How Do You Determine Whats Right For You
Whether youve recently been diagnosed with prostate cancer or youre dealing with recurrent or metastatic cancer, you may be facing difficult decisions about your treatment. Its normal to be unsure about what steps to take, and most patients have more than one choice.
Start by talking to your oncologist about the specifics of your case and your options. The American Society of Clinical Oncology has a helpful list of questions to ask your doctor about prostate cancer you may want to reference.
If possible, see a multi-specialty cancer care team to get a bigger picture of your case and your options. This is also important because, sometimes, factors outside of your cancer stage may impact your treatment options. For example, you may have an obstruction in your urinary tract that makes surgery a more appropriate choice than radiation. Or maybe you have another health condition that makes surgery more risky for you. In that case, radiation may be a better choice. You want these doctors to talk to one another about your case each has expertise that makes an important contribution to the decision-making process. To facilitate this coordination, you may have to set up appointments to see multiple doctors and ask them to discuss your case.
If youre interested in getting a second opinion for prostate cancer, or if youd just like to talk with someone at CTCA about your cancer care, or chat online with a member of our team.
Protons In Prostate Cancer
In prostate cancer the benefits are less clear. A big advantage of protons is the reduction in the total dose delivered to the patient. However, the main side effects associated with this are much less significant in adults: delays in development are not a factor, and the risk of additional cancers are much lower as they typically take decades to develop.
Instead, the main side effects are seen in organs close to the prostate that also receive a high dose, such as the bladder and rectum. A high dose must be delivered to a region that includes the prostate and some additional healthy tissues, to make sure the disease is treated fully. The extra margin allows for the variation that occurs during treatment, such as differences in the way the patient lies down, to make sure the cancer gets a full dose each day. As these patient variations are independent of the radiation type, protons and X-rays typically deliver similar high doses to these healthy tissues.
Despite this, proton therapy has been widely adopted because it is argued the physical benefits are clear, even if small, and will become apparent with time as more people reach the five and ten-year survival mark. But the results of studies investigating the effects of proton therapy on prostate cancer are mixed. While protons have been shown to an effective treatment for prostate cancer, no consistent advantage has been seen for either long-term survival or quality of life.
Safety And Efficacy Of Proton Therapy
Many people with locally advanced cancers are treated with a combination of chemotherapy and either traditional or proton radiation. For patients getting chemotherapy and radiation at the same time, finding ways to limit side effects without making the treatment less effective is a high priority, Dr. Baumann said.
He and his colleagues analyzed data from nearly 1,500 adults with 11 different types of cancer. All participants had received simultaneous chemotherapy plus radiation at the University of Pennsylvania Health System between 2011 and 2016 and had been followed to track side effects and cancer outcomes, including survival. Almost 400 had received proton therapy and the rest received traditional radiation.
Those who received proton therapy experienced far fewer serious side effects than those who received traditional radiation, the researchers found. Within 90 days of starting treatment, 45 patients in the proton therapy group and 301 patients in the traditional radiation group experienced a severe side effectthat is, an effect severe enough to warrant hospitalization.
In addition, proton therapy didnt affect peoples abilities to perform routine activities like housework as much as traditional radiation. Over the course of treatment, performance status scores were half as likely to decline for patients treated with proton therapy as for those who received traditional radiation.
You May Like: What Happens If You Have Your Prostate Removed
A Tailored Approach To Treating Prostate Cancer With Proton Therapy
Most proton centers treat prostate cancer with volumetric beams that deliver a fixed quantity of energy to the entire tumor and surrounding normal tissues. But the Pencil Beam Scanning technology available at the New York Proton Center uses intensity-modulated proton therapy, or IMPT.
IMPT is widely considered the most advanced form of proton therapy for prostate cancer. It delivers different radiation doses to different parts of the tumor based on its exact location, maximizing the chance of a cure while better protecting surrounding healthy tissue from radiation.
What Do We Think
For men with localised prostate cancer, current evidence suggests that proton beam therapy does not produce better outcomes than existing radiotherapy techniques. There is also limited evidence to suggest that it results in fewer side effects than radiotherapy. Because standard radiotherapy works just as well as, or better than proton beam therapy, it isnt used to treat prostate cancer in the UK.
Radiotherapy is a highly effective treatment for localised prostate cancer, enabling 98% of men with localised prostate cancer who receive conventional radiotherapy survive for at least 10 years. Men with this stage of the disease can also choose from a series of other treatment options that include active surveillance, radical prostatectomy and brachytherapy.
Unless further clinical trials are carried out to show that proton beam therapy will benefit men with prostate cancer through increased overall survival or the reduction of side effects, Prostate Cancer UK does not actively encourage men to pay for this treatment or seek it abroad.
If you have any concerns about prostate cancer or the treatment options for localised prostate cancer, you can confidentially contact our Specialist Nurses on 0800 074 8383.
i NHS England : Clinical Commissioning Policy: Proton Beam Therapy for Cancer of the Prostate. July 2016.
Read Also: Why Does Prostate Gland Swell
Potential Advantages And Disadvantages Of Pt
The potential advantages and disadvantages of PT result from its dosimetric features. Protons travel only a finite distance, proportional to their speed, which can be controlled during the acceleration process they deposit most of their energy at the end of their range in an area called the âBragg peakâ and, unlike photon-based radiation, there is no exit dose beyond the target. Additionally, the entrance dose is relatively low when compared to external-beam photon radiation. For many target locations, these features reduce the excess radiation dose delivered to surrounding organs and the number of beams needed to treat a target when compared to photon radiation . Multiple dosimetric comparisons have been performed evaluating the extent of the dosimetric improvements that PT offers for prostate cancer and, in general, they have shown that PT reduces the dose of excess radiation provided to OARs in the low-to-moderate range .
Figure 1
Nichols et al. retrospectively reviewed the medical records of 171 men treated with PT for localized prostate cancer and found that PT does not affect serum testosterone levels. PT provides less excess radiation dose to the testes when compared to photon-based radiation. Consequently, while photon-based radiation lowers testosterone by 9% to 27% on average, patients treated with PT can expect no changes in testosterone, which may reduce the risk for fatigue or sexual dysfunction after treatment .
Effect Of Dosage Schedules And Other Technological Factors On Patient Outcomes
Several clinical studies have examined whether dosage schedule , use of pencil beam modality, and total delivered dose influence outcomes. Hypofractionation has been examined in 2 small RCTs., The first RCT randomized 82 men to a moderate hypofractionated PBT dose schedule or an extreme hypofractionated schedule and compared long-term GI and GU toxicity and cancer control. The rates of GI and GU toxicity were slightly different between treatment arms, but these differences were not statistically significant. Cancer progression as measured by PSA levels was significantly higher in the extreme hypofractionation arm. The second RCT reported small and nonsignificant differences in GU and GI toxicity between patients on a hypofractionation schedule or conventional dosage schedule.
Pencil beam scanning is a newer technique that potentially can deliver more precise dosing in PBT, compared with conventional PBT. A multi-site registry study has enrolled patients receiving either PBS or conventional PBT and has reported data on toxicity rates for the 2 alternative modalities., Both acute and late GU toxicity were higher in the PBS group, while GI and sexual toxicity did not differ between the groups. The methods for controlling for confounding were limited in this study. Overall, the current evidence is insufficient to draw conclusions about the comparison of PBS to conventional PBT.
You May Like: Can Prostate Cancer Be Transmitted Sexually
Possible Risks And Side Effects Of Brachytherapy
Radiation precautions: If you get permanent brachytherapy, the seeds will give off small amounts of radiation for several weeks or months. Even though the radiation doesnt travel far, your doctor may advise you to stay away from pregnant women and small children during this time. If you plan on traveling, you might want to get a doctors note regarding your treatment, as low levels of radiation can sometimes be picked up by detection systems at airports.
There’s also a small risk that some of the seeds might move . You may be asked to strain your urine for the first week or so to catch any seeds that might come out. You may be asked to take other precautions as well, such as wearing a condom during sex. Be sure to follow any instructions your doctor gives you. There have also been reports of the seeds moving through the bloodstream to other parts of the body, such as the lungs. As far as doctors can tell, this is uncommon and doesnt seem to cause any ill effects.
These precautions arent needed after HDR brachytherapy, because the radiation doesnt stay in the body after treatment.
Bowel problems: Brachytherapy can sometimes irritate the rectum and cause a condition called radiation proctitis. Bowel problems such as rectal pain, burning, and/or diarrhea can occur, but serious long-term problems are uncommon.
What Are The Pros And Cons Of Proton Therapy For Cancer
The pros of proton therapy for cancer include that it is more accurate than alternative treatments and less likely to cause damage to surrounding tissues. Proton therapy also can be precisely targeted to the exact depth of the tumor, minimizing damage to other parts of the body. The treatment can cause the same side effects as other forms of radiation treatment, however, and also is expensive.
One of the main advantages of proton therapy is that it has a lower chance of causing severe side effects than other forms of therapy. This is because protons are larger and heavier than the particles used in other types of radiation therapy. The larger mass means the protons dont scatter into other parts of the body as much, reducing collateral damage to surrounding tissue.
It also is easier to target protons to tissue of a certain depth. If other types of radiation are used, such as X-rays, it is difficult to get the radiation to stop at the precise depth of the cancer. This means the radiation continues on and can affect other parts of the body. The energy of protons, on the other hand, can be adjusted so most cant penetrate any farther than required.
You May Like: How Bad Is Stage 3 Prostate Cancer
Proton Beam Therapy Compared To Imrt
Toxicity
Rates of moderate or severe toxicity symptoms varied across available studies. Early GI toxicity rates ranged from 4% to 17% among both IMRT and PBT patients, but the rates tended to be higher for IMRT patients in the 3 studies that reported on early toxicity. Rates of late GI toxicity ranged from 5% to 18%, and were lower among IMRT patients or comparable for IMRT and PBT groups . Rates of early GU toxicity ranged from 0 to 45% and were consistently higher among patients receiving IMRT. Rates of late GU toxicity ranged from 2% to 32%, and were higher among IMRT patients or comparable for both modalities .
No pooled estimate of GI or GU toxicity risk reached statistical significance. At 3 months after treatment initiation or completion, results from 3 studies suggest a possible lower risk of early GI toxicity and early GU toxicity after treatment with PBT compared with IMRT. The largest study reported a significant finding for GU toxicity. Observed toxicity risk and estimates of true risk in each study were consistent in direction , and all studies used a similar outcome definition .
Forest Plot of Toxicity Findings of Studies Comparing PBT to IMRT. Notes. Black diamonds indicate results of random-effects meta-analyses . Blue diamonds and error bars represent
Quality of Life and Survival
Incidence of Second Cancers
What Is Proton Beam Therapy
Proton beam therapy is a relatively new type of radiotherapy that uses tiny, high energy particles, so-called protons to target and kill cancer cells. It reduces the damage to surrounding healthy tissues and vital organs which is why certain groups of people such as young children or people whose cancer is close to vital organs benefit from the treatment. However, for other groups of patients or types of cancer, there has been little evidence of significantly improved treatment benefits, such as better cancer control and reduced side effects, than compared to conventional radiotherapy treatment.
You May Like: How Far Up The Rectum Is The Prostate
What Is Proton Therapy
Proton therapy, also known as proton beam therapy, is a radiation treatment that precisely delivers a beam of protons to disrupt and destroy tumor cells. Compared with traditional radiation, protons have unique properties that allow doctors to better target radiation to the size and shape of the tumor. The proton beam kills the tumor cells and spares more of the surrounding healthy tissue.
Radiation Therapy For Prostate Cancer

Radiation therapy uses high-energy rays or particles to kill cancer cells. Depending on the stage of the prostate cancer and other factors, radiation therapy might be used:
- As the first treatment for cancer that is still just in the prostate gland and is low grade. Cure rates for men with these types of cancers are about the same as those for men treated with radical prostatectomy.
- As part of the first treatment for cancers that have grown outside the prostate gland and into nearby tissues.
- If the cancer is not removed completely or comes back in the area of the prostate after surgery.
- If the cancer is advanced, to help keep the cancer under control for as long as possible and to help prevent or relieve symptoms.
Also Check: Are Almonds Good For Prostate Health
What Is The Recovery And Outlook After Proton Therapy
Most people return to their daily activities immediately following a proton therapy session. Many people see benefits from this procedure within 2-8 weeks. The tumors response to proton therapy depends on the type of cancer you have and its location within your body.
If you are diagnosed with cancer, ask your doctor about proton therapy as a possible treatment option. Your doctor will help you determine whether this treatment is a good option for you.
Last reviewed by a Cleveland Clinic medical professional on 05/26/2021.
References
Donât Miss: How Is The Prostate Removed In Robotic Surgery
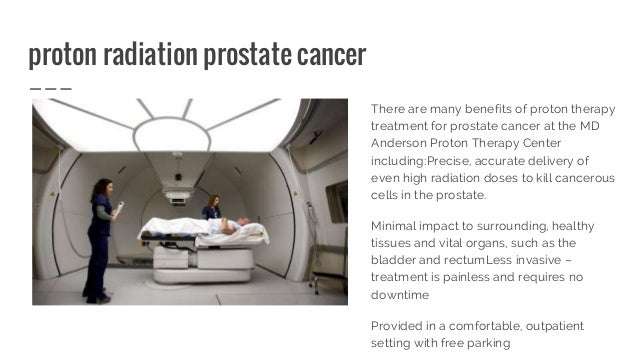
Proton Therapy Treatment For Prostate Cancer Patients
Proton therapy is a form of radiation treatment for cancer patients. Also called proton beam therapy, proton therapy involves focusing proton particles into a beam, which is then delivered to the cancer cells in a non-surgical procedure. The positively charged particles can be controlled to stop at the tumor site, enabling the cancerous tissues to be destroyed with high levels of radiation without causing damage to nearby healthy tissue and vital organs. Proton therapy is considered more precise than other types of radiation therapy. It is also non-surgical, non-invasive, and has minimal side effects. Proton therapy treatment requires little to no recovery time, and the radiation has very little impact on a patients energy level compared to other cancer treatment options.
Proton therapy exhibits higher success rates in prostate cancer patients.
According to a study published by the University of Florida, prostate cancer patients who received proton therapy treatment were found to be free of cancer progression for five years after their treatment. Patients with low to medium risk prostate cancer experienced a success rate of 99%, while those with high risk prostate cancer experienced a success rate of 76%.
Also Check: Why Does The Prostate Feel Good
Proton Therapy Versus Photon And Other Radiation Therapies
Unlike traditional photon radiation therapy that uses radiation in the form of X-rays or gamma rays, proton therapy uses proton particle radiation. Both photon and proton radiation damage the tumors DNA, but researchers say damage to the tumor cells caused by protons is more direct and harder to repair.
More importantly, protons only travel a certain distance into the body before they stop, and they deliver the highest dose of radiation at the end of their pathway. This burst of energy can appear on a graph as what is called the Bragg peak. Radiation oncologists plan proton therapy treatments so the maximum dose hits the tumor cells. In this way, proton therapy reduces radiation exposure and potential damage to healthy tissue, especially in sensitive areas such as the brain, eyes, spinal cord, heart, reproductive organs, major blood vessels and nerves.
In regular radiation therapy, such as photon therapy or gamma knife treatments, the beam of high-energy gamma rays or X-rays goes into the body, through the tumor and out the other side. Photons release energy along the entire path they travel, which means they radiate healthy tissues beyond the tumor. It is estimated that 30% to 40% of the photon dose passes through the tumor. This exit dose of radiation can damage the DNA of healthy cells. Proton therapy generates virtually no exit dose.
Proton Therapy | Targeted Cancer Treatment
