Safety And Efficacy Of Proton Therapy
Many people with locally advanced cancers are treated with a combination of chemotherapy and either traditional or proton radiation. For patients getting chemotherapy and radiation at the same time, finding ways to limit side effects without making the treatment less effective is a high priority, Dr. Baumann said.
He and his colleagues analyzed data from nearly 1,500 adults with 11 different types of cancer. All participants had received simultaneous chemotherapy plus radiation at the University of Pennsylvania Health System between 2011 and 2016 and had been followed to track side effects and cancer outcomes, including survival. Almost 400 had received proton therapy and the rest received traditional radiation.
Those who received proton therapy experienced far fewer serious side effects than those who received traditional radiation, the researchers found. Within 90 days of starting treatment, 45 patients in the proton therapy group and 301 patients in the traditional radiation group experienced a severe side effectthat is, an effect severe enough to warrant hospitalization.
In addition, proton therapy didnt affect peoples abilities to perform routine activities like housework as much as traditional radiation. Over the course of treatment, performance status scores were half as likely to decline for patients treated with proton therapy as for those who received traditional radiation.
Proton Beam Therapy Changes A Mayo Clinic Patient’s Life
Topics in this Post
An average kindergartener goes to birthday parties, builds forts and starts learning how to read. But she doesnt plan on getting cancer.
When Anika Chesak was diagnosed with rhabdomyosarcoma — a type of tumor that wraps itself around soft tissue — at age 5, the course of her childhood drastically changed.
Dark days
In the fall of 2009, Anika complained of headaches and didnt want to get out of bed, according to her mother, Sherry Chesak, Ph.D., a registered nurse and program director in Education and Professional Development at Mayo Clinic in Rochester, Minnesota.
Anika had seen her family medicine physician at Mayo Clinic Health System Albert Lea and Austin in Austin, Minnesota, for these symptoms, but Dr. Chesak and her husband noticed that Anika was rapidly losing weight, which concerned them.
I saw Anika squinting and closing one of her eyes while walking down the hall, and she said she saw two of everything, says Dr. Chesak. Their physician directed them to Mayo Clinic.
A computed tomography scan indicated a sinus infection, and Anika was placed on antibiotics. But the scan had revealed a questionable spot. An MRI showed a tumor behind Anikas right eye, on her optic nerve.
That was quite shocking, says Dr. Chesak.
Searching for hope
I was scared because I saw that my mom was scared, Anika says. I didnt know what I was going to have to go through.
Changing directions
Treatment
Hope restored
Topics in this Post
Mayo: Cost Of Trials Is Factor
With a 10-year investment in protons totaling almost a billion dollars, Mayo says the production of randomized trials on protons has been limited by cost
“RCTs are very expensive,” Laack says.
“For most new therapies, these are supported by pharmaceutical companies that are involved in developing the drug … there are many possible cancers and indications and not enough vendors to fund all the possible trials that could demonstrate the value of protons for our patients.”
Mayo researchers have contributed to more than 300 papers on the treatments, according to Laack. She says 12 of those papers are randomized controlled trials, but that they are concerned with which patients benefit most from protons, rather than whether protons are superior to photons.
Mayo currently has 10,459 patients enrolled in a registry that would allow comparisons of proton therapy patients to photon therapy, but that effort is not randomized. One reason is that it isn’t easy to get cancer patients to accept randomization, Laack says, and the patient count is small enough to begin with.
“We need more proton centers and more access to protons,” she says, “if we are going to be able to run randomized clinical trials in a reasonable timeframe.”
As the clinic moves more of its chips on the board in favor of protons, in other words, an answer to when the technology will demonstrate superiority according to the highest level research will have to wait.
Also Check: What Does Your Prostate Control
Mayo Clinic Plans $200m Proton Beam Expansion To Meet Growing Demand
Rochester, Minn.-based Mayo Clinic is planning a 110,000-square-foot, $200 million expansion of its proton beam therapy program facility. The addition is expected to be complete in 2025.
When the additions are complete, the health system anticipates the facility will be able to treat an additional 900 patients per year.
“When it opens in 2025, the expanded facility will feature two new treatment rooms, in addition to four treatment rooms currently in operation and improved access for patients requiring proton therapy,” said Nadia Laack, MD, chair of radiation oncology at Mayo Clinic.
The health system uses pencil beam scanning for its proton beam therapy, which enables highly targeted radiotherapy to cancerous tissue and reduces radiation exposure to healthy tissue. The therapy is ideal for patients with tumors near or within vital organs, Dr. Laack said.
Existing services provided at the facility will be available during the construction period, which is expected to begin in late 2022.
Five Years After Treating Its First Patient Mayo Clinic Is Considering Expansion
The extremely controversial $188 million program has delivered on its promise. Now, proponents are looking to build a second center in Rochester.
Jennifer Vyse, of Appleton, Wis., rings a bell signifying the end of her proton beam radiation treatment for nasal cancer Tuesday, Sept. 29, 2020, in Mayo Clinics Jacobson Building in Rochester.
ROCHESTER, Minn. Five years after the launch of the $188 million program, Mayo Clinic is looking to build a second center in Rochester.
Based in the Richard O. Jacobson Building in downtown Rochester, Mayo Clinics program has treated 4,142 patients as of August. That far surpasses the original goal of treating 3,200 in that time, according to Dr. Robert Foote.
Foote was the chairman of Mayo Clinics radiation oncology department and director of the proton beam program when it started treating patients in June 2015.
Mayo radiation oncologist and Proton Beam Therapy Program Director Dr. Robert Foote
He acknowledges that Mayo Clinics proton beam treatment facility was extremely controversial when it was first proposed.
It was a huge amount of money, Foote said.
Five years later, Foote and others are confident that the impact on patient care has justified the expense.
While the number of competing U.S. proton beam centers has grown to 34, including Mayo Clinics Arizona treatment center, Mayo Clinics Rochester facility, with its four treatment rooms, is still often busy from before 6 a.m. until midnight, according to Foote.
Don’t Miss: Can Mri Miss Prostate Cancer
Ideas For Future Studies Of Proton Therapy
Despite the studys limitations, these intriguing findings raise questions that should inform future prospective phase 3 trials, Dr. Buchsbaum said, although there are barriers to large studies of proton therapy.
For instance, it is particularly encouraging that proton therapy appeared to be safer in a group of older and sicker patients who typically experience more side effects, Dr. Baumann noted.
Dr. Buchsbaum agreed that proton therapy may be especially helpful for older and sicker patients, but he noted that ongoing phase 3 trials were not designed to analyze this group of patients.
And because proton therapy may cause fewer side effects, future trials could also explore whether combining proton therapy with chemotherapy might be more tolerable for patients, the authors wrote.
For example, both chemotherapy and traditional radiation for lung cancer can irritate the esophagus, making it painful and difficult for patients to eat. But proton therapy might limit damage to the esophagus, making it easier for a patient to tolerate the combination, Dr. Baumann explained.
Future studies could also explore whether combining proton therapy with higher doses of chemotherapy might increase cures without causing more side effects, he added.
Dr. Buchsbaum agreed, saying that it would be worthwhile to explore this possibility. Just asking the question: Is more effective? might not be giving it a fair opportunity to demonstrate its benefit to society, he said.
The Catch Is The Cost
The catch with proton beam treatment is the cost, which is usually at least double the price of photon treatment for a patient. That fact, coupled with limited research about proton beam treatment, causes many experts to be critical of hospitals investing so much to offer it.
The machines and the buildings needed to house them are considered the most expensive medical equipment available. Thats a health care investment that could have been spent on more traditional treatments.
Building centers in Rochester and Phoenix cost Mayo Clinic an estimated $370 million. A new center on Mayo Clinics Florida campus is expected to cost about $233 million.
Mayo leaders are well aware of the criticisms aimed at proton beam therapy, mostly centered around cost.
If there were no financial differences, there would be proton access at every medical center in the U.S., said Laack.
Money from donors gives nonprofits such as Mayo Clinic an advantage over for-profit institutions when trying to foot the bill. Richard O. Jacobson, an Iowa businessman, donated $100 million to help finance the construction of Mayo Clinics proton beam cancer therapy program. The result is Mayo Clinic doesnt need to recoup as much of an investment as a medical center that had to pay the entire bill.
Plus, Mayo Clinic has notably not increased the price for the treatment in the past five years, in order to keep the treatment accessible.
Don’t Miss: When To Get Prostate Test
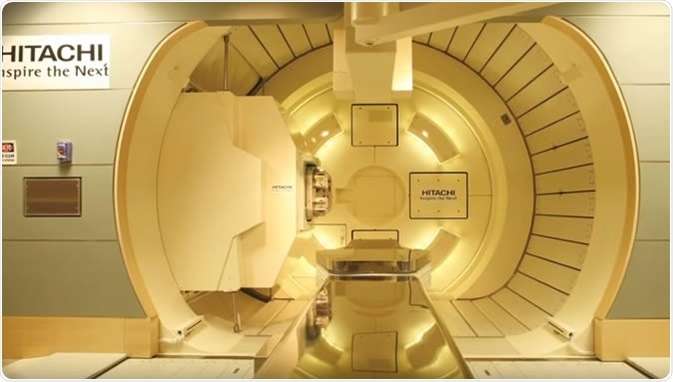
Mayo Clinic Begins Treatments With Hitachi Probeat
Minnesota facility first to install system with Discrete Spot Scanning capability Arizona campus to follow suit
Image courtesy of Hitachi Ltd.
The Probeat-V is a state-of-the-art proton beam therapy system used to deliver Hitachis Discrete Spot Scanning capability to each treatment room. The 190-degree half gantries provide efficient yet spacious treatment room environments patients no longer need to be positioned inside a 360-degree gantry, as all treatment angles are achieved by a 6-degree of freedom couch. A 30 percent smaller treatment spot size, achieved through refinements in nozzle design, enables the system to achieve highly precise treatments. In addition, installation and commissioning activities are already underway at a second Mayo facility in Phoenix, Arizona, with treatments scheduled to start in the spring of 2016.
Mayo Clinic treats more than 1.3 million patients annually from all 50 states and 143 countries. Mayo Clinic has maintained its position as one of the top hospitals in U.S. News & World Report rankings for more than 20 years.
The Probeat-V system also offers:
For more information: www.hitachimed.com
Before You Keep Reading
MPR News is made by Members. Gifts from individuals fuel the programs that you and your neighbors rely on. Donate today to power news, analysis, and community conversations for all.
Mayo will use the technology primarily for head and neck, breast, gastrointestinal, lung, spine and prostate cancers. Doctors also will use it to treat tumors in or near the eye.
An advancement to traditional radiation therapy, pencil beam scanning targets only the tumor, sparing the surrounding tissue, said Dr. Robert Foote, chair of Mayo’s Department of Radiation Oncology in Rochester.
“Its a lower dose of radiation to normal organs, so its a safer way of administering radiation treatments,” Foote said. “Much lower entrance dose as the beam enters the body and it stops at the tumor and theres no exit dose. So theres less harm to the normal organs that surround the cancer.”
Because of this, the benefit of pencil beam scanning for children is especially clear, he said.
Proton therapy can be considerably more expensive than traditional radiation, in part because of the cost of the equipment and facility. The four-room Rochester location will cost approximately $188 million. The center in Arizona is expected to cost $182 million. Funding for the projects will come from Mayo’s capital budget and benefactor support, according to Mayo officials.
To understand how pencil beam scanning works, check out this video from Mayo Clinic’s Medical Edge:
Also Check: How To Have A Prostate Orgasim
With Nearly A Billion Dollars Tied Up In Cyclotrons Rebar And Concrete The Superiority Of The Treatments Remains In Question
ROCHESTER, Minn. As Mayo Clinic invests hundreds of millions of dollars into proton beams, the wait continues for decisive evidence that the treatments are superior to existing methods at reducing tissue damage following radiation of tumors.
The lack of highest-level trial data in support of the sophisticated cancer treatments underscores a persistent dichotomy in medicine today, one in which calls to “follow the data” rise alongside projects reflecting the intangible, enduring fascination with technology.
Otherwise known as demand.
Mayo cited the demand for proton beam therapy when it announced plans earlier this month to build a $200-million, 110,000-foot addition to its Robert O. Jacobson Building, a $188 million center launched in 2015.
When it opens in 2025, the expansion will increase capacity for the high-tech treatments on the Rochester campus by 50%, allowing the care of an extra 900 patients annually.
At six rooms, the Jacobson Building will become one of largest proton beam centers in the nation.
It will join a trio of planned or completed proton centers under the Mayo banner, an infrastructure stockpile that includes a $182 million structure in Phoenix, and a $233 million building in Jacksonville, Florida, slated for 2026.
The arsenal will give Mayo more proton resources than those currently held within the entire United Kingdom .
It’s become a common analogy to describe a medical intervention like a parachute.
A More Precise Treatment
Proton beam therapy delivers radiation treatment via a pencil beam to specific areas of the body much more precisely and with more power than traditional photon radiation treatment. That means other organs are not unintentionally exposed, reducing negative patient side effects and the occurrence of secondary cancers. Mayo Clinic is conducting research about patient impacts from proton beam versus photon treatment. Due to the cost of the treatment centers, research has been limited.
Dr. Nadia Laack, chairwoman of Mayo Clinics Department of Radiation Oncology, explained that the precision of proton beam treatment compares very favorably to traditional photon radiation treatment.
Dr. Nadia Laack
Less radiation is good when it comes to long-term outcomes, she said. Why would you have 20,000 dental X-rays done, when you only need one?
The amount of radiation that proton treatment spares an average patient is equivalent to 5 million dental X-rays, 50,000 mammograms, or 5,000 chest CT scans, according to Laack.
Thats a particular benefit for pediatric patients. About 10 percent of the patients treated with proton beam radiation are children.
Also Check: How Many Men Die Of Prostate Cancer
Limitations Of The Studys Design
The study leaders and other experts noted several limitations to the studys design.
For instance, this observational study cant establish a cause-and-effect relationship between proton therapy and fewer side effects. In addition, all of the study participants were treated at a single institution, which can make it difficult to generalize the findings to a larger population.
Those are very significant limitations that shouldnt be understated, Dr. Buchsbaum emphasized.
Although single-institution studies have inherent limitations, Dr. Baumann noted, all patients in this study received high-quality treatment at a large academic medical center, regardless of whether it was proton or traditional radiation therapy, which suggests that the benefit of proton therapy that we saw is meaningful.
Also, because patients were not randomly assigned to treatment groups, there were differences between patients who got proton and traditional radiation, and that may have skewed the results.
For instance, patients who received proton therapy were, on average, older and had more health issues.
The proton therapy group may also have included more patients from privileged backgrounds, Drs. Park and Yu noted. Socioeconomic status and social support can affect treatment outcomes, they wrote.
In addition, fewer people with head and neck cancerwho are more likely to suffer from radiation-associated side effectswere included in the proton therapy group, the editorialists added.
It Costs More But Is It Worth More
Ezekiel J. Emanuel on health policy and other topics.
If you want to know what is wrong with American health care today, exhibit A might be the two new proton beam treatment facilities the Mayo Clinic has begun building, one in Minnesota, the other in Arizona, at a cost of more than $180 million dollars each. They are part of a medical arms race for proton beam machines, which could cost taxpayers billions of dollars for a treatment that, in many cases, appears to be no better than cheaper alternatives.
Proton beam therapy is a kind of radiation used to treat cancers. The particles are made of atomic nuclei rather than the usual X-rays, and theoretically can be focused more precisely on cancerous tissue, minimizing the danger to healthy tissue surrounding it. But the machines are tremendously expensive, requiring a particle accelerator encased in a football-field-size building with concrete walls. As a result, Medicare will pay around $50,000 for proton beam therapy for a patient with prostate cancer, roughly twice as much as it would if the patient received another type of radiation.
To generate sufficient revenue, proton beam facilities need to treat patients with other types of cancer. Consequently, they have been promoted for patients with lung, esophageal, breast, head and neck cancers. But the biggest target by far has been prostate cancer, diagnosed in nearly a quarter of a million men each year.
But it is crazy medicine and unsustainable public policy.
You May Like: What Hormones Cause Prostate Enlargement
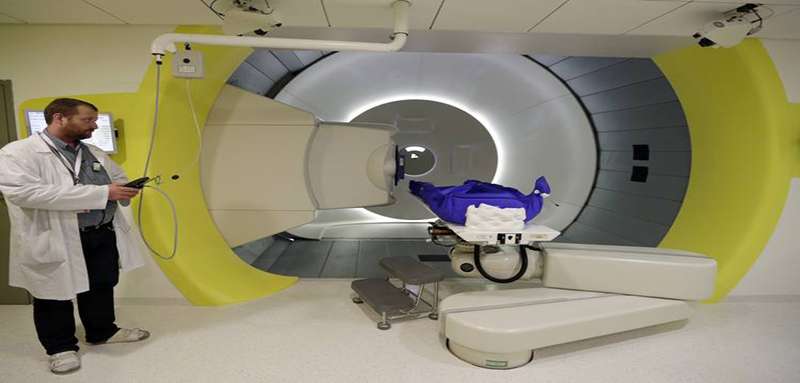
Is Proton Therapy Safer Than Traditional Radiation
Traditional radiation therapy delivers radiation to the tumor and to healthy tissues around the tumor. With proton therapy , the majority of the radiation is delivered to the tumor.
A type of radiation treatment called proton beam radiation therapy may be safer and just as effective as traditional radiation therapy for adults with advanced cancer. That finding comes from a study that used existing patient data to compare the two types of radiation.
Traditional radiation delivers x-rays, or beams of photons, to the tumor and beyond it. This can damage nearby healthy tissues and can cause significant side effects.
Plus, proton therapy is more expensive than traditional radiation, and not all insurance companies cover the cost of the treatment, given the limited evidence of its benefits. Nevertheless, 31 hospitals across the country have spent millions of dollars building proton therapy centers, and many advertise the potential, but unproven, advantages of the treatment.
In the new study, patients treated with proton therapy were much less likely to experience severe side effects than patients treated with traditional radiation therapy. There was no difference in how long the patients lived, however. The results were published December 26 in JAMA Oncology.
These results support the whole rationale for proton therapy, said the studys lead investigator, Brian Baumann, M.D., of the Washington University School of Medicine in St. Louis and the University of Pennsylvania.
