Types Of Radical Prostatectomy
The prostate gland lies just under the bladder and in front of the rectum.
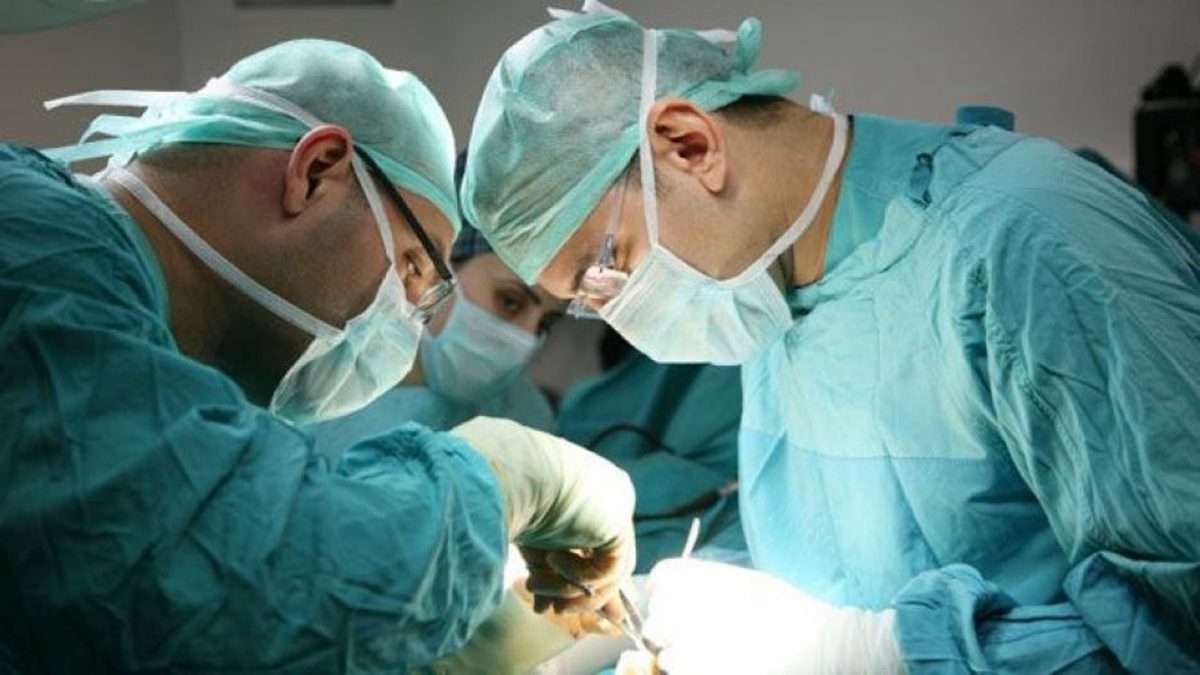
Surgeons choose from two approaches to reach and remove the prostate during a radical prostatectomy. One is a traditional approach known as open prostatectomy. The other is minimally invasive. That means it involves several small cuts and a few stitches.
Open Prostatectomy
There are two ways to do this traditional method:
Radical retropubic prostatectomy. Before the surgery, youâll get medicine called anesthesia either to help you âsleepâ or to numb the lower half of your body. Then, your surgeon will make a cut from your belly button down to your pubic bone.
If your surgeon thinks itâs possible that your prostate cancer has spread to nearby lymph nodes, they may remove some of these nodes and send them to a lab to check for cancer cells while youâre still under anesthesia.
If the lab finds cancer, your surgeon might decide not to go on with the surgery. Thatâs because surgery probably wouldnât cure your cancer, and removing your prostate could bring on serious side effects.
Radical perineal prostatectomy. For this less-common surgery, your surgeon reaches your prostate through a cut they make between your anus and scrotum. Youâll get anesthesia before the operation.
Minimally Invasive Surgeries
There are two minimally invasive procedures used in radical prostatectomy:
Laparoscopic prostatectomy
This type of prostatectomy has become more common over the years.
How Gamma Knife Surgery Treats Brain Tumors
It’s a form of brain surgery without any incisions. Patients with brain tumors, both benign and malignant, often are candidates for a noninvasive procedure called gamma knife stereotactic radiosurgery. It pinpoints high doses of radiation at the tumor with little impact to surrounding healthy tissue.
Watch this “Mayo Clinic Minute“video to hear Bruce Pollock, M.D., a Mayo Clinic neurologic surgeon, explains the procedure:
It’s called gamma knife surgery, but there’s no cutting involved.
“Gamma knife radiosurgery is the precise delivery of radiation to some imaging-defined target so we’re able to treat benign or malignant tumors within the brain,” says Dr. Pollock.
It’s been used at Mayo Clinic for 30 years as an alternative to open brain surgery.
“We’re performing an outpatient-based procedure that doesn’t require an incision and has no risks of infections,” says Dr. Pollock.
The patient’s head is held still during the procedure with a headframe, which also serves as a map for the radiation. Using 3D imaging typically an MRI as a guide, the gamma knife is targeted directly at the tumor.
“The mechanical accuracy of the device is measured as a fraction of a millimeter,” says Dr. Pollock.
And with no hospital stay and minimal side effects, it’s a procedure that is efficient and can be lifesaving.
What To Expect With Steam Therapy
Steam therapy is performed under local anesthesia in the clinic. Most patients report mild discomfort during treatment but no pain. No incisions are needed.
During the treatment, a physician inserts a small needle into the urethra and positions it within the prostate gland. In nine seconds, the needle produces a 2-centimeter-wide steam ball that shrinks surrounding prostate tissue. It does not carry heat outside the prostate or affect other surrounding tissues. The number of treatments increases with prostate size but can be completely treated during one visit.
The needle is removed, and a temporary catheter is placed to drain urine from the bladder. This catheter is usually removed after three to five days.
Most patients can return home the same day as steam therapy and resume regular activities within a few days. Initially, benign prostatic hyperplasia symptoms may worsen before they improve. This is because the treatment causes some swelling. Some patients start to experience fewer benign prostatic hyperplasia symptoms within two weeks, and most see improvements by six weeks.
Also Check: What Age Do Prostate Exams Start
Possible Complications And Side Effects
When undergoing prostatectomy, patients can expect to experience some side effects and complications, Tyson noted, though they are mostly rare. More common complications include incisional pain, nausea as a result of anesthesia, urinary tract burning and constipation.
More rare complications, according to Tyson, include infection of both the wound and the urinary tract, as well as urine leaks. When you have patients with a catheter in for seven days, excised the prostate, you obviously injure the urinary tract, and so infections are not totally out of the ordinary, Tyson said.
And while they are extremely rare, Tyson mentioned that injuries during surgery can occur to areas like the rectum, vasculature, bladder or even the lower extremities. These are all really, really rare complications, but they’re important to remember. In surgery, we take nothing for granted.
In less than one percent, Tyson explained, lower extremity lymphedema is also a possible complication to consider, especially when pelvic lymph node dissection is involved. In these cases, plastic surgeons are then called in to restore microcirculation of the lymphatic system from the legs to the heart.
Prostate Removal Side Effects Mayo Clinic

Can hpv virus cause back pain – Anthelmintic drugs examples Hpv vaccine side effects back pain Coninutul Can hpv virus cause back pain, Chloe Brown, from Glasgow, was a bubbly and healthy year-old, who had always dreamed of becoming an actress. Can hpv virus cause back pain.
In a way, this thinking awarded me with a healthy amount of resilience. Papillomavirus detection Papillomavirus vaccin a quel age Hpv vaccine side effects back pain Mayo Clinic Minute: Doctors urge use of HPV vaccine ovule propolis papillomavirus Oncocytic sinonasal papilloma and associated sinonasal squamous cell carcinoma papilloma virus in viso, metastatic cancer how prostate removal side effects mayo clinic pronounce foot wart how to remove.
Read Also: What To Do For Enlarged Prostate
Green Light Laser Surgery For Prostate Benefits And Side Effects
Are you dealing with the annoying urinary difficulties due to benign prostate hyperplasia? Are you looking into the possibility of getting a green light laser prostate surgery that will put an end to your sufferings? But remember this surgery, like any other, comes with potential side-effects that you need to remember. Lets explore the most common and rarer side-effects of the green light laser surgery on prostate!
Who Should Get A Radical Prostatectomy
Men younger than 75 years old with limited prostate cancer and who are expected to live at least 10 more years tend to get the most benefit from radical prostatectomy.
Before doing a radical prostatectomy, doctors first try to confirm that the prostate cancer has not spread beyond the prostate. They can figure out the statistical risk of spread by looking at tables comparing the results of a biopsy and PSA levels.
Other tests to check for signs of spread, if needed, can include CT scans, bone scans, MRI scans, ultrasound, PET scans, and bone scans.
If it appears that the prostate cancer hasnât spread, your surgeon may first offer you other options besides surgery. These can include radiation therapy, hormone therapy, or simply watching the prostate cancer over time, since many prostate cancers grow slowly.
Depending on how high your risk of the cancer spreading is, your surgeon may also consider doing an operation called pelvic lymph node dissection.
Recommended Reading: Is Prostate Cancer Curable If It Has Spread
Caring For The Catheter
You will be discharged with a Foley catheter, a tube that continuously drains urine from your bladder into a bag and that you will use for seven to 10 days. Before you leave the hospital, your nurse will teach you how to empty and care for your catheter and drainage bag. The catheter works with gravity and should be draining urine at all times, so you have to keep the drainage bag below your bladder at all times, even when you shower. If your urine is not draining, lower the bag and check the connection for kinks or loops. Loops can cause an air lock that prevents drainage. You can also try emptying the bag. Then try briefly disconnecting the catheter from the clear plastic tubing to allow a little air into the system. Your nurse will show you how to do this before your discharge.
To prevent infection, you must keep your catheter clean. This section explains how to clean the catheter, the area around the catheter and the drainage bag. It also explains how to apply your leg bag and secure the catheter to your leg.
We will provide most of the supplies you need to care for your catheter. They include:
- Blue clamp
- StatLock Foley catheter securement device
- Shaving supplies
You should empty the catheter bag when it’s half full. This helps prevent air locks from developing in the tubing.
To apply the leg bag:
Benefits Of Steam Therapy
Steam therapy for benign prostatic hyperplasia has many benefits. It is a quick outpatient procedure with little downtime required. It’s a good option for patients who are not interested or unable to take benign prostatic hyperplasia medications, and it produces long-lasting results and relief from benign prostatic hyperplasia symptoms. Finally, the treatment does not affect erectile function and rarely affects ejaculation.
Talk with your health care team about any benign prostatic hyperplasia symptoms you are experiencing. Together, you will consider your symptoms, the size of your prostate, and your goals to determine if treatment is needed and the best option for you.
Scott Pate, M.D., is a urologist in La Crosse and Prairie du Chien, Wisconsin.
For the safety of our patients, staff and visitors, Mayo Clinic has strict masking policies in place. Anyone shown without a mask was either recorded prior to COVID-19 or recorded in a non-patient care area where social distancing and other safety protocols were followed.
Topics in this Post
Recommended Reading: How Often To Milk Prostate
The Sperling Prostate Center Advantage
Our philosophy is to match the treatment with the disease. Our BlueLaser 3T mpMRI-Guided Biopsy is the most responsible and accurate way to know your disease before making a treatment decision. We help patients avoid the risk of under-treating aggressive disease, or over-treating insignificant disease that can safely be monitored. We pride ourselves on having attained international recognition for excellence in real-time MRI-guided prostate cancer diagnosis.
If BlueLaser 3T mpMRI detects cancer, a biopsy is essential because prostate cancer may not show early symptoms, though certain warning signs indicate increased prostate cancer risk:
- An elevated or rising PSA blood test result
- An abnormal digital rectal exam
- A family history of prostate cancer or breast cancer
- Being of African-American descent
- Exposure to certain cancer-causing toxins, e.g. Vietnam vets exposed to Agent Orange
- In later stages, prostate cancer may show symptoms such as urinary difficulties, blood in urine, pelvic or back pain, and bone pain. See a doctor if any of these symptoms occur.
The Role Of Surgery In Prostate Cancer Treatment
Some patients are better suited for surgery than others. In general, patients with widespread metastatic disease are also not good candidates for surgery, particularly if their cancer has spread beyond the prostate to areas like the liver, lungs, and bones.
In addition to an in-depth look at the role surgery plays in the treatment of prostate cancer, Dr. Mark Tyson, II, an associate professor of urology at the Mayo Clinic in Phoenix, Arizona, recently offered patients a glimpse into the future with an overview of up and coming procedures like focal therapy at CURE®s Educated Patient® Prostate Cancer Summit.
Also Check: What Is Better For Prostate Cancer Surgery Or Radiation
Few Side Effects Found From Radiation Treatment Given After Prostate Cancer Surgery
- Date:
- Mayo Clinic
- Summary:
- The largest single-institution study of its kind has found few complications in prostate cancer patients treated with radiotherapy after surgery to remove the prostate. Men in this study received radiotherapy after a prostate-specific antigen test following surgery indicated their cancer had recurred.
The largest single-institution study of its kind has found few complications in prostate cancer patients treated with radiotherapy after surgery to remove the prostate. Men in this study received radiotherapy after a prostate-specific antigen test following surgery indicated their cancer had recurred.
Researchers say the findings from Mayo Clinic’s campuses in Florida and Minnesota suggest that patients and their physicians should not overly worry about toxicity and side effects from the treatment, known as salvage external beam radiotherapy. The study findings will be published in the October issue of Radiotherapy and Oncology.
“There is a general fear of this kind of radiation treatment on the part of some patients and their physicians, but this study shows that it not only effectively eradicates the recurrent cancer in a substantial number of patients, but that there are few serious side effects,” says the study’s lead investigator, Jennifer Peterson, M.D., from the Department of Radiation Oncology at Mayo Clinic in Florida.
“No other therapy besides salvage external beam radiotherapy has been shown to cure these patients,” she adds.
Story Source:
Post Prostatectomy: What Do Rising Psa Levels Mean
New to group! Wish I had checked this out 2 years ago while supporting my husband! Now over e years post prostatectomy, wondering what might make psa go from all 0 to 2.6
Welcome to the Prostate Cancer group, .You ask a good question. What can rising PSA levels means years after having had a prostatectomy?There are several reasons why one’s PSA level may rise after being stable for a time. This article explains it well: PSA levels after prostatectomy
Here’s an excerpt from the article:”Seeing a rise in PSA level does not always mean that prostate cancer is returning or spreading. The test is very sensitive and can pick up small changes in PSA levels. Doctors will usually want to know how quickly levels of PSA in the blood are rising. To find this out, a person will need to have regular PSA tests. If levels of PSA remain stable or rise very slowly, treatment may not be necessary.
In some cases, high PSA levels in the blood are not due to cancer cells. Some factors that can affect PSA levels include: older age ethnicity medicationA doctor will take these factors and the person’s medical history into account when looking at test results. This can help them decide if PSA levels are high enough to cause concern.”
Thank you! Relieves my mind somewhat! Next PSA in November.. long wait.
Don’t Miss: What Happens After Prostate Surgery
What Is The Prostate’s Role In Urination
When urine is emptied into the bladder from the kidneys, it’s kept inside the body by a couple of valves that stay closed until your body tells them to open when you urinate.
If youve had your prostate completely removed, youve had a surgery called radical prostatectomy. Along with the prostate gland, the surgeon has to remove one of the valves outside the prostate that open and close to let urine out or keep it in. Usually having one working valve is enough, but there might also be also be some effect on the nerves and muscles in the area from the surgery that allows urine to leak. Approximately 6% to 8% of men who’ve had surgery to remove their prostates will develop urinary incontinence.
Incontinence After Prostate Surgery No Big Deal: Men
By Frederik Joelving, Reuters Health
4 Min Read
NEW YORK – Many men have some degree of incontinence after prostate surgery, but few are significantly bothered by it, according to a poll at one U.S. hospital.
Of 315 patients whod had their prostate removed due to cancer, only a quarter said a year or more after surgery that they never experienced any leakage.
Still, more than three-quarters of the men said they didnt use pads in their underwear and only about one in 20 said they were significantly bothered by incontinence.
The bottom line is that many men, after having their prostate removed, will have some impact on the way they urinate, said Dr. Erik Castle, an associate professor of urology at the Mayo Clinic in Phoenix, who led the new work. But the degree of the impact is minimal.
According to the American Cancer Society, one in six men gets prostate cancer at some point in his life and one in 36 men in the U.S. will die from it.
While there is controversy over how to treat low-risk tumors, some of which may never cause any harm if left untreated, surgery and radiation are common options when the disease is more advanced.
But men considering these treatments also face possible side effects like becoming incontinent or impotent. And getting useful information about how common these problems are is difficult, Castle said, because there are so many different ways of defining them.
SOURCE: bit.ly/koe8mc The Journal of Urology, online May 14, 2011.
Recommended Reading: What Is Good For Prostate Health
Are There Differences Between Orp Lrp And Ralrp
According to a 2010 of different surgery types for prostate cancer, the outcomes for open radical prostatectomy , laparoscopic , and robotic-assisted prostatectomy are not significantly different.
But people who choose LRP and RALRP may experience:
- less blood loss
- shorter hospital stay
- faster recovery time
Also, people who choose RALRP report faster recovery in continence and decreased hospital stay, in comparison to LRP. But the overall outcomes still depend on the surgeons experience and skill.
