Addition Of Hormone Therapy To Radiotherapy Benefits Men With Localized Prostate Cancer
Disclosures: We were unable to process your request. Please try again later. If you continue to have this issue please contact .
The addition of androgen deprivation therapy to radiotherapy improved survival outcomes among patients with localized prostate cancer, according to study results published in TheLancet Oncology.
Additionally, prolonging the adjuvant component of ADT provided significant benefit regardless of radiotherapy dose among those with intermediate-risk and high-risk disease, researchers noted.
Lancet Oncol
Rationale
Prostate cancer is an extremely common cancer worldwide that has been studied in multiple randomized trials. Yet, to date there has been no prior effort to pool data from multiple global trials to quantify the benefits we see from common treatment intensification strategies,Amar U. Kishan, MD, associate professor and vice-chair of clinical and translational research, and chief of the genitourinary oncology service for the department of radiation oncology at David Geffen School of Medicine at UCLA and UCLA Jonsson Comprehensive Cancer Center, told Healio.
These benefits include the addition of ADT to radiotherapy, prolonging the duration of ADT that follows radiotherapy , and extending the duration of ADT that may precede radiotherapy , Kishan added.
Methodology
Metastasis-free survival served as the studys primary outcome. Median follow-up was 11.4 years.
Key findings
Also Check: Symptoms Of Infected Prostate Gland
If Youre Having Radiation Therapy To The Pelvis
Radiation therapy to the pelvis can cause side effects such as:
- Bladder problems
- Fertility problems
- Changes in your sex life
You might also have some of the same problems people get from radiation to the abdomen, such as nausea, vomiting, diarrhea, or constipation.
Bladder problems
Radiation to the pelvis can cause problems with urination, including:
- Pain or burning sensations
- Blood in the urine
- An urge to urinate often
Most of these problems get better over time, but radiation therapy can cause longer-term side effects as well:
Factors That May Influence Treatment Decision
The drug mechanism of action, the route of administration, the duration of treatment, the impact on quality of life and the toxicity profile are important factors to consider when selecting a therapy for a particular patient, as they are quite different among the various strategies . Docetaxel has a major incidence of myelo-suppression with potential neutropenia, fatigue and neurotoxicity. Abiraterone is associated with mineralocorticoid-associated side effects including hypertension, hypokalemia and hepatic toxicity. Enzalutamide frequently causes fatigue, hypertension and falls. Apalutamide is associated with increased risk of rash, pruritus, hot flushes, hypothyroidism and fractures. Radiotherapy to the primary tumor can cause acute and late bladder and bowel toxic effects that can remarkably affect the quality of life .
In terms of costs, docetaxel in combination with ADT is likely to be the most cost-effective treatment option for patients with mHSPC . Docetaxel is administered every 21 days for six cycles at an approximate cost of $550 per cycle, whereas novel ARSi are prescribed as a daily dosing schedule until the time of progression at an approximate cost that exceeds $7000 per month . To administer lower dosages of ARSi might be an opportunity to reduce toxicities and costs, but phase 3 non-inferiority trials are still needed .
Don’t Miss: Can You Live Without A Prostate
Mental And Emotional Health
A cancer diagnosis and cancer treatment may affect how you feel mentally and emotionally. Hormone therapy can cause:
- A drop in mental sharpness
If you have any of these side effects, your doctor may recommend medication, counseling, or both.
Research shows that hormone therapy for prostate cancer may lead to problems with short-term memory, language, thinking, and concentration. But these problems are usually mild. Researchers are still studying the effect of hormone therapy on the brain.
When you stop taking hormone therapy, emotional and mental side effects usually disappear. But if youâve taken the drugs for many years, they may not fully go away.
Show Sources
You May Like: Polaris Test For Prostate Cancer
Side Effects Of Hormonal Therapy
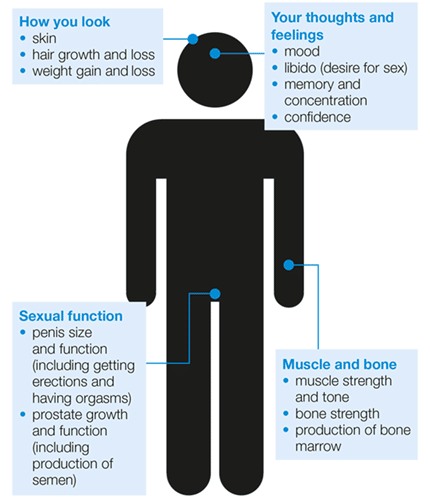
Side effects can happen with any type of treatment for cancer, but everyones experience is different. Some people have many side effects. Other people have few or none at all.
If you develop side effects, they can happen any time during, immediately after or a few days or weeks after hormonal therapy. Sometimes late side effects develop months or years after hormonal therapy. Most side effects go away on their own or can be treated, but some side effects may last a long time or become permanent.
Side effects of hormonal therapy will depend mainly on the type of hormonal therapy, the dose of a drug or combination of drugs and your overall health.
It is important to report side effects and your concerns about side effects to the healthcare team. Doctors may measure how severe certain side effects are. Sometimes hormonal drug therapy may need to be adjusted if side effects are severe.
The following are the most common side effects that people tend to experience with hormonal therapy.
Also Check: Why Incontinence After Prostate Surgery
How Often And For How Long Will I Need Hormone Therapy
How often you have hormone therapy will depend on the type of drug you are receiving and the type of cancer treated. Some medications need to be administered monthly, while others dont have to be administered quite as frequently.
In regards to how long hormone therapy will last, this will vary based upon the type of cancer you have and how well you are responding to treatment. For some people, it could continue for a few months. However, it is normal to need to continue with hormone therapy for several years. A common example is women undergoing hormone therapy for breast cancer it is normal to continue with treatment for five to seven years.
When Hormone Therapy Is Recommended
Hormone therapy is typically given to patients with intermediate- or high-risk prostate cancer. It may be used in the following ways:
- In combination with radiation, mostly for patients with high Gleason scores or other high-risk factors.
- After radiation or surgery when PSA rises, indicating a recurrence.
- As therapy for patients unsuitable for radiation or surgery.
- As therapy for metastatic prostate cancer . It may be given instead of or in combination with chemotherapy.
HT is usually not prescribed for:
- Patients choosing a localized treatment for low-risk prostate cancer
- Low-risk patients preferring to monitor their cancer on an active surveillance program
HT may be an option for patients who are not candidates for surgery, radiation or other localized treatment because of age, pre-existing health conditions or concerns about potential side effects of localized treatments.
Read Also: What An Enlarged Prostate Feels Like
T Cell In Oc Development
T cells have a dual role in OC development.
- T cells as foes in OC development
- T cells as friends in OC development
On the one hand, T cells can kill cancer cells through antibody dependent cellular cytotoxicity . ADCC occurs when CD16 is present on T cells. CD16 binds to the Fc region of IgGs, which is another T cell target recognition method besides TRAIL and FasL. Binding to target cells may trigger cytotoxicity or other effector functions . The researchers cloned the extracellular domain of V9 V2 T cell receptor from tumor infiltrating lymphocyte in OC and combined it with the Fc domain of human IgG1. This chimeric antibody mediates cell killing through ADCC in a dose-dependent manner. In vivo, this TCR V9 V2-Fc significantly inhibits cancer cell growth and improves survival rate in a human OC xenograft model.
On the other hand, T17 cells are the main source of IL-17 and play an immunosuppressive effect in tumors. T17 cells secrete IL-17, which induces the production of vascular endothelial growth factor and other angiogenesis-related factors. Studies have shown that the OC microenvironment may mobilize and recruit T cells, which secrete large amounts of inflammatory cytokine IL-17A, which reduces cytotoxicity, enhances immunosuppressive activity, establishes an effective immunosuppressive microenvironment, and promotes tumor progression and immune escape.
Fig.1 Antitumor and protumor functions of T cells.
Treatment Vs Side Effects
Prostate cancer treatment side effects can vary greatly from little to none, or create lifetime issues. Studying what treatments cause what side effects should be part of your treatment decision. Consenting to treatment means you understand the nature of the treatment, risks, benefits and alternatives.
Treatment or the combination of treatments in advanced cases can lead to a wide range of side effects. Prostate cancer treatment side effects include erectile dysfunction, incontinence, urinary issues, diarrhea, hot flashes, weight gain, loss of muscle, vomiting and hair loss. There are short term prostate cancer treatment side effects that subside over time, as well as long term side effects that can last for years. Question your Doctor about the side effects of the treatment you have selected. Make an informed decision.
Prostate cancer treatment side effects can vary greatly from little to none, or create lifetime issues. Studying what treatments cause what side effects should be part of your treatment decision. Consenting to treatment means you understand the nature of the treatment, risks, benefits and alternatives.
You May Like: How Long To Recover From Prostate Cancer Surgery
How To Not Get Picked For Grand Jury Duty Reddit
According to an article published in the Journal of Clinical Oncology, the timing of initiation of androgen deprivation therapy for the treatment of early-stage prostate cancer should be individualized, with each patient weighing individual side effects against outcomes.. Besides skin cancer, prostate cancer is the most commonly diagnosed cancer in men in the U.S. Anemia is when your bodys level of red blood cells goes below normal. When you do not have enough red blood cells, your body parts do not get enough oxygen. As a result, they cannot work the way they should and cause problems.You can develop anemia if your body does not make enough red blood cells or destroys them. You can also develop anemia if you lose too much.
Risk Factors In Phase 3 Trials
The CHAARTED and GETUG-AFU 15 trials assessed the role of upfront docetaxel plus ADT versus ADT alone in patients with mHSPC . The prospective stratification of high-volume versus low-volume metastatic disease was introduced for the first time as an amendment to the protocol of the CHAARTED trial . Given the uncertain role of chemotherapy in low-volume disease , several subsequent trials in mHSPC have analyzed patients outcomes based on disease burden . Different from the CHAARTED trial, the LATITUDE trial of abiraterone acetate in mHSPC used another classification to define high-risk patients, which was based on the presence of two or more high risk features that included 3 bone metastases, visceral metastases and Gleason 8 . A recent meta-analysis of the aggregate data of patient subgroups from the CHAARTED and GETUG-AFU15 studies evaluated overall survival according to the metastatic tumor burden and time of metastasis occurrence . The authors identified three prognostic subgroups: good prognosis for those with prior local treatment and low-volume disease intermediate prognosis for those with prior local treatment and high-volume disease, or those with low-volume disease and de novo metastases and poor prognosis for those with de novo high-volume disease. These data were recently confirmed by a retrospective cohort of 436 consecutive patients with mHSPC treated with ADT at the Dana-Farber Cancer Institute between 1990 and 2013 .
Don’t Miss: How Do You Do A Prostate Exam
What Is Intermittent Adt
Researchers have investigated whether a technique called intermittent androgen deprivation can delay the development of hormone resistance. With intermittent androgen deprivation, hormone therapy is given in cycles with breaks between drug administrations, rather than continuously. An additional potential benefit of this approach is that the temporary break from the side effects of hormone therapy may improve a mans quality of life.
Randomized clinical trials have shown similar overall survival with continuous ADT or intermittent ADT among men with metastatic or recurrent prostate cancer, with a reduction in some side effects for intermittent ADT .
Will I Need To See My Doctor During And After Hormone Therapy
 Niruja HealthTech” alt=”Side Effects of Hormone Therapy > Niruja HealthTech”>
Niruja HealthTech” alt=”Side Effects of Hormone Therapy > Niruja HealthTech”> Yes, you will need regular medical checkups while getting hormone therapy. During these checkups your doctor will look at your medical history and give you a physical exam. Your checkup may include blood tests and imaging tests. For example:
Imaging studies are ways used by doctors to take pictures of the inside of your body, such as x-rays or a CT Scan . These check-ups are important because:
Read Also: How To Properly Use A Prostate Massager
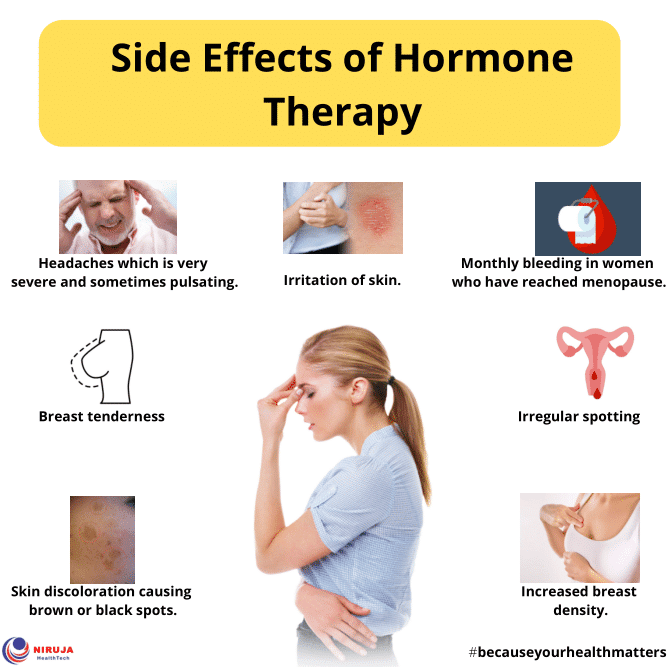
Hormone Therapy Side Effects
Testosterone is the primary male hormone, and plays an important role in establishing and maintaining typical male characteristics, such as body hair growth, muscle mass, sexual desire, and erectile function, and contributes to a host of other normal physiologic processes in the body. The primary systemic …
Staging Of Prostate Cancer
Doctors will use the results of your prostate examination, biopsy and scans to identify the stage of your prostate cancer .
The stage of the cancer will determine which types of treatments will be necessary.
If prostate cancer is diagnosed at an early stage, the chances of survival are generally good.
Read Also: How Long Does It Take To Get Over Prostate Surgery
Options In Hormone Therapy
Testosterone levels in the body can be reduced either surgically or with drugs. The surgical option is castration, achieved by removing the testicles during a bilateral orchiectomy. Once the only option, it has since been supplanted by drugs that lower testosterone levels to amounts achieved by surgery.
For men, normal testosterone levels range from 300 to 1,000 ng/dl. The FDA requires that any new drug used in hormone therapy for prostate cancer lower testosterone levels to 50 ng/dl or less. In my practice, I usually try to lower levels even further, to 20 ng/dl.
Recommended Reading: Johns Hopkins Prostate Cancer Second Opinion
What Side Effects May I Have After I Start Hormone Therapy
The side effects that you may have after you start hormone therapy include: erectile dysfunction or impotence , lower sexual desire , hot flashes, fatigue , weight gain, breast enlargement, osteoporosis, anemia, memory loss, and cardiovascular problems. The following side effects can happen as soon as you start your treatment.
Erection problems
Difficulty getting or keeping an erection is a common side effect of hormone therapy for prostate cancer. This is also called impotence. Hormone therapy lowers the amount of testosterone in your body or stops your body from making testosterone.
Lower sex drive
Hot flashes and sweating
Breast tenderness or growth
Some men may find that their chest becomes sore and that their breasts get a little bit swollen. This is called gynecomastia . There are medicines and treatments that you doctor or health care team can give you to help with this side effect.
Fatigue
The drop in your testosterone level may make you feel very tired. You may feel tired all the time or you may get tired more easily when you do your daily activities. This is known as fatigue or tiredness. There are things you can do to help deal with this treatment side effect.
Tumor flare pain
The following side effects may happen if you take hormone treatment for a long period of time. These are:
Weight gain
Memory problems
Anemia
Bone thinning
There are several ways you can help to lower your osteoporosis risk
Cardiovascular problems
Don’t Miss: What Age To Check Prostate
Dealing With Common Side Effects
Your treatment team can tell you about the side effects that are most common with your specific treatment and may be able to give you medicines to prevent or relieve side effects or suggest other ways to manage side effects. For general advice, see the see the symptom management section.
Almost all men receiving hormone therapy experience hot flashes. Hot flashes may get better or even go away over time, but if hot flashes are a problem for you, ask your doctor about medications or alternative-medicine approaches to help alleviate them.
Hormone therapy lowers the level of both testosterone and estrogen, which maintains bone strength. Men who receive hormone therapy for prolonged periods may develop bone thinning, which can lead to osteoporosis and broken bones. Your doctor may follow the density of your bones using a DEXA scan during hormone therapy and, if appropriate, prescribe medications to prevent complications from osteoporosis. In addition, diet and exercise can help keep your bones strong.
Hormone therapy can decrease muscle mass and increase the percentage of body fat, increasing body weight overall. It can also increase your risk for heart attack, stroke, diabetes and high cholesterol. Talk with your doctor about how to modify your diet and what exercise is appropriate to prevent these complications or reduce your risk. Seattle Cancer Care Alliance also has nutrition services to help you optimize your nutritional health during and after treatment.
What Should Patients Know About Msks Approach To Treating Prostate Cancer
At MSK, we manage prostate cancer in a very comprehensive way, tailored to each patients disease. There is no one specific therapy that is best for everyone.
Our initial assessment includes a carefully evaluated biopsy and a very detailed MRI to show the location of the disease, the integrity or soundness of the capsule surrounding the prostate, and the amount of disease. We will often obtain next-generation imaging and do genomic testing. Then, based on that information and with input from the urologist, the radiation oncologist, and the medical oncologist we can provide a comprehensive recommendation.
The radiotherapy we do here at MSK is state-of-the-art and unparalleled. We are one of the few centers in the world to do MRI-based treatment planning and one of the few centers in the US to offer MRI-guided treatment. When we give brachytherapy, we use computer software that provides us with real-time information about the quality and accuracy of the seed implant during the procedure. It requires a great deal of collaboration with our medical physics team to try to get the most accurate positioning of the prostate during the actual three or four minutes of the treatment.
We make adjustments while the patient is still under anesthesia, so that when the procedure is completed, we have been able to achieve ideal placement of the radiation seeds. This translates into improved outcomes.
Recommended Reading: What Is The Best Food For Prostate Cancer
