eat a balanced diet that includes lots of fruits and vegetables
Genes Linked To Prostate Cancer
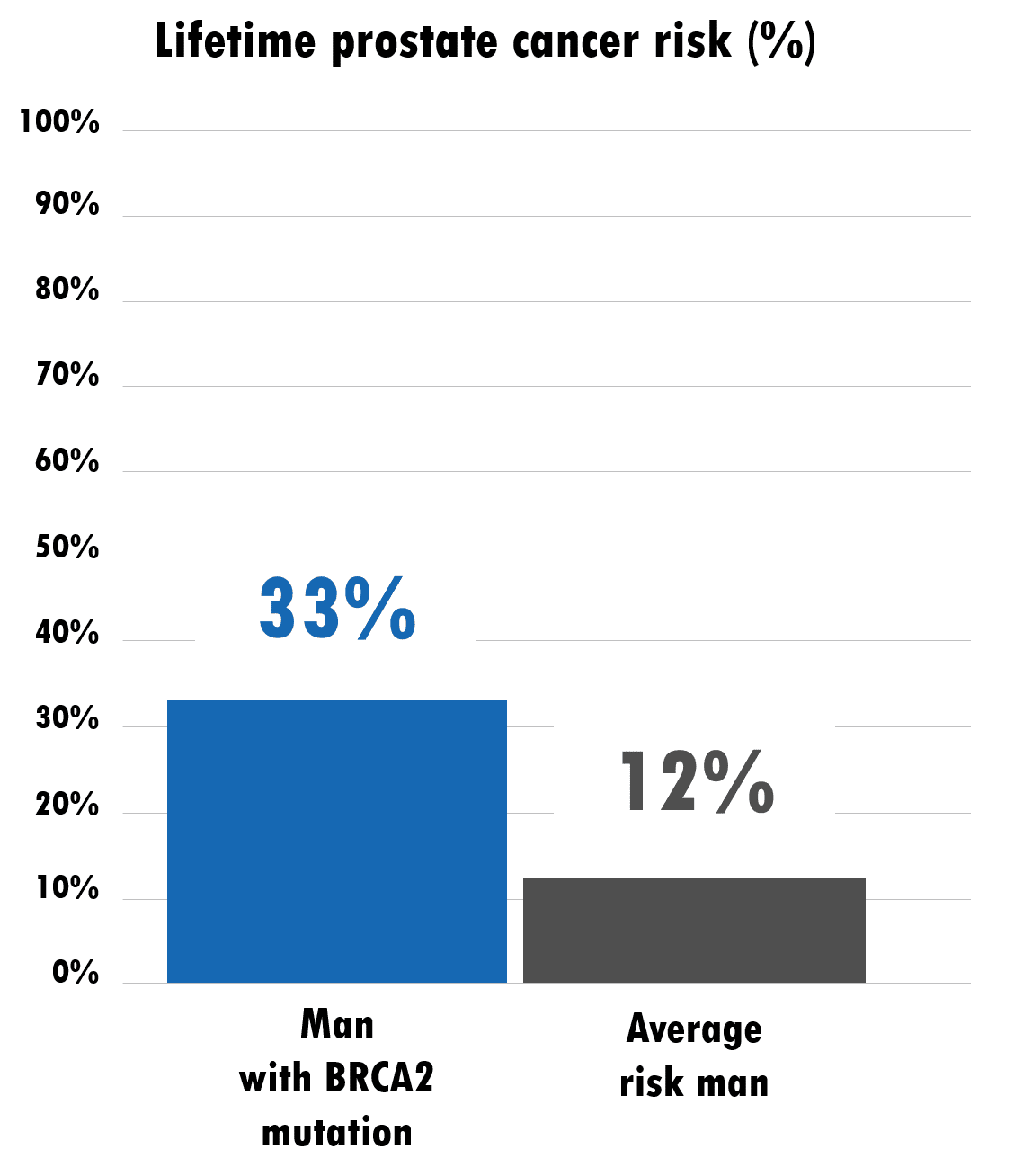
The odds of a man developing prostate cancer in his life is about 11%, but certain mutations like those in the BRCA2 and HOXB13 genes can potentially raise your risk by as much as
15% of men with stage IV prostate cancer have mutations in the genes BRCA1 or BRCA2, whereas, only about 5% to 7% of men with early stage prostate cancer carry these mutations. BRCA2 mutations are thought to increase your risk of prostate cancer eight times while BRCA1 mutations are thought to increase your risk three times.
Mutations in BRCA genes are seen in about people in the general population but as many as 1 in 40 people of Ashkenazi Jewish ancestry.
According to the authors of a published in the American Cancer Society Journals, analysis of the ongoing IMPACT clinical trial has found evidence that people carrying BRCA2:
- have a high incidence of prostate cancer
- receive a diagnosis at a younger age
- are more likely to have advanced disease at the time of diagnosis
Don’t Miss: How Successful Is Hormone Therapy For Prostate Cancer
Frequency Of Germline Mutations In Men With Prostate Cancer
While germline mutations in genes that predisposes to prostate cancer have relatively low mutation prevalence individually, together they account for a significant proportion of prostate cancer cases. The prevalence depends on the population studied and the number of genes surveyed. In a cohort of 53,105 men with no diagnosis of cancer , the frequency of DNA-repair gene mutations was 2.7%. Among 499 men with localized prostate cancer in the Cancer Genome Atlas Research Network the frequency of germline mutations was 4.6%. In a recent study of localized prostate cancer, 4% of men with European ancestry carried a DNA repair gene mutation compared 2.8% of unaffected controls. Of 351 men with African ancestry and localized prostate cancer, 1.4% had a mutation. It is important to note that this study excluded men who later progressed to metastatic disease.
The prevalence rates are higher than this in men with metastatic disease and/or a family history of prostate cancer. In a study of 692 men with metastatic prostate cancer, 82 men were found to carry a mutation in one of 16 cancer susceptibility genes,, . The frequencies of mutations in ATM and BRCA1 and BRCA2 were compared in 313 men who died of prostate cancer and 486 men with localized prostate cancer. The mutation rate was much higher among those with lethal prostate cancer . For those who died below age 60, 10% carried a mutation. Of those who died within five years of diagnosis 12.3% carried a mutation.
Targeting Brca Mutations In Prostate Cancer
1.3.1. Platinum Agents
Platinum-based chemotherapy, alkylating DNA, induces genomic strand breaks that may be translated in a synthetic lethality in tumor cells with DDR mutation. Carboplatin is a standard treatment for BRCA1/2 patients in breast . and ovarian cancer . Satraplatin provided a significant reduction in the risk of progression or death in a randomized phase 3 trial that enrolled unselected mCRPC patients who had progressed to prior taxane . However, this benefit did not translate in OS advantage compared to placebo .
Retrospective series and case reports also described the potential efficacy of platinum-based chemotherapy in mCRPC patients harboring gBRCA2 mutations . A retrospective study carried out at Dana-Farber Institute assessed the activity of carboplatin AUC 3â5 and docetaxel 60â75mg/mq in 141 mCRPC patients who were previously progressed to standard therapies . The combo significantly improved the rate of PSA decline in 6 out of 8 BRCA2 carriers compared to 23 out of 133 noncarriers , and improved OS was also observed .
Several ongoing trials are evaluating the efficacy of platinum-based chemotherapy in mCRPC patients selected for DDR mutations .
1.3.2. PARP Inhibitors
DDR defects cause the accumulation of genomic mutations in cancer cells, eventually leading to their proliferation, immortalization, and acquisition of an aggressive phenotype .
Read Also: How Do You Know If You Have An Enlarged Prostate
