When You Need Themand When You Dont
It is normal to want to do everything you can to treat prostate cancer. But its not always a good idea to get all the tests that are available. You may not need them. And the risks from the tests may be greater than the benefits.
The information below explains why cancer experts usually do not recommend certain imaging tests if you are diagnosed with early-stage prostate cancer. You can use this information to talk about your options with your doctor and choose whats best for you.
How is prostate cancer usually found?
Prostate cancer is cancer in the male prostate gland. It usually grows slowly and does not have symptoms until it has spread. Most men are diagnosed in the early stages when their doctor does a rectal exam or a PSA blood test. PSA is a protein made in the prostate. High levels of PSA may indicate cancer in the prostate.
If one of these tests shows that you might have prostate cancer, you will be given more tests. These tests help your doctor find out if you actually have cancer and what stage your cancer is.
What are the stages of prostate cancer?
Prostate cancer is divided into stages one to four . Cancer stages tell how far the cancer has spread.
Stages I and II are considered early-stage prostate cancer. The cancer has not spread outside the prostate. However, stage II cancer may be more likely to spread over time than stage I cancer. In stages III and IV, the cancer has already spread to other parts of the body.
Imaging tests have risks.
09/2012
Ct Scanning Mri And Bone Scanning
Men with PSA levels above 10 ng/mL, high-grade histology , or physical findings that suggest stage T3 disease should probably undergo a staging computed tomography scan and bone scan. CT scanning is the one modality with evidence-based guidelines. The CT scan can be used to evaluate extension into the bladder and lymph nodes to help stage the patient’s cancer or to consider lymph node sampling prior to treatment.
According to the National Comprehensive Cancer Network , technetium-99m-methyl diphosphonate bone scan is indicated in the initial evaluation of patients at high risk for skeletal metastases, as indicated by any of the following :
- T1 disease, PSA 20
- Symptoms suggestive of osseous metastasis
The NCCN recommends pelvic CT or magnetic resonance imaging in patients with any of the following:
- T1-T2 disease and nomogram-indicated probability of lymph node involvement > 10%
Conventional endorectal MRI is helpful for localizing cancer within the prostate and seminal vesicles and for local staging. Dynamic, contrast-enhanced MRI and MR spectroscopic imaging are complementary in local staging, but their use is currently limited to a research setting.
- Detection of large and poorly differentiated tumors
- T staging: Detection of extracapsular extension, with high negative predictive values in low-risk men
- N staging: MpMRI is equivalent to CT scan
- M staging: MpMRI outperforms bone scan and targeted x-rays for M staging, with 98-100% sensitivity and specificity
What Does The Equipment Look Like
Ultrasound machines consist of a computer console, video monitor and an attached transducer. The transducer is a small hand-held device that resembles a microphone. Some exams may use different transducers during a single exam. The transducer sends out inaudible, high-frequency sound waves into the body and listens for the returning echoes. The same principles apply to sonar used by boats and submarines.
The technologist applies a small amount of gel to the area under examination and places the transducer there. The gel allows sound waves to travel back and forth between the transducer and the area under examination. The ultrasound image is immediately visible on a video monitor. The computer creates the image based on the loudness , pitch , and time it takes for the ultrasound signal to return to the transducer. It also considers what type of body structure and/or tissue the sound is traveling through.
For ultrasound procedures such as transrectal exams that require insertion of an imaging probe, also called a transducer, the device is covered and lubricated with a gel.
Don’t Miss: What Are The 5 Early Signs Of Prostate Cancer
How The Prostate Changes As You Age
Because the prostate gland tends to grow larger with age, it may squeeze the urethra and cause problems in passing urine. Sometimes men in their 30s and 40s may begin to have these urinary symptoms and need medical attention. For others, symptoms aren’t noticed until much later in life. An infection or a tumor can also make the prostate larger. Be sure to tell your doctor if you have any of the urinary symptoms listed below.
Tell your doctor if you have these urinary symptoms:
- Are passing urine more during the day
- Have an urgent need to pass urine
- Have less urine flow
- Feel burning when you pass urine
- Need to get up many times during the night to pass urine
Growing older raises your risk of prostate problems. The three most common prostate problems are inflammation , enlarged prostate , and prostate cancer.
One change does not lead to another. For example, having prostatitis or an enlarged prostate does not increase your risk of prostate cancer. It is also possible for you to have more than one condition at the same time.
Tests Used To Check The Prostate
This first step lets your doctor hear and understand the “story” of your prostate concerns. You’ll be asked whether you have symptoms, how long you’ve had them, and how much they affect your lifestyle. Your personal medical history also includes any risk factors, pain, fever, or trouble passing urine. You may be asked to give a urine sample for testing.
Also Check: Where Is Your Prostate Diagram
How Can I Clean My Prostate
10 diet & exercise tips for prostate health
What Does Heterogenous Echostructure In Ultrasound Mean
My prostate volume is 44 ml with heterogenous echostructure in ultrasound what that means?
Doctor’s Assistant: Is the condition chronic, or acute?
All the signs and symptoms started appearing one month ago
Doctor’s Assistant: Anything else in your medical history you think the doctor should know?
Only urinary urgency is very old but without any other problem
Recommended Reading: What Does A Swollen Prostate Feel Like
Somatic Mutations Of Spop Foxa1 And Idh
Somatic point mutations in SPOP were found in six cancer samples from five foci in five patients. Eight samples from seven foci in six patients had point mutations in FOXA1. The same mutation in IDH1 was identified in two samples from one focus within a single patient . All mutations were validated by Sanger sequencing .
Imaging Of Nodal Metastases At Initial Staging
The probability for LN metastases at initial diagnosis of localized PCa is associated with risk classification very low risk and low-risk patients have an exceedingly low probability for LN metastasis . Accurate assessment of LN status helps in therapeutic decision making, prediction of recurrence risk, and assessment of prognosis.
The presence of LN metastasis is an independent risk factor for BCR , and there is great interest in preoperative imaging-based identification of LN metastases to optimize surgical and adjuvant or neoadjuvant treatment planning. Currently, the clinical practice and urologic guidelines primarily rely on validated clinical nomograms to help guide decision making for pelvic lymph node dissection, with a calculated estimated risk of more than 5% being an indication to perform extended pelvic lymph node dissection . Even though pelvic lymph node dissection is the traditional gold standard for LN staging, it is an invasive, time-consuming approach largely dependent on surgical skill and templates.
As of yet, no single imaging modality has shown optimal diagnostic performance in the assessment of metastatic LNs. Studies with the PET tracers 18F-choline, 11C-choline, and 18F-fluciclovine reported similar high specificities but low sensitivities ranging from 40% to 50% .
You May Like: How To Properly Milk Prostate
What Customers Are Saying:
I feel so much better today, and upon further investigation believe that there is a chance that the responses I got saved me from a serious, even life threatening situation. I am very grateful to the experts who answered me.
Susan O.USA
I can go as far as to say it could have resulted in saving my sons life and our entire family now knows what bipolar is and how to assist and understand my most wonderful son, brother and friend to all who loves him dearly.Thank you very much
Corrie MollPretoria, South Africa
I thank-you so much! It really helped to have this information andconfirmation. We will watch her carefully and get her in for theexamination and US right away if things do not improve. God bless you aswell!
ClaudiaAlbuquerque, NM
Outstanding response time less than 6 minutes. Answered the question professionally and with a great deal of compassion.
KevinBeaverton, OR
Suggested diagnosis was what I hoped and will take this info to my doctor’s appointment next week.I feel better already! Thank you.
ElanorTracy, CA
Thank you to the Physician who answered my question today. The answer was far more informative than what I got from the Physicians I saw in person for my problem.
JulieLockesburg, AR
You have been more help than you know. I seriously don’t know what my sisters situation would be today if you had not gone above and beyond just answering my questions.
John and StefanieTucson, AZ
Citation Doi & Article Data
Citation:DOI:Dr Marcin CzarnieckiRevisions:see full revision historySystems:
- Prostate Imaging Reporting and Data System version 2.1
- PI-RADS version 2.1
- Prostate Imaging Reporting and Data System
PI-RADS is a structured reporting scheme for multiparametric prostate MRI in the evaluation of suspected prostate cancer in treatment naive prostate glands. This article reflects version 2.1 , published in 2019 and developed by an internationally representative group involving the American College of Radiology , European Society of Urogenital Radiology , and AdMeTech Foundation 6.
You May Like: Brca Gene And Prostate Cancer
Imaging Of The Primary Prostate Tumor
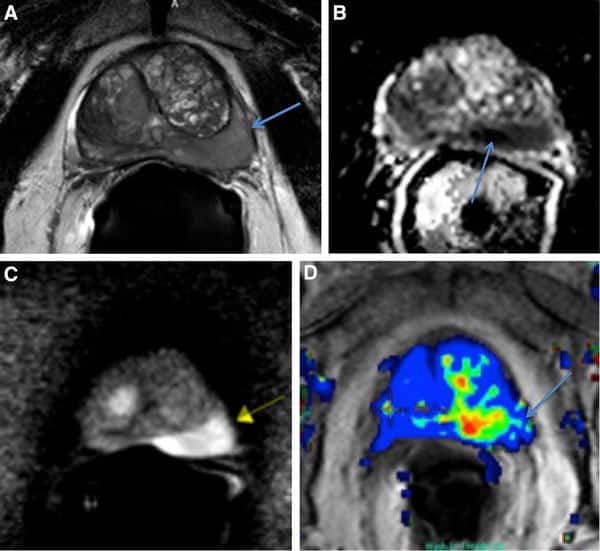
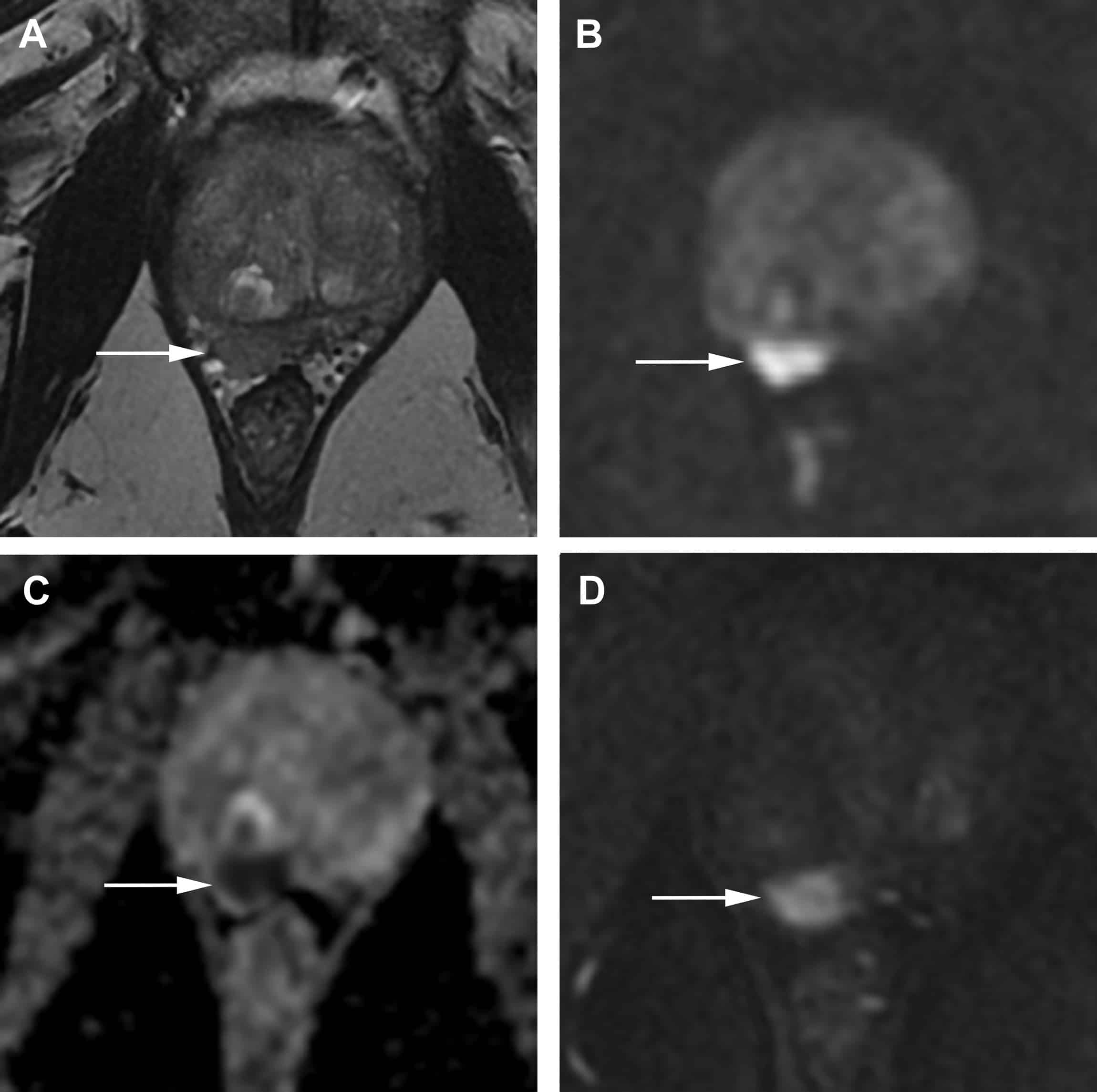
Because of its superb soft-tissue resolution, MRI has established itself as the modality of choice for the assessment of primary prostate tumors and has been applied in clinical practice for over 3 decades. During most of this time, it was predominantly used in tertiary academic centers with special interest and expertise, but most recently its adoption has been more widespread, partly because of the introduction of PI-RADS in 2012 and the updated version 2 in 2015 and version 2.1 in 2019 . PI-RADS standardized image acquisition and reporting, with assessments based on the appearance of lesions on T2-weighted imaging, diffusion-weighted/apparent diffusion coefficient imaging, and, as an ancillary adjunct, dynamic contrast-enhanced imaging. Prostate tumors typically demonstrate homogeneously low T2 signal intensity, diffusion restriction, and early enhancement . Per-lesion assessment categories are assigned, ranging from 15 and reflecting the likelihood of clinically significant PCa. Thus, PI-RADS 1 suggests a very low probability of clinically significant cancer whereas PI-RADS 5 suggests a very high probability. PI-RADS 3 defines an intermediate probability.
Two landmark papers providing level 1 evidence for the incremental benefit of mpMRI have substantiated the strength of MRI in the detection of clinically significant PCa, that is, the PROMIS and PRECISION trials .
Patient Cohort And Fresh
The total cohort consisted of 571 prostate cancer patients who underwent prostatectomies between 2010 and 2012 at Oslo University Hospital-Radiumhospitalet. Ethical approval for the study was obtained from the regional Ethics Committee South-East Norway . All included patients had acinar adenocarcinomas and informed consent was obtained from all patients before initiation of the study. All methods were performed according to the relevant guidelines and regulations. From this cohort, 39 patients with fresh-frozen cancer samples from at least two clearly distinct cancer foci were selected for this study. From each patient, samples from two or three distinct cancer foci and one corresponding benign tissue sample were included. In total, the sample set consisted of 145 cancer and benign samples representing 85 distinct cancer foci.
From each prostatectomy, three to seven tissue cores with diameter of 6mm were biobanked . The holes were marked and the sections and orientation photographed. Both cancer and benign samples were selected by a pathologist, based on microscopy of hematoxylin and eosin stained sections through formalin-fixed and paraffin-embedded tissue blocks of the remaining tissue. Samples were considered benign if they had no tumor tissue present around the site of the sample used for DNA and RNA extraction.
Total RNA and DNA were isolated from all samples using the AllPrep DNA/RNA/miRNA Universal Kit according to the manufacturers protocol.
Read Also: Does Prostate Cancer Cause Back Pain
Imaging Of Distant Metastases At Initial Presentation
The most common site of distant metastases in PCa is the skeletal system, but the prevalence is variable and dependent on risk categories. For example, in patients with newly diagnosed PCa undergoing preoperative staging mpMRI, the prevalence of bone metastases is only 1.5% . Therefore, whole body imaging is indicated only in patients with intermediate- or high-risk disease. Visceral metastases are rare at initial diagnosis.
Although current guidelines recommend conventional imaging modalities such as BS and CT for the detection of metastases, it is well recognized that these suffer from moderate sensitivity, a significant rate of equivocal findings, poor performance for PSA levels of less than 20 ng/mL, and a lack of specificity. Therefore, more advanced techniques are being increasingly used . However, BS is established for treatment response assessment and has been shown to be an independent prognostic imaging biomarker of survival in patients with metastatic disease .
An important role for imaging in advanced PCa is the identification of patients with unfavorable features, namely bone metastases beyond the axial skeleton, lytic-appearing bone metastases, visceral metastases, or bulky tumor masses . These patients with unfavorable features will likely benefit from intensified treatment regimens including targeted radiation therapy and chemotherapy .
Prostate Imaging Features That Indicate Benign Or Malignant Pathology On Biopsy
Catherine Elizabeth Lovegrove1,2, Mudit Matanhelia1,2, Jagpal Randeva1,2, David Eldred-Evans1,2, Henry Tam1,2, Saiful Miah1,2, Mathias Winkler1,2, Hashim U. Ahmed1,2, Taimur T. Shah1,2
1Division of Surgery, Department of Surgery and Cancer, Imperial College London 2Imperial Urology, Charing Cross Hospital, Imperial College Healthcare NHS Trust , , UK
Contributions: Conception and design: None Administrative support: None Provision of study materials or patients: None Collection and assembly of data: None Data analysis and interpretation: None Manuscript writing: All authors Final approval of manuscript: All authors.
Correspondence to:
Keywords: Prostate magnetic resonance imaging imaging quantitative qualitative benign malignant parametric
Submitted Mar 01, 2018. Accepted for publication Jul 11, 2018.
doi: 10.21037/tau.2018.07.06
Read Also: What Is Scraping Of The Prostate
Symptoms Of Prostate Cancer
- Frequent urge to pass urine, especially at night
- Weak or interrupted urine stream
- Pain or burning when passing urine
- Nagging pain in the back, hips, or pelvis
Prostate cancer can spread to the lymph nodes of the pelvis. Or it may spread throughout the body. It tends to spread to the bones. So bone pain, especially in the back, can be a symptom of advanced prostate cancer.
Risk Factors For Prostate Cancer
Some risk factors have been linked to prostate cancer. A risk factor is something that can raise your chance of developing a disease. Having one or more risk factors doesn’t mean that you will get prostate cancer. It just means that your risk of the disease is greater.
- Age. Men who are 50 or older have a higher risk of prostate cancer.
- Race. African-American men have the highest risk of prostate cancerâthe disease tends to start at younger ages and grows faster than in men of other races. After African-American men, prostate cancer is most common among white men, followed by Hispanic and Native American men. Asian-American men have the lowest rates of prostate cancer.
- Family history. Men whose fathers or brothers have had prostate cancer have a 2 to 3 times higher risk of prostate cancer than men who do not have a family history of the disease. A man who has 3 immediate family members with prostate cancer has about 10 times the risk of a man who does not have a family history of prostate cancer. The younger a man’s relatives are when they have prostate cancer, the greater his risk for developing the disease. Prostate cancer risk also appears to be slightly higher for men from families with a history of breast cancer.
- Diet. The risk of prostate cancer may be higher for men who eat high-fat diets.
Also Check: What Type Of Doctor Treats Prostate Issues
Eligibility Criteria And Patient Characteristics
The inclusion criteria for our study were as follows: patients referred with a suspicion of PCa who underwent prostate mpMRI between October 2015 and January 2019 and with no history of biopsy prior to MRI either a negative MRI or diffuse PIRADS 3 change reported on MRI a subsequent negative systematic prostate biopsy or at least 1-year clinical follow-up to exclude malignancy. The exclusion criteria were as follows: severe artifacts on MRI the presence of prostatic intraepithelial neoplasia , high-grade PIN , or atypical small acinar proliferation at pathology pathologically confirmed acute or chronic prostatitis . The final study population included a total of 175 patients.
What Is A Heterogeneous Prostate
What is a heterogeneous prostate?
Doctor’s Assistant: Is the condition chronic, or acute?
Dont know. I saw the following on a lab result from a ultrasound..The prostate is heterogeneous with probable calcifications and measures approximately 4.2 x 3.0 ? 2.7 cm with a volume of approximately 18 cc.
Doctor’s Assistant: Anything else in your medical history you think the doctor should know?
Had the ultrasound due to some issues. Dont have a follow up with my doctor for a few weeks but received the lab results which has me looking for information
This can be easily treated with antibiotics and with various medications to improve the flow of and reduce the night time urination. The blood test that you had done was for prostate cancer, if you had prostate cancer then the PSA would have been MARKEDLY elevated. In your case, it is completely normal which is a good thing.
So in your case, the ultrasound likely represents inflammation of the prostate along with stones which can be treated with medications.
Do you have any more questions?
I sincerely ***** ***** I have helped you and that I have earned my 5-star rating today! Please remember to rate my service by selecting the 5 stars at the top of the screen . We can continue here until you are satisfied, simply use the reply box and let me know. Thank you!. You can also ask questions from me directly by going to the link below,
http://www.justanswer.com/medical/expert-dr-muneeb-ali/
Do you have any more questions?
Also Check: Cystoscopy Transurethral Resection Of Prostate
